How to Use an Interdisciplinary Approach for Successful Space Appropriation
By Greggory Kinzer on October 22, 2015 | comments One of the most difficult clinical situations that we encounter is to manage patients that have issues with the mesial-distal positioning of teeth. The process of obtaining the correct spacing of teeth becomes more of a challenge when faced with clinical findings that include multiple missing teeth, retained deciduous teeth, or mal-proportioned teeth.
One of the most difficult clinical situations that we encounter is to manage patients that have issues with the mesial-distal positioning of teeth. The process of obtaining the correct spacing of teeth becomes more of a challenge when faced with clinical findings that include multiple missing teeth, retained deciduous teeth, or mal-proportioned teeth.
Most commonly, these situations cannot be treated by a single clinician. An orthodontist is needed to position teeth to allow for correct tooth proportion and to create room for implant placement; a surgeon is needed to provide any necessary hard/soft tissue augmentation and place the implants. It must be understood that challenges are present when working as part of a team.
Fundamentally, a successful interdisciplinary approach is the need to learn from each other and to share knowledge with each other. To manage patients with complex needs, communication between the intertdisciplinary team is critical.
This article will present information that is important for all the members of the dental team to effectively participate in collaborative treatment.
Determination of appropriate spacing of teeth
The orthodontist plays a key role in helping to determine and establish the correct space requirements for patients with missing teeth or retained deciduous teeth. (Fig. 1, Fig. 2, Fig. 3, Fig. 4)
However, in this example, there is an obvious question that arises: Given the obvious difference in tooth dimensions between the deciduous and permanent teeth, how does the orthodontist know where to position the teeth in order to provide adequate room for replacement of the deciduous teeth?
The most common mistake that orthodontists can make when trying to appropriate space for patients with multiple missing teeth is not obtaining input from their fellow interdisciplinary team members. Therefore, when planning treatment for these patients, it is imperative that the orthodontist be aware of the desired final restorative and surgical objectives.
Often it’s the restorative dentist that actually has the most influence over the desired final tooth position, while the orthodontist educates the team on which tooth movements are biomechanically realistic and when auxiliary implant anchorage may be necessary to achieve those initial restorative and surgical goals.
How is the correct tooth position and spacing decided upon and communicated? The most predictable guide for determining appropriate spacing is to construct an orthodontic set up/diagnostic wax-up. (Click this link to read more about segmenting a full-mouth diagnostic wax-up.) The set up is used to help determine the position of the teeth for optimal esthetics as well as the proper overbite/overjet for development of the lateral and protrusive functional pathways. As was stated earlier, the set up must be completed with input from the treating members of the interdisciplinary team. As it true with any treatment plan, the esthetic position of the incisal edges of the maxillary centrals incisors is the starting point in the starting point in the treatment plan.
The orthodontic set-up/diagnostic wax-up is no different and it must begin by determining the correct esthetic position of the maxillary central incisors relative to the face. (Fig. 5, Fig. 6)
By evaluating the teeth relative to the lips in repose and with a full smile, it is determined that the incisal edges of the maxillary centrals may be slightly long in the patient’s face. Given the existing proportion of these teeth, shortening the incisal edges and increasing the width in the definitive tooth size will enhance their esthetic appearance.
Once the position and shape of the maxillary centrals is determined, diagnostic waxing can be used to determine the correct size and position of the laterals, canines, and premolars. This then will ultimately help determine the position of the natural first molars, which are not in need of restoration. In addition to esthetically positioning the teeth in the diagnostic set-up, the function must also be discussed. Positioning of the lower incisors is based in part on esthetics, as well as function.
Overbite and overjet
How much overbite and overjet should be given to the anterior relationship? Typically the amount of overbite anteriorly is related to the cusp-fossa relationship of the posterior teeth. The deeper the cusp-fossa relationship, the deeper the overbite must be to ensure the disclusion of the posterior teeth. In this patient, the posterior teeth are relatively flat. This means that the anterior relationship can be kept shallower.
The benefit of keeping a more shallow anterior guidance is seen in the force distribution during lateral disclusion. (Click on this link for more on anterior guidance.) Given that we will have maxillary implants guiding our lateral disclusion, we know that for every 10 degrees (plus or minus) in the angle of disclusion, there is a 32 percent increase or decrease in torsional stress at the abutment level.
To help provide some proprioception with lateral disclusion it was decided that the mandibular canines be moved back into a more natural canine position so that the lateral disclusion will not be completely derived by two implants opposing each other. It must be understood that the diagnostic set-up at this point is only an estimate of the anterior/posterior tooth positioning and can only be ideally evaluated in the mouth. (Fig. 7, Fig. 8)
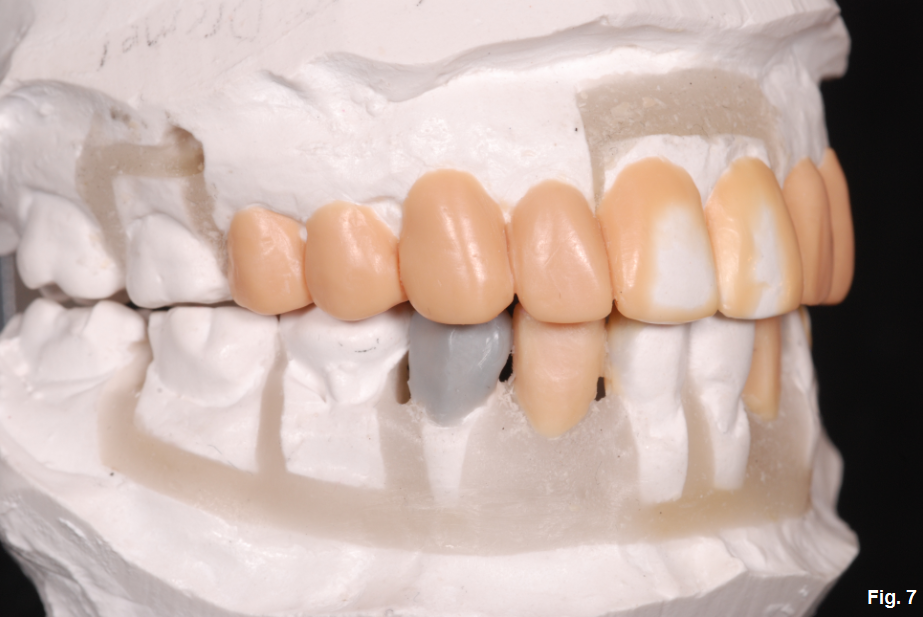
The orthodontic phase
Upon completion of the diagnostic set-up/wax-up, the orthodontic phase of treatment can begin. The difficulty in managing these types of patients often lies in the communication of the new tooth position from the diagnostic work-up back to the mouth. Typically this can be done in a multitude of ways. If the diagnostic work-up was done digitally (ie. if Invisalign were to be used) the communication of tooth position would be accomplished through the trays.
Another option is to correct the tooth size intra-orally by changing the tooth size and shape with composite or by placing provisionals. A third option would be to estimate the correct position of the teeth orthodontically and check/refine the position by taking progress models and performing another diagnostic wax-up. All three methods can be used successfully and often times, more than one option can be utilized in the same patient.
The first surgical phase of treatment consisted of extracting the primary molars, placing two mandibular molar implants, and sinus bone grafting. Provisionalizing the mandibular molar implants after integration will allow them to be used for anchorage to retract the natural canines into the canine position.
The second stage of surgery consisted of placing implants in maxillary canine and first premolar positions. The position of the implants was communicated with the use of a surgical guide that was fabricated utilizing a diagnostic wax-up that was completed on an orthodontic progress model. (Fig. 9, Fig. 10)
Note that implants were not yet placed in the second premolar position, as there was insufficient space given the position of the maxillary molars. Once the canine and first premolar implants were provisionalized, orthodontic brackets could be placed on the provisional in order to distalize the molars and create room for implant placement in the second premolar positions. The third and fourth surgical phases allowed for implant placement in the mandibular anterior and the maxillary second premolar positions. (Fig. 11)
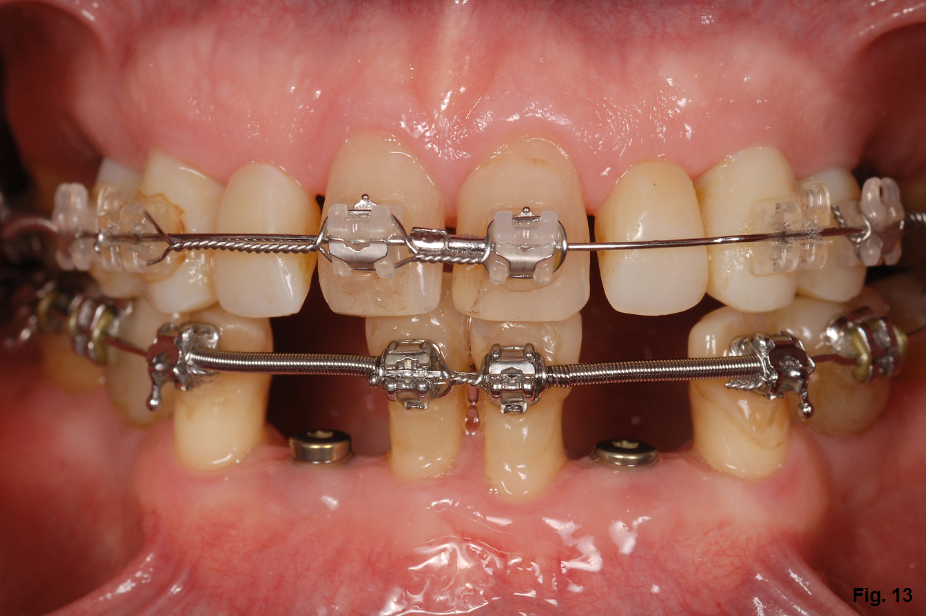
All of the tooth movements and implant positions were determined in general by the initial diagnostic set-up / wax-up. (Fig. 12) Because the diagnostic work-up is only an estimate, fine-tuning the tooth position needs be accommodated along the way using progress models. For example, it appears that the mesial-distal spacing in the mandibular anterior is too large. Refining the tooth forms using composite on the canines and provisionalizing the lateral implants helps assure the correct tooth position as the orthodontics is finalized. (Fig. 13) (Click this link for an article on composite versus ceramic.)
After the completion of the orthodontics, the last teeth to be provisionalized were the maxillary and mandibular central incisors. (Fig. 14, Fig. 15)
In setting up the case in this manner, the final restorative treatment becomes quite predictable, as the appropriate tooth position has been accounted for with all of the pre prosthetic planning. (Fig. 16, Fig. 17, Fig. 18)

(If you enjoyed this article, click this link for more by Dr. Gregg Kinzer.)
Gregg Kinzer, D.D.S., M.S., Spear Faculty and Contributing Author