- Techniques / Materials
4 Tips for Decreasing Sensitivity After Composites
Do you struggle with sensitivity after placing composites? Are your patients reluctant to proceed with treatment because they have had sensitivity in the past after having composites placed by you or another dentist? Have you yourself come to believe that sensitivity after placing composites is normal?

If you answered yes to any of these questions, keep reading for four easy tips to help make sensitivity with your composites a rarity.
Excellent isolation
This is #1 because without this, you are sunk and can expect sensitivity no matter how well you do everything else. For me, hands down, this means an Isolite (Fig. 1), IsoDry, or rubber dam in the posterior because I believe cotton roll isolation and dry angles are just too risky in the posterior. The risk for contamination is high.
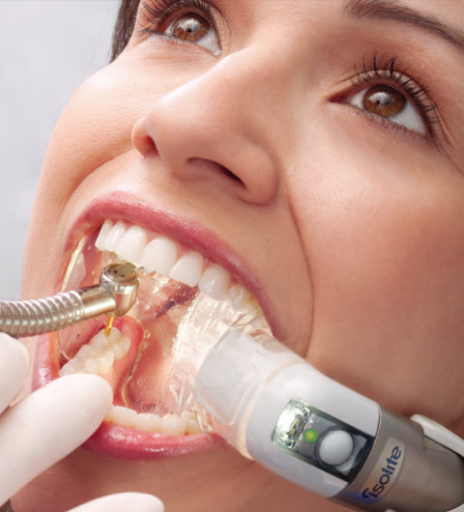
When it comes to the anterior, you can sometimes safely use something like cotton roll isolation. If that is not enough, you’re best to go to an Isolite, IsoDry, or rubber dam, just like the posterior. The key thing to remember is that even the tiniest bit of contamination means you’re sunk.
Proper etching
With the advent of self-etching bonding resins, this has in some ways gotten easier. However, with most if not all bonding agents, even the self-etching ones, it is best to etch the enamel. With some agents like universal bonding systems (Adhese Universal from Ivoclar, Scotchbond Universal from 3M), it can be advisable to still etch the dentin, depending on the case.
Sensitivity usually results from improper enamel etching; over-etching is usually the biggest culprit. The typical time for dentin is 10–15 seconds, but you should check the instructions for your specific product. When it comes to enamel, it’s way harder to over-etch it, but the typical time is 15–20 seconds. If you are pre-etching the dentin, the key here is remembering that time is critical. You need to be right on time — not over and not under.
Proper drying
As we know, after etching, we must rinse and dry the tooth. If we have etched the dentin, we have another big potential source for sensitivity: over-drying the dentin and collapsing the dentinal tubules. This results in poor penetration of our bonding resin and, therefore, sensitivity.
It’s important to note that even if you get the drying part right and don’t over-dry (think moist dry, not bone dry), it’s also essential to be sure you’re using clean air to dry the teeth. It’s not uncommon for our air-water syringes to blow a little water or oil with them when using the air. In my office, I have switched to Adec warm air tooth dryers to eliminate this risk. If Adec tooth dyers are not in your future or you want an immediate way to help check for contamination from your air-water syringe tips, blow air across your clean mouth mirror. You should see nothing in your mirror.
Proper curing
This one is simple: We have to make sure our composite is fully cured all the way, though; otherwise, we can expect bad things. The keys here are to make sure your layers aren’t too thick and to get as close as you can to whatever you are curing without touching it. You must also cure for the length of time specified by the manufacturer for the material you are curing.
I cannot stress enough the need to get close enough to your curing light; small increases in distance significantly decrease your light’s curing intensity. Another essential thing to consider is periodic testing with a light meter (Fig. 2) to ensure your light’s intensity is as it should be. Playing with these meters is also a great way to see how fast the intensity drops as the distance increases. Lastly, you must also ensure your light guide is undamaged and the tip is clean.
SPEAR campus
Hands-On Learning in Spear Workshops
With enhanced safety and sterilization measures in place, the Spear Campus is now reopened for hands-on clinical CE workshops. As you consider a trip to Scottsdale, please visit our campus page for more details, including information on instructors, CE curricula and dates that will work for your schedule.

By: John Carson
Date: March 18, 2017
Featured Digest articles
Insights and advice from Spear Faculty and industry experts