As a young dentist when I first started hearing about condylar position, I was wondering if we were talking about dentistry or something related to the Kama sutra. Not knowing much about either subject, I decided it best to pursue an understanding of the foundational components related to functional stability in dentistry.
This topic has been the subject of massive food fights in dentistry, bordering on tribal warfare between the Centric Relation advocates, the Neuro-muscular camp, the Behavioralists and, of course, traditional Gnathology. Some representatives of these philosophies at one time or another seem to claim some proprietary knowledge; however, as time painfully teaches, "No one is right if everybody else is wrong."
Optimal condylar position
So the question becomes what is an optimal condylar position? Or maybe a better question is what is the health of the condyle disc assembly as a foundation for the restorative process? Does it really matter? And subsequently, what risk am I facing in the restorative process relative to that state of stability or instability?
The obvious answer to those questions lies in the findings we get from our comprehensive evaluation. Too often assessment of the TMJ is based on an anecdotal complaint by the patient about pain or discomfort rather than a routine commitment by the practitioner to assess the health of the stomatognathic system on a regular basis. We don't limit our routine assessment of periodontal or other disease on this basis, so why should we for other structural components of the system?
Read more about comprehensive dental care in action.
In subsequent articles in this series, I'll talk a little bit more about specific instances that demonstrate the utilization of a variety of condylar positions, but perhaps nowhere is this more important than the orthodontic treatment of the adolescent as illustrated by this case.
Case Study
This bright young lady is a college student in our community and is from a rural area of Kansas. She was referred to me and stated that she was done with her braces and was ready to get her implants placed where she was missing her lateral incisors. She said she heard we were really good and asked for our help.

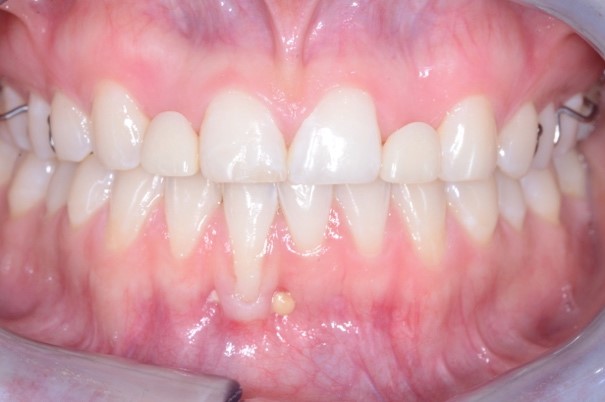
It won't take you long looking at this photograph to identify myriad complexities associated with this case. We could go into great detail about the divergent roots of the centrals, tooth size and proportion, soft tissue challenges, and the like; however, the most significant challenge to me was foundational.
The dehiscence at the facial root of number 25 tells the story of over-advancement of the lower incisors in order to correct an apparent angle Class II occlusion. However, during the discovery phase of the examination, we found in translation, after a loud bilateral pop, both articular disks reduced leaving her with an end-to-end occlusion anteriorly and a posterior open bite as shown on the mounted casts.


Incidentally because the discs still had a fairly substantive posterior band (evidenced by the loud pop), she could maintain the reduction clinically without guidance. Again you can see this position on the study casts.
Additionally, if you look at the fully seated joint position (FSJP) in this photo, you see initial posterior contact with open anteriors before she slides in her maximum intercuspal position (MIP).


So now what? Well, unfortunately, I can't tell you how this turned out because as diplomatic and non-judgemental as I tried to be I had to point this out to her parents. After an initial pleasant interaction with the orthodontist, as soon as I raised the joint issue I found myself under the bus in this treatment loop as her mother explained to me that her orthodontist found someone who “agreed with his treatment.”
Read about managing the second opinion.
As we teach at Spear Education, all I can do is report my observations and the implications of that evaluation; the patient had to make decisions from there. The real tragedy here is that she will likely get implants placed and they may be just added to an already precarious clinical situation. Think about what might have been? Had the previous clinicians identified the condition and position of the articular discs, it is likely that they would have found that the Class II relationship was the result of the displaced discs and, in a reduced disc position, the case might have indeed been a Class I.
My heart still breaks over this case, and it's my hope that someone will address all of the issues that could compromise the success of the implants. Most important, however, is her long-term oral health. I wasn't willing to prescribe implant fixture placement into an anterior tooth arrangement I didn't consider appropriate, and I maintain considerable concern for her TMJ stability in the future.
Condylar position? You bet it's important!
James “Jim” Otten, D.D.S., Spear Visiting Faculty and Contributing Author
Read more dental articles by Dr. James Otten.