Intrinsic Dental Erosion: Causes and Diagnosis
Dental erosion is caused by sustained contact between tooth surfaces and acidic substances. The demineralization of dental enamel will occur once the oral environmental pH reaches the critical threshold of 5.5, when it can be inherently classified as either “extrinsic” or “intrinsic.”
Intrinsic dental erosion, also known as perimolysis, is the process whereby gastric acid from the stomach comes into contact with the teeth. This is often secondary to conditions such as gastro esophageal reflux disease (GERD) or the eating disorder Bulimia Nervosa. Numerous scientific studies have shown that the prevalence of GERD in the U.S. adult population could be as high as 40%.
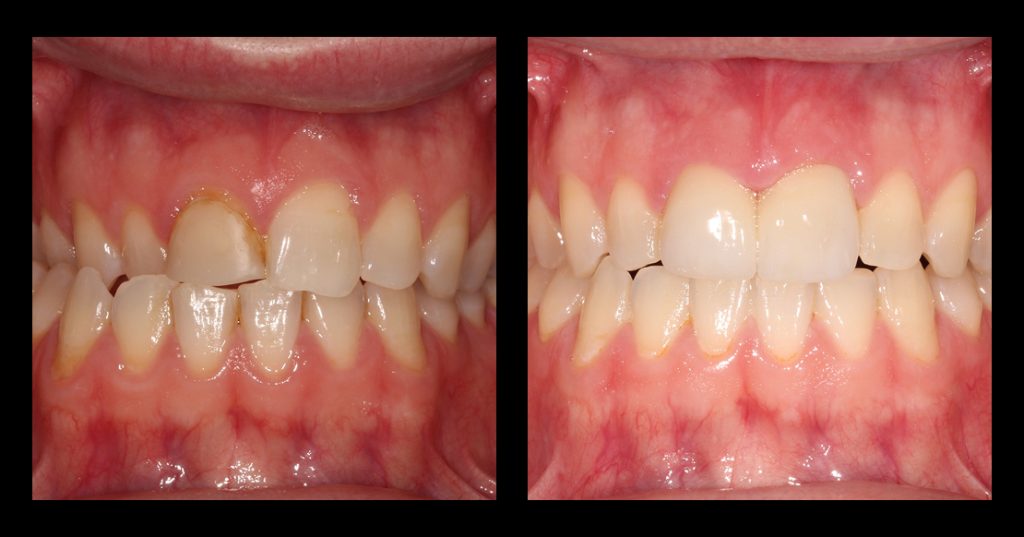
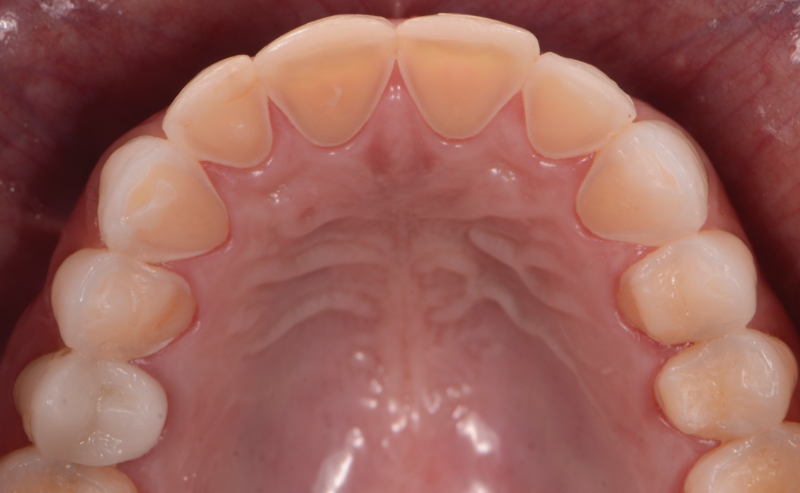
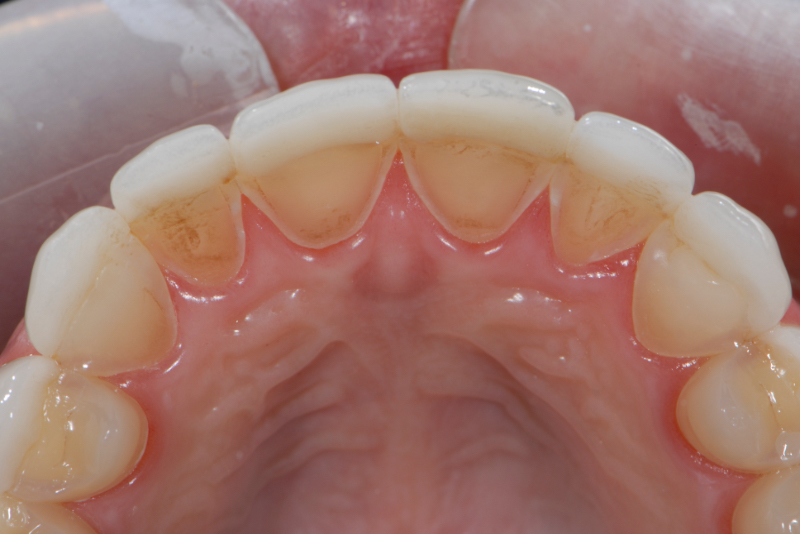
Self-induced vomiting increases the risk of dental erosion by a factor of 5.5 compared to healthy controls. These intrinsic erosion lesions are most commonly found on the palatal surfaces of the maxillary teeth, followed by the occlusal and then the buccal surfaces (Figs. 1–5).
While dental erosion in bulimic patients is most likely associated with oral retention of regurgitated gastric contents, dietary habits of bulimic patients may also include bingeing on high-energy foods and foods with high erosive potential, which may further exacerbate erosion.
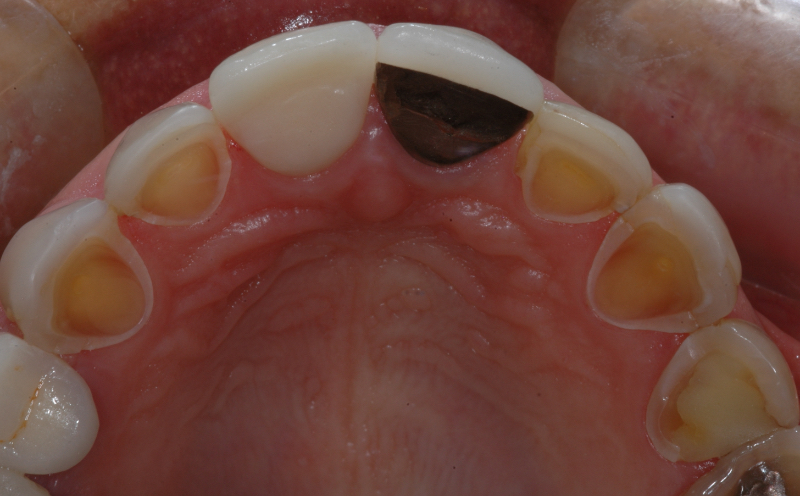
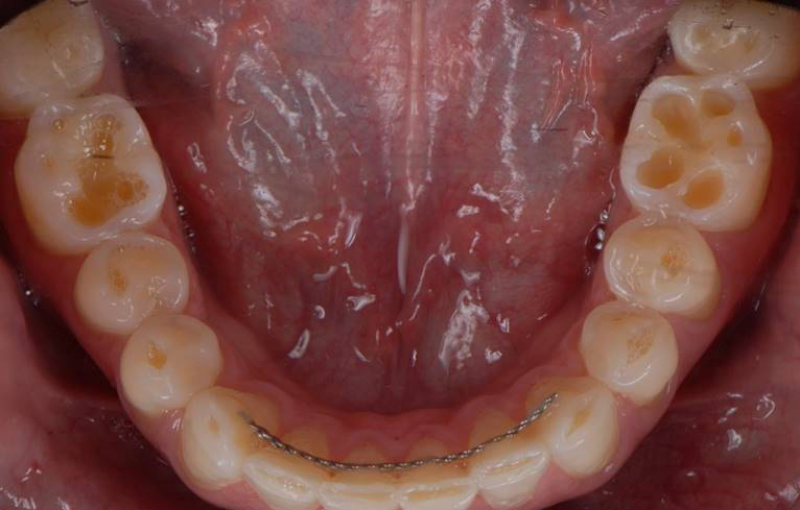
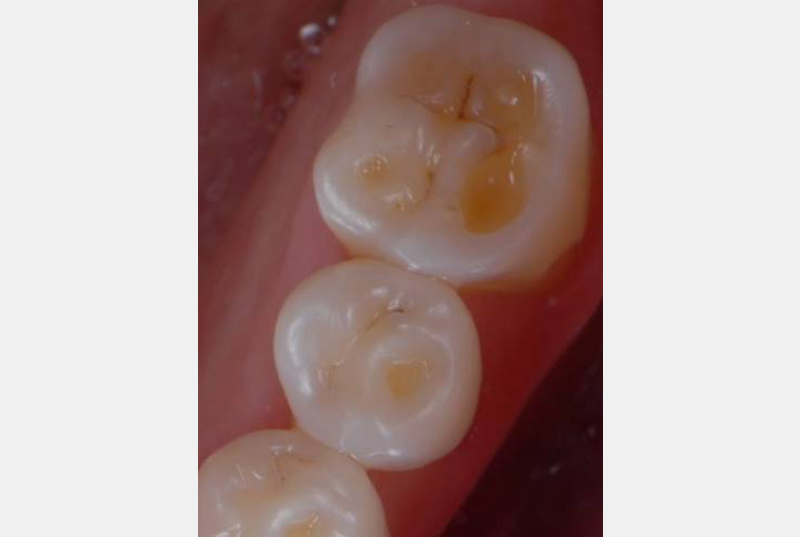
While the leading cause of GERD is increased acid production by the stomach, this is not exclusive to adults, since GERD and other gastrointestinal disorders may also cause dental erosions in children. Interestingly, while this condition is well known in the medical community, some hospital websites still fail to mention dental findings as part of the diagnosis. This is particularly important when we understand that “Silent GERD,” or the complete absence of awareness of signs and symptoms, occurs as often as 80% of the time.
Now this becomes quite serious since GERD can chronically irritate the esophagus and result in a condition known as Barrett’s esophagus. Now it is well described in medical literature that there is a significant correlation between Barrett’s esophagus and cancer. Barrett’s is considered a precursor of esophageal adenocarcinoma, also known as EAC.
The human body has a buffering capacity with saliva to counteract the negative actions of acid. When acidic substances enter the mouth, salivary glands increase secretion, and saliva flow accelerates to clear the acids from the mouth. Since human saliva contains bicarbonates and urea, it rapidly neutralizes the acidic remnants and returns the oral pH to normal.
Many factors affect saliva flow rate and buffering capacity, including autoimmune diseases (Sjögren’s syndrome), medications (antidepressants and antipsychotics), and aging. When saliva flow rate is reduced, its clearance and buffering capacity will be impacted, resulting in abnormal acid retention in the mouth, which, in turn, may contribute to dental erosion.
Describing clinical conditions to the patient is one of the most important steps during treatment. At my practice in Mexico City, we use Spear’s Patient Education videos consistently with great success to achieve better communication and understanding.
The dental erosion video (Fig. 6) is a one-minute, narrated animation using lay terms to define the condition and explain its leading causes.
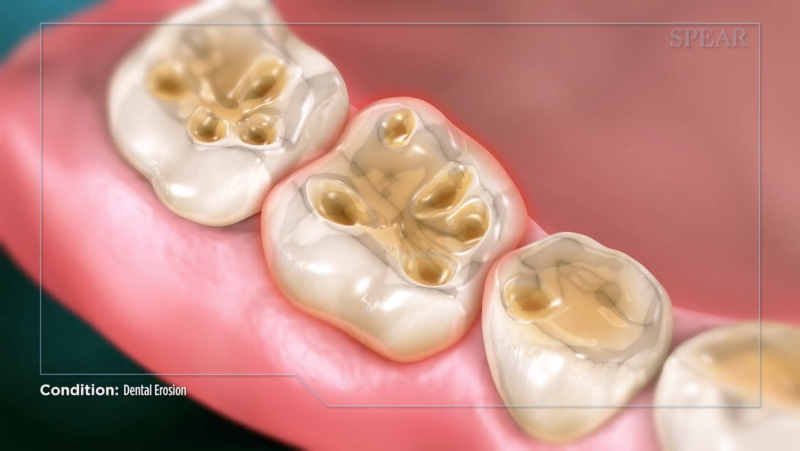
After the video is played during the consultation appointment, we go through some valuable screening questions that we may use that can lead to a diagnosis:
- Do you often get heartburn?
- If so, how often do you get heartburn?
- Do you have a bad taste in your mouth or sour breath on an ongoing basis?
- Do you need to sleep with your head elevated to avoid painful burning in your throat or chest?
- Do you notice that food or drink “comes back up” easily after eating or drinking?
Any affirmative answers merit a referral to a physician, especially if there are dental signs as well.
One additional procedure we usually use to increase patients’ awareness is to show a still image from the Patient Education video alongside a photograph of the patient’s clinical condition. This truly helps them visualize and further understand the need for therapy and the harmful potential consequences of inaction.
References
- El Aidi, H., Bronkhorst, E. M., & Truin, G. J. (2008). A longitudinal study of tooth erosion in adolescents. Journal of Dental Research, 87(8), 731-735.
- Lussi, A., & Carvalho, T. S. (2014). Erosive tooth wear: a multifactorial condition of growing concern and increasing knowledge.
- Schlueter, N., Jaeggi, T., & Lussi, A. (2012). Is dental erosion really a problem?. Advances in Dental Research, 24(2), 68-71.
SPEAR Membership
Learn Faster. Treat Better.
Whether you have 10 minutes or time to dive deeper, Spear Membership gives you the learning, tools, and support to keep improving.
Choose the level of support and structure that fits your goals.

By: Ricardo Mitrani
Date: December 30, 2019
Featured Digest articles
Insights and advice from Spear Faculty and industry experts