Restoring the Edentulous Arch - Are Fixed Hybrids Always the Best Answer?
By John Carson on January 24, 2020 | 4 commentsA recent article about Spear’s “Restoring the Edentulous Arch” workshop highlighted how we have a lot more options beyond the ever-popular fixed hybrid solution known as an “All-on-4,” for those of you working with the Nobel or the DIEM from Zimmer Biomet, or Pro Arch from Straumann.
Have you been wondering why? I mean, why, if fixed hybrids are so popular, would this workshop cover and focus on so many alternatives?
First off, I’ll say that as clinicians, the “Edentulous Arch” workshop instructors understand that fixed hybrids are some of the most advertised and among the most popular options for restoring the edentulous arch. But just because they are popular and heavily advertised does not make them the right choice for every patient.
EDENTULOUS ARCH TRAINING: The two-day “Treating the Terminal Dentition and the Fully Edentulous Patient” seminar provides a thorough, lecture-based introduction to help address a key subset of your restorative practice’s patient base — people who’ve already lost all their teeth, or who will soon be faced with that reality. You can also register for the “Restoring the Edentulous Arch” workshop for an intensive, three-day, lab-based experience.
Before we go any further, let me be clear — there is no doubt that fixed hybrids can be an excellent option for the right cases. One of the most attractive things about them is the fact that they can offer a “fixed” highly functional prosthesis for a lower fee than many of the alternatives.
However, in many cases, there are better options and I’ll even argue that the fixed hybrid is vastly overused simply because many dentists do not understand the alternatives. We must educate ourselves about the potential problems with fixed hybrids and accept the fact that in some cases that lower initial fee that made the fixed hybrid attractive won’t matter if things fail and the result is a poor outcome. As we know, failure of any restoration may also result in a net higher cost, and then things are even worse.
Issues to consider with fixed hybrids include:
Potential excessive bone reduction
In most cases, a lot of bone is going to have to be removed to give you the restorative space you need for a predictable long-lasting hybrid.
Skimp on the reduction and your patient is going to eventually be faced with a broken prosthesis. Take the bone you need and in most cases you will have no ridge left. I understand that no ridge is OK if you’re going to use implants to support a prosthesis, as would be planned in the case of a fixed hybrid. But what if the implants fail?
Simply put, that’s a big issue for at least the amount of time it takes to get some new implants integrated, assuming of course you can get enough implants to integrate to support a prosthesis. If you can’t you and your patient will be faced with the fact you now have a terrible ridge (in many cases no ridge). So now even a conventional denture is not going to work well. Seriously, think about how bad this would be to deal with.
The prosthesis could break
Let’s say the prosthesis breaks and needs to be repaired. In most cases this means it is going to have to be removed from the patient's mouth, which means they are going to have to come in and you are going to have to find time in your schedule to remove the prosthesis.
Then once repaired you and your patient will have to find time again to put it back in.
Cumbersome cleaning
Last and certainly not least is that fixed hybrids used in less-than-ideal situations can be very difficult if not impossible to clean.
While this can occur in either arch, it is especially common in the maxilla since they need to make tight contact with the tissue for proper speech.
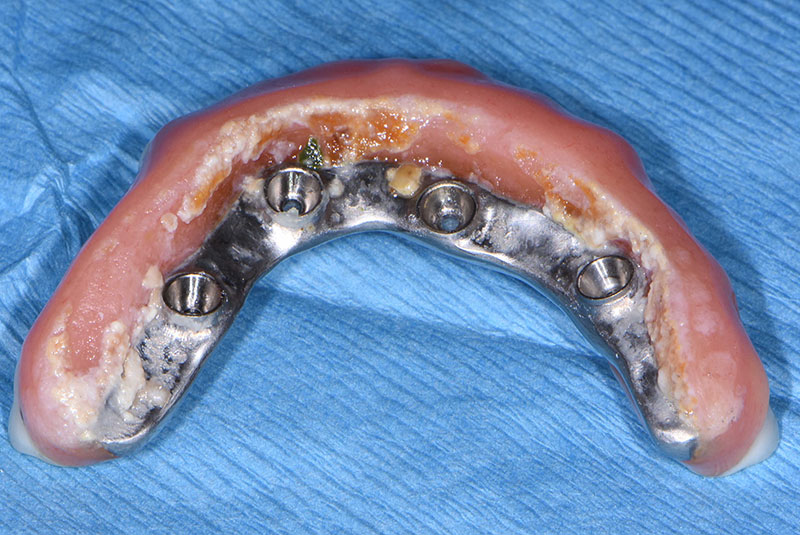

It’s important to remember that if your patient can’t clean it the risk of peri-implantitis is high, particularly if your patient has shown any susceptibility to periodontal disease. We all know once implants develop peri-implantitis it is very difficult to manage and if we lose the implants we will likely be in the situation discussed above: having a patient who has a terrible ridge for a conventional denture and will have to wear one for at least the time it takes to get new implants integrated. If you can’t get new implants to integrate then you and your patient are stuck with that terrible denture forever.
If you’re thinking you’ll just take it off every six months and clean it in the office, realize that will likely not be enough if your patient is indeed susceptible to peri-implantitis and they can’t clean the prosthesis at home, since we know periodontal pathogens establish themselves in 21 days.
Think about that. Tell me a single patient that is going to want to come in to have their hybrid cleaned every 21 days if they can’t do it themselves at home. Next, think about the feasibility of doing that every 21 days in your office even if your patient was willing to do so.
Cautions and considerations with fixed hybrids
While I may be coming across as fixed hybrid “hater,” I must say that is not the case. I consider using fixed hybrids, but only in the right cases.
I think fixed hybrids are great if they are made so the patient can clean them at home. But I also think in many cases there are far superior options.
As a general rule, some of my favorite options — and there are too many to cover here in-depth, which is why the “Edentulous Arch” workshop is days long — are those that are implant-supported but removable by the patient, which eases cleaning at home.
Another great benefit of the patient removable options is if they have a backup prosthesis (such as their initial interim prosthesis) they can swap the definitive prothesis for the backup and simply drop their definitive prothesis off for repair if needed. I really can’t stress how great it is for the patient to be able to swap things out themselves. This makes things way easier for them but also for you.
Envision a patient with a broken fixed hybrid prosthesis. Say they broke a front tooth out of their fixed hybrid. They are going to be disappointed, even if they can get in to have you fix it quickly.
Now envision that front tooth is out and they can’t get in to see before a social event they have been looking forward to. That’s going to be way worse. It surely will not be a practice-builder for you, and at best you are going to have a frustrated patient.
Now think about the same scenario but consider if you could simply swap the definitive prosthesis for their interim prosthesis. That would be pretty nice for you and it will leave your patient feeling more comfortable with the situation as well.
John R. Carson, D.D.S., is a member of Spear Visiting Faculty and a contributor to Spear Digest.
Comments
February 3rd, 2020
February 3rd, 2020
February 7th, 2020
February 9th, 2020