Working the Slopes: It's All In the Edges
By Kevin Huff on February 13, 2019 | commentsIt is Monday morning, and you have just gotten back that beautiful anterior cosmetic case from the lab: beautiful ceramic restorations for all of the anterior teeth, from cuspid to cuspid, on the maxillary and mandibular arches. You meticulously prepared them using proper reduction techniques complete with excellent photography, precision reduction guides, tissue management, and all the trimmings that you spent countless hours of continuing education workshops, lectures, and true grit to master.
You seat the case in half the time you have scheduled, and everything fits perfectly. You don’t have to touch any of the restorations with a polishing bur because your lab technician is phenomenal! All of your dots and stripes are flawless from the fully-seated condylar position and excursively for about 3mm. It’s truly amazing, and both you and your patient do the happy dance. Fast forward to that evening at about 8:00 at night. You get a call:
“Doc, I’m so glad I got you. You won’t believe this … I just bit into a banana and I heard a crunch. A little sliver of my front tooth just came off. Will it be OK?”
We’ve all had this happen to us at least once. If it hasn’t happened to you, then you’ve probably either been extremely lucky, or you just haven’t done enough anterior ceramic cases. The fact of the matter is that it’s quite common for even the best clinical dentists, using the most amazing master ceramists, to have challenges with what are called the leading and trailing edges of the anterior teeth (and sometimes the bicuspids, when group function is involved).
In the scenario just described, the key to failure in this case is the statement, “You don’t have to touch any of the restorations with a polishing bur because your lab technician is phenomenal!”
It does not matter how amazing a lab technician is - it is nearly impossible to duplicate every detail of occlusion on an articulator somewhere outside of the mouth.
Remember, articulators are a tool that is used to replicate the basic motions of the temporomandibular joints. Since most of us use “arbitrary facebows” to transfer relationships from the clinical to laboratory settings, there is inherent error there. Even with fully adjustable articulators with pantographic tracings, there are still errors that are inherent with laboratory restorations that have to do with variables in model accuracy, impression distortion, bite registration material error, etc.
Even though digital imaging may very well reduce many sources of error, error cannot be avoided when it comes to rebuilding occlusion. It has been said by others much smarter than me that the best articulator is, in fact, the patient. The true magic of occlusion happens in the dental chair and requires intense clinical skill and serious cooperation by the patient. It requires attention to detail by both the patient and the doctor.
Nothing brings this point to light more than places where leading and trailing incisal edges are involved. In fact, Steve Ratcliff wrote an interesting article where he talked about the critical two millimeters that can make or break a case.
As a rather pathetic snow skier (some might call me a gapher), I think leading and trailing edges can be illustrated with a skiing analogy. When I evaluate occlusion, I like to imagine myself as one of the incisor teeth “skiing” over the slopes of the opposing teeth. Please allow me to explain my insanity to you …

After what I consider to be a death-defying ride up to the top of a slope on a chairlift (with your feet laden with heavy, curved, narrow boards attached to Storm Trooper boots that don’t allow you to move your ankles), you must jump off the “swing” at the top of the hill. At this point, you either move forward or are pushed quite abruptly on the back of the shoulder blades by the board you’ve been clutching for dear life as someone yells, “Move, idiot!” At that point in your journey, the snow is flat under your feet.
This is the incisal table. As you start to move down the piste, or downslope, the transition is not abrupt. It is a smooth transition (otherwise, you would fall on your face - I can attest to this from frequent personal experiences). This area of the slope can be thought of as the trailing edge on the incisal facial line angle of a tooth.
As you go up an ego bump (one of those smooth little hills slightly off-piste from the main trail to control your speed), there is a smooth rise up (leading edge) to the plateau (incisal table) before going over the trailing edge to return smoothly down to the main trail. If the junction from the leading edge to the table were sharp, you would launch up, miss the trailing edges and crash down to the slope.
This would not be an ego bump, but a mogul. With incisal edges, it's the same. Moguls cause crashes in crossover and eccentric movements.
Since the process of stacking and layering ceramic - and even milling - creates relatively right angles at incisal line angles, and because articulators typically only allow replication of the pathway from fully-seated condylar position (“centric”) to approximately 2 to 3mm excursively, the laboratory process almost always results in moguls when evaluated clinically in excursive movements.
Therefore, “moguls” must be converted into “ego bumps” chairside with rubber wheels and porcelain polishers. Incidentally, this is also extremely critical with denture occlusion, but it often also involves most of the posterior teeth as well as the anterior teeth.
When evaluating anterior occlusion, I personally watch for roughness, skipping, or catching throughout a full range of excursive movements after the restorations are definitively seated. I also listen … squeaking or scraping is BAD when ceramic is the medium, and suggests moguls somewhere on the slope - maybe even gravel.
Paper shredding in lateral excursion or protrusion strongly suggests moguls to me, and a hard drop off - when the patient grinds all the way to one side or the other or into protrusive - suggests a cliff! When evaluating occlusion, we always want smooth slides and glides - ego bumps, not moguls.

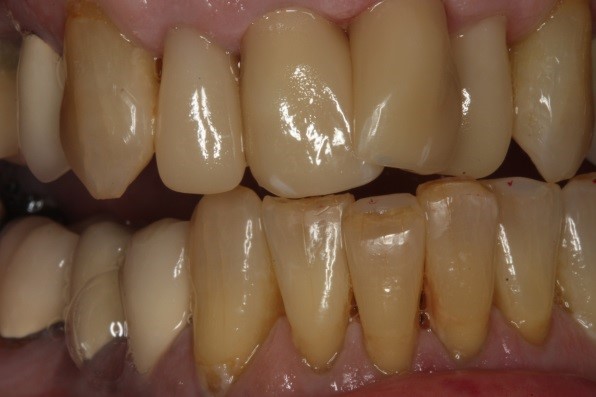


If it’s difficult to follow the method to my madness in the skiing analogy, let’s think about what happens with horizontal pathway wear on natural anterior teeth. Flat tables become broad and flat with dentin islands surrounded by enamel borders that have 90-degree line angles. These are moguls!
What happens next? The facial enamel shears because the jaw muscles prefer smooth ego bumps over moguls. The same thing happens with ceramic - only faster - and failure will occur at the weakest point, often at the facial/incisal/interproximal line angle, where the preparation angle is often most acute. If we look back at the scenario that started this article, it is interesting to note that many times, teeth or restorations break with soft foods. I believe that this is because it is with these foods that the teeth are brought closest together in functional excursion, during which times leading and trailing edges are most important.
Kevin D. Huff, D.D.S., M.A.G.D., Spear Visiting Faculty member, SpearTalk Moderator, Spear Digest contributing author - dr@doctorhuff.net