A Protocol for Symptom-Free Direct Composites
When I first graduated and started placing composites in private practice, it became routine to have patients call with postoperative sensitivity. I would see the patient for a second appointment, typically squeezed between already-scheduled patients, and I‘d grind down the occlusion, somewhat confident that would solve the problem. If they called with continued symptoms, I’d see them for a third appointment and do the same. If they called a following time, they fell into the category of being a “baby.” It was never my fault.
This is arguably one of the worst repeat occurrences to throw into your schedule: The patient is in discomfort and your schedule becomes a nightmare. When grinding doesn’t solve the problem, you become frustrated, your patient loses trust in you, and your restorations end up looking like you placed them with your thumb.
Like many, dental materials class was just another hoop to jump through in dental school for me. Because it was taught before doing any dentistry, I didn’t realize until a few years into private practice how important it is to respect the chemistry. The number of seconds you spend agitating the primer does matter: “Too wet” or “too dry” is a real issue.
There’s a personality quirk among dentists to want to get to the point, the bottom line, the black-and-white protocol we can use tomorrow. With hundreds of adhesives on the market today and almost an equal number of composites, there is no black-and-white system for everyone. Part of it ultimately comes down to what works in your hands. But there are some areas of your technique that will make or break the outcome of your work.
I took a course from Ron Jackson that changed my entire perspective on adhesion. I can give him full credit for teaching me to respect the chemistry. I started implementing what I learned from him, and I now have maybe one call per year with postoperative sensitivity from a direct restoration.
I used to think cold sensitivity after a composite is placed was “normal” and would eventually go away. Today, I almost never hear a patient complain about temperature sensitivity.
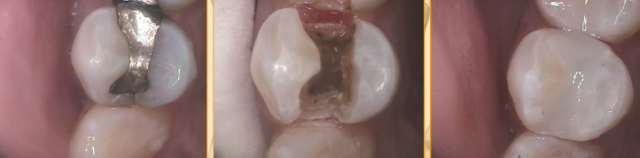
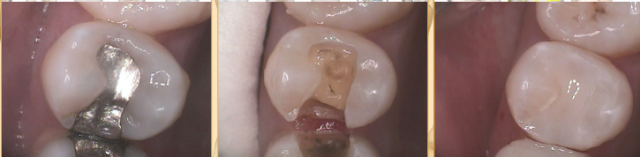
I’m going to walk you through the exact protocol that I use in my office, but not with the intent of you throwing out your current system. I hope that by sharing what I’m using, and why I complete each step, you can look at your own protocol and see if you can justify each part of your own process. If you can’t, hopefully you can better evaluate the areas of your protocol that may need adjusting.
Here’s how a composite is done in my practice:
Check the occlusion
There’s nothing worse than building beautiful anatomy into a composite, only to grind it away. I find that checking from the beginning allows you to have minimal adjustments at the end and preserves your beautiful work.
Isolate
I don’t think you can ever expect reliable outcomes with adhesive dentistry unless you properly isolate. I honestly believe that if you’re routinely using dry angles and cotton rolls, especially with mandibular teeth, precision with the remaining steps doesn’t truly matter — you’ve lost any consistency or predictability straight out of the gate. For most of my posterior composites, I’m isolating with an Isovac; when that can’t be tolerated, I’ll switch to a rubber dam.
Evaluate the tooth’s enamel-to-dentin ratio before etching
Enamel likes etch; dentin doesn’t. Enamel needs to be etched at least 15 seconds; dentin shouldn’t be etched more than 15. How do we handle that?
I use Bisco HV selective etch, which has chlorhexidine in the etchant to eliminate MMPs. When there’s enamel present, I place the etch (with a fine tip) along the enamel, count to three, then place the etch over the dentin. Because in the next step you’ll see that I’m using a self-etching primer, if I have a deep preparation, sometimes I won’t etch the dentin at all and I’ll only etch the enamel. If you aren’t using a self-etching primer, you need to etch the entire surface before moving to the next step.
After etching enamel for 15+ seconds and dentin for no more than 15 seconds, I rinse and air-dry the tooth. I like to see a bit of frothy enamel, but I don’t overdry the dentin.
Place gluteraldehyde
My next step is to use glutaraldehyde. (Check out this article, which elaborates on why I think this should be used in both direct and indirect placement.) I use Clinician’s Choice G5; Gluma is an arguably more popular alternative and it works equally well but costs significantly more. I place G5 on the tooth and rub it into the surface for 30 seconds; I have a time clock running in the corner of my computer screen during treatment. When I’m not setting it for impression lengths, I’ll keep it running for counting these steps. I will lightly air-dry the glutaraldehyde, but I don’t overdry it. Primer doesn’t mind water!
Use a self-etching primer
I then use a self-etching primer. I’ve been using Kerr’s Optibond XTR universal adhesive system for about three years with great success. It’s the only universal that I’m aware of with chemistry that I can get behind. Other than this particular brand, I only have Generation IV and V systems in my office. I was using Optibond FL, a fourth-generation (etch/prime/bond in separate steps), for a few years with equally good success, but I switched to the universal to simplify my bonding system so I can use the same for both my direct and indirect protocols. I also like being able to evaluate on a tooth-by-tooth basis where to etch.
The other adhesive system I have in my office is Excite F, a fifth-generation system of total etch, followed by primer/adhesive in one bottle. I will use this system in the anterior when I’m working exclusively in enamel. I don’t have any single-bottle systems in my office and haven’t read any literature that convinces me that you can get the same predictability and longevity of restorations with seventh-generation systems. Likewise, I’m not confident in a lot of the other universal systems available today. Optibond XTR is unique in its two-bottle system, and I use it more like a fourth-generation with the exception of necessitating dentin etching.
After I place the primer, I agitate it aggressively into the tooth surface for 10 seconds before air-drying. Adhesives don’t like water, so this is the step to confidently dry after adequate placement.
Place adhesive and composite
I then place Optibond XTR adhesive. After placing the adhesive, I lightly air-dry it to create a thin, even film on the tooth and light-cure. Optibond XTR calls for 10 seconds of curing. Some of the newer lights can do a one-second cure, but I stick to a 10-second cure without blasting the tooth with heat. Again, this is only my technique, and it works, so I’m hesitant to introduce change.
I have a few different composites in my office depending on the location, size, and expectations of outcome on the tooth. I use Sonicfill when there isn’t a lot of discoloration on the tooth, because it’s too translucent to mask amalgam staining well. I use Estelite Omega in some cases and Venus Diamond in others. I always layer when I’m not using a bulk composite — and even when using a bulk composite, I find that you have to condense repeatedly to avoid air bubbles.
Sometimes the patient is cooperative and I have time, so I’ll use tints and stains and really go at the anatomy. Sometimes the patient wants out of the chair or the schedule doesn’t allow for me to have as much “fun,” and at the end of the day, I’m more than likely the only person who’s going to appreciate the detail of the occlusal pit of #31!
In summary, here is my go-to protocol for routine posterior composites:
- Bisco HV selective etch — always on enamel, selectively on dentin
- G5 Glutaraldehyde, air lightly
- Optibond XTR primer, air-dry
- Optibond XTR adhesive, lightly air, light-cure
- Composite in layers; if not bulk, light-cure
While I don’t want you to throw what you’ve got away and start using everything I’m using, if you’re having post-operative complications with your composites, take out the manufacturer’s suggestions for use and make sure you’re using them correctly and can justify each step.
SPEAR campus
Hands-On Learning in Spear Workshops
With enhanced safety and sterilization measures in place, the Spear Campus is now reopened for hands-on clinical CE workshops. As you consider a trip to Scottsdale, please visit our campus page for more details, including information on instructors, CE curricula and dates that will work for your schedule.

By: Courtney Lavigne
Date: April 1, 2018
Featured Digest articles
Insights and advice from Spear Faculty and industry experts