Should Dentists Screen for Sleep-Related Disorders?
This follow-up to my previous Spear Digest article will review some of the devices dental care providers can use when screening for sleep-related disorders (SRD).
SRD is an epidemic that can significantly impair a patient’s health. Poor quality sleep has been linked to various medical diseases, such as diabetes, high blood pressure, cardiovascular disease, anxiety, depression, stroke, Alzheimer’s, and dementia, to name a few. Patients typically see dentists more than any other health care provider due to the frequency of routine dental maintenance appointments. This creates an opportunity for dental health care providers to ask questions about patients’ sleeping habits and routines. This is also a time that providers can review a patient’s prescribed medications and past and current medical history, which can influence the quality of a patient’s sleep.
Combining that information with a comprehensive dental exam can provide insight into an undiagnosed sleep issue. In my previous article, I discussed how the clinical exam can reveal signs and symptoms of sleep-disordered breathing (SDB). Once SDB is suspected, dentists can use adjunctive devices to screen and determine if treatment would be beneficial, allowing patients to achieve the necessary and required health benefits of sleep.
When health care providers suspect SDB, as the current medical model dictates, patients are referred to a sleep specialist who orders a sleep study. Then, if necessary, they prescribe either CPAP, mandibular advancement device (MAD), positional and weight loss therapy, or surgery. Outside of surgery, practitioners are only managing end-stage disease, as in most cases, the etiology of SRD is anatomic in origin.
Early intervention can prevent the progression of sleep-related diseases and the negative impact they have on patients’ overall health, growth, and development. As more research is published about the progressive nature of SRD, dental care providers must be at the forefront of early detection. Many signs and symptoms of SRD begin in early childhood and can be uncovered during routine oral care maintenance. It is vital that providers — at each dental wellness visit — review patients’ medical and dental history, look for signs of erosive or destructive wear, be aware of mouth breathing, determine possible causes for chronic pain and headaches, and perform a thorough review of sleep hygiene and history.
Often, a picture develops of a patient in distress with a high apnea-hypopnea index (AHI) and various medical conditions. However, sometimes you’ll face a different type of patient with no obstruction, but rather flow limitation issues. This condition is known as upper airway resistance syndrome (UARS), which also has significant medical and social implications due to its association with inadequate sleep. Screening for these conditions provides an efficient, non-invasive, and cost-effective way to uncover and treat patients when the condition is more manageable. Dentists can now have screening devices in their armamentarium to help uncover and prevent disease progression, not just restore teeth. Dental care providers can improve patients’ lives and potentially prevent diseases both now and in the future. The goal is to detect, understand, and manage SDB to optimize a patient’s quality of life.
Screening patients is within the scope of work for dental practitioners. If an SRD is uncovered, appropriate referrals to ENT specialists, orthodontists, oral surgeons, and sleep specialists may be necessary. Most health care providers are familiar with both polysomnograms (PSG) and home sleep testing (HST) to monitor and measure sleep staging, blood oxygen levels and desaturation, respiratory effort and airflow, heart rate, and body position.1
These tests need to be read by a certified sleep specialist so an accurate diagnosis can be made. Unfortunately, many patients fail to initiate treatment due to cost, inconvenience, misconceptions about available treatment options and inaccurate beliefs about having a sleep related issue.
Reviewing medical history, sleep disturbances such as snoring or nocturnal bruxism, and observing clinical and anatomic signs may indicate an SRD. To confirm suspicions of a sleep-related disorder, diagnostic tools such as a high-resolution pulse oximeter, cardiopulmonary coupling unit (CPC), HST, the Gem Pro Wellness Monitor, and even standard innovative technology, including phones, watches, and fitness bands, can be used to objectively determine the quality of sleep.
This article will primary focus on the HR pulse oximeter and the CPC, which are both cost-effective and non-invasive for the patient. (View Spear Resident Faculty member Dr. Jeff Rouse’s online courses Airway Screening Tools: Cardiopulmonary Coupling and Airway Screening Tools: High-Resolution Pulse Oximetry for more clinical lessons on these issues.)
Understanding HR Pulse Oximetry
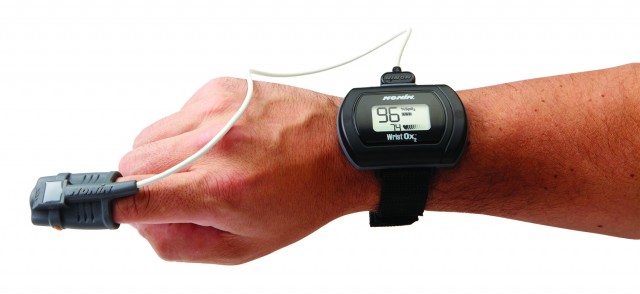
HR pulse oximeters provide helpful information regarding patients’ quality of sleep. The pulse oximeter measures the percentage of the patient’s hemoglobin, which is saturated with oxygen. This provides objective data about oxygen desaturation events and the percentage of time they occur. These devices also demonstrate pulse rate and heart rate variability (HRV), which can indicate respiratory effort or a sympathetic response to insufficient breathing. This data can then be analyzed to determine the number of oxygen desaturation events, which is used to calculate an adjusted index. Certified sleep specialists often use this index to obtain the apnea/hypopnea Index (AHI).
These devices analyze and record events when the oxygen levels decrease by 3% for more than 10 seconds. HR pulse oximeters are excellent for use when obstructive sleep apnea is suspected, as they quantify the percentage of oxygen desaturation. These units are very durable, can be used multiple nights, are compact, non-invasive to the patient, and easy to use. Monitoring SPO2 in arterial blood is a critical finding for diagnosing and evaluating treatment in patients with SRD. HR pulse oximeters are also useful to determine the efficacy and titration of sleep disorder treatments.
Exploring Cardiopulmonary Coupling (CPC)
The CPC is a second device dentists can use for routine screening at a low cost to the patient. These units are unobtrusive tests that create an algorithm based on HRV that can help detect potential sleep disorders. The CPC is an FDA-approved device that provides an objective sleep quality measurement of sleep quality, duration and sleep pathology by a single lead ECG.
Specifically, it measures the synchronicity of the heart rate with respiration. Research studies have compared data obtained from a CPC to a PSG and found the data and diagnosis to be statistically comparable.3
A CPC uses a single lead ECG and high-precision 3-axis accelerometer data to obtain four data streams. Snoring, body position, actigraphy and ECG are measured to determine heart rate variability and tidal volume flux. Respiration is observed with changes in amplitude of the QRS complex which is directly related to tidal volume changes with inhalation and exhalation. Heart rate variability is measured from the R-R interval on the ECG. The data collected indicates physiologic changes in sleep via the autonomic nervous system though the lower brain centers and networks including the thalamus, hypothalamus and hippocampus.
Sleep staging is typically done with a PSG and is classified as Stages 1-3 (NREM) and REM sleep. A CPC can classify sleep as stable, unstable, and REM based on the frequency data collected. Stable sleep creates a high vagal tone, blood pressure dip, and consistent breathing, which is recognized as high frequency on a CPC. In essence, the heart rate and respiration are in sync with each other, exhibiting high variability – thus resulting in a high frequency reading.
In unstable sleep, which correlates with Stage 1 sleep, the opposite is observed — cyclic variations in heart rate, an absence of blood pressure dip, and tidal volume fluctuations. This data creates a low frequency and represents a period of awakening when coupled with movement. During REM sleep, the body is atonic, and brain activity, heart rate, and blood pressure are all increased. These create greater variability with respiration, which can be evidenced on a CPC. The low frequency is differentiated from an awakening due to a lack of movement. Elevated low-frequency signals are broken down into two categories: narrow and broad bands. These eLFC broad bands are an indicator of sleep pathology (e.g., pain) or airway-disordered breathing patterns (e.g., obstructive sleep apnea, upper airway resistance). In contrast, eLFC narrow bands are an indicator of periodic-type breathing patterns (e.g., central sleep apnea and restless leg syndrome).
When the data is analyzed. A sleep apnea indicator (SAI) is calculated, which displays “one number” for apnea events through the recording period by automatically detecting known changes that occur in the cardiovascular system during periods of sleep disordered breathing. Providers can use this data to help determine and confirm suspicions of SDB. However, since no apnea/hyponia index is recorded, a diagnosis cannot be made from a CPC alone, per the AASM guidelines. A board-certified sleep specialist is still required for a formal diagnosis of an airway and breathing disorder.
Why Sleep Quality Matters for Dental Health
Both an HR pulse oximeter and a CPC are necessary screening devices for understanding and managing sleep-related disorders. Quality sleep is critical to a patient’s well-being and health. Patients who lack the proper amount and benefit of sleep are at an increased risk. Stable sleep, also known as deep sleep, is correlated with Stage 2 and Stages 3-4 sleep, as seen on a polysomnogram. It is during this period of sleep that the body undergoes the most critical recovery and restoration processes necessary for both short-term and long-term health.
Growth hormone released from the pituitary stimulates tissue growth, which is critical for pain and inflammatory management, growth and development. Decreased stable sleep has been linked to cardiovascular disease, high blood pressure, chronic pain, headaches, daytime somnolence, anxiety disorders, an exacerbation of chronic pain, autoimmune diseases, cancer, and Alzheimer’s and dementia. REM sleep is important in the facilitation of learning and consolidation of memories, which is the period of sleep where the mind recovers and is restored. REM sleep is also critical for cognitive function.
As the body transitions from one stage of sleep to the next throughout the night, we can gain a better understanding of how the quality of a person’s sleep may be affecting their overall health, including their teeth. Through screening and the initiation of appropriate sleep-related treatments, dental care providers can help improve a patient’s health and quality of life.
References
- Minkoff, K. (2016). HST vs. PSG. J Sleep Disord Ther, 5, e137.
- Romem, A., Romem, A., Koldobskiy, D., & Scharf, S. M. (2014). Diagnosis of obstructive sleep apnea using pulse oximeter derived photoplethysmographic signals. Journal of Clinical Sleep Medicine, 10(3), 285-290.
- Hilmisson, H., Lange, N., & Duntley, S. P. (2019). Sleep apnea detection: accuracy of using automated ECG analysis compared to manually scored polysomnography (apnea hypopnea index). Sleep and Breathing, 23(1), 125-133.
SPEAR campus
Hands-On Learning in Spear Workshops
With enhanced safety and sterilization measures in place, the Spear Campus is now reopened for hands-on clinical CE workshops. As you consider a trip to Scottsdale, please visit our campus page for more details, including information on instructors, CE curricula and dates that will work for your schedule.

By: Andrew Cohen
Date: April 29, 2019
Featured Digest articles
Insights and advice from Spear Faculty and industry experts


