How Can a Patient’s Overall Health Offer Clues To Potential Airway Issues?
Proper sleep quality is critical for optimal health and the prevention of disease. When patients do not get enough healthy sleep, they are at increased risk of getting sick. In this three-part series, I will review how dentists can better understand, uncover, and diagnose potential sleep-related disorders. I will also review treatment and management principles with the ultimate goal of patients having an improved quality of life and more successful outcomes with their dental care. This article will discuss the key elements that can provide insight into potential airway issues.
Untreated airway and sleep-related issues have been proven to increase the likelihood that these diseases could progress without intervention. Dentists can often diagnose or suspect various medical ailments patients may have through comprehensive oral examinations. There are clearly established findings that suggest the oral cavity can provide insight into a patient’s potential medical disease, such as temporomandibular disorder, diabetes, gastroesophageal reflux disease, and cardiovascular health, to name a few. Current research demonstrates that poor sleep contributes to patients’ health. Patients’ sleep histories — such as nocturnal bruxism, snoring, insomnia, and frequent nocturia — need to be investigated and understood, since they can be clear signs of sleep-related disorders.
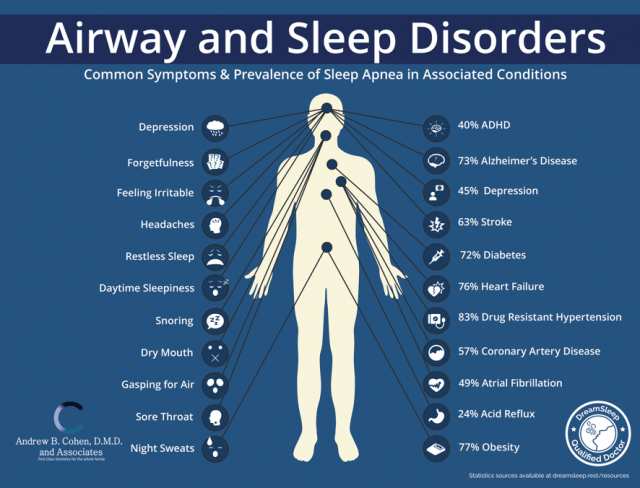
Dental providers typically see patients a minimum of two times a year for routine maintenance, which is sometimes more often than patients see their own physician. This creates an opportunity to help patients become educated about the effects of poor sleep through diagnosis and examination so they can understand and receive medical care for this health-related epidemic.
Sleep-related disorders are mentioned more regularly in the media, so patients are more likely to ask if they have a problem and if they are at risk. Dental care providers can often be the first to uncover sleep-related issues by inquiring about and observing signs and symptoms that patients may not be aware of. Providers must become more knowledgeable about the appropriate questions and what to look for as an essential first step to diagnosing and improving a patient’s health.
Routine review of a patient’s medical, dental, and sleep history — combined with a thorough clinical exam — can uncover and bring to light multiple risk factors resulting from poor sleep quality. Knowing the signs and symptoms can alert practitioners to a potential issue.
To ensure clinical success of a restorative dental treatment, dentists have been taught to fully understand the etiology of a patient’s oral breakdown. Facially Generated Treatment Planning (FGTP) has transitioned into “Airway” Facially Generated Treatment Planning, and providers must now understand how the airway impacts patients’ medical and dental health.
The most crucial part of understanding a patient’s airway is the exam, which can begin as you watch your patients walk down the hall. Observing head position, gait, and eyes can be initial signs that a patient suffers from poor sleep quality.
Diagnosing Airway Issues Through Comprehensive Exams
My comprehensive and routine exams begin with carefully reviewing a patient’s medical history. Poor sleep is associated with multiple co-morbidities. Therefore, when patients report conditions such as high blood pressure, atrial fibrillation, diabetes, gastroesophageal reflux disease, headaches, depression, and TMD, providers should start to consider the airway as a contributory factor. Reviewing medications, such as blood pressure medication, beta-blockers, sleep aids, anti-depressants, and H2 blockers, provides a window into a patient’s medical health.
Clinically, the physical exam may be the best indicator of potential airway issues. Personally, I start from the outside and work my way into the mouth, exactly the same way we are taught in the FGTP workshop. However, now I am looking for additional signs of an airway disorder.
Patients not only have airway issues while they sleep, but they must also overcome this problem while awake. The human body is proficient at compensating and working around many physical and anatomic limitations, and these mechanisms leave clues to an underlying problem.
How the Body Compensates for Airway Issues
When we sleep and our bodies become atonic in stage N3/N4, we lose the ability to compensate for hard and soft tissue factors, resulting in sleep-related disorders. A forward head posture —where the head will be positioned in front of the shoulders — is the body’s compensatory mechanism for stretching the soft tissue, making breathing easier.

Mouth breathing is another example of compensation. Many patients who mouth breathe will also have a strong gag reflex, since the body is trying to protect the airway. A patient with a deviated septum, enlarged tonsils, allergies, or nasal stenosis will learn to breathe through the mouth. This mechanism must be corrected, as nasal breathing is a more efficient and advantageous way to breathe. 1

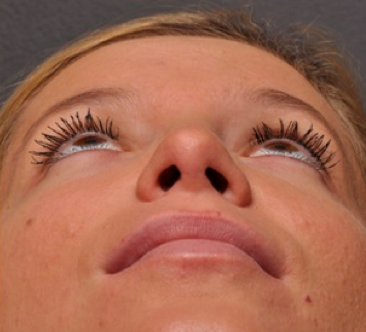
Asymmetric nostrils provide an easy way to screen for a deviated septum. Examining the internal aspect of the nose for red and inflamed tissue should also be considered. The concern is that mouth breathing is a less effective way of breathing, since the nose warms and filters air.
Mouth breathing can also lead to craniofacial developmental deficiencies that can negatively affect growth, development, and the airway. Dentally, mouth breathing contributes to dry mouth, which often increases the risk of a breakdown of the dentition.
As previously mentioned, when we sleep, our bodies become atonic in stage 3/4 sleep or deep sleep. Mouth breathing can make the tongue fall back and block the airway. An individual who mouth breathes and is unable to compensate by breathing through their nose will thus suffer from sleep-disordered breathing.
Impact of Pre-Existing Conditions on Airway
Venous pooling, or dark discolorations around the eyes, is another sign of disturbed sleep and can indicate a more serious issue. Patients with myofascial pain and TMD should be screened as airway patients since headaches, migraines, and chronic muscular and joint pain can help uncover airway issues.
The muscles often have to hold the jaw in a more forward position so patients can breathe, resulting in the muscles building up with lactic acid and becoming sore. As a result, we must examine and palpate these muscles. Correcting airway and sleep disorders often leads to the alleviation of these muscular and joint issues. Primary and secondary damage to the joint and joint position should be evaluated, since many patients have craniofacial deficiencies that can severely impact this area. 1 As I have advanced in both my restorative and airway treatments, I have found a great need for a cone beam computed tomography (CBCT) to elucidate better anatomical issues that may be associated with sleep disordered breathing. This understanding of anatomy can then influence treatment approaches.
Intraorally, the signs of an airway issue can be even more evident. Tongue position and shape provide information about a patient’s airway, childhood growth and development, and sleep. Tongue scalloping occurs when the tongue does not have enough room, and the teeth indent the tongue along the sides.
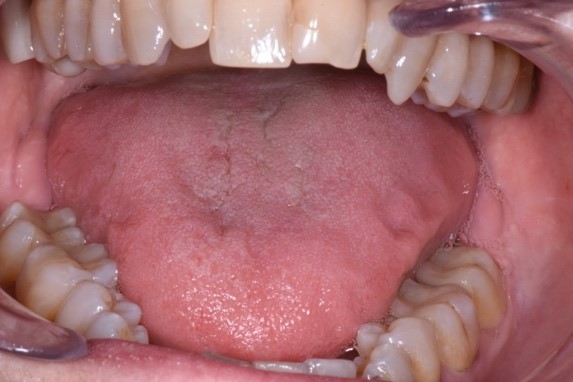
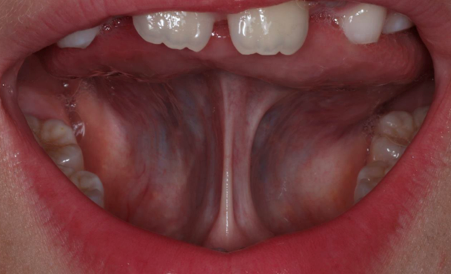
Typically, in constricted arches, the tongue will be forced to sit high in the mouth. This can result in the tongue blocking the airway during sleep. During the day, the body constantly tries to move the jaw forward to create more room so a patient can breathe.
Dentists should also look for tongue ties. A tongue limited in functional movement cannot help form and influence the maxilla during its growth. This often leads to deficient maxillary and mandibular growth in both the anterior/posterior and transverse dimensions. This is often the anatomic cause of malocclusion and the resulting airway issues. An elongated soft palate and an enlarged uvula indicate that the soft tissue may impede one’s airway. A Mallampati score should be recorded, which can predict sleep-disturbed breathing and potentially obstructive sleep apnea.
How Teeth Can Indicate Airway Obstruction
Finally, examinations must observe the teeth for alignment, wear, and structure. Lingual inclination can mean a transverse dimensional issue and constricted arch form. Tooth wear can show signs of erosive and pathway wear, often due to airway issues.
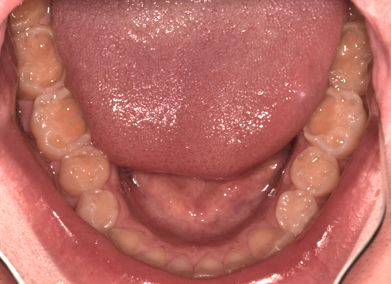
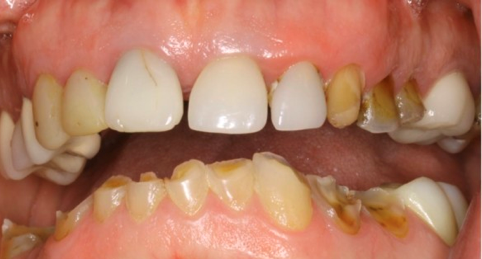
Sleep-related bruxism can devastate the dentition, leading to further loss of vertical dimension and an even greater sleep-related disorder.

Bicuspid extraction was once a method many orthodontists used to compensate for skeletal issues. However, the net effect was decreased arch length and, ultimately, a loss of airway volume, making breathing more difficult. Vaulted palates are another example of skeletal constriction, which again decreases airway volume.
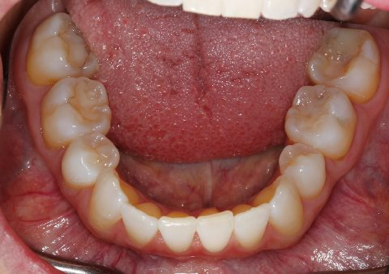
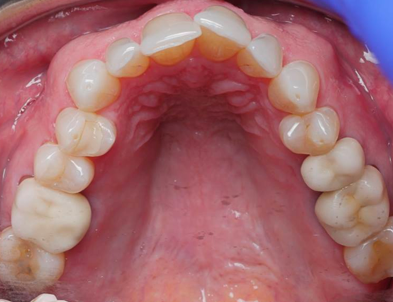
The positive effect dental care providers can have on patients’ lives is far-reaching. Routine dental exams and ultimately finding ways to manage and control a patient’s airway can help lessen the risk of high blood pressure, stroke, cardiovascular disease, cancer, anxiety, dementia, Alzheimer’s, and many other medical diseases. Understanding and treating the etiology behind a patient’s dental care and treatment is the foundation for ensuring optimal dental health. Research proves it’s critical to their overall health and quality of life.
More information about airway and sleep-related disorders can be found on Spear Online, which includes a video with Dr. Jeff Rouse explaining basic steps to conduct a comprehensive pediatric airway exam.
In my next article, I will review various screening tools dental providers can use to help further understand what is happening during a patient’s sleep.
References
- Fitzpatrick, M. F., McLean, H., Urton, A. M., Tan, A., O’donnell, D., & Driver, H. S. (2003). Effect of nasal or oral breathing route on upper airway resistance during sleep. European Respiratory Journal, 22(5), 827-832.
- Bozzini, M. F. R., & Di Francesco, R. C. (2016). Managing obstructive sleep apnoea in children: the role of craniofacial morphology. Clinics, 71(11), 664-666.
VIRTUAL SEMINARS
The Campus CE Experience
– Online, Anywhere
Spear Virtual Seminars give you versatility to refine your clinical skills following the same lessons that you would at the Spear Campus in Scottsdale — but from anywhere, as a safe online alternative to large-attendance campus events. Ask an advisor how your practice can take advantage of this new CE option.

By: Andrew Cohen
Date: January 9, 2019
Featured Digest articles
Insights and advice from Spear Faculty and industry experts


