Dental Treatment Planning: You Only See What You Know
By Dave St. Ledger on August 15, 2016 | commentsIn the first two parts of this three-part series (click the links for Part I and Part II), we discussed caries detection clinically and radiographically, and some newer and older (tried and true) methods through technology of caries detection and cracks.
With all of the technology at our fingertips, and with all of the hours in chair time amassed, experience certainly mounts through all that is encountered. But do we always understand what we are looking at, and are we seeing it with intention? It is not as easy as it sounds.
Truly staying in the moment, focusing on the clues before you, requires a level of attention and dedication that is difficult to obtain without a supreme commitment to furthering one’s education. I did not know this until I started my journey into advanced dental education in the early 2000s. And it hit me like a ton of bricks, with the swift words of the incomparable Dr. Henry Tanner (for more on Dr. Tanner click here), spoken by the finest conduit to deliver, the equally incomparable Dr. Gary DeWood:
“You only see what you know, you only treat what you see. What do you see?”
It was July of 2004 at an institute far, far away in South Florida, and Gary continued to pepper us in a lecture with:
“You only see what you know, you only treat what you see. What do you see?”
“You only see what you know, you only treat what you see. What do you see?”
Slide after slide, on and on and on. There was a point to this, and that point was that, although we were taught from dental school to look at each tooth and plan treatment by order of units and surfaces, we should instead stop, step back, and look at the patient comprehensively. We need to relate what we are looking at to everything else we are looking at:
- Marginal ridge cracks
- Abfractions/NCCLS
- Troughed or V-shaped second molars
- Mucogingival defects on a single tooth
- Short looking teeth; no room for materials
- Cupped appearance of certain teeth
- Patterns of caries; surfaces and styles
For all of us at some point in our careers, we are looking at things but not necessarily seeing them. We aren’t seeing their meaning and their relationship to each tooth or even a systemic condition. The above are just some of the many observations we make every day without understanding when, why and how these conditions developed. Subsequently, we may quickly act like dentists and want to fix what is seen before we know the when, the why, and the how. In our attempt to help – because all we want to do is help and fix – we place a restoration that may become compromised and fail sooner, leaving questions and concerns for both the patient and the practitioner.
Between Gary’s eloquent oration and the visual PowerPoint candy before me, I entered the realm of realization that I did not know what I did not know. Not knowing what I did not know was a concern. Hopefully it concerns you as well. That is the purpose of this article.
“You only see what you know, you only treat what you see. What do you see?”
Let that marinate for a while.
You only see what you know – All that you have learned to this point and attempted to apply
You only treat what you see – Most of dentistry; react and treat on what you report; itemize them and deliver care per unit and as needed
What do you see? – Here lies the challenge; this is where the last of this three-part question asks us to disseminate all of the information. With all that is in front of us, do things make sense, are they clear, and can you correlate the data and deliver your findings? If it has crystallized and makes sense, then you are seeing with intention. If it is confusing to you, as it often was and still can be for yours truly, then you are not alone. It is daunting to sift through and make sense of extra- and intraoral data without a system or a better understanding of the etiologies of tooth wear, susceptibility to caries, periodontal disease and systemic health.
Come along and look at these photos and examples of some conditions and ask yourself:
What do you see?
Example I


Do you see what parafunctional wear can do to a dentition? But do you see what chronic use of a segmental appliance can do to collapse a dentition? The combination of the two in this case creates significant interdisciplinary treatment challenges.
Example II
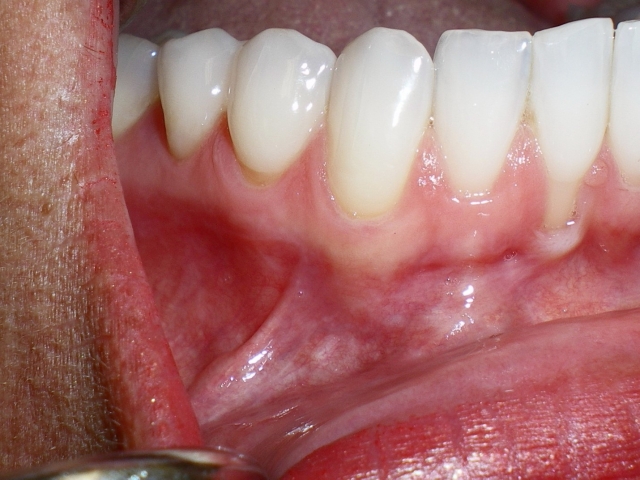
Do you see the labial defect on #25? Some see that and often think the cause is periodontal disease from bacteria or the patient brushing too hard. It has been offered that way, and that can happen. But if you attempt to repair with grafting of some sort, and not see the other clues, the graft may fail and the patient may be disheartened.

Go back to Figure 3 photo. Do you see the slanted incisal edge of #25? Now come back and look at Figure 4 just after grafting. Do you see the incisal edges of #8 and #9 and how they correlate with the incisal edge of #25? That angled wear is crossover wear and highly contributory to that labial tissue defect that did not exist until the patient decided to stop wearing her occlusal appliance indefinitely. This graft could not be successful without orthodontics. Her teeth are beautiful, but there are plenty of subtleties that suggest they no longer handle loading very well. She went through ortho treatment …

And after about two years, Figure 5 is the result. Providing her more stable contacts when her mandible moves made the difference.
Example III

Do you see things like this come into your practice? One tooth alone in a quadrant with so much more work than any other, but for a small bonding on #31. Why did #30 have RCT and a crown? Do you see the wear through the occlusal but not much elsewhere? What do you see when you look up? Next slide …

You see something similar, crowns on the opposing, but not much else in the quadrant. She states that the temporary (#3) has not felt right since it was done and wanted another opinion. This area is unique in the patient’s mouth. As a dentist, you so want to help. Do you see something is different here? But do you see the value in gathering data before picking up a handpiece: mounted study models, centric and protrusive bite records, and photographs? Fast forward: These were the areas of initial points of contact in centric relation.
Example IV


Here, there is too much to see and sort. Where do you even begin? For the sake of the two patients in these photos, specifically their systemic health, being up to date on trends in the industry is critical. The wear is obvious, but the etiology may be the trick. Do you see erosive wear and the pathway wear? The literature shows that pathway wear, along with signs of acid erosion in the mouth, which may be suggestive of GERD, may also suggest the possibility of obstructive sleep apnea.
When signs like this present, regardless of a patient’s restorative desire, always consider a discussion of a sleep study. If he or she exhibits with clues like weight challenges, a narrow airway, hypertension, diabetes, high cholesterol, fatigue, to name a few, you may be saving them from something far worse than a worn dentition.
Example V
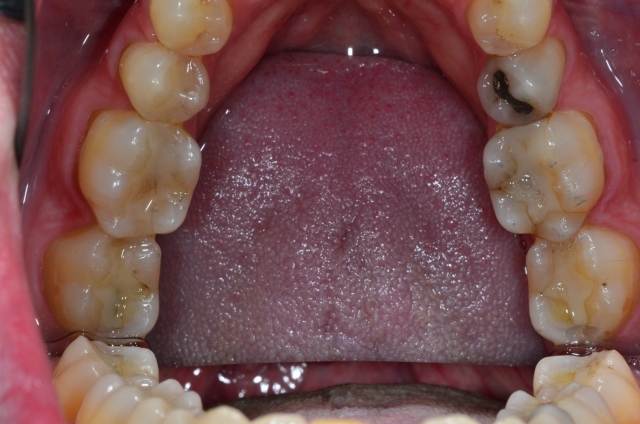

Do you see anything different on Figure 10? This patient has no complaints, a beautiful smile and cannot understand why bothering with mounted models may assist him in future tooth issues. Figure 11 shows those beautiful teeth. That first image shows trouble. Do you see the troughed out second molars? Do you appreciate that level of retrusive/centric relation wear?
The patient’s mandible postures downward and forward and grinds when he seats his own condyles. These teeth already touch in MIP. If left untreated, it continues. Where will the restorative room be? Sometimes equilibration may be appropriate here. If CO and MIP become one, the condyles are seated and the patient can retrude no further.
Example VI



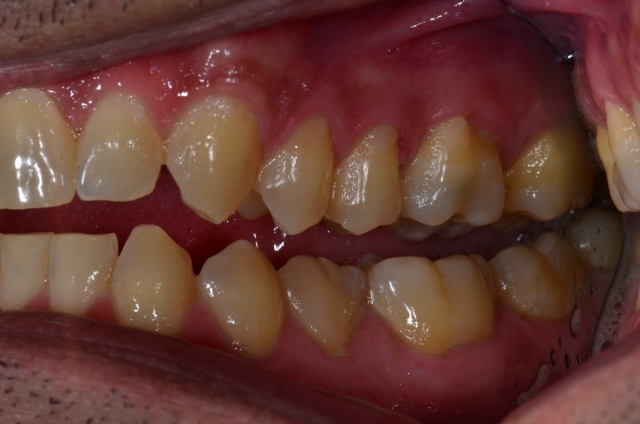

Do you see this patient with flat incisors, end to end wear, and his desire to make his smile look less square? He sees the lowers are flatter and smaller and wants them bonded. Do you see his teeth couple in MIP/ICP? There is no room for material. Do you see what happened? Did he lose VDO? Do you see the clues?
A look at the posterior teeth shows nice looking teeth that look like teeth. So if VDO has not changed, then what happened? Do you see the gingival levels of the lower anteriors positioned more incisally than the posteriors? They have super-erupted secondary to the incisal wear. The lower occlusal plane is stepped. He plays with his teeth in the front, but nowhere else. To do the least amount of work, you can offer intruding the lower anterior to add composite and position the cuspids better for improved canine guidance (he has lateral excursive wear and as the cuspids shorten, the posterior teeth will start to bump into each other).
Dental CE: Learn more, see more
I intentionally selected these types of examples because these were exactly the situations I would not know what to do with or where to start. I would not think globally but tooth to tooth, because as a young dentist it was all I knew from my education. All of the “do you see” questions in the six cases were asked of you because my answer used to be, “No.” So I decided long ago to expand upon the “you only see what you know” part of what Henry Tanner was stating. I wanted to be able to treat more of what I was able to “see.”
It is impossible to know all that there is to know. I mentioned in Part II of this series with caries detection that formal dental education – dental school – really is just a small percentage of one’s education. It may be rather difficult and confusing to learn piecemeal by attending seminar after seminar, fulfilling continuing education requirements, without a definitive outline for a definitive outcome. The beauty in attending advanced institutes for dental education lies in the structure within their curriculum. Core building blocks give way to pathways for development, how they tie together, and the immediate effect of hands on workshops. The personal relationships you develop and the camaraderie you feel yields the safest of learning environments. This same opportunity exists for you. I hope you come and join us at Spear Education. Thank for your time in reading this series. I hope it was useful.
(Click this link for more dentistry articles by Dr. David St. Ledger.)
David St. Ledger, DDS, Visiting Faculty, Spear Moderator, Contributing Author