As If the Debate About Centric Relation Wasn't Enough: Part III
By Kevin Kwiecien on November 19, 2015 | 2 commentsIn Part I and Part II of this series, I shared with you my initial dilemma from many years ago. After fabricating a significant number of orthopedic appliances for my bruxing patients in an attempt to help them get worse at the slowest possible rate, I ran into some confusion and questioned everything I had done and learned relating to splint therapy.
My goal was always to adjust appliances to a fully-seated condylar position in an attempt to create a physiologic occlusion while protecting the teeth. I felt great about my role until I stumbled upon the fact that some of my bruxing/grinding patients being treated with appliances might have been showing signs of being negatively affected by my attempt to create a home for their teeth in the retruded position.

Contributing to Sleep Apnea
I came to the realization and subsequent confirmation in the literature that I might be contributing to the nightly self-suffocation pattern that is related to bruxism, also knows as sleep apnea.1 In the second article, I reviewed several avenues to help question our patients in an attempt to identify the at-risk population for sleep apnea, but also noted and provided literature supporting that not all patients match the profile.2
Once the patient is in the dental chair, it is important to have a system to finish the evaluation, either to help support the initial questionnaire findings or bring attention to signs and symptoms that do not match the questionnaire. There are several key components that can be easily adapted into your current clinical exam. In an attempt to avoid confusion, I am going to address the inherent conflict of managing the tooth destruction, while addressing the airway issue. (Click this link for more on airway.)
Let's assume for a moment that there is an option for a full-face or nasal mask to be used with continuous positive air pressure (CPAP) to handle the airway, while we build our appliance to manage the tooth destruction.

That is certainly a beneficial outcome to address two serious problems at the same time. Even with positive air pressure, I question the possibility of providing the optimal possible outcome of the airway issue if we build our appliance in a fully-seated condylar position. It would seem that the amount of air pressure needed to push past the retruded airway could make the CPAP therapy less comfortable and decrease the already low compliance rate. Yes, I know that CPAP compliance is directly related to the follow-up care and that the follow-up care often leaves much to be desired. But for this conversation, let's assume that the machine and mask are optimally fitted and adjusted.
Poiseuille's Law, in simple terms, states that if all else is held constant, a doubling of the radius results in a sixteen-fold increase in the flow. In other words, a very small increase in the size of the hole through which the air flows makes a really, really big difference on the amount air that flows through it.
So, even if positive air pressure (CPAP) is being used for therapy, creating physiologic occlusion on the protection appliance (night guard) to protect the teeth might be having the opposite effect on the air-hole than we want.
The great news is that there is ample evidence to support that we can decrease the bruxism while treating the apnea. If we bring the mandible forward to open the airway, bruxism has been shown to decrease while airflow increases. (Click this link for more on what causes sleep bruxism.)
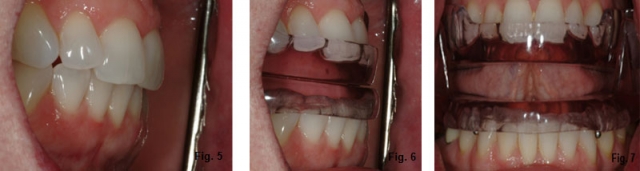
In one sleep laboratory study, the mean number of sleep bruxism episodes per hour was reduced by 39 percent and 47 percent from baseline with the mandibular advancement appliance at a protrusion of 25 percent and 75 percent, respectively.3 The bad news is that in doing so, we can create or exacerbate issues with the temporomandibular joint, as well as muscles of mastication and/or stabilization muscles.
In another controlled study, a significant reduction in the number of sleep bruxism episodes per hour (decrease of 42 percent, P < .001) was observed with the maxillary occlusal splint (MOS). Compared to the MOS, active mandibular advancement devices, with advancement, also revealed a significant reduction in sleep bruxism motor activity. However, eight of 13 patients reported pain, localized on mandibular gums and/or anterior teeth, with active MADs.4
- Temporomandibular joint pain, inflammation, clicking, popping
- Muscle tension, tenderness, discomfort
- Tooth tenderness, pain, pressure
- Bite changes, shifts, movements
"Yes" versus
- Airway opening
- Brain oxygenation
- Adequate sleep
- Healing
- Memory consolidation
- Neuronal repair
- Vigilance
- Alertness
- Sense of wellbeing
"I know what I would prefer."
So much of what we teach at Spear Education involves focusing on creating a harmonious system involving the joints, muscles, teeth and periodontium, whether it has to do with teeth or on an appliance. The use of a mandibular advancement appliance creates just the opposite! So, you should be the one to treat these patients.
Why Should I Treat Sleep Apnea?
First, you have the contact frequency, care and compassion to ask. A 2011 article reviewed a 2005 study that found 29 percent of physicians asked about sleep on a routine basis. The reasons for the low frequency ranged from a limited amount of time, to a lack of awareness, to lack of reimbursement, and to a high demand for patients’ immediate concerns.5 Second, the American Academy of Sleep Medicine Guidelines recognized early (2006) that “oral appliances should be fitted by qualified dental personnel who are trained and experienced in the overall care of oral health, the TMJs, dental occlusion and associated oral structures.” That is you.
The intent of this series of articles is in no way intended to provide a comprehensive review or treatment of sleep apnea with an oral appliance or a comprehensive understanding of the cause. On the contrary, I hope you see the value of questioning and assessing all of your patients for possible sleep disordered breathing. The intent was for us all to appreciate the conflict and ambiguity of treating sleep disorders with a mandibular advancement appliance, as well as the inherent complications of using positive pressure with an orthotic appliance.
Remember, the patient is already compromised. That is why he or she is being treated! Our goal is to try not to compromise the initial compromise. The best way to achieve this comes at the beginning of the process with a referral to a sleep physician and realizing that we may eventually be called on to create and manage the dental issues associated with mandibular advancement that we work so hard to avoid with the rest of our patients. That is how we can play such an impactful role in facilitating health for our patients.
(Did you enjoy this article? Click this link for more content from Dr. Kevin Kwiecien.)
Kevin Kwiecien, D.M.D., M.S., Spear Faculty and Contributing Author
References:
- Int J Prosthodont. 2004 Jul-Aug;17(4):447-53. Aggravation of respiratory disturbances by the use of an occlusal splint in apneic patients: a pilot study. Gagnon Y, Mayer P, Morisson F, Rompré PH, Lavigne GJ.
- Prospective Randomized Study of Patients with Insomnia and Mild Sleep Disordered Breathing, Guilleminault C; Davis K; Huynh N, Stanford University Sleep Medicine Program, Stanford, CA, SLEEP, Vol.31, No. 11, 2008, 1527-33
- Effect of an adjustable mandibular advancement appliance on sleep bruxism: a crossover sleep laboratory study. Landry-Schönbeck A, de Grandmont P, Rompré PH, Lavigne GJ., Int J Prosthodont. 2009 May-Jun;22(3):251-9.
- Reduction of sleep bruxism using a mandibular advancement device: an experimental controlled study. Landry ML, Rompré PH, Manzini C, Guitard F, de Grandmont P, Lavigne GJ., Int J Prosthodont. 2006 Nov-Dec;19(6):549-56.
- National Sleep Foundation “Sleep in America”, March 2005; Journal of Clinical Sleep Medicine “Evaluation of Sleep Disorders in the Primary Care Setting: …” Vol.7,No.1, 2011
Comments
November 19th, 2015
November 30th, 2015