Esthetics
Condylar Inclination? I'm Just Restoring the Front Teeth...
By Kevin Kwiecien on June 16, 2014 | 5 comments
Most of us are doing diagnostic wax-ups before restoring front teeth – we might even be using the wax-up to make a stent for our provisional restorations, which is a great way to test-drive our permanent restorations and make sure we like them. (Fig. 1-2)

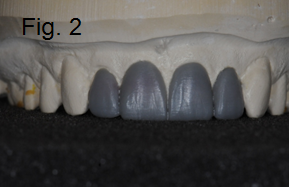
If nothing else, this is a great way to identify any esthetic or functional issues before we place the permanent restorations. (Fig. 3)
Even if the wax-up is done on an un-mounted model or a simple hinge articulator, we have at least visualized a desired end-point before we prep, right?
If we are restoring the guiding teeth, usually and hopefully the anterior sextant, would you be open to the possibility that they might be affected by the back teeth – especially if one or two of the back teeth are pretending to be guiding teeth? (Fig. 4-5)
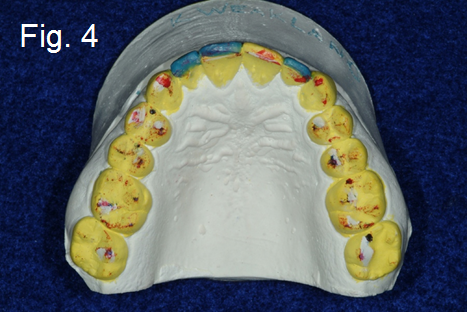
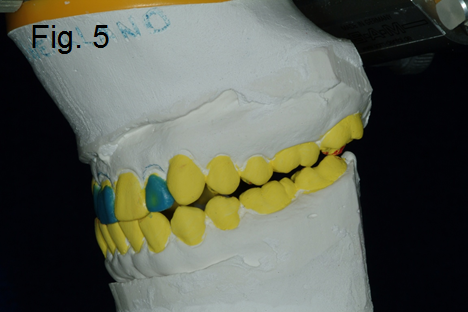
If a back tooth bumps while the front tooth is trying to do its job, also known as excursive interference, it directly affects what is happening to our beautiful restoration in the front.
The condylar inclination represents the angle, steep vs. shallow, of the condyle translating down the condylar eminence as the mandible moves left, right and protrusive. The steeper the angle, the more quickly the back teeth come apart. The more shallow the angle, the slower the back teeth will disclude. Taking a few minutes to set the condylar inclination on the articulator will help clear up two possible issues:
1. Back teeth are bumping/guiding when the front teeth should be (condylar inclination set steeper on the articulator than it is on our patient).When we miss this, the front teeth will not be touching when we assume they would be. This could result in many signs or symptoms including muscle tenderness, soreness of the interfering molar, a broken cusp of the interfering molar, mobility of the interfering molar and/or your beautiful new restoration clunking down on the lower incisors after it moves past the posterior interference. (Fig. 6)
 2. Lingual of upper front teeth designed steeper than necessary (condylar inclination set shallower on the articulator than it is on our patient). When we miss this, it appears that the back teeth are interfering on the articulator when in reality, they are discluding much more easily. This could result in designing a steeper restoration than needed, tender muscles, sore joints or chipped edges on your beautiful new restoration. You might also be planning to re-contour some back teeth that don't really need it.
2. Lingual of upper front teeth designed steeper than necessary (condylar inclination set shallower on the articulator than it is on our patient). When we miss this, it appears that the back teeth are interfering on the articulator when in reality, they are discluding much more easily. This could result in designing a steeper restoration than needed, tender muscles, sore joints or chipped edges on your beautiful new restoration. You might also be planning to re-contour some back teeth that don't really need it.
Certainly, there is more to this conversation but I thought it might be helpful to create some curiosity here and hopefully create some clarity about what you might be seeing clinically.


If nothing else, this is a great way to identify any esthetic or functional issues before we place the permanent restorations. (Fig. 3)

Even if the wax-up is done on an un-mounted model or a simple hinge articulator, we have at least visualized a desired end-point before we prep, right?
If we are restoring the guiding teeth, usually and hopefully the anterior sextant, would you be open to the possibility that they might be affected by the back teeth – especially if one or two of the back teeth are pretending to be guiding teeth? (Fig. 4-5)


If a back tooth bumps while the front tooth is trying to do its job, also known as excursive interference, it directly affects what is happening to our beautiful restoration in the front.
The condylar inclination represents the angle, steep vs. shallow, of the condyle translating down the condylar eminence as the mandible moves left, right and protrusive. The steeper the angle, the more quickly the back teeth come apart. The more shallow the angle, the slower the back teeth will disclude. Taking a few minutes to set the condylar inclination on the articulator will help clear up two possible issues:
1. Back teeth are bumping/guiding when the front teeth should be (condylar inclination set steeper on the articulator than it is on our patient).When we miss this, the front teeth will not be touching when we assume they would be. This could result in many signs or symptoms including muscle tenderness, soreness of the interfering molar, a broken cusp of the interfering molar, mobility of the interfering molar and/or your beautiful new restoration clunking down on the lower incisors after it moves past the posterior interference. (Fig. 6)
 2. Lingual of upper front teeth designed steeper than necessary (condylar inclination set shallower on the articulator than it is on our patient). When we miss this, it appears that the back teeth are interfering on the articulator when in reality, they are discluding much more easily. This could result in designing a steeper restoration than needed, tender muscles, sore joints or chipped edges on your beautiful new restoration. You might also be planning to re-contour some back teeth that don't really need it.
2. Lingual of upper front teeth designed steeper than necessary (condylar inclination set shallower on the articulator than it is on our patient). When we miss this, it appears that the back teeth are interfering on the articulator when in reality, they are discluding much more easily. This could result in designing a steeper restoration than needed, tender muscles, sore joints or chipped edges on your beautiful new restoration. You might also be planning to re-contour some back teeth that don't really need it.Certainly, there is more to this conversation but I thought it might be helpful to create some curiosity here and hopefully create some clarity about what you might be seeing clinically.
Comments
June 16th, 2014
June 17th, 2014
June 18th, 2014
June 20th, 2014
July 31st, 2014