- Case Presentation
‘Frank Phrases’: Educate Patients on What Is Possible
[Editor’s note: Want to hear more “Frank phrases” from Dr. Frank Spear himself?
- To hear him talk more about presenting a report of findings, as well as more about the Spear research study discussed in this article, Spear members can check out the online course Case Acceptance in Modern Dental Practice, Part 1.
- Dr. Spear also talks about having the “what is possible?” discussion in the course What Does a Comprehensive Approach to Treatment Planning Look Like?
- And to get a hands-on immersive experience that fully expands on the Spear philosophy of treatment planning, check out our popular campus workshop Treatment Planning With Confidence.]
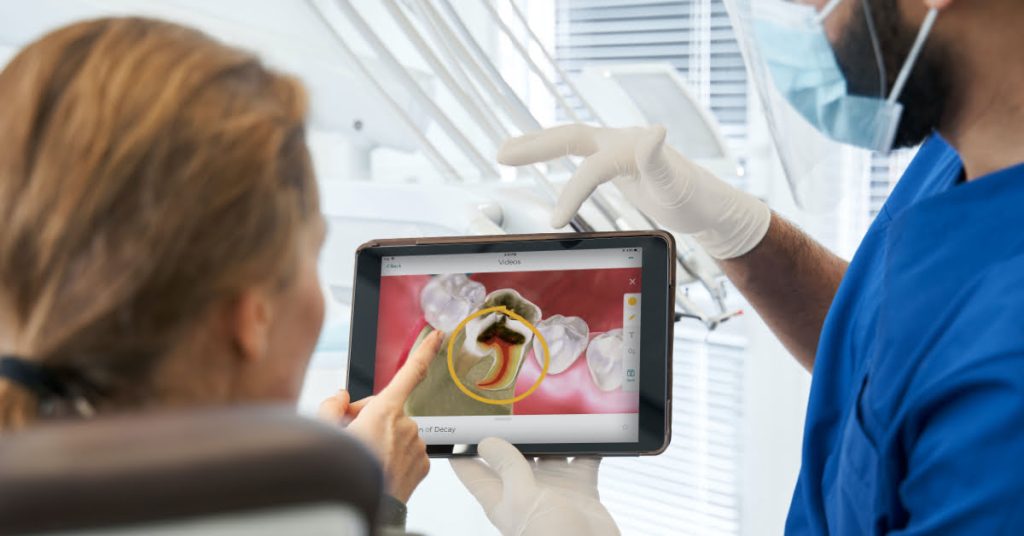
Show them everything
Spear teaches dentists to use a consistent method to record exam findings. The clinician looks at airway, esthetics, function, structure, and biology (AEFSB) to ensure a full picture of the client’s overall oral health is obtained during the exam. Notes are recorded and a complete report of findings should be presented to the patient at the exam’s conclusion.
Presenting all of the findings is crucial because it ensures there will be no surprises for the patient. But why is eliminating surprises so important?
To answer this question, let’s look at some research Spear Education did in 2018, when we analyzed Yelp reviews of dental offices across the country. Through sentiment analysis, we categorized reviews to better understand what makes patients happy or unhappy. We found that 63% of negative reviews alluded to some sort of communication error. Most negative communication reviews had a tendency to begin with the patient being surprised by something, which led to some sort of conversation that left the patient feeling displeased. While you can’t make everyone happy, the more you can do to set expectations helps sidestep huge communication landmines.
This finding aligns with what we saw in Spear’s initial research for our Patient Education videos platform. As part of the platform’s creation, we worked with a medical research firm that brought focus groups together so we could learn how patients would react to the animations we created.
During focus group sessions, we heard several conversations about patients changing clinicians within the previous two years. They described how during their prophy appointments, the doctor found several issues to be addressed but questioned why those same issues were never mentioned at previous appointments.
While this was a small sample size, the patients were consistent when sharing their feelings and their desire to get a second opinion. In each case, the patient ultimately went to the clinician who gave the second opinion, even when the same dental issues were identified.
The insight gained from these two research experiences is to give a patient a complete list of findings. Discussing treatment and moving forward are separate actions, but what we know now is that holding back findings or showing them what you think they can manage (or pay for) will ultimately be harmful to the practice. The key is not to surprise them later, but to build trust by being upfront from the outset, regardless of how long they’ve been with the practice.
Report what’s possible, not just findings
Once a patient is aware of the findings, it’s up to the clinician to move the patient’s mindset to where they’re ready to learn about possibilities. This transition is crucial if a practice wants to increase the average case size in new or existing patients. Beyond the economic value for the practice, it also allows the patient to actively participate in their treatment decision.
Dr. Spear uses a simple phrase to smoothly transition from a “report of findings” to a “what is possible” conversation. While he adapts it slightly based on what the patient is presenting with, he essentially asks, “Would you be interested in learning more about what we can do to correct [condition]?”
It’s a simple but powerful question. First, it removes a power differential as it puts the patient back in charge and makes them responsible for their own treatment. Read my last article to understand how this helps to further counteract the effect of previous case presentations (see Friestad and Wright’s persuasion knowledge model).
Secondly, when the patient agrees to learn more — and most everyone does — it causes their brain to listen to what you have to say. This cognitive dissonance was studied in the 1950s by Leon Festinger. Essentially, when people say (or do) something that they don’t believe in, they create turmoil in the brain called dissonance. Humans then tend to change their beliefs to match their actions to relieve that dissonance.
What does that mean for our patients who agree to learn about possibilities? Essentially, the act of saying “yes” is enough to change or strengthen their beliefs that they really do want to hear more, which results in a more open-minded and interested chairside listener. This doesn’t mean they’ll always move forward with recommended treatment, but it does ensure they’ll truly listen to what you have to say and consider it. This consideration is essential to building a strong practice.
Think about your own time in practice. How many times have you presented something to a patient to no avail, then suddenly years later, the same patient tells you they’re ready to move forward? Most clinicians I’ve spoken with attest that this really happens, but it won’t happen if you don’t show patients your findings and educate them on what’s possible.
SPEAR ONLINE
Team Training to Empower Every Role
Spear Online encourages team alignment with role-specific CE video lessons and other resources that enable office managers, assistants and everyone in your practice to understand how they contribute to better patient care.

By: Adam McWethy
Date: July 13, 2023
Featured Digest articles
Insights and advice from Spear Faculty and industry experts


