When Should I Order an MRI?
The Piper MRI protocol provides restorative dentists, specialists, and patients with valuable insight into TMJ health. MR imaging helps assess TMJ anatomy in patients with a high likelihood of structural changes.
These patients often present with malocclusion, pain, or both. In most cases, malocclusion appears first, while pain lags behind — just as in other joints where structural alterations precede discomfort.
Choosing a Condylar Position for Occlusion Assessment
When evaluating occlusion, dentists must decide which condylar position to use:
- Fully-seated condylar position (centric relation if the TMJ is intact)
- Maximum intercuspation
Although many patients function in maximum intercuspation, the fully-seated condylar position offers richer diagnostic information. It allows dentists to assess anterior tooth relationships both horizontally and vertically, revealing how close the anterior teeth are to providing guidance in excursive movements. Under normal growth and development, canines typically sit close to providing that guidance.
Identifying Signs of TMJ Structural Change
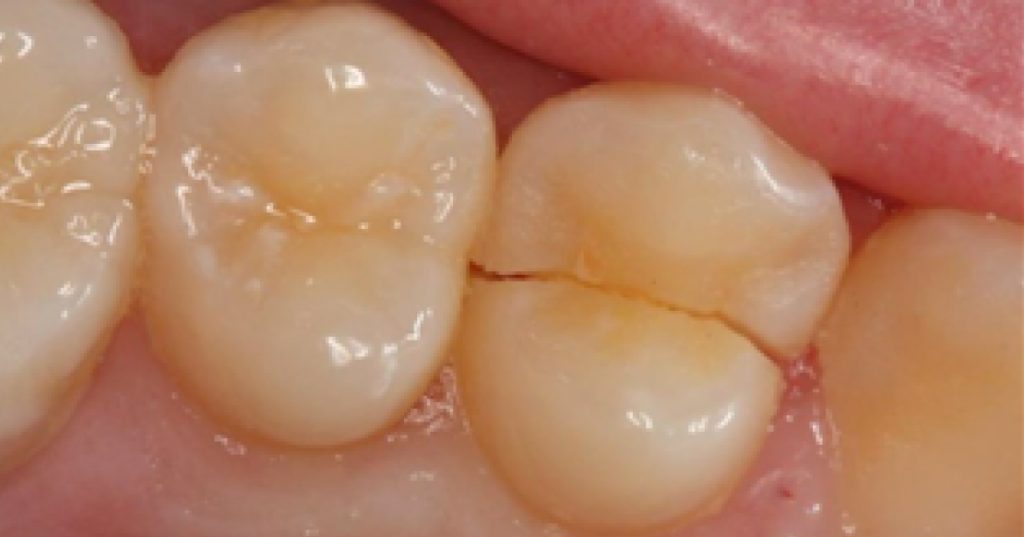
If canines are uncoupled by more than 2.0 mm, the cause may be a loss of vertical dimension in the TMJ. Structural changes usually begin with soft tissue breakdown, which alters anterior tooth contact. Recognizing these changes helps dentists identify structural issues — often before pain develops.
This is especially critical in growing patients, where TMJ changes can occur frequently without pain.
The Limits of Maximum Intercuspation
In maximum intercuspation, muscles can shift the mandible forward, masking structural problems. Tooth-level evaluation allows teeth to hide skeletal defects, while skeletal-level evaluation (fully-seated condylar position) gives a clearer picture of TMJ health.
Key Assumptions in Fully-Seated Condylar Evaluation
When assessing occlusion in a fully-seated condylar position, dentists should keep two assumptions in mind:
- Tooth position has not been altered by orthodontic, restorative, or orthognathic treatment. If it has, clinicians must account for it.
- Teeth are in normal three-dimensional position. Retroclined anterior teeth or supraerupted teeth may require the dentist to visualize them in a normal orientation to properly evaluate occlusion.
The Role of Load Testing
A fully-seated condylar position also allows dentists to use load testing to assess pain. This test reveals whether joint tissue can be compressed under functional forces without discomfort.
- Positive light loading (pain present): Often suggests structural alterations.
- Negative light loading (no pain): Does not guarantee joint stability, since some altered TMJs can still be loaded without pain.
When to Order an MRI
Dentists should consider an MRI when:
- Patients show anterior tooth uncoupling that suggests loss of TMJ dimension.
- Light compression of the TMJ produces pain.
As with other dental conditions, patients must understand both the problem and the benefits of MR imaging before moving forward. Clear knowledge of TMJ structure allows dentists and patients to make informed decisions and pursue treatment with greater predictability.
VIRTUAL SEMINARS
The Campus CE Experience
– Online, Anywhere
Spear Virtual Seminars give you versatility to refine your clinical skills following the same lessons that you would at the Spear Campus in Scottsdale — but from anywhere, as a safe online alternative to large-attendance campus events. Ask an advisor how your practice can take advantage of this new CE option.

By: Jim McKee
Date: August 16, 2018
Featured Digest articles
Insights and advice from Spear Faculty and industry experts