Radiographs and Cement: You Can’t Handle the Truth!
Do you take radiographs to check for cement and document fit after you seat restorations? If you’re like me, the answer is yes.
If you’re not, I encourage you to start doing them on at least your implant restorations so you’ll have documentation of bone levels at the time of seating. In the case of cement-retained implant crowns, doing this provides an extra check for any residual cement you may have left behind.
This is especially great when dealing with implants, because we know leaving any residual cement around them can have disastrous effects, so any extra check is great. But what I want to caution you on in this article is the fact that our radiographs don’t tell the whole story. They are lousy at showing things — especially cement — on the buccal and lingual.
Yes, we have all heard a million times that our radiographs don’t tell the whole story, but let me share an example that occurred in my office, as I think it shows really well how severely our X-rays lie! (Honestly, I can’t say how shocked I was, and I’m a bit hesitant to share this, as it’s kind of unbelievable.)
The story starts with a patient who had been referred to me for restoration of an implant in the position of #10. By the time the patient was referred to me, the implant was already in and the surgeon had done an immediate provisional, as you see here:
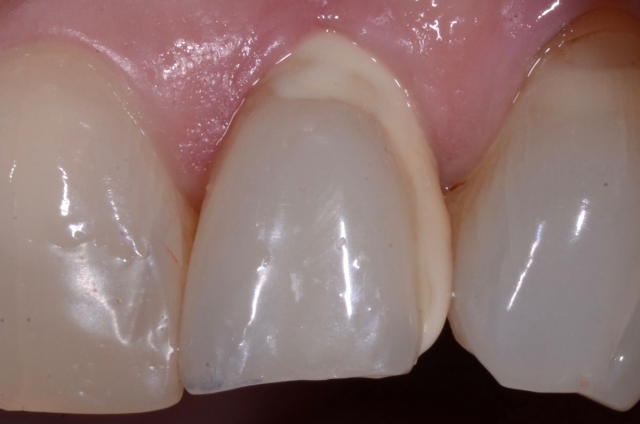
So after completing our comprehensive exam and establishing a clear picture of what the patient wanted to attain with her treatment, we made plans to restore the implant. The implant provisional was removed, records were taken and the implant provisional was put back on.
The fun started when the patient broke the provisional when biting a sandwich while the case was at the lab. When she presented, the only thing left in her mouth was a temporary implant abutment post. Of course, we made her a new one and sent her on her way.
Lo and behold, when she returned for delivery, the temporary abutment post was the only thing left again, but this time she had decided to just stick wax on the post and leave it be.
Obviously, the problem with this was that the tissue was a mess. Despite this, we decided to go ahead with delivery and see how things went, knowing that if the tissue was too tender or we had concerns about delivering the case, we could and would abort delivery and go back into yet another provisional.
The temporary abutment post was removed and the area irrigated and cleaned. As we delivered the case, everything went great— the abutment dropped right in, as did the crown, and the patient had zero sensitivity, not even a hint of gingival sensitivity (which was contrary to what we expected, given how angry the tissue was and the fact that she was not anesthetized).
Given we were positive that both the abutment and crown were perfectly seated, we decided a radiograph of the abutment seated prior to cementation of the crown was not needed.
The surprise came when we took our final radiograph:
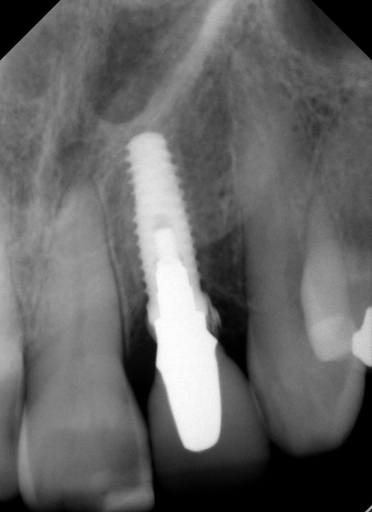
We couldn’t believe what we saw! How on earth did I leave such a large piece of cement? I mean, seriously, I was using RMGI cement that is easy to clean up, and we had done a custom abutment, so the margins were super accessible. We went after the debris and felt like we got some out, but honestly not as much as we expected, so we took another radiograph to see how we were doing. Here’s what we saw:
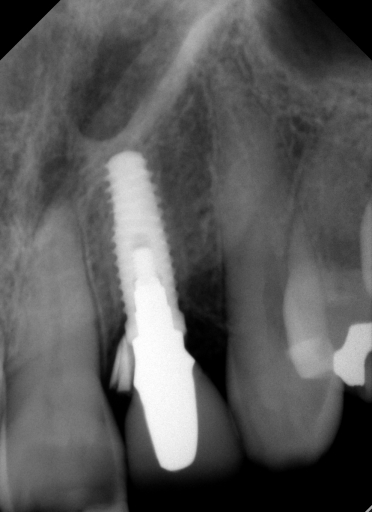
We were saying, “What’s going on? How did this piece move from one side to the other and not come out?” It was clear we needed to remove the restoration so we could better visualize things; needless to say, this was super disappointing.
So we drilled a hole in the lingual of the crown, accessed the screw and removed the abutment and crown as a single unit, converting the restoration to what I like to call a “screwmented restoration.” When we took out the abutment and crown and examined the interface between the crown and abutment, we confirmed that we had indeed removed all the cement.
While this is great, this meant we had missed something else! What we had been seeing was part — or should I say parts — of the provisional that had broken. These are the pieces we found:

The crazy part is that we had looked (and yes, I am not blind) for anything like this before delivery … but the tissue was so inflamed and the pieces were so embedded that we literally could not see them.
The crazier part is that these pieces had not fallen or been rinsed out before delivery. As if that wasn’t enough, the craziest part is that you’d think the patient would have been really uncomfortable with these pieces in the tissue when we placed the abutment and crown.
As you can see, the radiographs really never told the whole story! What had been happening was there was one big fragment in the shape of a ring that was rotating around the implant as we attempted to remove it. In addition to the large ring, there were also some small fragments. All these pieces were so embedded that we actually had to take several radiographs as we removed them, since we wanted to be 100% sure we got them all.
It was really shocking to take a new radiograph and see we still had more as we worked. Frankly, I was so shocked that if I didn’t see it with my own eyes, I would be saying, “Well, that guy must be blind or not looking.” I promise, I really was looking and my eyes do work! It was really just that crazy. I know it seems unbelievable and, like I said, I really had second thoughts about sharing this, because I get that folks could easily be saying, “Seriously?! How could you miss that?”
But honestly, the only way anyone would have seen it sooner would have been to take a radiograph sooner. I ‘m sharing this story because it illustrates just how limited our radiographs really are. Sure, they show us mesial and distal pretty well, but they’re lousy at telling us about the buccal and lingual. Yes, we all know this, but this case is a great illustration to remind us just how limited they are!
The good news is we identified that we had a problem and headed it off before it got worse. As we know, had we not caught this when we did, we could have had serious damage to the hard and soft tissues in the area, and we could have easily been headed for a disastrous long-term outcome.
If you’re wondering how it all turned out, I’m happy to report that we were we able to redeliver the restoration as a screw-retained restoration and avoid a remake, which made both us and the patient very happy.
What would I do differently if I had to do this over again? Of course I would have taken a radiograph prior to cementation, but the kicker is that I had no reason to think I needed to for the reasons mentioned above.
The bottom line is that radiographs are a great tool, but never forget that they only tell some of the story, and just when you think you’ve seen it all … you’re wrong!
SPEAR campus
Hands-On Learning in Spear Workshops
With enhanced safety and sterilization measures in place, the Spear Campus is now reopened for hands-on clinical CE workshops. As you consider a trip to Scottsdale, please visit our campus page for more details, including information on instructors, CE curricula and dates that will work for your schedule.

By: John Carson
Date: December 29, 2017
Featured Digest articles
Insights and advice from Spear Faculty and industry experts


