Become a Better Client With The Lab Check-In Checklist
By Gary DeWood on July 30, 2015 | comments The use of checklists is a proven strategy to reduce errors and increase predictability. This strategy propelled mobile surgical clinics in Africa and Asia to better morbidity and mortality scores than the top US hospitals [1,2,3].
The use of checklists is a proven strategy to reduce errors and increase predictability. This strategy propelled mobile surgical clinics in Africa and Asia to better morbidity and mortality scores than the top US hospitals [1,2,3].
Also, since the early crashes of the B-17 during testing led to the creation of checklists for pilots, no other B-17 crashed other than in combat for five decades [3].
Using the checklist process when restorations return from the lab will catch issues before the patient is in the chair.
Our practice had one assistant assigned to lab communication. It was her responsibility to review the Case Checklist, pack and ship all cases, and then check-in all returning cases from the lab using the Lab Check-In Checklist. Any scores other than OK were immediately directed to the attention of Dr. Cheryl DeWood or me for disposition.
This effort saved us many frustrations and innumerable rescheduled seat appointments. The lab was often able to manage whatever issue(s) we discovered prior to the patient’s appointment. If that was not possible we still had adequate time to get the schedule altered so that the doctors could use their time efficiently. There is not much worse than that sinking feeling in your stomach when you pull out the restoration, try it on the die model, and realize this is not going to be a good day – all with an expectant patient sitting numb in the chair. It’s just like being on one of those early B-17s before the checklist, only you can feel it longer.

Here are the things we checked. You will note that not all of the things are the responsibility of the laboratory. An evaluation of the materials and information provided to your technician is an appropriate and valuable step for improving what you send. At the end of that long prep appointment your judgement is usually less “crisp” that it can be when things return from the lab.
Additionally, you can now see what your lab was able to create from what you sent and judge the adequacy of those items and instructions in getting back what you hoped for. We discovered that the increased communication created by the use of the Check-In Checklist made us a better client and our lab a better lab.
- Model work
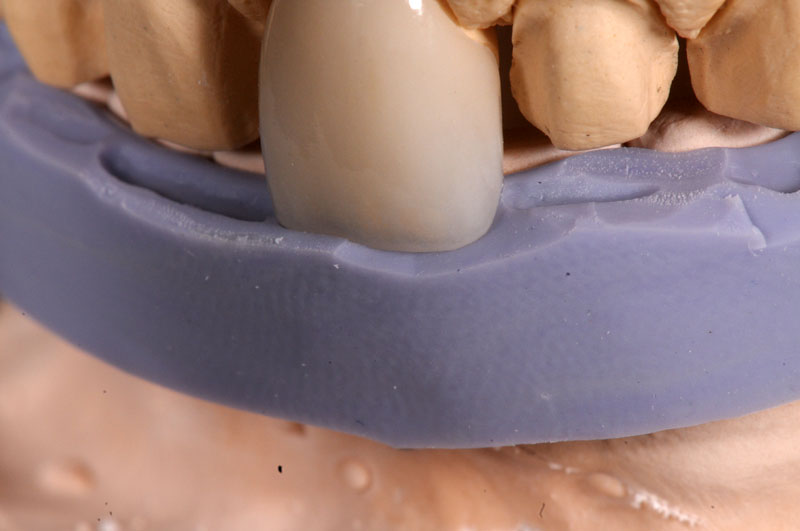
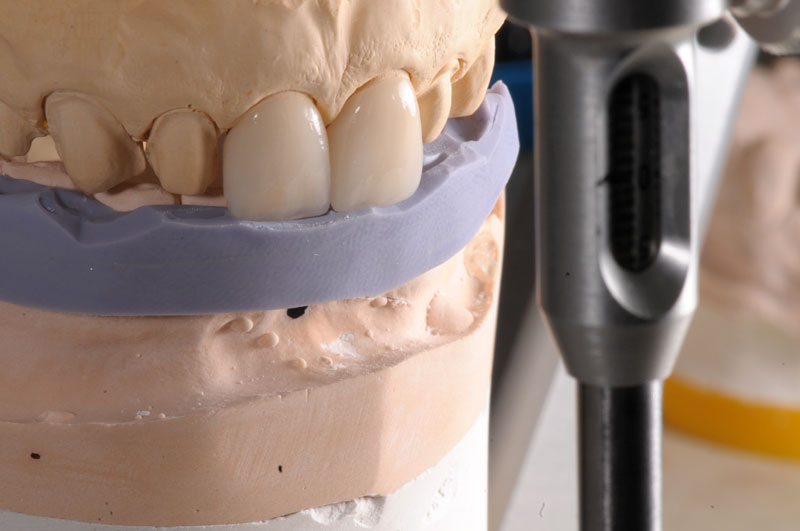
- Marginal fit on the die model
- Marginal fit on the solid model
- Adaptation to the edge guide
- Occlusal anatomy
- Axial contours
- Embrasures
- Pontic design
- Proximal contacts
- Centric stops
- Pathway Guidance
- Cross-Over and edges
- Incisal edge and bevels
- Shape/Texture/Luster
- Translucency
- Value
- Shade characterization
- Bite registration
- Opposing model
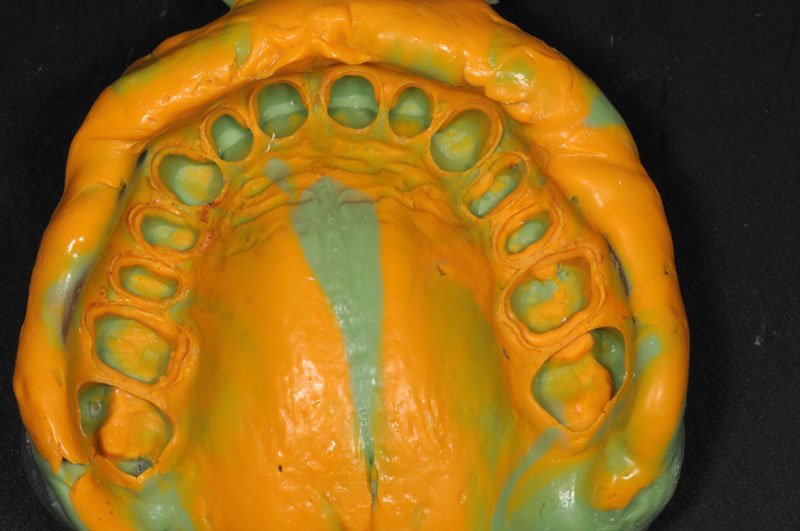
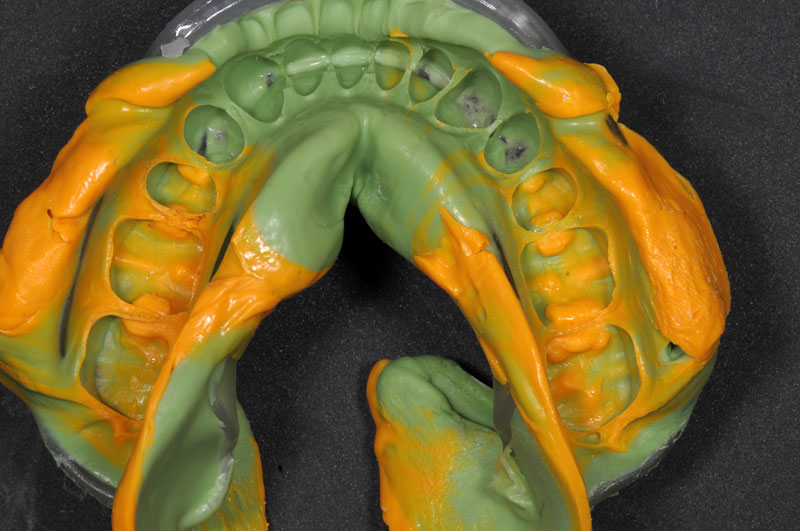
- Impression
- Preparation
- Go-By model
- Imaging sent with case
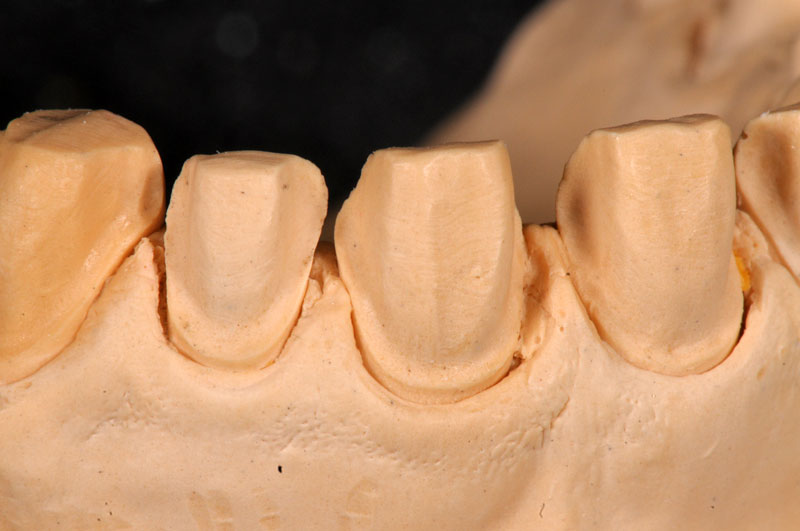
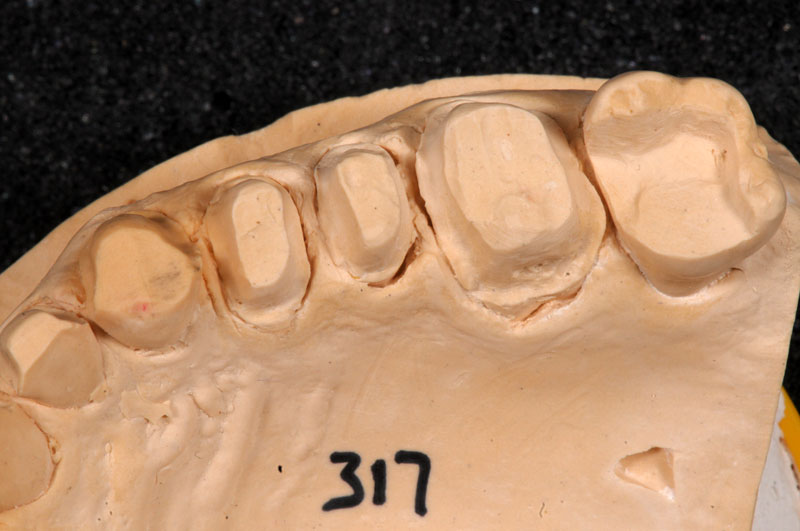

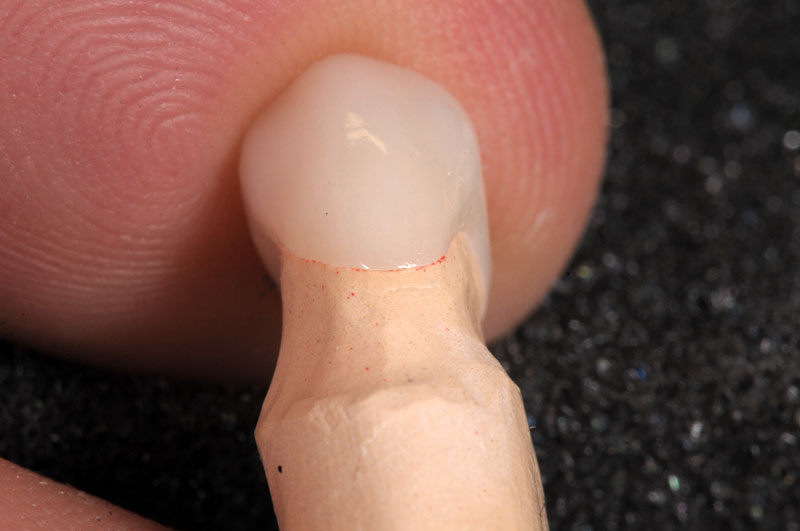
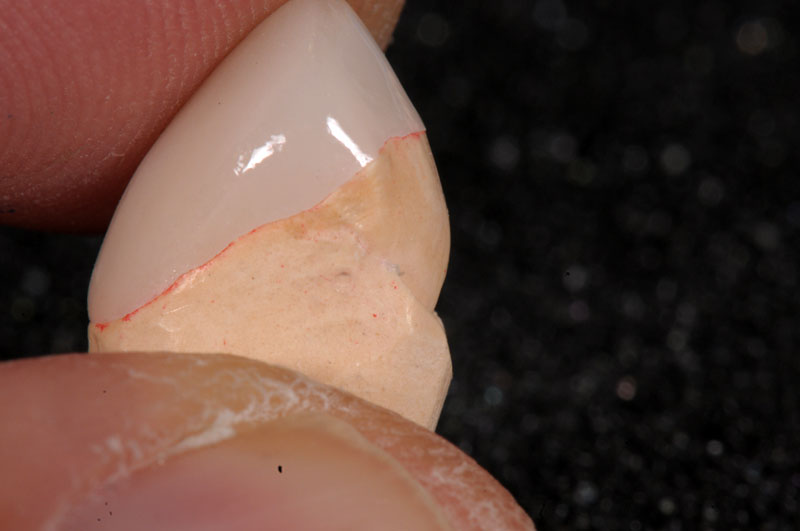
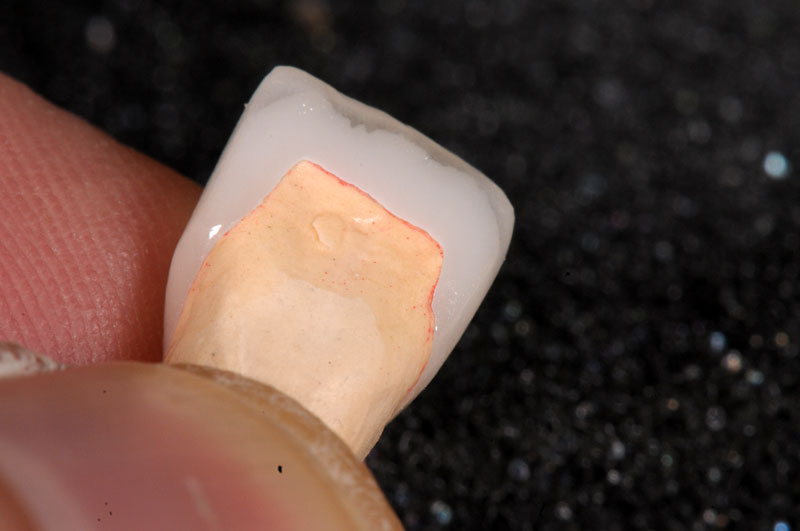
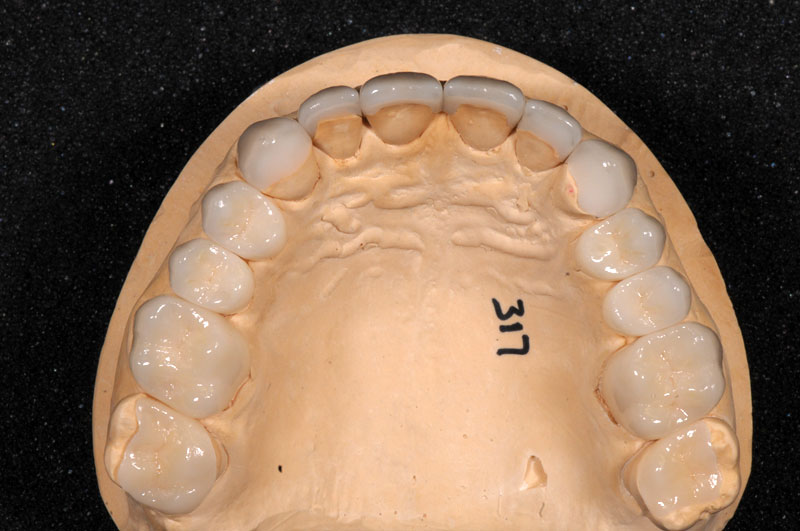
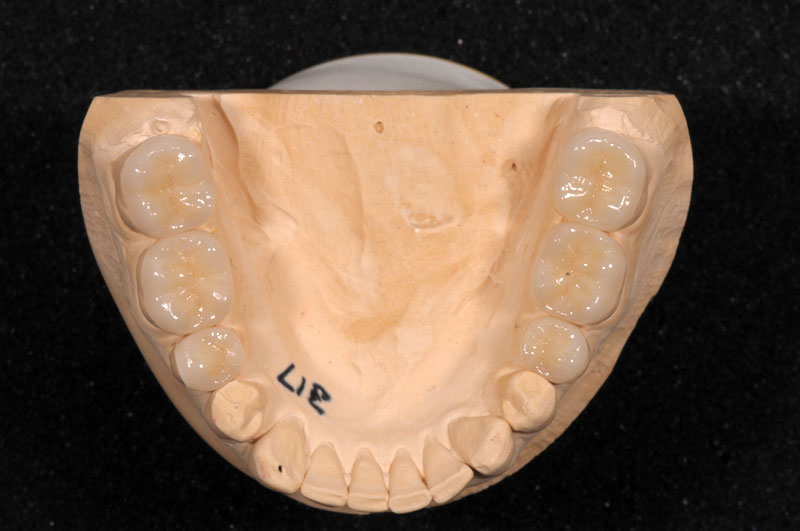
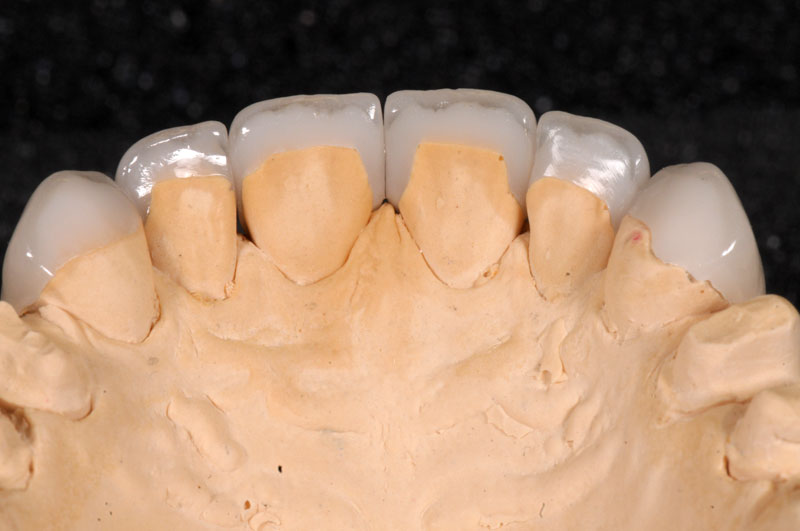
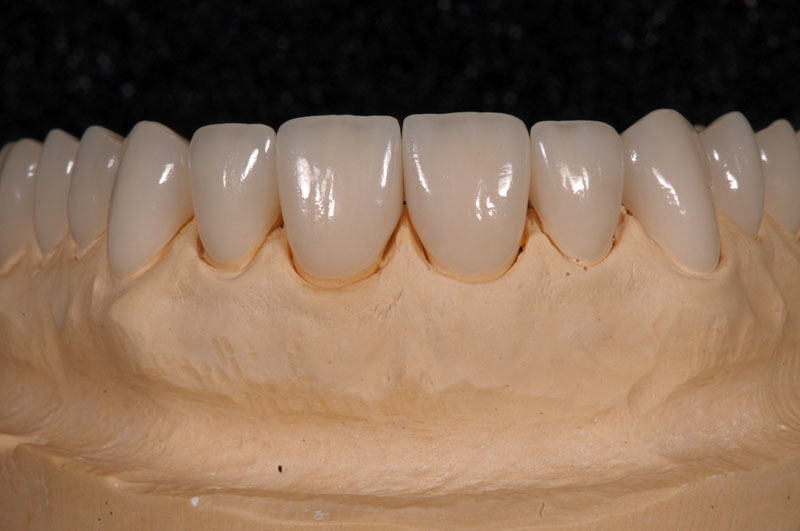
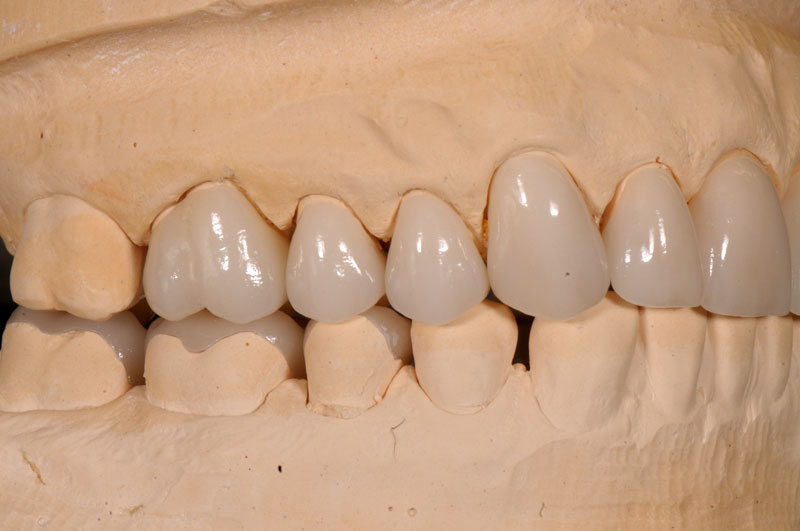
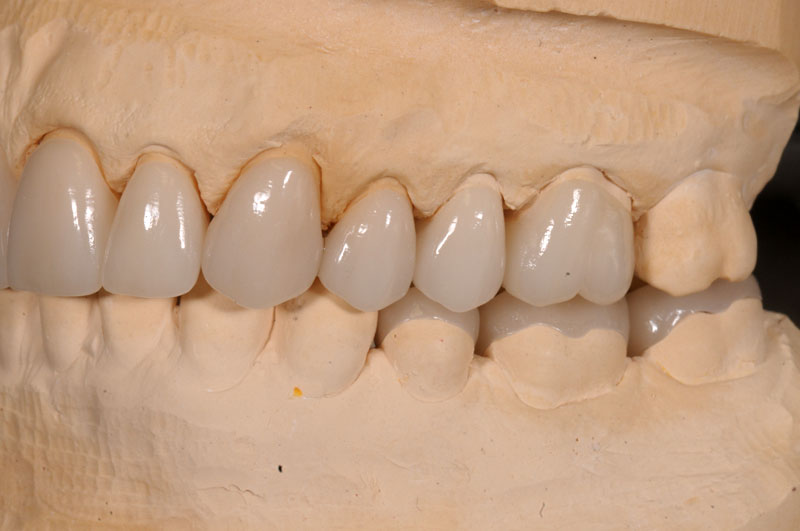
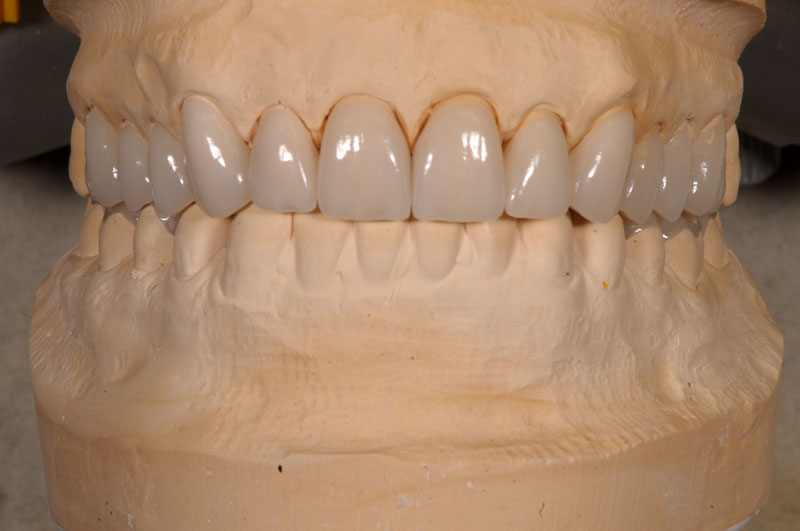
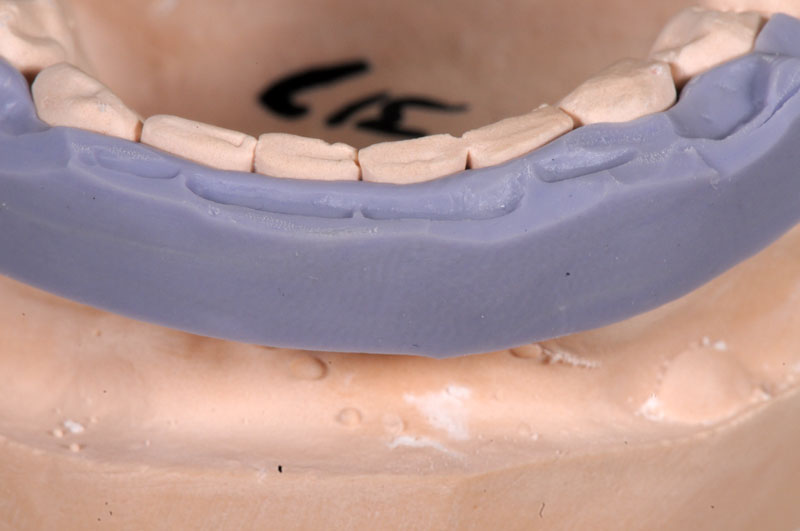
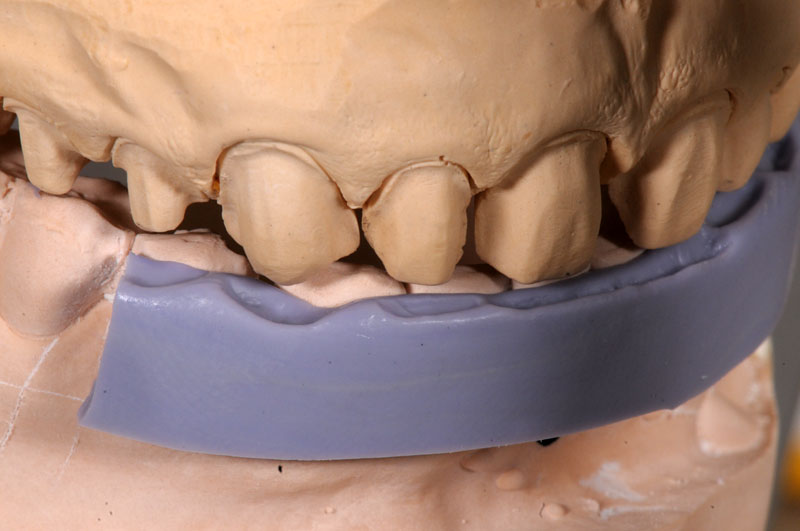
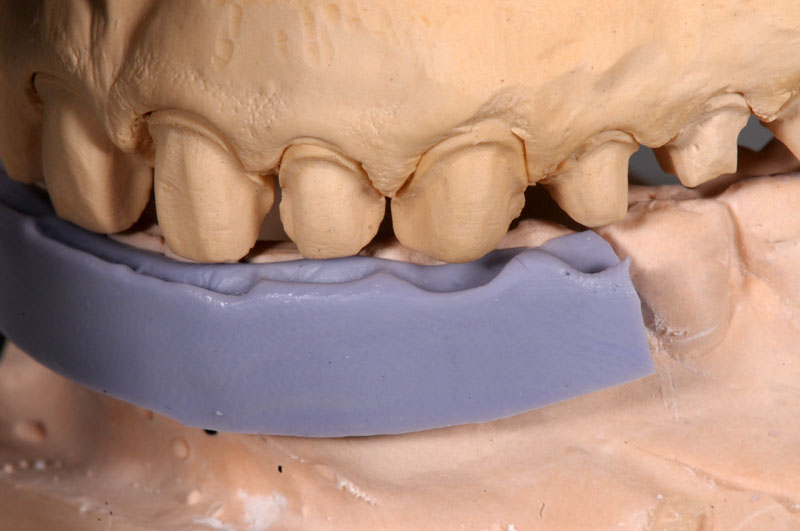
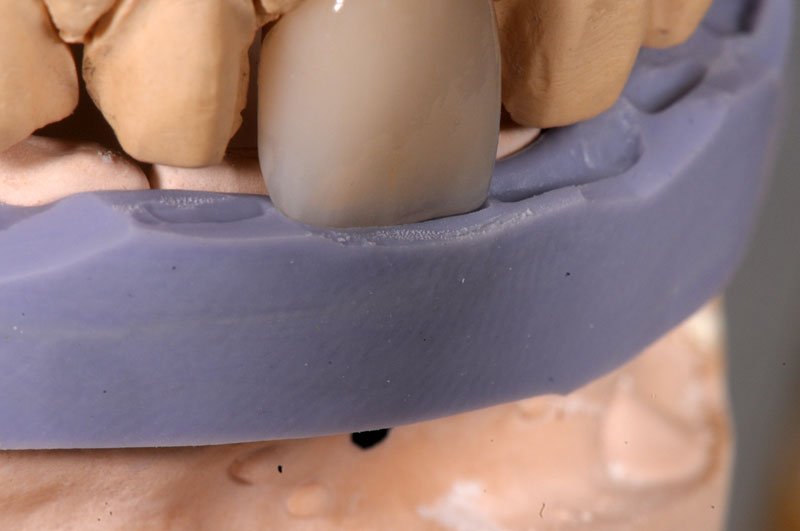
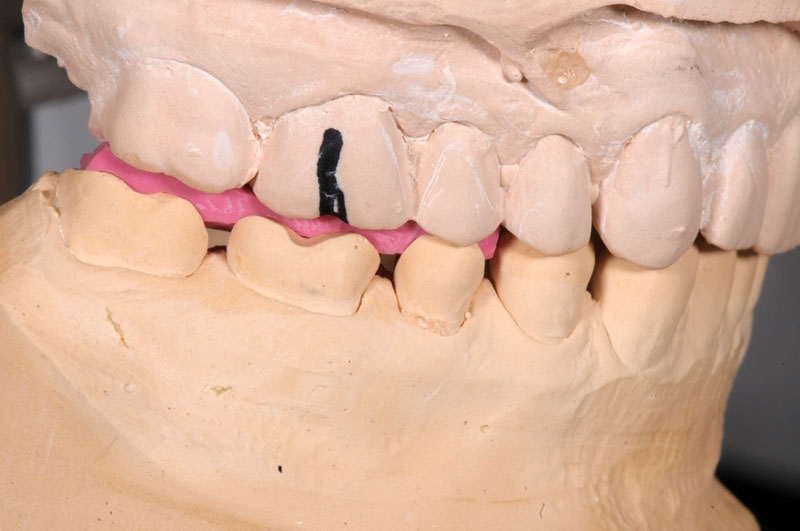
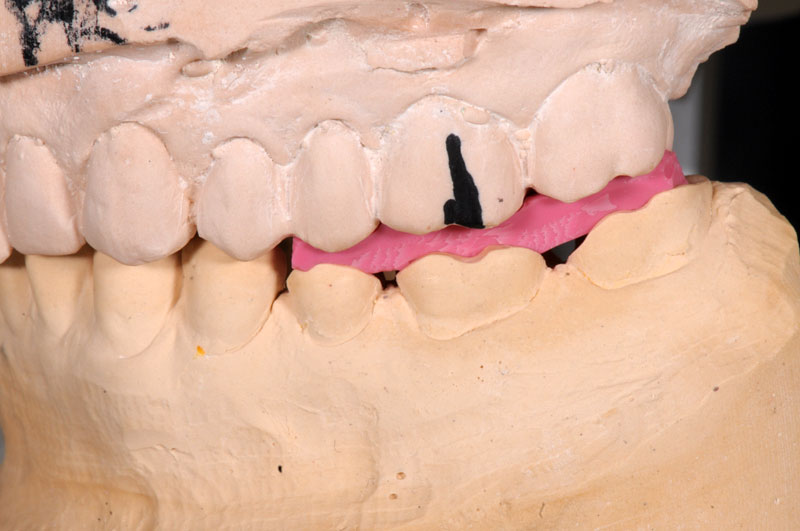
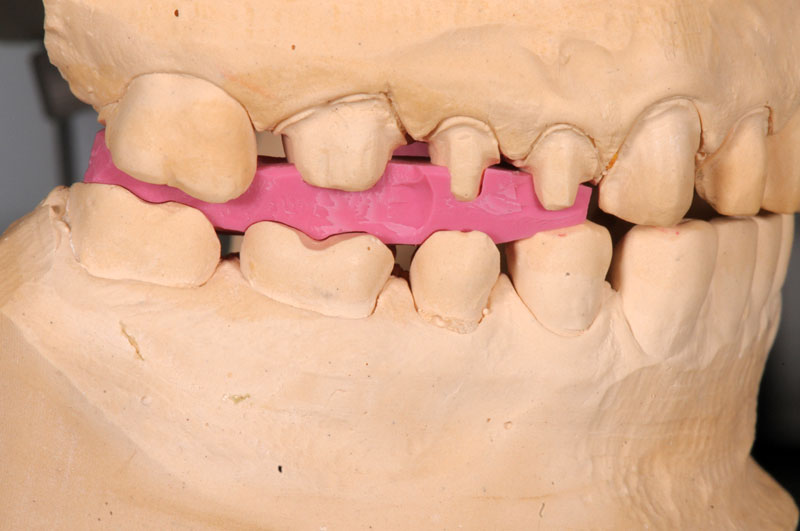
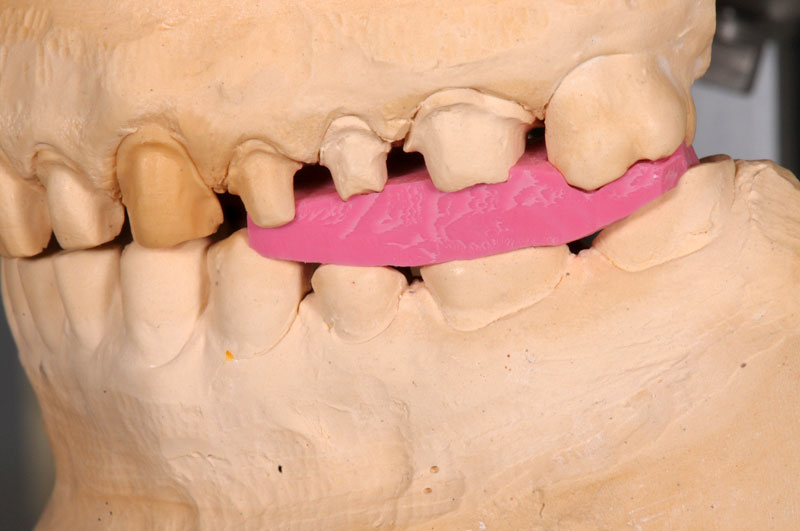
Some things, especially occlusal evaluations, can only be made in the mouth after seating — these are left unmarked so the team is aware these were not checked.
For your convenience, download the Lab Check-in Checklist
References:
- Atul Gawande. Making surgery safer worldwide. Lancet. 2010 Sep 25;376(9746):1045. doi: 10.1016/S0140-6736(10)61473-0.
- Mahajan RP. The WHO surgical checklist. Best Pract Res Clin Anaesthesiol. 2011 Jun;25(2):161-8. doi: 10.1016/j.bpa.2011.02.002...
- Atul Gawande. The Checklist Manifesto: How to Get Things Right. New York: Metropolitan Books, 2009.
Gary DeWood, D.D.S., M.S., Spear Faculty and Contributing Author