Occlusal Stability in Restorative Dentistry: When Is It Safe To Treat?
Occlusal stability in restorative dentistry determines whether treatment succeeds or fails over time. A stable occlusion protects restorations, supports joint health, and reduces biomechanical risk. Before initiating treatment, dentists must evaluate the temporomandibular joints (TMJs), airway, and craniofacial development to ensure the system can support long-term outcomes.
What is occlusal stability in restorative dentistry?
Occlusal stability refers to a balanced relationship between the teeth, muscles, TMJs, and airway that allows function without breakdown. When these components work in harmony, forces are distributed predictably, minimizing wear, fracture, and joint strain.
Without occlusal stability in restorative dentistry, even well-executed restorative work can fail because the underlying system cannot support it.
A restorative treatment plan aims to establish a stable occlusal relationship to protect the restorations. However, understanding “when it’s safe to treat” can be complicated. The dentist and the patient must understand the risks before treatment, and when the patient understands the risks beforehand, they can make an informed decision.
Why occlusal stability matters before restorative treatment
If the dentist fails to recognize the risks and the restorative work fails, the patient may perceive the failure as poor dental work, when the actual reason for the failure is often instability that may have contributed to the breakdown of the existing dentition. Therefore, it’s imperative to ensure the occlusal stability in restorative dentistry before treatment begins.
Evaluating stability starts by understanding the design of the occlusal system. Historically, dentists believed that malocclusion was the root of parafunction, muscle soreness, and temporomandibular dysfunction (TMD), with the notion that “bad bites cause bad joints.” However, a growth disturbance in the maxillary or mandibular skeleton may also contribute to malocclusion. Form inevitably follows function, and disturbances in craniofacial growth often lead to malocclusion, affecting both the static and dynamic occlusal systems.
How craniofacial growth affects occlusal stability
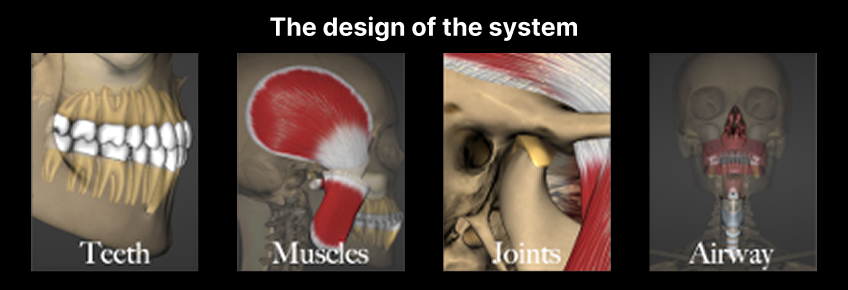
The “design of the occlusal system” includes the teeth, muscles, temporomandibular joints (TMJs), and airway (Fig. 1). Proper occlusion depends on all four areas working in harmony. Understanding growth provides insight into why malocclusion develops and how early intervention can provide a platform for occlusal stability in restorative dentistry.
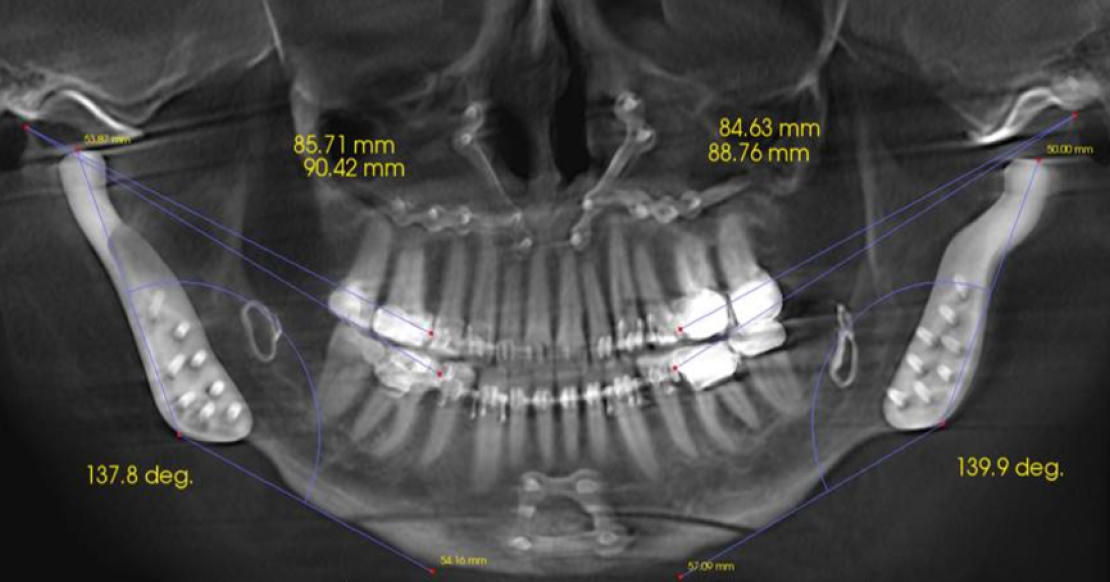
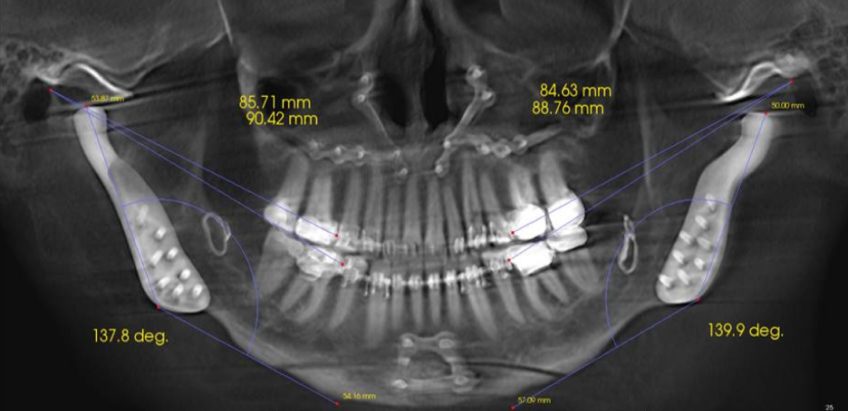
The three main areas of craniofacial growth are the maxillary suture system, the dentoalveolus, and the mandibular condyle, all of which influence occlusal stability in restorative dentistry. In normal development, much of maxillary growth occurs during the first five postnatal years, and the anterior dentoalveolar height approaches its adult dimensions by age five, establishing an early foundation for functional occlusal development.
What role does the airway play in occlusal stability?
Airway-disordered breathing often originates from nasal breathing dysfunction and can significantly impact occlusal stability in restorative dentistry. When nasal breathing is inhibited, patients adopt oral breathing and an open-mouth posture. A “mouth breather” rests the tongue on the floor of the mouth rather than against the palate, limiting its role in maxillary development. In contrast, proper tongue posture supports palatal widening and forward growth of the pre-maxilla by balancing facial muscle forces. Patients with a dolichocephalic profile (Fig. 2) frequently present with a history of airway-disordered breathing.

How TMJ health influences occlusal stability in restorative dentistry
Growth of the condyle is the primary influence on mandibular development and plays a key role in occlusal stability in restorative dentistry. Bone apposition in the condylar cartilage drives forward mandibular growth. Studies have shown disruption of vertical condylar growth in adolescent patients with disc displacement, likely due to a chronically displaced disc altering the normal functional environment.
The disc is responsible for load distribution and, under compression, secretes synovial fluid that lubricates the joint and provides nutrition to the articular cartilage of the condyle. In a structurally altered TMJ, damage can occur to tissues because of the compressive and shear forces of the condyle under normal function. In growing patients, this may lead to a premature closure of the growth center, inhibiting the anterior projection of the mandible and impacting the occlusal stability in restorative dentistry.
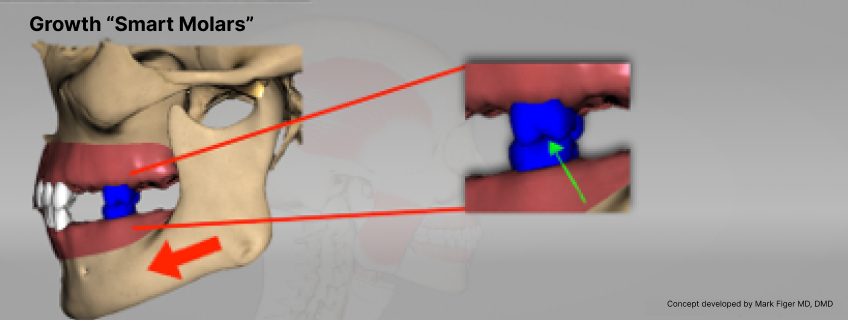
Normal growth depends on a symbiotic relationship between the maxillary and mandibular arches. As the maxillary arch develops, condylar growth is stimulated by the interaction of the mandibular teeth with the maxillary teeth. Dr. Mark Piper described the adult first molars as the “smart molars,” emphasizing that the interaction between the maxillary and mandibular molars stimulates growth. When the mesial inclines of the maxillary molars contact the distal inclines of the mandibular molars, it pulls the condyle out of the fossa, inducing growth, a process similar to distraction osteogenesis (Fig. 3).
However, a growth disturbance in either the maxilla or mandible may result in malocclusion and instability in the system.
How to identify occlusal instability before treatment
Class I patients are typically the easiest to treat because the skeleton and dentition are properly positioned, supporting occlusal stability in restorative dentistry. The risk of instability increases when the skeletal and dental relationships are misaligned. A deficient maxilla combined with normal mandibular growth can lead to a Class III skeletal–dental relationship, often presenting both functional and esthetic concerns.
Patients presenting with a Class II occlusion can also be challenging to restore because of the lack of anterior tooth contact. Depending on the extent of the Class II relationship, these plans require more extensive intervention; they may necessitate orthodontic treatment, orthognathic surgery, or both (Fig. 4) to correct the skeletal relationship before predictable restorative treatment can begin.
Early recognition and intervention are ideal to ensure adequate growth. The window to stimulate growth has often been missed in the adult population, so restorative, orthodontic, or orthognathic interventions may be needed to correct the occlusion and esthetics. System stability is imperative for the long-term success of the treatment.
Historically, pain was used to recognize instability, but skeletal and dental malocclusion, with or without pain, needs to be evaluated before treatment.
When pain is associated with a structurally altered TMJ, symptom relief often becomes the primary reason to treat. However, occlusal stability in restorative dentistry depends on a stable TMJ foundation, making accurate diagnosis essential before treatment begins. Historically, TMJ evaluation relied on a “tentative diagnosis” based on clinical findings, but a definitive assessment requires advanced imaging to evaluate both hard and soft tissues.
What imaging is needed to assess occlusal stability?
A CBCT provides a noninvasive means to diagnose osseous pathology, and an MRI is used to assess the position and condition of the articular disc. However, the cost and availability of MRIs can remain obstacles to obtaining this imaging.
The prevalence of TMD in the general population can reach 75% and can occur at any age. As previously mentioned, treatment has focused on symptom relief, but the key to patient management is determining whether the articular disc is stable. Dr. Piper said, “Both the dentist and their patients must understand that the ultimate foundation for the dental occlusion is the temporomandibular joint itself, and it is this foundation that ultimately will determine whether occlusal management will remain predictable and stable.” Instability in the TMJs can lead to unsatisfactory treatment outcomes in terms of function, esthetics, stability, and pain.
Understanding the condition of the osseous structures and the position of the articular disc is critical to diagnosing the TMJs and establishing occlusal stability in restorative dentistry. Because the TMJ is one of the most complex joints in the body, a clear understanding of its anatomy is essential before treatment, using advanced imaging techniques. MRI is considered the gold standard for evaluating the condition and position of the articular disc.
A CBCT can serve as a screening tool by assessing the joint space and cortical plate in sagittal, coronal, and axial views. The normal thickness of the disk is typically 2–3 mm, and as Dr. Jim McKee describes in Spear’s Advanced Occlusion workshop, it acts as a gasket in the temporomandibular joint. If the articular disc herniates, it can lead to a “wobble” and instability in the system.
Assessing and evaluating the TMJ
A cone-beam computed tomography (CBCT) is considered the best method for assessing the osseous structures of the TMJs and plays an important role in evaluating occlusal stability in restorative dentistry. However, assessing joint space can also serve as a useful screening method for disc displacement. An increased anterior joint space combined with decreased posterior and superior joint space may indicate an anterior disc herniation.
A study by Yu that used both MRI and CBCT images showed that, of 52 joints with larger-than-normal anterior joint spaces and reduced posterior and superior joint spaces, 45 (87%) had disc displacements. A disc displacement changes the position of the condyle in the fossa, and an altered position of the condyle is dependent on the extent and direction of the disc displacement.
The same study revealed that healthy joints’ posterior–anterior (P-A) and superior–anterior (S-A) ratios were 1.6 and 1.9, respectively, when the condyles were in a centric position. In the disc displacement group, the joints showed a significant decrease in the P-A and S-A ratios because of an enlarged anterior joint space.
How CBCT and MRI improve TMJ diagnosis
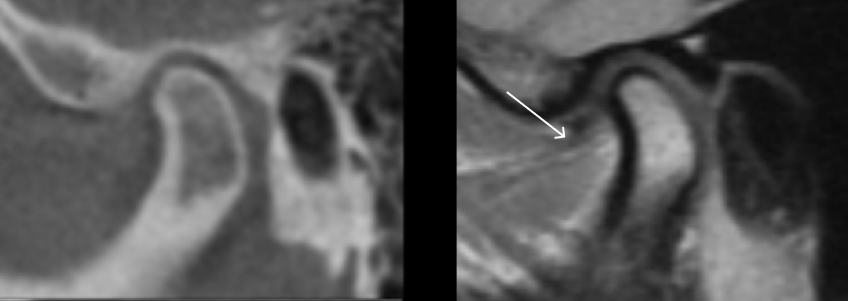
However, caution must be exercised when using CBCT alone to diagnose disc position, as misinterpretation can impact occlusal stability in restorative dentistry. The clinician may be misled when a degenerated and anteriorly displaced disc is present, especially if the retrodiscal tissue assumes a similar dimension to a healthy disc (Fig. 5).
Understanding the anatomy of the TMJs before starting treatment in both adolescent and adult patients is imperative for occlusal stability in restorative dentistry outcomes. Because disc displacements are frequently found in asymptomatic patients, including pre-orthodontic patients, CBCT and MR imaging are necessary for those exhibiting signs of decreased growth in the maxillary and/or mandibular arches.
The MRI provides superior images in multiple condylar positions without radiation exposure, but availability can be an obstacle. Therefore, a CBCT can be used as a screening tool through joint space evaluation. While an increased anterior joint space can suggest anterior disc displacement, an MRI is necessary to diagnose the TMJs accurately.
Occlusal stability in restorative dentistry is not optional; it’s the foundation of long-term success. Without it, even technically excellent dentistry can fail. Establishing stability first is a fundamental step in advanced dental treatment planning, leading to more predictable outcomes and long-term success.
By evaluating the TMJs, understanding craniofacial development, and recognizing the role of airway and function, clinicians can identify instability before treatment begins. Establishing stability first leads to more predictable outcomes, fewer complications, and better patient trust.
In restorative dentistry, success is not just about what you build, it’s about what you build on.
Frequently Asked Questions
References
- Flores-Mir, C., Nebbe, B., Heo, G., & Major, P. W. (2006). Longitudinal study of temporomandibular joint disc status and craniofacial growth. American Journal of Orthodontics and Dentofacial Orthopedics, 130(3), 324-330.
- Nebbe, B., Major, P. W., Prasad, N. G., Grace, M., & Kamelchuk, L. S. (1997). TMJ internal derangement and adolescent craniofacial morphology: a pilot study. The Angle Orthodontist, 67(6), 407-414.
- Morais‐Almeida, M., Wandalsen, G. F., & Solé, D. (2019). Growth and mouth breathers. Jornal de Pediatria (Versão em Português), 95, 66-71.
- Yu, W., Jeon, H. H., Kim, S., Dayo, A., Mupparapu, M., & Boucher, N. S. (2023). Correlation between TMJ space alteration and disc displacement: A retrospective CBCT and MRI study. Diagnostics, 14(1), 44.
SPEAR campus Workshops
Step Into a Place Built for Mastery
Step away from the noise of practice and into focused, immersive training that changes how you think, diagnose, and lead.

By: Curt Ringhofer
Date: November 6, 2025
Featured Digest articles
Insights and advice from Spear Faculty and industry experts