8 Steps for the Esthetic ‘Emergency’ Anterior Composite
Big or small. Class III or IV. Incisal edge with or without the mesial or distal corner.
A systematic approach that makes sense and is easy to reproduce and trust for every anterior composite will decrease anxiety, increase the fun, and increase your confidence. But what if you and your patient actually see the value in taking a closer look at what caused the break (Fig. 1)?
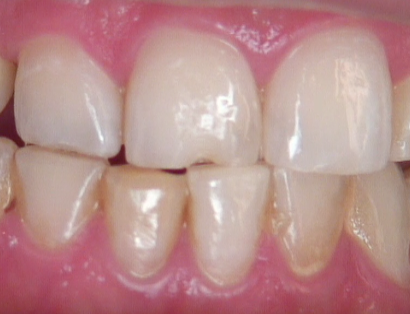
And what if you both want to avoid putting it back into the situation that caused it in the first place? But what if you don’t have time because your patient has an important meeting coming up later that day? Sound familiar?
Consistently incorporating these eight simple steps will allow you to actually look forward to these situations, as opposed to putting a kink in your day.
1. Putty stent (or alternative)
Use whatever model you have in the office to create a putty stent. It might even be an old printed model from fabricating a night guard (that was originally made to at least protect the teeth at nighttime and during exercise — shocker, right?!) while waiting to do a comprehensive evaluation (Fig. 2). Including the incisal edge will save time and increase the predictability (Fig. 3).
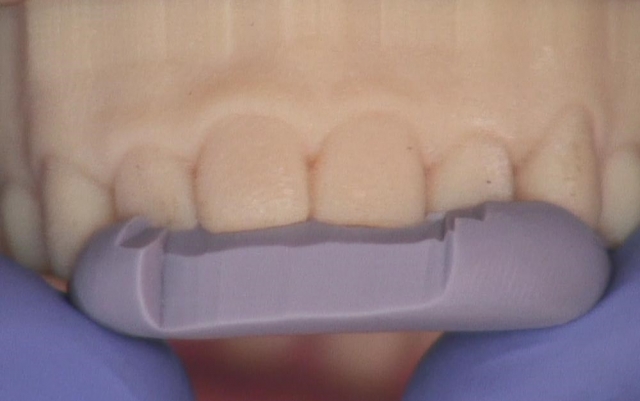
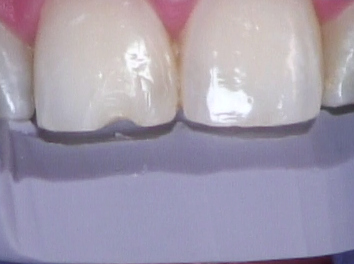
If you don’t have an old model hanging around, maybe your finger holding a piece of Mylar when creating the lingual wall will be the “stent.” Regardless, identifying the source of a stent and knowing you’re going to use it is the first step. An old model and some putty can very quickly be used for the greatest predictability.
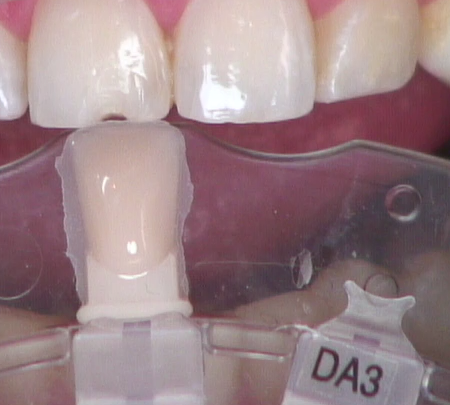
2. Dentin and enamel shade
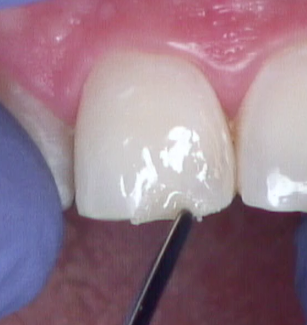
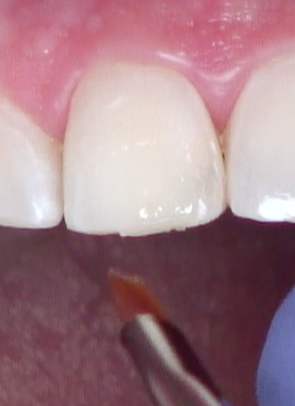
Before desiccating, or even drying, the tooth, identify the proper shade of the enamel using the tooth to be restored and the adjacent tooth (Fig. 4). Use the broken or chipped tooth to identify the dentin shade (Fig. 5).
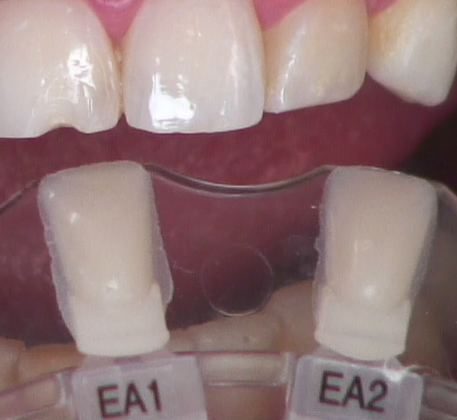
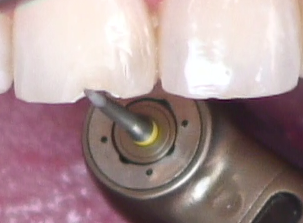
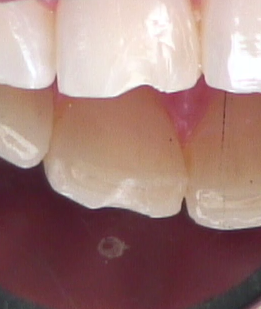
3. Create a distinct lingual margin
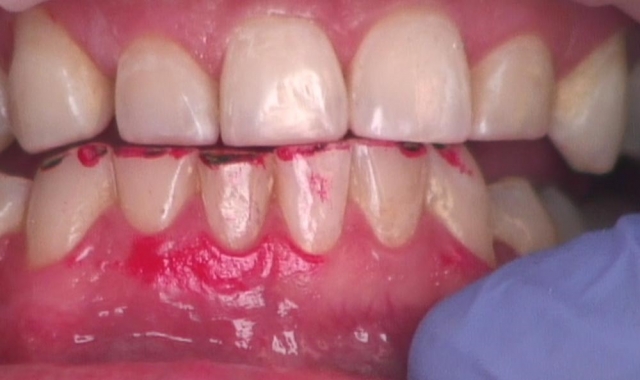
Remember, there’s no reason to blend the lingual margin for esthetics. You would rather see it clearly avoiding unsupported enamel and facilitating easy removal of excess composite and subsequent evaluation of the margin, as opposed to being the proud creator of an “invisible margin” that you and your hygienist will see every six months, and very clearly when the flashing starts to stain (Figs. 6 and 7).
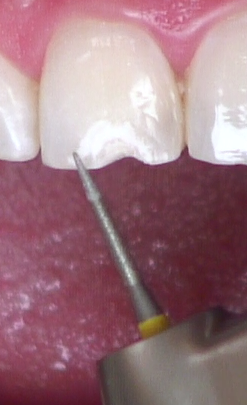
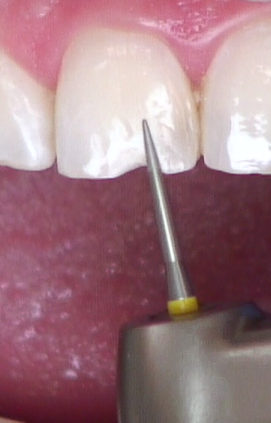
Step 4: Create an irregular and long bevel on the facial
Begin the bevel from the deepest part of the broken tooth/preparation (Figs. 8 and 9). Imagine a swimming pool transitioning from the deep end to the shallow end. It’s hard to see any distinct transitions, right? Compare that to the ocean, where there’s a quick and dramatic drop-off from shallow to deep. Which will be easier to hide and blend? It’s more than just a long bevel in enamel. It’s a slowly transitioning bevel from deep to shallow.
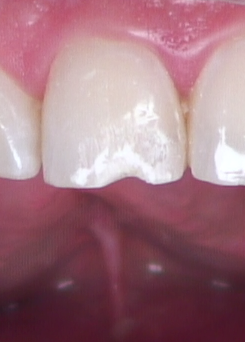
Intentionally create some irregularities of different shapes and lengths on the superficial enamel beyond the edges of the original “long bevel” (Fig. 10). Irregular patterns or scratches of different shallow depths, combined with the long bevel, will hide the edges of any composite, even if the shade is not perfect. Try it. You’ll see! How do you think I know?
5. Create the lingual wall
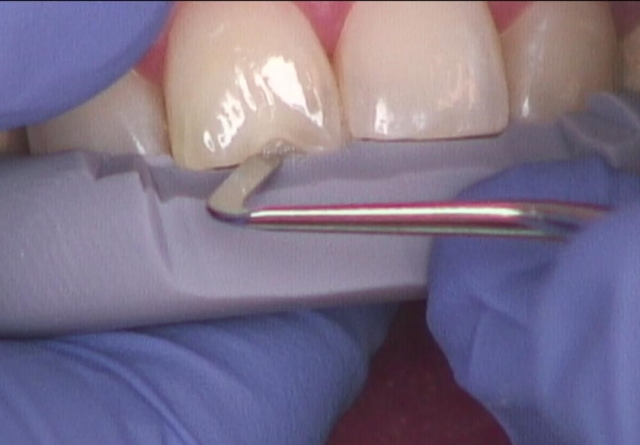
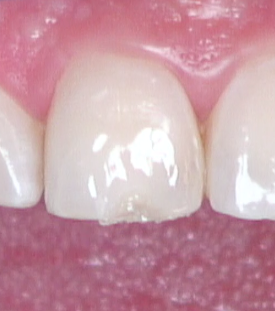
Use the putty (or a Mylar strip with your finger behind it) to replace the enamel lingual wall (Fig. 11). By using the putty matrix, you can predictably create the incisal edge position, leaving room to place deep discoloration, translucency, hypocalcification, or halo. The wall should be thin, creating space to build out the necessary layers of dentin and facial enamel in the next step (Fig. 12).
6. Replace only what’s missing
Matching dentin layer
The dentin layer should replace only where the dentin was. By leaving the lingual wall thin, there is space to create irregular depths of dentin and mamelons. Most importantly, the edges of the dentin shade composite should be almost imperceptible to differentiate from the natural tooth, especially after curing (Fig. 13). Remember, the enamel is translucent, so don’t expect it to mask any underlying irregularities. If you don’t like the look or color at this point, don’t place the enamel layer. Change the dentin shade or blend the “bottom of the transitioning pool” a little more before moving on.
Enamel layer
The enamel layer should replace only the thickness of the missing or broken enamel. When applied intentionally and smoothed with a brush, you can confidently avoid bulking up the enamel just so you can remove half of it with a bur two minutes later. Feels a little counterproductive to me. Just sayin’ …
7. Identify primary anatomy
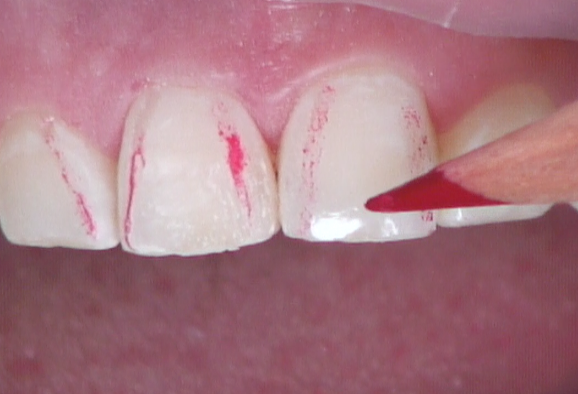
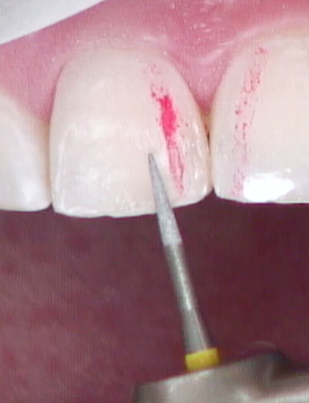
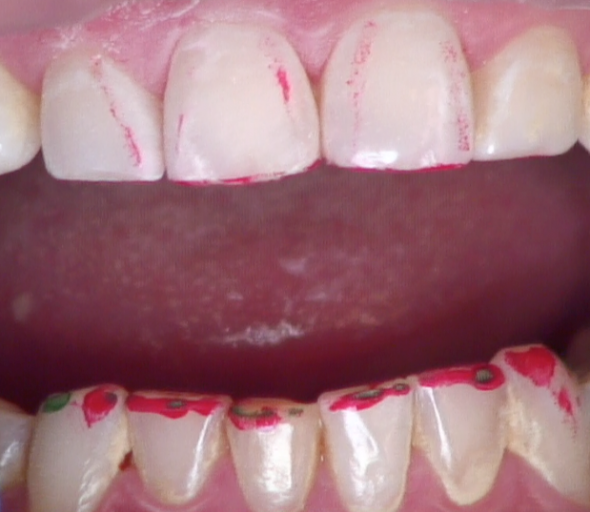
Even teeth with subtle shade differences look good at speaking distance if they actually look like teeth. You can take 30 seconds to use the flat side of a “sterile pencil” to expose all heights of contour on the restored tooth and the adjacent tooth (Fig. 15). By identifying the primary line angles, convexities, concavities and embrasure distances, you can quickly identify what changes are needed (Fig. 16). Those changes are now made with intention, increasing efficiency and confidence.
8. Create smooth and broad
Because you haven’t yet comprehensively evaluated the esthetics or occlusion, or identified predictable steps to restore the situation that caused the the broken tooth in the first place, what can be done to help the patient make it until that time? You don’t want to make any big changes at this point, right? But you can do some very slight recontouring of enamel edges to create two very smooth surfaces and create a broad surface area so when the patient does move to the position we think was a contributing factor, the odds of a similar fate are dramatically decreased (Fig. 18).
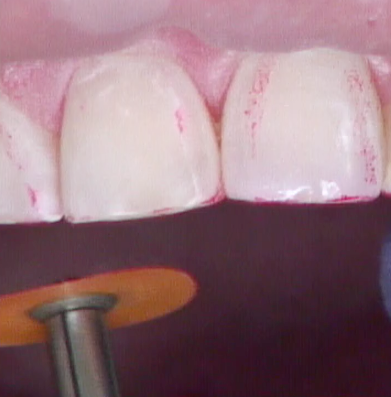
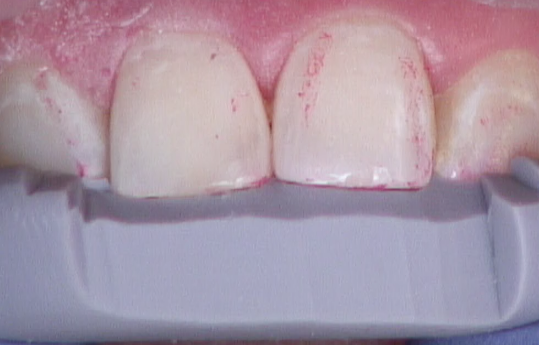
At this point, you can do the final polishing of those edges, as well as the rest of the restoration, intentionally preserving the primary anatomy created and appreciating the depth of color and flow also intentionally created in the restoration (Fig. 19). You also should not be surprised that the tooth fits right back into the stent that was used to create it all (Fig. 20).
Many dentists think that fabricating and using a stent is just for the “big cases.” Many of the same dentists think there’s no reason to layer the composite and routinely use one shade.
However, these eight steps are not just for the big cases. Every case is a big case, right? And the more we create predictable systems in our offices for procedures like this, the more we trust it and enjoy it. That is my hope for you.
SPEAR campus
Hands-On Learning in Spear Workshops
With enhanced safety and sterilization measures in place, the Spear Campus is now reopened for hands-on clinical CE workshops. As you consider a trip to Scottsdale, please visit our campus page for more details, including information on instructors, CE curricula and dates that will work for your schedule.

By: Kevin Kwiecien
Date: March 16, 2017
Featured Digest articles
Insights and advice from Spear Faculty and industry experts


