CBCT: A Window Into ‘Why’
The goal of a health care provider is to evaluate patients, establish a differential diagnosis of a disease process, determine the proper etiology, and provide treatment options to ensure optimal care with the best possible outcome.
To do so, a practitioner must gather as much information as possible, which is achieved by a thorough medical, dental, and sleep history, a comprehensive exam and data collection, radiographic imaging, and screening tests so that treatment options can be evaluated, and a proper course of action can be implemented. Patients must then be educated on the cause of their issues and informed about treatment options that can offer the best possible outcome and prognosis.
What Is the ‘Why?’
Foundational courses and concepts taught at Spear, like The Treatment Planning Process and airway, esthetics, function, structure, biology, educate dentists about the benefits of combining a comprehensive exam, data collection, and photography. This information can then be integrated into a PowerPoint or Keynote presentation for patient education, which is called the Tour of the Mouth.
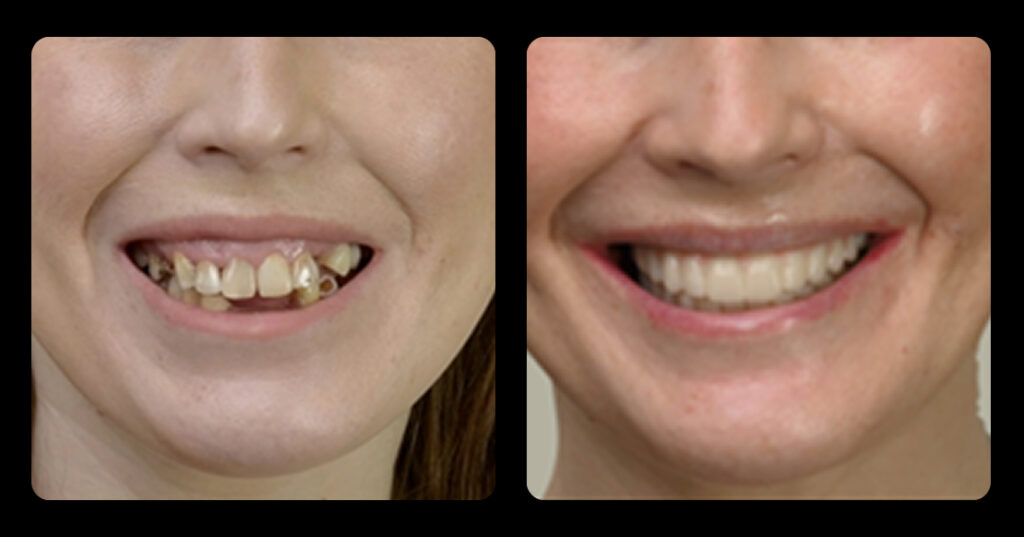
These tools provide patients with the necessary education to understand the root cause of their medical/dental issues and the potential treatments. It is my opinion that the best possible clinical outcomes can be achieved when both doctor and patient understand the “why” or etiology, then choose “how” they want to correct it, or treatment options, and finally achieve an outcome or the “what” — a healthy, beautiful smile.
As more information is understood about the benefits of sleep, the impact of proper growth of skeletal anatomy, and its correlation to health, dental providers are at the forefront of helping patients who choose to optimize their health and seek to improve the quality of their lives.
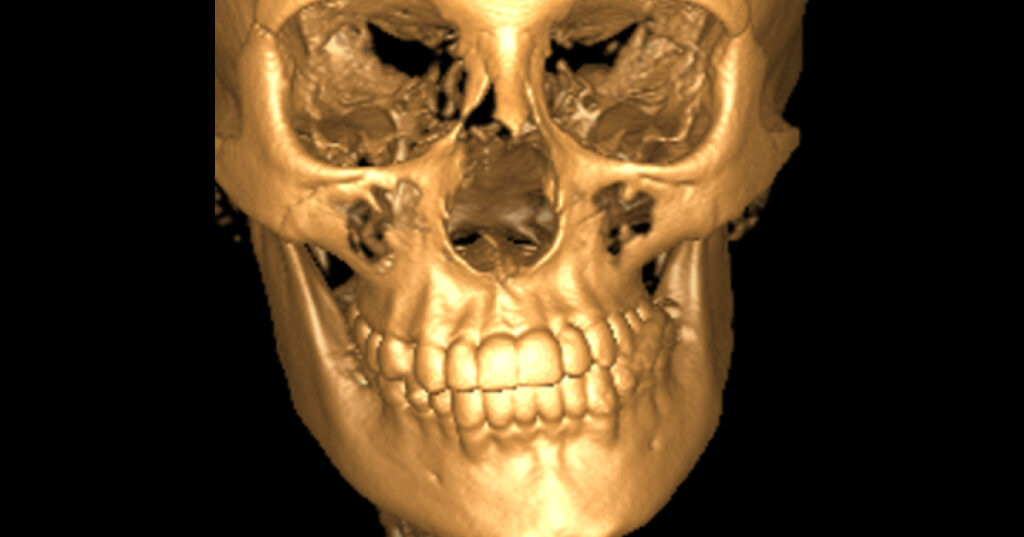
Many of the factors surrounding sleep and airway issues, TMD, and dental breakdown can be traced back to skeletal and traumatic sequela that occur during a patient’s lifetime. Radiographic imaging using cone beam computed tomography (CBCT) can offer insight into potential causes and possible treatment solutions by visualizing patients’ bony and structural anatomy.
Cone-Beam Imaging
CBCT provides detailed images of bone and is performed to evaluate diseases of the jaw, dentition, bony structures of the face, nasal cavity, and sinuses. It does not provide the full diagnostic information available with conventional CT, particularly in evaluating soft tissue structures such as muscles, lymph nodes, glands, and nerves; however, CBCT has the advantage of lower radiation exposure than conventional CT.
Common uses of CBCT include:
- Surgical planning for impacted teeth
- Diagnosing TMD
- Accurate placement of dental implants
- Evaluation of the jaw, sinuses, nerve canals, and nasal cavity
- Detecting, measuring, and treating jaw tumors
- Determining bone structure and tooth orientation
- Locating the origin of pain or pathology
- Cephalometric analysis
- Reconstructive surgery.
A CBCT has been of great value in my restorative practice. I like to include images in my Tour of the Mouth to help patients better understand and visualize the skeletal issues impacting their health. Comprehending the impact of deficiencies in any or all of the three skeletal dimensions is critical when determining the proper etiology and then initiating the optimal treatment course.
Anterior/Posterior Dimension
Cephalometric images can identify anterior/posterior deficiencies (Fig. 1). Witts Analysis indicates this child is maxillary deficient, stressing the importance of early orthodontic intervention. Failure to correct this now potentially creates a future where the soft palate may impinge upon the airway, resulting in a sleep disorder and other health-related sequelae. The same can be evident for a retrognathic mandible, potentially forcing the tongue back into the throat and pharyngeal region, impinging on the airway.
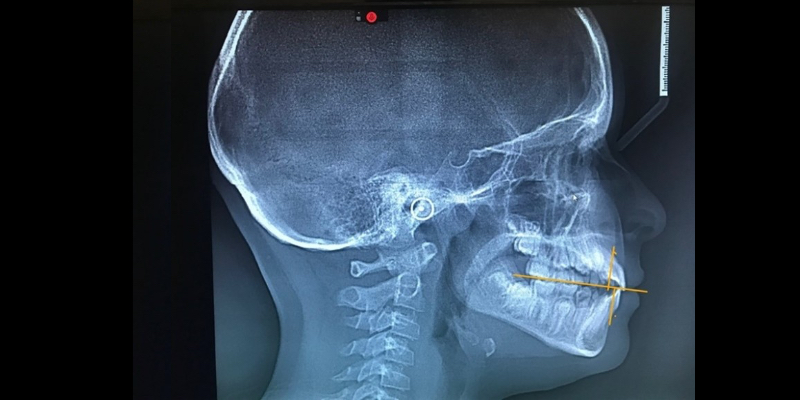
Both children and adults display deficiencies in the anterior/posterior dimension, a common finding in sleep-related disordered (SRD) patients due to improper growth of the maxilla and mandible.
Early interventions can offer solutions to correct and prevent these outcomes and their effects on a patient’s health. The social, educational, and growth implications can be far-reaching and often mistreated when failure to diagnose the true etiology of the disorder properly is not fully understood and acted upon.
Nasal Septum

Many factors lead to mouth breathing, one of which is a deviated septum (Fig. 2). A CBCT can clue a practitioner into this problem, and noninvasive treatments like Buteyko breathing or nasal breathing can greatly improve a patient’s quality of life.
This can provide an inexpensive option to better sleep, using mouth tape and nasal dilators, which is Step 1 in The Seattle Protocol; however, if a patient desires correction and an actual fix to the skeletal issue, these images can help an ENT provide a surgical plan.
Proper nasal breathing is critical and vital to maximize a patient’s health, correcting and preventing mouth breathing, and improving sleep quality.
TMJ and Vertical Dimension
Imaging is essential in recognizing problems in the temporomandibular joint region, which is vital in airway management, treating TMD, and providing restorative care. Active or passive joint degeneration and disk injury can result in a loss of vertical dimension (Fig. 3).
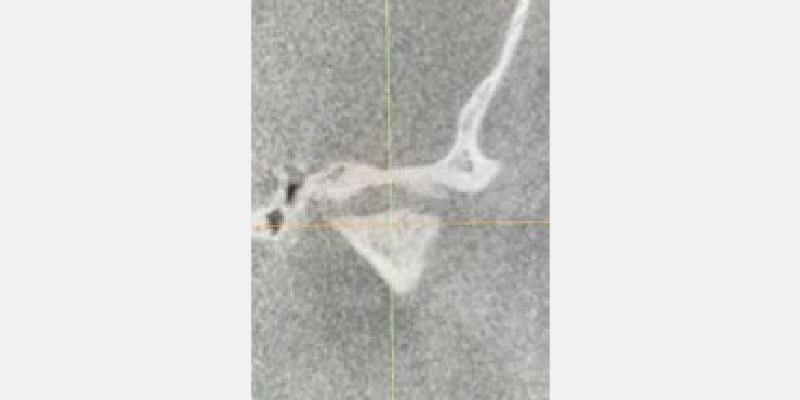
This loss can have a multitude of causative effects, such as pain and/or loss of function in the joint region or any of the head and neck muscles. This dimensional loss can also impact a patient’s occlusion and tooth wear. These images can also indicate the need for additional imaging, like an MRI, to understand better the impact and damage to the temporal mandibular disc.
Additionally, a loss of vertical dimension can negatively impact the airway. When considering a mandibular advancement appliance (MAD) to treat obstructive sleep apnea (OSA), it is essential to have a complete understanding of disk position and the presence of active or passive condylar degeneration since compressive forces can exacerbate these conditions.
Airway Volume
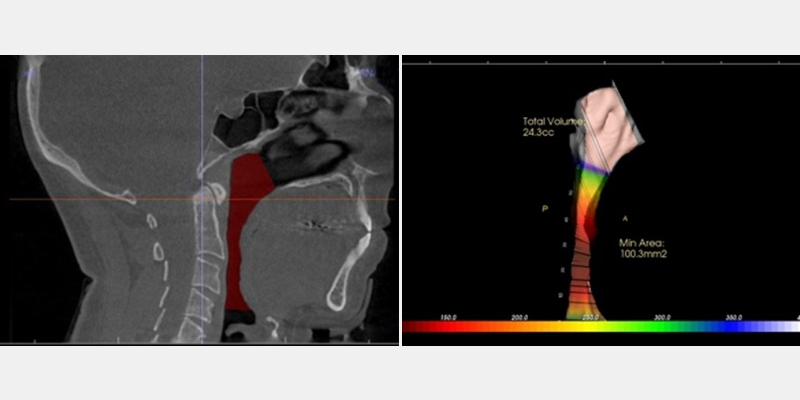
Images of the airway space and the overall airway volume are beneficial when trying to understand the impact of the soft tissue and its effect on airflow. While Figure 4 is a “snapshot” of a patient’s anatomy, it can provide insight into the cause and effect and the potential chokepoint, which is the area where the tissue can close off, impairing breathing.
Typically, a normal range is 150.0 mm, so if a patient, for example, shows a volume of 50.0 mm, a practitioner would want to consider ordering a sleep screening test to rule out an SRD.
Tonsils and Adenoids
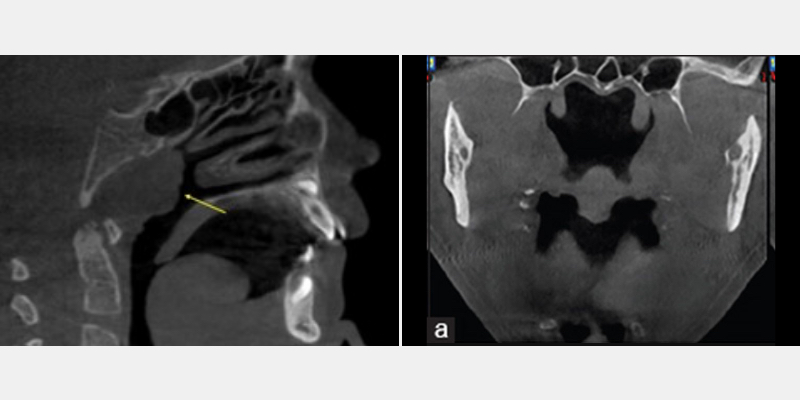
A CBCT can also indicate the presence or absence of enlarged tonsils and adenoids (Fig. 5). These anatomic structures in the parapharyngeal region can impact a patient’s health and sleep by narrowing, restricting, or blocking the airway.
When evaluating patients and their sleep disorders, the “why,” or the etiology, is critical when offering solutions and/or treatment options. This is especially true with children, as early intervention can prevent and improve the quality of their growth and development.
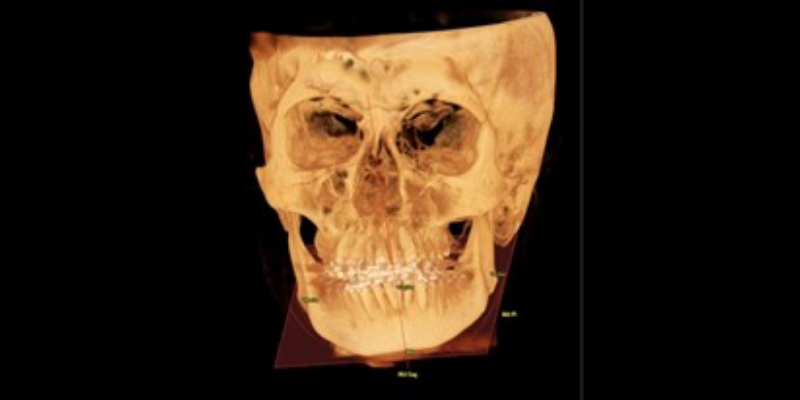
Ramus Asymmetry
Asymmetry in ramus length indicates abnormal growth in the condylar region or a history of trauma. Oftentimes, this is benign; however, it can harm occlusion and facial esthetics. This condition can also cause changes in pharyngeal airway morphology, which has been shown to improve following orthognathic surgery. Visualizing and measuring the ramus length is helpful in a differential diagnosis.
Transverse Dimension
The transverse dimension is also critical to visualize and understand, as deficiencies can result in sleep disorders, malocclusion, tooth wear, and improper growth. Practitioners can measure the maxilla and mandible to understand better their growth relationship (Fig. 7). The ideal relationship would be a measurement of maxilla plus 5.0 mm compared to the mandible. The image also demonstrates the patient’s inability to get their tongue to the palate.
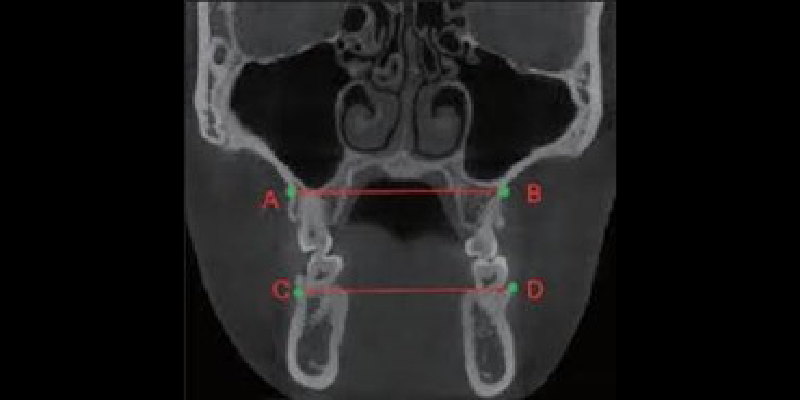
How the tongue fills this space is an excellent indicator of narrow arches and a likely tongue-tie, which affected growth. Recognizing transverse dimension issues early can produce very predictable corrections through expansion. With the introduction of TAD expanders and surgical intervention, adults can correct these issues improving occlusion, sleep, and overall health.
The benefit of a CBCT is to provide a better understanding of the skeletal anatomy of a patient. With this information we can ask questions that can provide more answers and solutions to correct and prevent problematic sleep, esthetic, and occlusal issues.
Having this information is beneficial in helping to educate patients why they may be having some of the medical conditions they are faced with and offer ways to fix the problems. Many of the medical/dental conditions we see in everyday practice can be traced back to skeletal anomalies. Oftentimes, the best outcomes can only be achieved when the proper diagnosis is made. It is my belief a CBCT is a valuable tool to help practitioners understand and treat patients optimally.
References
- Andrucioli, M. C. D., & Matsumoto, M. A. N. (2020). Transverse maxillary deficiency: treatment alternatives in face of early skeletal maturation. Dental Press Journal of Orthodontics, 25, 70-79.
- Radiological Society of North America (RSNA) and American College of Radiology (ACR). Dental Cone Beam CT. RadiologyInfo.org. https://www.radiologyinfo.org/en/info.cfm?pg=dentalconect. Accessed Feb. 23, 2021.
SPEAR ONLINE
Follow a Clear Path to Clinical and Practice Confidence
Next-level confidence isn’t random. It’s structured. Follow a clear pathway that will accelerate your clinical and practice progression.

By: Andrew Cohen
Date: March 1, 2021
Featured Digest articles
Insights and advice from Spear Faculty and industry experts