The Point of the First Point
Ignorance is bliss. The more you know, the more you care. The more you care, the more you want to know more. And so it goes. When we were all in dental school, it was just easier. This “idea” of centric relation was no more than a mention in a lecture on the mandibular jaw relationship relative to its position in the glenoid fossa and its relation to the maxilla. It was part of the lecture only. There was no practical application, no clinical relevance (at the time, of course), and it was never discussed further than those lecture halls.
And that’s OK. Dental school was hard enough, with never enough time to discuss and apply the most practical applications that were gospel and driven into our souls. Learning and dealing with just one jaw position, the maximum intercuspal position, was plenty to figure out how to put people back together.
Do I delve into all the translations of what Centric Relation means to so many different clinicians or sects of dentistry? The Journal of Prosthodontic Terms lists the following:
centric relation \sĕn΄trĭk rĭ-la΄shun\: acronym is CR; a maxillomandibular relationship, independent of tooth contact, in which the condyles articulate in the anterior-superior position against the posterior slopes of the articular eminences; in this position, the mandible is restricted to a purely rotary movement; from this unstrained, physiologic, maxillomandibular relationship, the patient can make vertical, lateral or protrusive movements; it is a clinically useful, repeatable reference position. — Journal of Prosthodontic Terms
But there are many academic arguments about what it means, what position the condyle assumes, and where it is in the fossa. For brevity, and because of my extensive studies with The Pankey Institute and Spear Education, I ask that we consider centric relation as:
The relationship of the maxilla to the mandible when both condyles are seated in the most anterior, and superior portion of the Glenoid fossa.
During my time with Spear Education, things have changed with how the resident faculty and we visiting faculty think about and verbalize “that” jaw position that used to be thought of as so mystical. To dispel the mysticism, we provide simple clinical methods to achieve what we mostly refer to as a “fully seated condylar position.” This keeps the ganthologists and occlusal scholars at bay, so we may move forward and evaluate the position and use it simply as a place to plan from.
And so it goes — the years, I mean. Patient after patient, visit after visit, tooth after tooth. You see things. You learn things. You learn that you need to learn. As time passes, you discover just how different so many dentitions are.
Why are they so different? How many variations can there be to how a maxilla relates to a mandible? There are only skeletal Class I, II, and III classifications with some subdivisions; jaw positions can vary with cross bites, discrepancies in the sizes of the maxilla to the opposing mandible, and so on. But we now know it is not the relationship of the maxilla to the mandible when the mandible is at rest. Indeed, no. The variations come from what the patients do with their mandible when moving. That is when all variations result, where and how any singular dentition becomes personalized.
The Mandibular Positions Requiring Evaluation
- MIP/ICP — maximum intercuspal position or intercuspal position (to some); a patients’ acquired bite, the one they live in everyday, the bite du jour; the place where the entire dentition comes together best or is most comfortable; or so it seems (more on this later); this is ALWAYS subject to change; incidentally, it is the position where the vast majority of dentistry is fabricated or executed.
- End to End — the relationship of how the maxilla and mandible relate to one another when someone is articulating on their incisal edges in the anterior segment; it can be two, some, or all teeth meeting in the anterior segment.
- Pathway and Crossover — the pathway component is simply the lateral movement of the mandible as well as the anterior movement of the mandible just short of the point of it coming into the end-to-end position; think of it as anywhere between maximum intercuspal position and the end-to-end position; the crossover component is the position as the mandible continues laterally so much that the cuspids pass one another; the same for the incisors as the mandible protrudes forward and the incisal edges pass.
- Retruded/A Seated Condylar Position – when the mandible moves posteriorly, behind MIP, and the patient seats their condyles; This is your Holy Grail, right? Seated condyles. Not so much when the patients move there on their own;
This article is, in fact, this former position. The hope is to simplify its purpose and create invaluable data about a Fully Seated Condylar Position (FSCP) and the first place teeth touch in this arc of closure. But at the end of this piece, I add a new wrinkle provided by my friend and newest resident faculty at Spear Education, Dr. Jim McKee, which may change everything relative to planning certain cases with retrusive wear.
When participants come to Spear Education for the Treatment Planning With Confidence workshop, admittedly, they are given a great deal of information in a short and concentrated three days. Our job as visiting faculty is to help them sift through and decipher ways to manage and implement what they are learning. You cannot go home to your office and implement everything right away, can you? But there are a number of tools you can immediately add to your toolbox, all you have to do is trust the process and practice on as many people as you can find: friends, family, staff, colleagues, and yes, even patients, because they love you and believe it or not would love to help be a part of your journey into advanced methods of education.
One of the tools of utmost importance is finding the Holy Grail, the first point of contact in an FSCP. Furthermore, determining the degree of slide from the initial point of contact to MIP is even more relevant. Further still, we can measure the degree of slide in three different vectors:
- Vertical
- Anterior/Posterior
- Horizontal
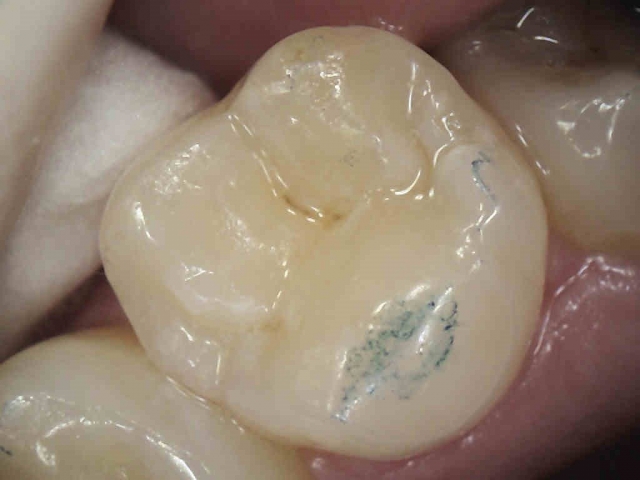
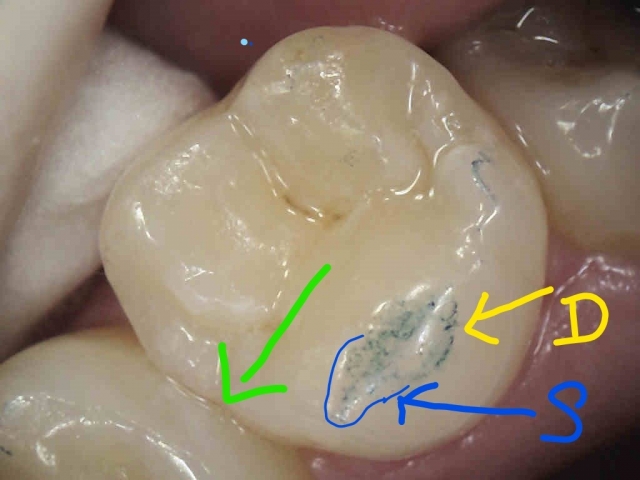
During the workshops in our small groups, I emphasize how important this information is to record in every patient’s chart, regardless:
- Of the level of treatment they accept
- Of whether they have muscle or joint pain
- Of whether they exhibit wear patterns on teeth coincident with the aforementioned mandibular movements and positions
- Of whether you have a pristine dentition that requires no treatment
- Of whether you plan on treating the two teeth you happen to find to be the initial point of contact
Because someday, you may have to change that tooth. And if you have to alter the tooth, AND if you are not aware it is the first point of contact, AND the degree of slide associated, you may find yourself in an unenviable position, a position so many of us have been in clinically but did not know until we studied to know enough to look before we leap. We have all been there! As stated before, most of the dental universe works in MIP, and so many times, that is fine to treat there. Unfortunately, there are so many dentitions with significant dental issues that are unbeknownst to the patient.
Attention Please
One of the most challenging things to do in dentistry is to prepare a tooth for occlusal coverage restoration: crown or onlay, where you are altering the entire occlusal portion. Suppose that tooth is your initial point of contact, and you alter its height. In that case, it’s no longer in the way of the arc of closure; the lateral pterygoid muscles that worked so hard in posturing the jaw away from that initial interference, now can relax a bit or entirely (depending on the degree of slide). And if the lateral pterygoids relax, then the condyles can seat. And when they seat, there is a dimensional change vertically, and all of a sudden, the preparation space you worked so hard to create for your crown is gone (yes, the opposing tooth may even touch the newly prepared tooth), BUT you do not know why. The patient is not biting differently — you moved furniture in the way. But whether or not you lose all of the height depends on the degree of the slide.
This is just one of the reasons why working the patient up comprehensively with mounted models in an FSCP, a muscle and joint exam, and photographs is so important, especially in circumstances where the teeth you see may not look age-appropriate for that patient. Other patients who might benefit from finding the initial point of contact:
- patients who cannot find their bite
- patients who complains of muscle pain
- patients who claim they have “TMJ”
- patients with actual joint pain, internal derangement
- patients who complain of localized and generalized tooth sensitivity
- patients who requires significant rehabilitation of their dentition
- ANYONE you plan on making a segmental appliance for, such as an anterior bite plane
This last bullet point is so important. Why? If you make a segmental appliance, even the anterior bite plane taught in the Spear workshops:
- AND you do not measure the slides from FSCP to MIP, especially the vertical slide
- AND the vertical slide is significant (2.0+ mm, for example)
- AND the lateral pterygoid was working hard to posture the mandible forward
- AND you did not know it
- AND you got it to relax on the anterior bite plane,
The lateral pterygoids may lose memory, the mandible may retrude, and the occlusion may change, likely leaving the patient with an anterior open bite. Frank often speaks of this in workshops, seminars, and the online video library. It was never my experience
This finally happened to a patient of mine who barely had a 2.0 mm vertical slide, had an existing anterior open bite, and wore a Quick Splint (an anterior-only prefabricated appliance) for a couple of months as a diagnostic tool to discern her symptoms as either muscle or joint. She wore it only at night, as nocturnal bruxing was considered the source. Yes, even though she was evaluated thoroughly, it happened anyway.
Record Your Data
One way to record this data in an easily-accessible way is by making notes like this in the patients’ chart, provided you still use charts:
FPC – #2 with #31 Leaves – 12
V A/P H
_____________________________________________
FSCP 9 7 3
MIP 7 4 3
______________________________________________
Slide 2 3 0
The next example, using images from the Treatment Planning With Confidence workshop, is how to measure the slide clinically:
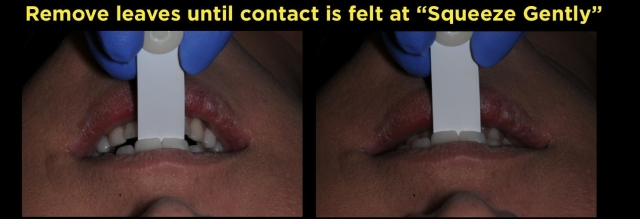
- After identifying the first point of contact (FPC) – while holding a leaf gauge behind the maxillary centrals with enough leaf thickness to separate the posterior teeth, having the patient move their mandible forward, back, and then having them use their master muscles to squeeze lightly, or half-hard; keep removing leaves until the patient feels two teeth bump or glance each other
- To measure the slides, see the images below.
- Move the leaf gauge laterally; measure all three positions using the SAME reference point for FSCP and MIP, examples:
- Vertical — the free gingival margin of the same lower incisor to the incisal edge of the same upper incisor
- Anterior/Posterior — the facial of the same lower incisor to the incisal edge of the same upper incisor
- Horizontal — the difference in the midlines 8-9 relative to 24-25
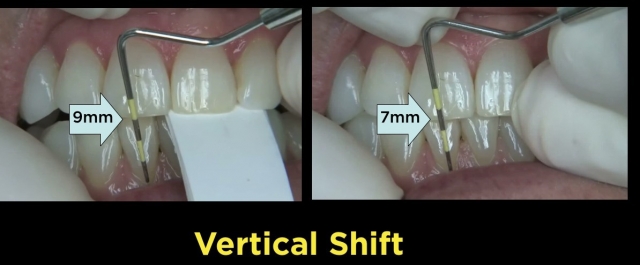
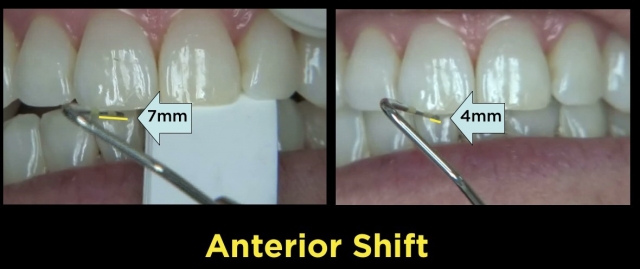
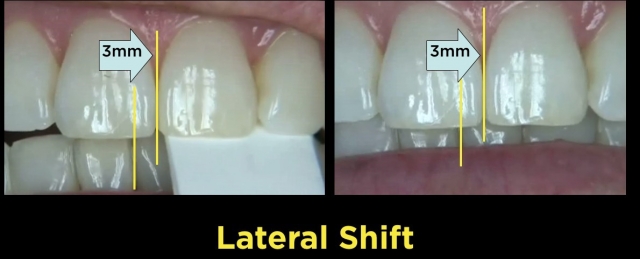
Bring It All Together
If you get into a habit of at least gathering FPC and slides, the following has a great chance of happening:
There will come a time when the tooth with the FPC requires treatment, and the patient will be ready. You have recorded the data in the chart, dusted it off, and shared this information with them.
Explain that this tooth is different, and treating teeth with crowns, crownlays, or onlays is not always the same. Explain that altering this tooth will likely change their daily bite, and you are uncertain how (because you have not gathered all of the data) or what changes may occur. Explain that this tooth gets in the way of another before all the teeth come together, essentially the reason the tooth is worse. Once the tooth is altered, it may cause another group of teeth to touch in ways they have not. You should even go so far as to explain that you are NOT comfortable treating this tooth unless their system is evaluated further. Ask them if it is OK to look further so that things may be more predictable during treatment. This nearly always leads to:
- A comprehensive exam — muscles, joint, mounted models in FSCP, photographs
- Trial equilibration — adjusting teeth on models until all of the bite interferences and deflections are gone, and teeth touch simultaneously. There is certainly more to it, but it gives you a road map as to what happens after altering the FPC, and so on.
Most patients are not accustomed to this type of analysis. Ask their permission to perform some or all of the things you learned in the Treatment Planning With Confidence workshop. Get them involved and do it together (co-discovery). Explain in simple ways that jaws do not close like door knockers — that specific muscles help jaws fit together as best they can, but it does not mean it is the best fit.
The Wrinkle: Beware of Long Slides
In September 2016, at the annual Spear Summit, Jim McKee, DDS, presented new ways of thinking about diagnosing occlusal problems and TMD. This is an article in and of itself and will be one in the near future.
He suggests we are first looking in the wrong place: the teeth. His newer beliefs are that we were trained to look at the front end of the mechanism first, the teeth, and the subsequent occlusion. Then, if necessary, look at the back end of the mechanism, the temporomandibular joint. And with that, only look at it if there are signs and symptoms. It was ingrained in us in academics that “bad bites make bad joints,” says Jim.
He believes we should start with the joint, both the hard and soft tissues: the disc, the condyle, and the fossa, then work back to the occlusal scheme and discern a relevance between the two. Hence, “it’s bad joints that make bad bites.”
One very relevant circumstance of how the anatomy of the joint can give clues and change how we treat patients is when there is a long vertical slide from FSCP to MIP. This is where it got interesting to me and everyone else listening. Jim believes that if a vertical slide is greater than the thickness of the disc (2.0 mm), then there is something awry with the joint itself, be it:
- A thinning of the disc
- A reshaping of the condyle (degenerative)
- A loss of the disc forward
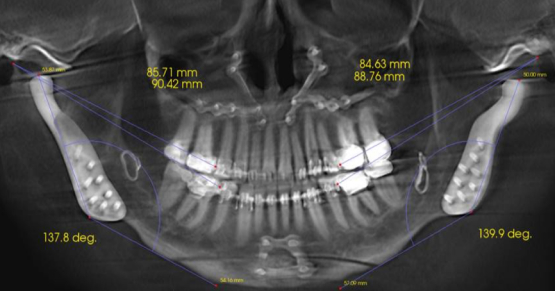
After gathering data from a comprehensive exam, there should be cause for concern if you record a vertical slide, especially greater than 2.0+ mm. Longer slides of 2.0+ to 4.0 mm often correlate clinically to those patients with troughed out mandibular second molars, #18 and #31, where the four second molars often look and act like a mortar and pestle. #2 and #15 may appear as having a deep plunging palatal cusp, with long facets on inclines. Below is an example of significant wear predominantly on the distal half of the second molars. Note the mirror image AND the actual teeth looking posteriorly without the mirror.
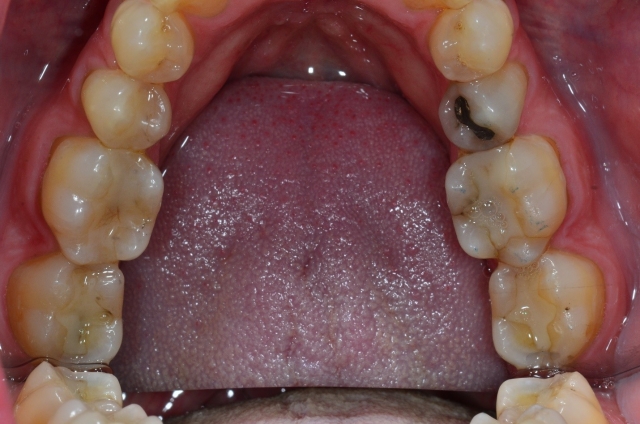
Here is another example in another patient. Note the significant wear on #18. Both male patients had vertical slides greater than 3.0 mm.
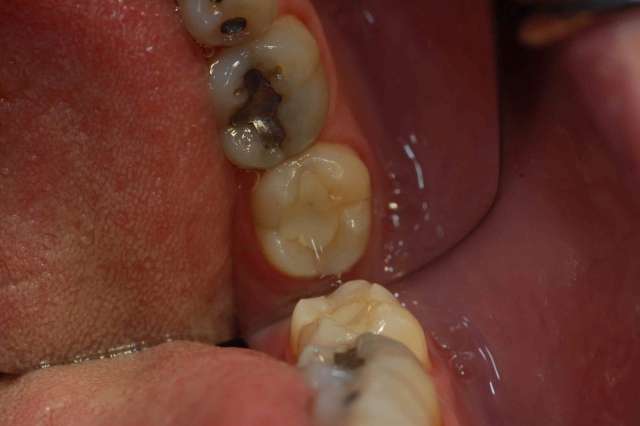
In a future article, we will delve deeper into thinking about the joint before occlusion. Just feel fortunate you can learn from Jim McKee, DDS, in an intimate small group of about 30 people in the Treatment Planning With Confidence and Occlusion workshops, and receive groundbreaking insight from one of the finest minds on joints and occlusion.
And so it goes, more patients, another day, but how different are you since you started your journey? Are you better equipped than yesterday? For those of you who come to Spear Education for the Treatment Planning With Confidence and the Occlusion workshops, practice and use your new skills. This one bit of data can be significant in your growth, confidence, and peace of mind.
Find that first point of contact: log it, use it, study it, teach it, and plan from it — those considering an advanced understanding of your craft should consider visiting Spear Campus. Immerse yourself in the available content, find a local Spear Study Club, and we will help you further understand The Point of The First Point. Thank you for reading — I hope it was helpful.
SPEAR STUDY CLUB
Join a Club and Unite with
Like-Minded Peers
In virtual meetings or in-person, Study Club encourages collaboration on exclusive, real-world cases supported by curriculum from the industry leader in dental CE. Find the club closest to you today!

By: Dave St. Ledger
Date: August 22, 2018
Featured Digest articles
Insights and advice from Spear Faculty and industry experts