Anterior Guidance: Always, Never, Sometimes?
The issue of anterior guidance arises when the opportunity to idealize a patient’s occlusion while constructing an expansive restoration involving multiple occlusal contacting surfaces is presented.
What occurs in nature?
- Bilateral canine guidance — 2.3%
- Unilateral canine guidance — 0%
- Bilateral balancing interference — 40%
- Unilateral balancing interference — 60%
Generally, the younger the patient, the more likely they are to have canine guidance. Scaife and Holt examined 1,200 young people and observed that most North Americans under 25 had canine guidance either bilaterally or unilaterally.1
Anterior guidance is often considered a convenience position for restorative dentistry. It’s simply easier to adjust the lateral movements of the canine as opposed to multiple teeth in the quadrant to create and optimize a group function concept with occlusal contacts present in eccentric movements either unilaterally or bilaterally.
Another reason to work with anterior guidance relates to turning off the muscles that create parafunctional wear. Widmalm and Ericsson found that canine plus cross-arch molar contact produced greater activity than cross-arch molar contact alone.2 Williamson and Lundquist found that group contact plus cross-arch molar contact produced greater activity of both masseter muscles.3 O’Leary and his team found that teeth in group-function demonstrated less mobility than teeth in cuspid-protected occlusion.4 And of course, Siebert wrote that canine protected occlusion is a key component in occlusal design to limit tooth mobility.5
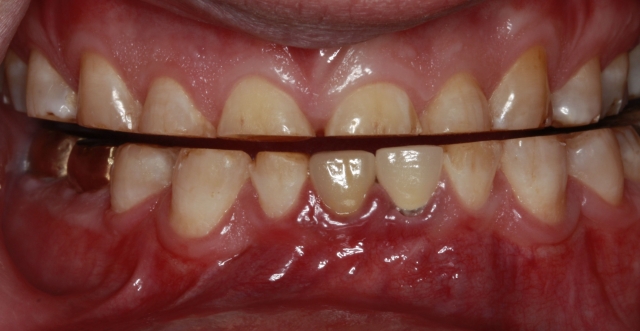
While a balancing contact (unilateral or bilateral) occurs frequently, is this something to mimic when designing the occlusal contacting points? Could it be as simple as describing the findings as pathway wear? With all of the dynamically changing components of the TMJ and the occlusal surfaces of the teeth over time, it makes sense that the teeth wear due to consistent and repeated mandibular movement.
Davies and Gray explain that guidance from any tooth, anterior or posterior, could be defined as anterior guidance. “No matter how far back these teeth are, they are anterior to the temporomandibular joints, so a patient with a severe anterior open bite would still always have anterior guidance of their mandible. It could, for instance, be on the second molars. Therefore, despite the ambiguity of the word ‘anterior’ in the term anterior guidance, it does not mean that the anterior guidance of the mandible is always on the front teeth.”6
A balanced occlusion is routinely discussed in the denture-related occlusal design to promote stability of the removable complete dentures during function. Carlsson includes the balanced occlusion concept in complete dentures as one of the prosthodontic dogmas simply because once food enters the mouth, the desired effect of the balance is gone.7 While creating a balanced occlusion lies at the opposite end of the spectrum from a prosthetic convenience position, when would group function provide an option for our patients?
Group function provides a restorative alternative for patients with concerns related to the canine: significant restorative history, loss of periodontal support for the canine, a canine FPD pontic, or a dental implant-supported canine. Other findings that might lead toward group function occlusal design would include parafunctional bruxism and internal derangement of the TMJ, resulting in pain on working side movements.
References
- Carlsson, G. E. (2009). Critical review of some dogmas in prosthodontics. Journal of Prosthodontic Research, 53(1), 3-10.
- Scaife Jr, R. R., & Holt, J. E. (1969). Natural occurrence of cuspid guidance. The Journal of Prosthetic Dentistry, 22(2), 225-229.
- Widmalm, S. E., & Ericsson, S. G. (1982). Maximal bite force with centric and eccentric load. Journal of Oral Rehabilitation, 9(5), 445-450.
- Williamson, E. H., & Lundquist, D. O. (1983). Anterior guidance: its effect on electromyographic activity of the temporal and masseter muscles. Journal of Prosthetic Dentistry, 49(6), 816-823.
- O’Leary, T. J., Shanley, D. B., & Drake, R. B. (1972). Tooth mobility in cuspid-protected and group-function occlusions. The Journal of Prosthetic Dentistry, 27(1), 21-25.
- Siebert, G., & Siebert, G. (1981). Recent results concerning physiological tooth movement and anterior guidance. Journal of Oral Rehabilitation, 8(6), 479-493.
- Davies, S., & Gray, R. M. J. (2001). What is occlusion?. British Dental Journal, 191(5), 235-245.
SPEAR Membership
Learn Faster. Treat Better.
Whether you have 10 minutes or time to dive deeper, Spear Membership gives you the learning, tools, and support to keep improving.
Choose the level of support and structure that fits your goals.

By: Doug Benting
Date: November 12, 2018
Featured Digest articles
Insights and advice from Spear Faculty and industry experts