An increasing number of studies are helping us to become more aware of the effects of airway issues on our adult patients. Obstructive Sleep Apnea (OSA), Upper Airway Resistance Syndrome (UARS), and other Sleep Disordered Breathing (SDB) issues have found their way on restorative problem lists.
SDB was the subject of an article last year by Dr. Steve Carstensen: "Sleep Apnea: A History of Present Illness." Relationships have been proven to exist with airway issues and high blood pressure, cardiac disease, depression and anxiety. Dental issues can include tooth wear from bruxism, tooth erosion from acid reflux and occlusion changes that can become severe and difficult to restore. Another consideration to keep in mind regarding the airway is soft tissue. Dr. Kevin Kwiecien addressed this issue in his article “That’s a Lot of Soft Tissue to Look At, But It’s Our Responsibility.”
It appears that the typical “stereotype” of the OSA patient is no longer so definite. An overweight male who snores may not be the only person we should question or screen for airway and sleep issues. “Skinny” women can have sleep related airway issues too. Even less obvious to us is the young patient, the one we could possible help reduce future risks of airway issues that can occur with aging. Children have a very low threshold of AHI (Apnea Hypopnea Index). With sleep issues they are not immune to the affects of bruxism and enamel erosion that we see in adults. Their school performance and behavior can be negatively influenced by sleep disorders.
As dentists, screening young patients for airway and breathing issues is certainly not new. Mouth breathing, daytime tiredness and “stuffy nose” have long been indications for a referral to an ENT for evaluation of adenoids and tonsils. Orthodontic literature also describes long lower face, vertical excess skeletal patterns associated with greater risk for lip incompetence and mouth breathing issues. All these indicators merit a close watch on airway and guiding growth in a more favorable direction.
An additional measurement for airway risk that dentists can add to their screening in children is palatal or intermolar width. Keeping in mind that the roof of the mouth is the floor of the nose, a narrow palate can affect the upper airway. The average inter molar width is measured from the lingual gingival margin of the upper first molars, where the lingual groove meets the gingival margin. The average width range for the permanent dentition is 35-39 mm.1 An easy addition to your exam routine is to screen for this is by using a cotton roll which measures 35-36 mm. Since it is already on the hygienist/assistant’s tray during a prophy it is an easy tool to help you see if any further investigation is indicated. (Figure 1)

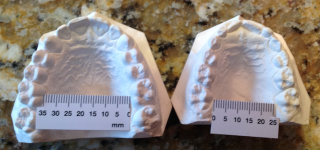
The presence of a cross bite is often the diagnostic criteria for palatal expansion which can be too limiting. In the case below the intermolar width was 25 mm. The primary teeth were severely worn and, as in adult tooth wear, is another indicator there could be airway issues. (Figure 2)

Expansion was completed early at age eight before the full eruption of the upper permanent incisors. The final alignment was completed and intermolar width stabilized at 35 mm. Not only was space for eruption achieved, no wear of the permanent incisors is noted. (Figures 3,4,5)


Try expanding the screening of your young patients for potential airway issues, to include palatal width. An improvement in patient health and well-being and reducing risks of tooth wear and future crowding, make it worth the extra step.
Resource
1. Orthodontics and Dentofacial Orthopedics, James L. McNamara Jr. and William L. Bruton
Donna J. Stenberg D.D.S., M.S., P.A. Spear Visiting Faculty and Contributing Author. www.stenbergorthodontics.com
Comments
April 8th, 2015
April 10th, 2015
April 11th, 2015