Three Keys to Ceramic Dental Adhesion: Enamel, Dentin, and Cementum Variations
The longevity and retention of direct composite restorations or indirect ceramic veneers depend on adequate dental adhesion to the tooth surface, making ceramic adhesion an essential aspect of restorative dentistry. Therefore, knowing tooth structural variations helps when creating esthetic and sealed gingival margins to enhance the predictability of outcomes.
One reason indirect anterior restoration margins are commonly placed on root structure with a cemented, full-coverage type of restoration is that many believe it is too challenging to isolate the area for bonding. However, this is not practical thinking because to attain a long-term, predictable result, both margins must be isolated to the same degree, a challenge just as great.
Although proper isolation is essential for cementation and bonding indirect restorations, this mindset can stem from a doctor’s lack of confidence in adhesive bonding protocols and techniques.
Adhesive bonding to tooth structure involves variables. First, the type of bonding strategy, etch and rinse vs. self-etch vs. self-adhesive, plays a role in marginal integrity and overall bond strength. Then the choice of material plays a role in the integral strength of the restoration and longevity of the bond. Finally, managing the cleanliness of substrate surfaces (both tooth structure and restorative material) also influences adhesive predictability. Due to de-bonding, improper process management in these areas may lead to marginal leakage, tooth sensitivity, secondary caries, or restoration failure.
Tooth Structure and Its Impact on Dental Adhesion
Tooth structure is a bio-composite of enamel and dentin, which are diverse in biologic makeup and different in various regions of the tooth.
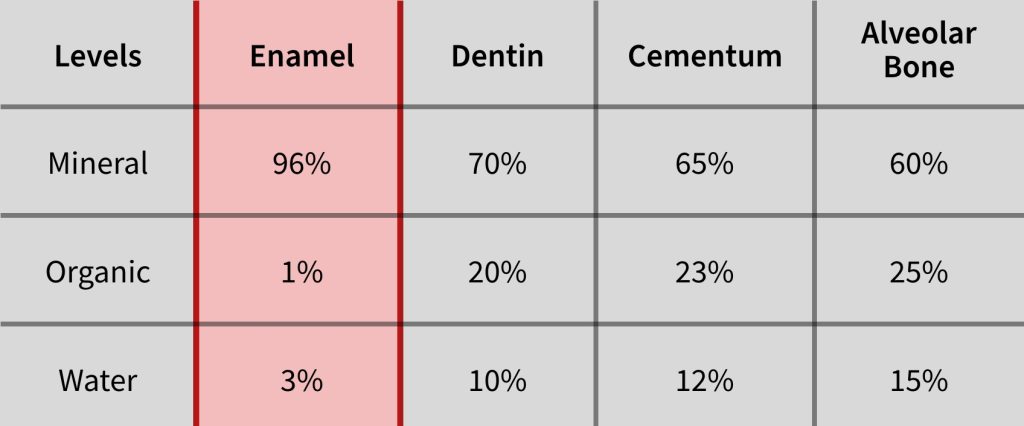
Enamel is primarily inorganic in structure. Approximately 95% hydroxyapatite crystals are mixed with some collagen and minimal water. Dentin, however, is primarily organic and humid. It is approximately 20% water mixed with hydroxyapatite crystals attached to a meshwork of collagen fibrils. This contrast in structure significantly impacts bond strength and durability.
Cementum is primarily an inorganic matrix covering the root surfaces, protecting and sealing the dentinal tubules. In addition, the rough surface (an acellular fiber-matrix) allows for the attachment of the periodontal ligament fibers. The critical feature differentiating demineralized (etched) cementum from dentin is the lack of patent tubule orifices. The capillary action of the resin to produce micro-mechanical integration is limited, giving cementum a distinct disadvantage in bonding dental adhesion.
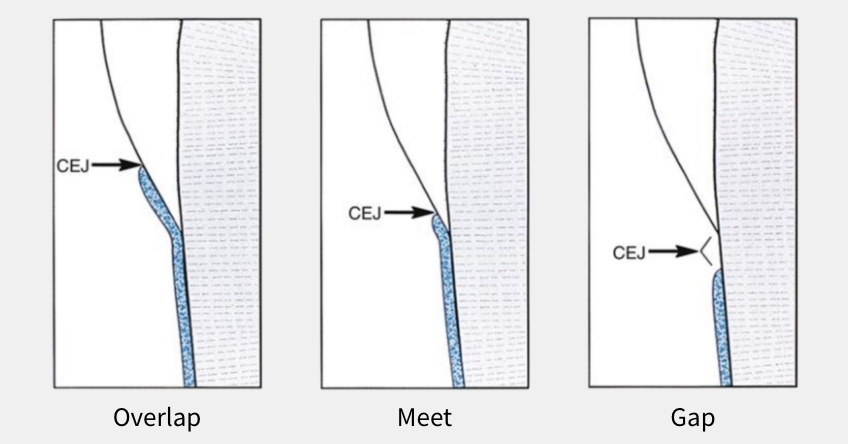
Preparing indirect veneers requires tooth reduction from the incisal edge to the gingival margin. The desired shade change primarily dictates the amount of tooth reduction necessary for the material of choice. Thus, enamel and dentin structures are affected by any preparation greater than ultraconservative (e.g., no-prep).
It is well documented that the bond to enamel is stronger (~60 MPa) and more durable than the bond to dentin(~30MPa). These studies primarily ensue from enamel and dentin obtained from the “body” of the tooth, i.e., tooth structure components that are mid-facial or mid-buccal in origin. However, the cervical aspect of the veneer preparations can be the most critical relative to longevity and integrity. Understanding those differences and utilizing strategies that enhance the dental adhesion and bring predictability to the outcome is essential.
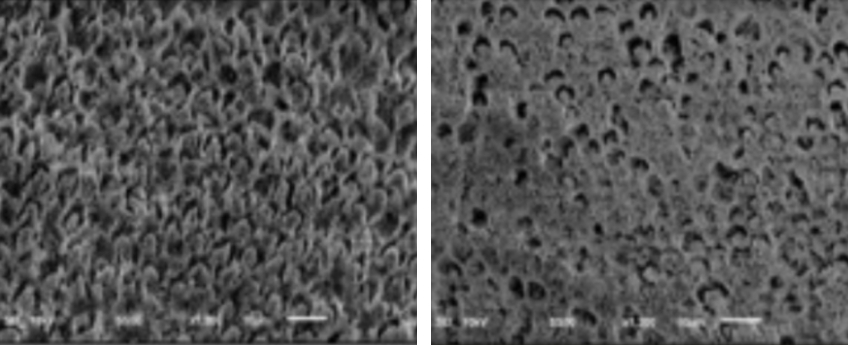
Since enamel is primarily inorganic in structure, body enamel crystals are arranged in a regular pattern. Histologically, they exhibit a hexagonal appearance in cross-section. When etched with 30-40% phosphoric acid, the enamel exhibits a regular, patterned, highly micro-retentive surface. The hydrophobic adhesive resin penetrates into these pores by capillary action, creating interlocking resin tags.
Conversely, cervical enamel is thin and less structurally organized than enamel and demonstrates a thicker a-prismatic structure. This structural difference results in shorter resin tags and lower bond strengths. Many studies confirm this decrease in bond durability.
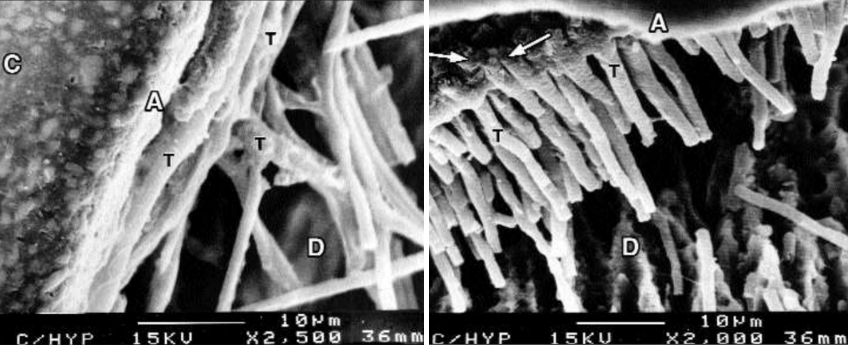
Dentin consists of dentinal tubules and an interdental matrix. Dentin tubules run from the dentin-enamel junction (DEJ) in coronal dentin toward the coronal pulp and course from the cementum-dentin junction to the radicular pulp. Dentinal tubules are narrower, contain less pupal fluid toward the outside of the tooth/root, and are wider pulpally. Root dentin has fewer dentin tubules than coronal dentin. The fewer dentinal tubules dramatically affect the bond’s strength and durability to cervical dentin. Additionally, physiologic aging and secondary caries (sclerotic dentin) affect adhesive strength.
Clinicians must remain aware of the structural differences between enamel, dentin, and cementum and use strategies that enhance bond strength and durability when placing margins at or below the gingival tissues.
Key Aspects for Long-Term Restorative Outcomes
- Field isolation and prevention of fluid intervention (e.g., blood, saliva, etc.) are critical. Contamination jeopardizes dental adhesion and leads to failure, such as the loss of restoration, cervical staining, secondary caries, etc.
- Developing confidence and competence in bonding strategies and protocols is necessary. Bonding techniques are essential. You must follow the manufacturer’s directions and recommendations.
- According to a literature review, the etch and rinse strategy is preferred for dental adhesion in the cervical region. Because cervical enamel has a thick a-prismatic layer and the dentinal root tubules are fewer, this strategy provides improved resin micro-mechanical interlocking to both the enamel and dentin.
- Following adhesive bonding, polishing the cervical margins may lead to greater restoration longevity and improved marginal gingival health. Surface resin tags may remain at the margin following clean-up. Cementum, if present, is rough compared to enamel and dentin, so it is possible to have micro-roughness at the gingival margins following clean-up. Polishing these margins with a composite polishing system/strategy (versus ceramic polishing) may enhance the longevity of the restoration.
Ceramic dental adhesion is an essential aspect of restorative dentistry. Creating esthetic and sealed gingival margins is crucial to restoration longevity, as is understanding tooth structural variations to enhance the predictability of outcomes.
References
- Kikushima, D., Shimada, Y., Foxton, R. M., & Tagami, J. (2005). Micro-shear bond strength of adhesive systems to cementum. American Journal of Dentistry, 18(5), 364-368.
- Toledano, M., Perdigão, J., Osorio, R., & Osorio, E. (2000). Effect of dentin deproteinization on microleakage of Class V composite restorations. Operative Dentistry, 25(6), 497-504.
- Barnhart, E. C., Campbell, P. M., Noureldin, A., Julien, K., & Buschang, P. H. (2021). The quality of etched enamel in different regions and tooth types and its significance in bonding and the development of white spot lesions. The Angle Orthodontist, 91(5), 576-582.
- Andermatt, L., & Özcan, M. (2021). Micro-shear bond strength of resin composite cement to coronal enamel/dentin, cervical enamel, cementoenamel junction, and root cementum with different adhesive systems. Journal of Adhesion Science and Technology, 35(19), 2079-2093.
SPEAR ONLINE
Team Training to Empower Every Role
Spear Online encourages team alignment with role-specific CE video lessons and other resources that enable office managers, assistants and everyone in your practice to understand how they contribute to better patient care.

By: Jeffrey Bonk
Date: August 30, 2022
Featured Digest articles
Insights and advice from Spear Faculty and industry experts