Continuing our series on erosion and attrition, one of the more common causes of intrinsic erosion is Chronic Gastroesophageal Reflux Disease or GERD.
GERD is a condition where the esophageal sphincter allows stomach acids to leak out of the stomach and into the esophagus and even the throat and mouth. It frequently causes heartburn, a burning sensation in the throat, sometimes difficulty sleeping and occasionally a bad taste in the mouth or sour breath. The diagnosis is made if this occurs more than twice a week.
Although the condition is well known in the medical community, if you look at some hospital websites they still fail to mention dental findings as part of the diagnosis. This is particularly important when we understand that "silent GERD" or the complete absence of the awareness of signs and symptoms occurs as often as 80 percent of the time. GERD can chronically irritate the esophagus and result in Barrett's Esophagitis a condition linked to esophageal cancer.
Dental findings are erosion on the palatal surfaces of the maxillary anterior teeth and progress posteriorly to the lingual surfaces of all teeth. The occlusal surfaces of lower posteriors may be involved and occasionally facial surfaces of teeth if the patient sleeps on their side and pools the refluxed acid into their mouth.
Screening questions that may lead to a diagnosis:
- How often do you get heartburn?
- Do you have a bad taste in your mouth or sour breath on an ongoing basis?
- Do you need to sleep with your head elevated to avoid painful burning in your throat or chest?
- Do you notice that food or drink "comes back up" easily after eating or drinking?
Any positive answers merit a referral to a physician, especially if there are dental signs as well.

Notice the defined "finish line" at the gingival level (above).
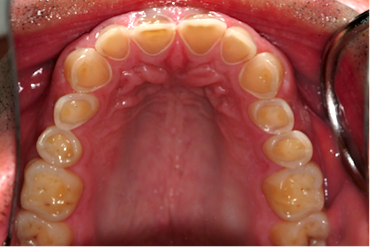
GERD diagnosed at age 10, patient is now 36. Notice the erosion has also affected the entire facial surface of all the teeth from premolar to premolar (above).