Nasal Breathing: Keystone to Oral and Systemic Health
Dr. Maurice H. Cottle suggested more than 40 years ago that sleep patterns are, in great measure, dependent on good nasal function.1 Muscle tone in the oropharynx is partially regulated by airflow receptors in the nose, maintaining a patent airway.2 Smooth laminar flow provided by nasal breathing is more conducive to improved sleep and greater release of nitric oxide from the paranasal sinuses, which dilates blood vessels, reduces swelling and congestion, and improves lung oxygen transfer.
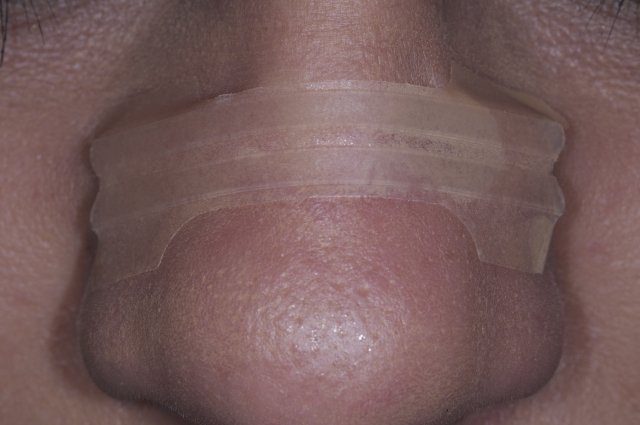
It has been estimated that between 10% and 25% of children mouth-breathe while they sleep; most are not obligate mouth-breathers but have significant periods during their sleep when they breathe through their mouths. The vast majority of nocturnal mouth-breathers will also breathe orally during wakefulness.
Impact of mouth breathing on overall health
It’s becoming more accepted that habitual mouth breathing and/or snoring in children is abnormal. Not only does this make them more prone to neurocognitive alterations like ADHD, but it can also lead to changes in craniofacial growth and development, making subjects more prone to the development of sleep-disordered breathing years later.3
Mouth breathing may also explain an increased risk factor for common dental problems. Mouth breathing during sleep is responsible for decreased intraoral pH compared with nasal breathing patients. This is suggested to be a causal factor in caries and erosion.
Furthermore, one of the most crucial host response factors in periodontal disease is mouth breathing and airway compromise. For more than 40 years, it’s been known that mouth breathing is responsible for higher gingival and plaque indices. Current periodontal research notes that disease control and surgical healing are improved when the airway dysfunction is controlled. The compromised airway and mouth breathing alter the oral flora and increase inflammation in mouth-breathers.
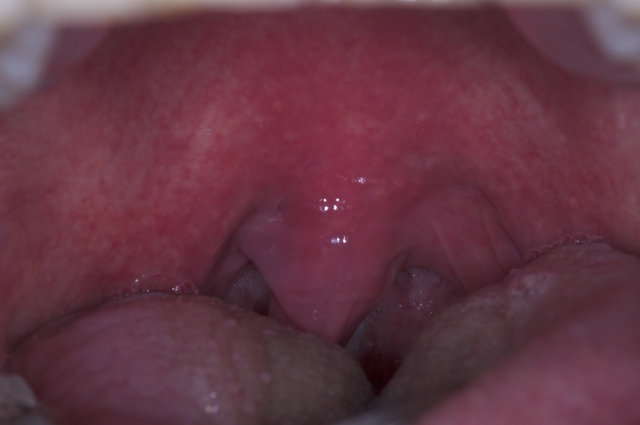
An Italian study recently looked at 10 patients with severe apnea, 10 with mild apnea and snoring, and 10 patients with only nasal impairment and monitored them for inflammation. Urine and blood biomarkers for oxidative stress showed no significant difference between the levels of the three groups. This suggests that the lack of nasal breathing is the key to controlling the pathogenesis of apnea.4
Lastly, obstructive apnea and hypopnea are significantly more frequent when breathing orally (AHI 43 + 6) than nasally (AHI 1.5 + 0.5).5
Restoring nasal breathing capacity
Decongestants and nasal dilators can have a dramatic effect on sleep. Subjects with moderate obstructive sleep apnea (OSA) with significant nasal turbinate obstruction and normal retroglossal airway dimension showed an average Apnea-Hypopnea Index reduction of 12 events per hour, improved sleep efficiency, and increased REM and Stage 3 NREM sleep, compared with placebo controls with the use of nasal spray.6 The number of apnea events from a sizable increase in flow-limited breathing will significantly increase in patients with abnormal nasal structures.7
A recent report demonstrates that upper airway resistance syndrome (UARS) is primarily a nasal issue.8 UARS subjects demonstrated an increased frequency of “altered nose”: septal deviation, inferior turbinate hypertrophy, or other airflow obstruction.
Furthermore, UARS subjects had significantly more complaints of oropharyngeal dryness, indicative of MB during sleep. Therefore, the nose has a key role in the physiopathology of the disease and should always be thoroughly assessed in a patient diagnosed with UARS.
The treatment of our airway patients is not complete until nasal breathing has fully recovered both day and night. Myofunctional and Buteyko techniques for achieving this goal will be discussed in detail as these concepts are developed at Spear Education.
References
- Cottle MH (1968). Clinical benefits and disorders following nasal surgery. Southern Medical Journal, 61(12), 1281-1286.
- White, DP, Cadieux RJ, Lombard RM, Bixler EO, Kales A, Zwillich CW. (1985). The effects of nasal anesthesia on breathing during sleep. American Review of Respiratory Disease, 132(5), 972-975.
- Guilleminault C, Akhtar F. (2015). Pediatric sleep-disordered breathing: new evidence on its development. Sleep Medicine Reviews, 24, 46-56.
- Passali D, Corallo G, Petti A, Longini M, Passali FM, Buonocore G, Bellussi LM. (2016). A comparative study on oxidative stress role in nasal breathing impairment and obstructive sleep apnoea syndrome. Acta Otorhinolaryngologica Italica, 36(6), 490.
- Fitzpatrick MF, McLean H, Urton AM, Tan A, O’donnell D, Driver HS. (2003). Effect of nasal or oral breathing route on upper airway resistance during sleep. European Respiratory Journal, 22(5), 827-832.
- McLean HA, Urton AM, Driver HS, Tan AKW, Day AG, Munt PW, Fitzpatrick MF. (2005). Effect of treating severe nasal obstruction on the severity of obstructive sleep apnoea. European Respiratory Journal, 25(3), 521-527.
- de Godoy LB, Palombini LO, Martinho Haddad FL, Rapoport DM, de Aguiar Vidigal T, Klichouvicz PC, Togeiro SM. (2015). New insights on the pathophysiology of inspiratory flow limitation during sleep. Lung, 193(3), 387-392.
- de Oliveira PWB, Gregorio LL, Silva RS, Bittencourt LRA, Tufik S, Gregório LC. (2016). Orofacial-cervical alterations in individuals with upper airway resistance syndrome. Brazilian Journal of Otorhinolaryngology, 82(4), 377-384.
VIRTUAL SEMINARS
The Campus CE Experience
– Online, Anywhere
Spear Virtual Seminars give you versatility to refine your clinical skills following the same lessons that you would at the Spear Campus in Scottsdale — but from anywhere, as a safe online alternative to large-attendance campus events. Ask an advisor how your practice can take advantage of this new CE option.

By: Jeffrey Rouse
Date: May 27, 2017
Featured Digest articles
Insights and advice from Spear Faculty and industry experts


