Technique for ‘Cementing’ and Retaining Conservative Ceramic Onlay Provisionals
Indirect partial coverage ceramic restorations are becoming a mainstay of conservative restorative dental procedures. As traditional full coverage crowns have been the “go-to” for restoring structurally compromised teeth for decades, newer materials and the ability to bond restorations, rather than cement, have supported the growth of indirect ceramic onlays and inlays.
Full-coverage crown preparations require significant removal of tooth structure. This irreversible extensive preparation may have adverse effects on the pulp and gingival tissues. Additionally, the iatrogenic reduction of enamel and dentin weakens tooth integrity and flexural strength.
While full-coverage crowns are appropriate in specific structurally compromised circumstances, this service may ultimately lead to tooth loss. The literature states that crown preparations can be the “circle of death” for teeth. This may be true in certain circumstances, but it is important that the restorative dentist performs the most conservative restorations possible in a given situation.
Why Partial Coverage Restorations Matter
Partial coverage restorations may be performed on both anterior and posterior teeth. Anteriorly, these indirect ceramic restorations are commonly known as veneers. Posteriorly, depending on how much tooth structure requires replacement and coverage, these conservative restorative alternatives are called inlays, onlays, or “veneer-lays.”
These thin ceramic shells are adhered to the minimally prepared tooth structure through an adhesive technique rather than cementation for strength and longevity. The limited mechanical retention of the specific partial coverage tooth preparations requires strict adherence to bonding protocols. These partial coverage alternatives to crowns predictably restore esthetics and function to structurally compromised teeth. Literature studies report 85% success (integrity) at 20 years of service.
There are differing techniques and strategies applied toward preparing teeth conservatively for partial coverage ceramic restorations. The design of the tooth preparation (how much tooth structure is removed) is primarily dependent upon the esthetic shade change desired and the inherent strength requirements of the restorative material to be utilized.
Spear’s Restorative Design workshop encompasses three days of hands-on technique for analyzing and preparing teeth for conservative partial coverage restorations. Both anterior and posterior partial coverage preparations are introduced and practiced. This workshop provides comprehensive guidelines for restoring teeth predictably with indirect ceramic restorations. The goal of tooth preparation design is to conserve as much tooth structure as possible and provide a restorative solution that creates longevity of service.
Provisionalization Challenges and Solutions
Provisionals are a necessary component of all indirect restorative procedures. Fabricating partial coverage provisionals utilizes the same techniques as full coverage provisionalization. A direct (intraoral) or indirect (made on a stone model) technique may be chosen as the fabrication method. Typically, a matrix of putty or “suck-down” style plastic overlay of the wax-up contour is used as the “provisional former.”
The provisional restores esthetic and functional contours that resemble the final restoration. These outlines also guide the dental laboratory when fabricating the final ceramic product. Additionally, management of tooth sensitivity is a critical requirement for provisionalizing prepared tooth structure.
Both thermal and surface irritation may occur from open exposure of the prepared dentin. The conservative nature of the partial coverage preparations results in challenging retentive designs for provisionalization. The more conservative the preparation, the fewer contours and features present for resistance and retention of the provisional.
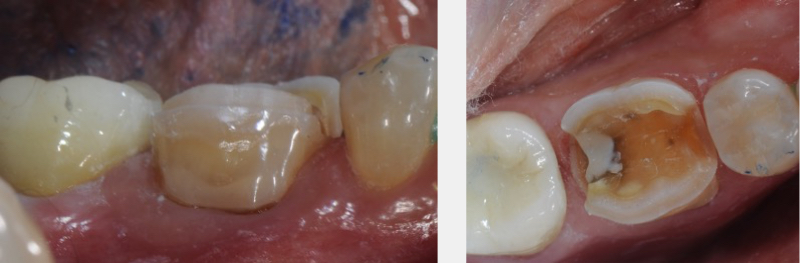
In many circumstances, posterior partial coverage restorations replace pre-existing large, old fillings. Many of these old restorations include a significant portion of the occlusal surface and extend into the interproximal areas. The resultant partial coverage tooth preparation then contains interproximal “boxes” following removal of the old filling material.
These “boxes” aid in retention of the provisional restoration by promoting resistance to dislodgement. A conventional provisional cement may be utilized (Kerr’s Temp-Bond or Caulk Fynal are examples of these more conventional provisional cements).
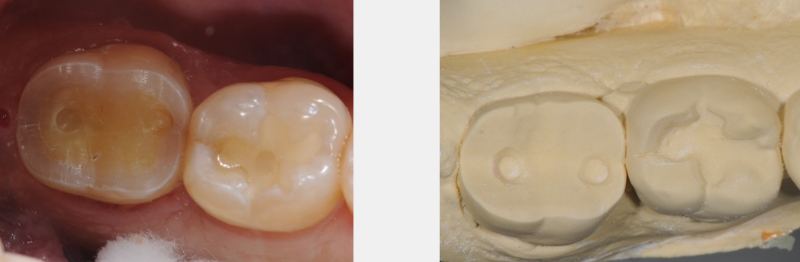
Alternatively, there can be situations where no preexisting restorations exist, and there is a need to “contain the cusps” to manage fractures and cracks within the teeth. These minimal partial coverage restorations become very challenging to predictably provisionalize.
The significant lack of resistance and retention form necessitates creative ways to provisionalize and manage tooth sensitivity during the interim weeks until final ceramic fabrication and insertion. One “resistance tool” we suggest in the Restorative Design workshop is to prepare “lugs” in the occlusal surface of the tooth.
These “lugs” are 1.0 mm “pot-hole” preparations designed to provide restoration stability when seating both the provisional and final restoration. Additionally, they provide a degree of “increased surface area for the “cement” or bonding resin.
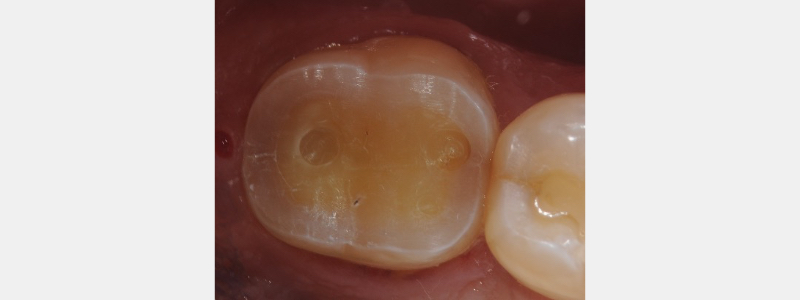
When conventional provisional cementation has minimal retention form, we must take advantage of the structural design of the natural tooth to aid in maintaining the provisional during ceramic fabrication. The photo above clearly indicates a normal tooth’s enamel and dentinal integrity. From an occlusal view, the outer enamel rim thickness can be close to 1.5 mm (when approximately 2.0 mm of occlusal reduction has occurred).
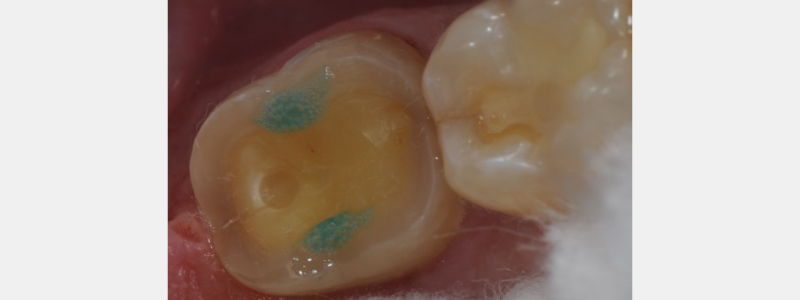
Challenges with retention form may be overcome in conservative tooth preparation by taking advantage of adhesive dentistry and the enamel/dentin complex. Provisional restorations can be retained predictably by strategically “spot etching” enamel and dentin.
As shown in Fig. 4, a definitive and contained area of enamel and dentin is etched on both the buccal and lingual aspects. Care is taken not to include the marginal areas of the tooth preparation. The circumference e of the etched surface needs to be no larger than 2-2.5 mm. This “spot” is the “retentive key” to maintaining the provisional over time.
After 30 seconds, this etchant is rinsed, and the enamel and dentin primers are placed. Self-etching materials must be avoided, as the entire enamel/dentin matrix may be bonded to the provisional.
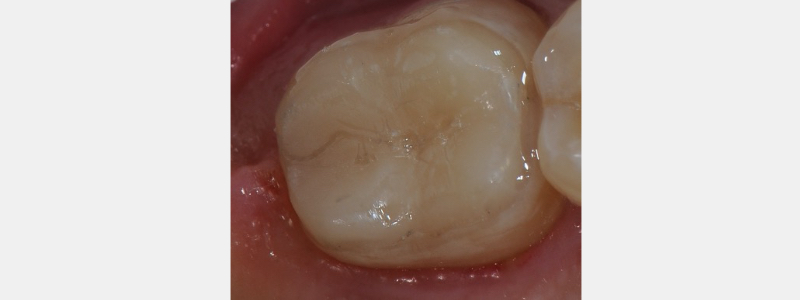
With the dentin primed, the bonding resin may be applied as “the cement.” Resin is applied with a micro brush to both the enamel dentin primed surface and the intaglio (inside aspect) of the provisional. With the provisional seated, the excess resin is wiped and the provisional is light-cured to place. Additionally, a flowable composite may be placed inside the provisional to help create a more intimate (filled) connection to the tooth. The patient is instructed to “pull” the floss through the contact rather than “snapping” the floss out from under the contact point.
At the time of ceramic restoration insertion, the provisional is removed by wedging a small excavator or scaler between the contact point of the adjacent tooth. Before processing the ceramic try-in, the enamel and dentin’s etched and bonded surfaces must be lightly abraded.
One can use a fine football-shaped diamond rotating at low speed to clear the surface of resin tags. Care must be taken not to contact the preparation enamel margins. Alternatively, the occlusal surface may be “micro-etched” with air particle abrasion. The fit and stability of the ceramic restoration can now be evaluated.
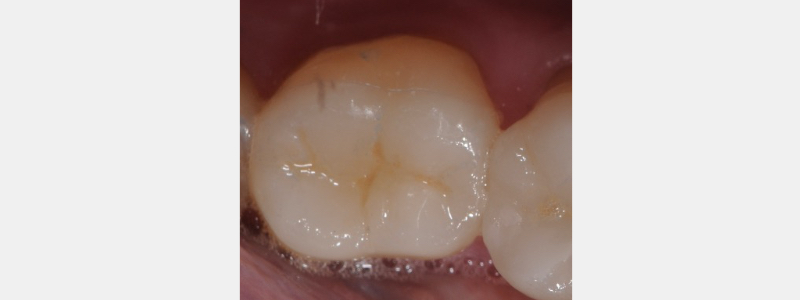
Creating Predictable, Long-Term Success
Conservative partial coverage ceramic restorations are important esthetic and functional restorative solutions in our practices today. Maintaining tooth structure allows patients to keep their teeth for a lifetime. Although managing the interim provisionalization can be challenging, techniques like “spot-etching” can prove instrumental in creating successful and predictable outcomes.
SPEAR campus
Hands-On Learning in Spear Workshops
With enhanced safety and sterilization measures in place, the Spear Campus is now reopened for hands-on clinical CE workshops. As you consider a trip to Scottsdale, please visit our campus page for more details, including information on instructors, CE curricula and dates that will work for your schedule.

By: Jeffrey Bonk
Date: April 7, 2021
Featured Digest articles
Insights and advice from Spear Faculty and industry experts


