All-on-X Dental Implants: A Clinical Restorative Guide
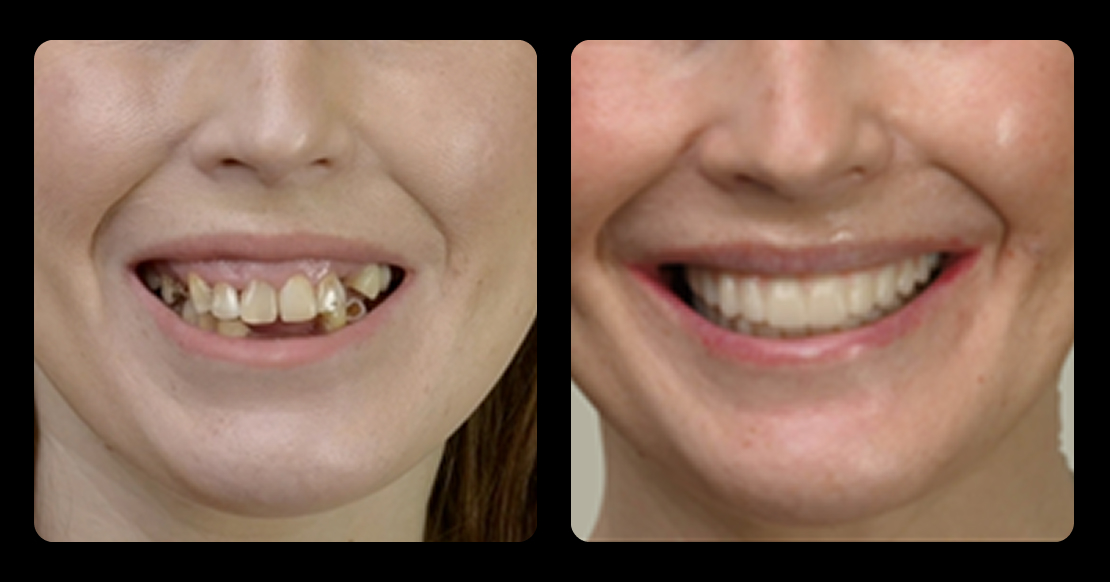
All-on-X dental implants solve one of the hardest problems in dentistry: full arch rehabilitation that is stable, efficient, and predictable.
At its core, the concept is straightforward. Four or more implants support a fixed prosthesis across a full arch. The exact number depends on anatomy and load requirements, but the objective stays consistent. Cross-arch stability. Immediate function. Long-term success.
This approach did not start as a comprehensive solution. It was introduced to treat mandibular edentulism. A focused use case with clear constraints. Over time, it expanded. Today, it shapes how we approach full arch care. Surgical precision and prosthetic control working together in a coordinated system.
That evolution has been significant. What began as a four-implant protocol is now a flexible, digitally driven strategy. Treatment planning is more precise. Execution is more controlled. Outcomes are more predictable.
In my practice, this has become one of the most impactful treatments we provide. When case selection is disciplined and execution is intentional, it improves clinical outcomes, increases efficiency, and builds patient trust.
What defines the All-on-X concept clinically?
“All-on-X” has become a catch-all term for what we call in prosthodontics a fixed implant-retained and supported prosthesis. The prosthesis is fully supported by implants. It may sit above or place slight pressure on the tissues, but it does not rely on tissue support for stability.
The “X” represents an unknown number of implants. Traditionally, the concept began with four implants. As we have better understood biomechanics and long-term risk of implant failure, most clinicians now place more than four implants in many cases.
Implant companies have introduced their own branded versions of this concept. In Fig. 1, for example, Straumann refers to its solution as Pro Arch.
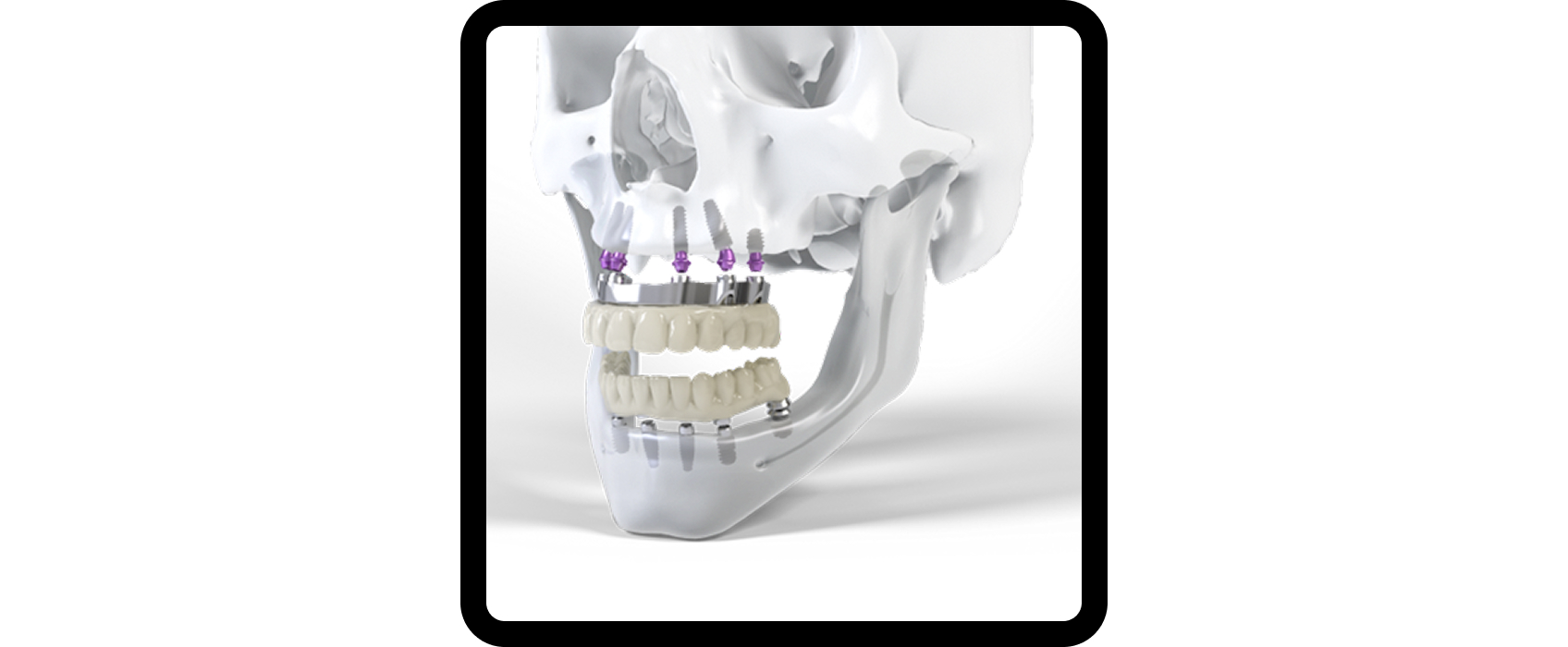
Why do clinicians often place more than four implants in All-on-X cases?
You may have heard the phrase: “All-on-4, but none-on-3.” If one implant fails in a four-implant configuration, additional surgery is typically required. A new prosthesis must be fabricated because it is not biomechanically sound to support a fixed full arch prosthesis on only three implants.
If additional implants cannot be placed, the case may need to be converted to an implant-assisted removable prosthesis.
Cross-arch stability allows immediate loading in these cases. This biomechanical principle is foundational to the long-term success of All-on-X dental implants. The rigid arch form minimizes micromotion and lateral forces during healing, which is why immediate provisionalization is often possible, unlike with many single-unit implants.
The All-on-X treatment concept employs a graftless approach by placing tilted dental implants in ideal native bone, offering a solution even for patients with atrophic jaws. For many clinicians, this is one of the most compelling advantages of All-on-X dental implants.
Long-term studies show survival rates above 95% for full arch implant restorations. According to the International Team for Implantology, careful treatment planning and maintenance protocols are critical to long-term implant success.
It eliminates the complications associated with sinus augmentation and grafting and significantly shortens the surgical timeline, since no staging is necessary.
All-on-4 vs. All-on-X dental implants: What’s the difference?
While the terms are often used interchangeably, All-on-4 and All-on-X dental implants are not identical. The key difference lies in flexibility and long-term risk management. The distinctions become clearer when we compare the two concepts side by side.
|
All-on-4 |
All-on-X Dental Implants |
|
|
Number of implants |
Fixed at four implants |
Four or more implants, based on anatomy and biomechanics |
|
Biomechanical redundancy |
Limited redundancy if one implant fails |
Greater redundancy with additional implant support |
|
Risk tolerance |
Higher risk if one implant fails (may require remake) |
More flexibility if an implant fails, depending on design |
|
Treatment planning flexibility |
Standardized concept |
Customized to bone volume, arch form, and restorative goals |
|
Long-term maintenance considerations |
Fewer implants may increase load per implant |
Load distribution can be optimized across more implants |
In clinical practice, All-on-X dental implants allow for more individualized treatment planning. Rather than committing to a fixed number, the restorative and surgical teams determine the ideal number of implants based on available bone, esthetic requirements, occlusal forces, and long-term prognosis.
This distinction matters because the number of implants directly influences load distribution, failure management options, and long-term restorative predictability. When planned thoughtfully, All-on-X dental implants allow for greater customization than a fixed All-on-4 model.
How do All-on-X dental implants improve patient quality of life?
Quality of life improves dramatically.
All-on-X dental implants are the closest replacement we have to natural teeth for fully edentulous patients. Implants are not teeth, and they have their own risks, but compared to removable prostheses, patients experience:
- Improved chewing efficiency
- Broader food selection
- Better alveolar bone preservation
- Increased social confidence
Before implants, conventional dentures were the only option. We know that dentures significantly reduce chewing efficiency, affecting nutrition and overall health. Many patients withdraw socially because they are concerned about movement, speech, or instability. Bone loss and facial collapse also progress over time.
Especially in elderly patients, maintaining dietary variety, social engagement, and effective mastication helps reduce health risks, including the risk of aspiration.
Who is a good candidate?
Case selection is critical.
Full arch implant treatment with All-on-X dental implants is one of the most transformative procedures we offer.
Some of my best candidates are patients whose tooth-borne restorations repeatedly fail due to high caries rates that cannot be controlled, despite otherwise healthy hard- and soft-tissue architecture. Patients with severe xerostomia or systemic contributors to rampant decay may benefit from full arch implant rehabilitation.
Other candidates include patients with:
- Significant arch discrepancies
- Uneven occlusal planes
- Poor esthetic display
- Complex restorative histories with guarded long-term prognosis
In these cases, orthodontics, orthognathic surgery, and extensive restorative dentistry may be required to achieve symmetry, but their longevity is questionable. Edentulation, while significant and irreversible, may provide a more predictable long-term solution.
I strongly reference published treatment planning algorithms, such as Mitrani’s work on terminal dentition, when deciding whether to save teeth or move toward full arch implants.
Who is not a good candidate?
This decision cannot be taken lightly.
Failure of a full arch implant prosthesis can leave limited future options. Unlike natural tooth loss, which may leave bone for future implant placement, full arch surgery often includes bone reduction. If failure occurs, there may not be enough anatomy remaining to support a future denture, let alone new implants.
Medical screening is essential. Relative contraindications include:
- Uncontrolled diabetes
- Autoimmune disorders
- Tobacco use
- Alcoholism
- Titanium allergy
- Conditions affecting circulation
As I explain to patients in simple terms, their body needs energy and blood flow to form new bone around implants. If healing is compromised, success is compromised.
Patients must also understand this is irreversible and expensive, both initially and over a lifetime of maintenance. Clear communication about the lifelong commitment required for All-on-X dental implants is essential before proceeding.
How has digital technology improved outcomes?
This is where I have seen the most dramatic change.
In Spear’s restorative curriculum, prosthetically driven implant placement is emphasized because implant position should always follow restorative design.
Historically, significant bone reduction was typical to avoid bulky, ridge-lap style prostheses that were unaesthetic and difficult to clean. Today, with CBCT imaging, Facially Generated Treatment Planning (FGTP), and high-strength zirconia materials, we can be far more conservative.
I do not follow a predetermined amount of bone reduction. Instead, I evaluate what anatomy must be replaced. If disease is present, that dictates what must be removed. The prosthesis replaces what pathology requires, not what dogma dictates.
We classify these prostheses as FP1, FP2, or FP3. My planning is driven by what anatomical structures need replacement, not by arbitrary reduction guidelines.
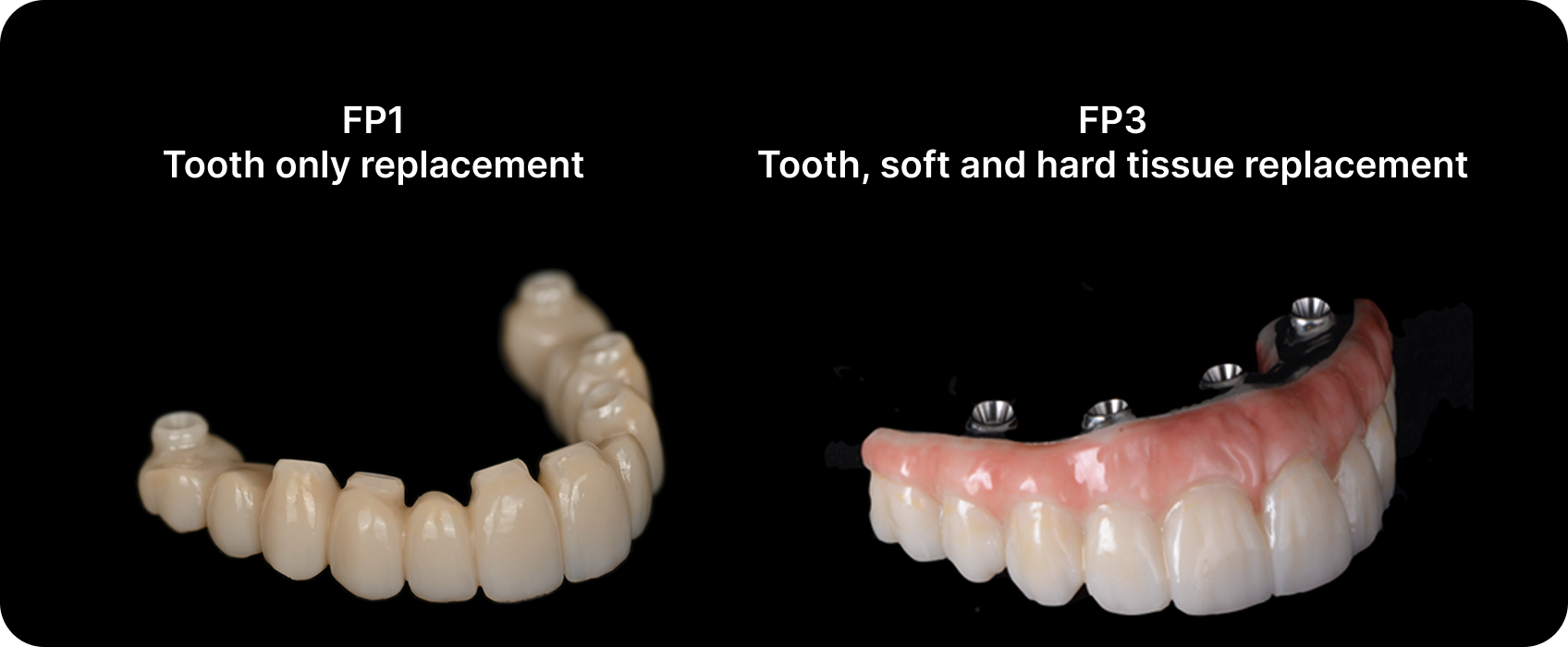
In my experience, zirconia prostheses without ridge laps show less plaque retention and fewer peri-implant complications than older hybrid acrylic-metal designs.
What are common challenges for All-on-X dental implants?
Full arch implant rehabilitation is complex. Without proper knowledge, sequencing, and team coordination, complications are inevitable. In other words, systems matter.
Although I am surgically trained, I practice as part of an interdisciplinary team. I collaborate with an oral surgeon for implant placement and a technician for prosthetic fabrication. My primary role is treatment planning, digital smile design, vertical dimension management, esthetic control, and long-term maintenance.
Some clinicians choose to manage every phase themselves. I recommend a stepwise approach. Gain experience gradually. Lean on colleagues with expertise. Catastrophic failures in these cases are complex, and sometimes impossible, to revise.
Deepening clinical systems for All-on-X dental implants
As I mentioned earlier, full arch implant rehabilitation is not simply a surgical procedure. It’s a coordinated system that includes diagnosis, prosthetic design, surgical planning, provisionalization, and long-term maintenance. When any one of those phases is weak, complications follow.
For clinicians who want to strengthen those systems, Spear offers Restoring the Edentulous Arch, a three-day hands-on workshop. It focuses on assessing and treating edentulous arches by choosing and implementing suitable restorative options, ranging from removable to implant-supported solutions, while managing risks, materials, techniques, and patient expectations.
What I appreciate most about this format is that it emphasizes decision-making. When should we save teeth? When should we transition to full arch implants? How much bone reduction is truly necessary? And how do we design prostheses that are both esthetic and maintainable long term?
For clinicians already restoring implants who want to refine predictability, reduce complications, and build stronger interdisciplinary workflows, structured immersion in these concepts can make a meaningful difference.
Why prosthetic planning drives everything
This is where advanced dental treatment planning becomes critical, because the prosthesis dictates implant position.
If the immediate prosthesis is canted, poorly contoured, or inaccurately set in vertical dimension, implants will be placed based on those errors.
Correcting that later is extremely challenging.
I compare it to building a house. If the foundation is poured incorrectly, remodeling the structure later becomes complicated and expensive.
Digital smile design allows us to preview tooth shape and alignment in 2D with the patient before transferring the design to the CBCT and surgical plan. Centric relation records are critical because the patient will not function in their previous occlusion.
What does sequencing of care look like?

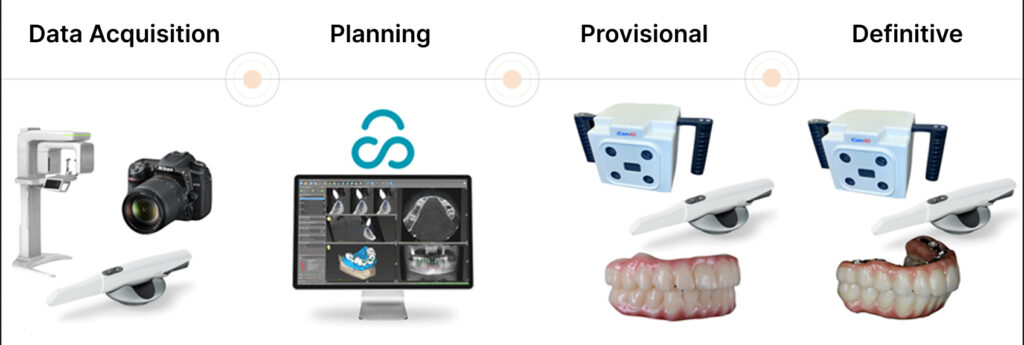
My workflow for All-on-X dental implants includes:
- Comprehensive data acquisition: IOS scans, CBCT, extraoral photography, digitally generated smile design, clinical exam, and detailed patient interview
- Virtual surgical planning and guide fabrication: Medical clearance and anesthesia evaluation, pre-prosthesis design, implant planning, guide design and fabrication, and fiducial selection
- Surgical placement with immediate prototype prosthesis: Implant placement, intraoral scanning, photogrammetry, fiducial alignment, immediate prosthesis fabrication, and post-op care
- Implant evaluation and definitive restoration design: Torque testing, verification of proper healing, impressions with IOS, and photogrammetry
- Additional prototyping if needed: Gain esthetic approval in printed material before fabrication of definitive material
- Delivery of definitive restoration: Insertion of final restoration, tracking of parts and pieces to aid in future maintenance, fabrication of protective occlusal guard, and final maintenance plan
- Long-term rehabilitation and maintenance care: Customized maintenance plan utilizing guided biofilm therapy, home care use with Waterpik, and selected picks and brushes
Each step builds predictability for All-on-X dental implants.
What ensures long-term success?
Maintenance systems.
Having a well-planned system for checking in on the patient during healing and determining when to restore implants will give you and your team predictability and provide the patient with a clear understanding of what to expect throughout the process.
It’s also essential to maintain a soft diet during implant osseointegration, which usually lasts 3-4 months, to prevent fracture of the immediately loaded prosthesis.
Reinforcing proper hygiene of the interim prosthetics emphasizes the importance of maintenance and complication prevention throughout life.
For this, our practice uses Spear Patient Education videos to show patients what the prostheses look like and how to care for them. We also provide a Waterpik and different toothbrushes with various stiffness levels throughout their care.

We instruct them on what constitutes a prosthetic emergency, such as a loose prosthesis, versus issues that can wait until their next checkup. Setting the stage and expectations for these patients will prevent many calls for your team.
Radiographic evaluation intervals and decisions regarding prosthesis removal for cleaning vary among specialists. In our practice, maintenance protocols are individualized based on clinical findings and patient compliance.
Guided biofilm therapy has been particularly helpful in accessing and cleaning beneath full arch prostheses. Long-term stability of All-on-X dental implants depends heavily on structured hygiene protocols and patient compliance.
Contrary to some advertising, these restorations are not easier to maintain than natural teeth. They require lifelong commitment.
If you remember three things
- Edentulism is irreversible, but implants significantly improve the quality of life compared to removable prostheses.
- Success requires strong internal systems and interdisciplinary collaboration.
- Digital technology has dramatically improved predictability, accuracy, and long-term outcomes in All-on-X rehabilitation.
Full arch rehabilitation with All-on-X dental implants is one of the most transformative procedures we offer. When approached carefully, planned prosthetically first, and maintained properly, All-on-X dental implants can profoundly improve patients’ lives.
Frequently Asked Questions
References
- Mitrani, R., Papaspyridakos, P., Bedrossian, E. A., Goldberg, J., Tsigarida, A., & Chochlidakis, K. (2024). Treatment planning algorithm for patients with a terminal dentition. The Journal of Prosthetic Dentistry.
- Misch, C. E. (1989). Bone classification, training keys to implant success. Dentistry Today, 8(4), 39-44.
- Maló, P., Nobre, M. D., & Lopes, A. (2011). The rehabilitation of completely edentulous maxillae with different degrees of resorption with four or more immediately loaded implants: a 5-year retrospective study and a new classification. European Journal of Oral Implantology, 4(3), 227-243.
- Malo P, de Araújo Nobre M, Lopes A, et al. A longitudinal study of the survival of All-on-4 implants in the mandible with up to 10 years of follow-up. Journal of the American Dental Association 2011;142(3):310–320.
- Malo, P., de Araújo Nobre, M., Lopes, A., Moss, S. M., & Molina, G. J. (2011). A longitudinal study of the survival of All-on-4 implants in the mandible with up to 10 years of follow-up. The Journal of the American Dental Association, 142(3), 310-320.
SPEAR campus Workshops
Step Into a Place Built for Mastery
Step away from the noise of practice and into focused, immersive training that changes how you think, diagnose, and lead.

By: Kimberly Schlam
Date: April 14, 2026
Featured Digest articles
Insights and advice from Spear Faculty and industry experts