Understanding and Recognizing Mouth Breathing
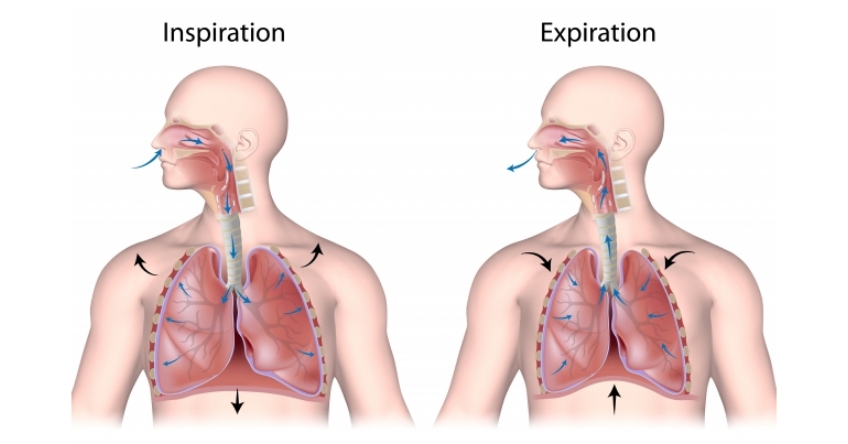
Physiology of Breathing
Normal breathing is done through the nose. Each nostril functions independently and synergistically to filter, warm, moisturize, dehumidify, and smell the air.
Babies are born obligate nose breathers, but somewhere along the way, nose breathing can change to mouth breathing, with dire consequences. The most obvious adverse effect of mouth breathing is dryness of the oral and pharyngeal tissues, leading to inflamed tonsils, tonsil stones, dry cough, swollen tongue, halitosis, gingivitis, and caries.
Normal respiration follows a gentle wave pattern with 10 to 12 breaths per minute. Mouth breathers take too many breaths, with rates from 12 to 20 breaths per minute or more. Breathing delivers oxygen to the body’s cells and removes excess carbon dioxide. Carbon dioxide is produced as a byproduct of exercise and the digestion of food. Carbon dioxide plays a significant role in the release of oxygen from hemoglobin. It also triggers breathing, maintains blood pH, and prevents smooth muscle spasms. All of these functions are reduced or impaired in mouth breathers.
Surprisingly, oxygen is absorbed on the exhale, not on the inhale. The back pressure created in the lungs with the slower exhale of nose breathing allows more time for the lungs to transfer oxygen to the blood. This exchange requires carbon dioxide. Exhaling through the mouth blows the carbon dioxide out too quickly, absorbing less oxygen. Nasal breathing results in more oxygen being absorbed because nitric oxide is released in the nasal cavity and inhaled with nose breathing. Nitric oxide increases the efficiency of oxygen exchange by 18%. No nitric oxide is inhaled with mouth breathing; therefore, less oxygen is absorbed. The reduced oxygen absorption leads to sleep, stamina, energy level, and ADHD problems. Children diagnosed with ADHD may, in fact, be mouth breathers who are sleep deprived.
With nasal breathing, the tongue rests against the palate without touching the teeth. In this position, the tongue provides passive pressure that stimulates stem cells in the palatal suture and within the periodontal ligaments around all the teeth, directing normal palatal growth. The teeth erupt around the tongue, producing a healthy arch form. The tongue’s lateral pressures counter the buccinator muscles’ inward forces.
What Goes Wrong With Mouth Breathing

Several things go wrong with mouth breathing. The low carbon dioxide levels associated with mouth breathing lead to overbreathing or hyperventilation. With less oxygen being delivered to the brain, muscles, and all the body’s cells, the body functions less than optimally. Sleep is often disturbed and of poor quality, leaving the mouth breather tired in the morning and feeling fatigued mid-afternoon. As the mouth dries out, the pH of saliva drops, leading to increased caries. This dryness and lack of air filtration in mouth breathing causes enlarged and inflamed tonsils and adenoids, and increased risk of upper respiratory tract infections. Lower carbon dioxide levels cause smooth muscle spasms associated with gastric reflux, asthma, and bed wetting. Smooth muscle is found throughout the body — in the respiratory, digestive, and circulatory systems.
With mouth breathing, the tongue is down and forward, allowing the buccinator muscles to push unopposed, causing the upper arch to collapse. Children who mouth breathe have an underdeveloped, narrow maxilla with a high vaulted palate. They develop a retrognathic mandible and generally have a long face. This is known as long face syndrome.
Some think the long face syndrome associated with mouth breathing is dictated by genetics rather than breathing. To see if mouth breathing alone could change jaw development and occlusion, Dr. Egil Harvold and his team tested this idea in monkeys. They artificially switched nose-breathing monkeys to mouth-breathing by surgically blocking their noses with silicone plugs. The monkeys were uncomfortable with the new mouth breathing, but eventually adapted; all developed changes in their jaws and malocclusion.
Mouth-breathing-related problems of skeletal development will set children up for obstructive sleep apnea later in life. In addition to changes in both maxilla and mandible development, the airway is constricted, predisposing the child to sleep problems.
It may seem logical that mouth breathing occurs because the nose is congested, but that is not always true. The brain of a mouth breather thinks carbon dioxide is being lost too quickly from the nose and stimulates the goblet cells to produce mucous in the nose to slow the breathing. This creates a vicious circle of mouth breathing, triggering mucous formation and blocking nasal passages, leading to more mouth breathing. So, in fact, mouth breathing can cause nasal congestion, leading to more mouth breathing.
Recognizing Mouth Breathing
Determining if someone is a mouth breather is not always easy. Some people admit they always breathe through their mouth. Others believe they are nose breathers, but if you watch them, their mouth is open most of the time. Sitting still, they may have their mouth closed, but if they get up and walk across the room, their mouth is open. Chewing with the mouth open may be done so the person can breathe while eating. One sign of mouth breathing is an addiction to Chapstick or lip gloss. An open mouth leads to drooling, both awake and asleep, causing chapped lips and a tendency for mouth breathers to lick their lips frequently. Closed-mouth lip seal is efficient at keeping saliva in and air out, but chronic mouth breathers may find it very difficult to hold their lips together.
Mouth breathing at night dries the tissues, so the mouth, teeth, tissue, and throat are all dry upon waking. Always having a glass or bottle of water at hand might signal systemic xerostomia, but it is also a sign of mouth breathing. If someone wakes with a dry mouth, they are likely a mouth breather at night, which means they are also likely mouth breathing during the day.
Dental hygienists are in the perfect position to recognize mouth breathing. Before asking patients to “open wide,” check first for mouth breathing.
SPEAR ONLINE
Follow a Clear Path to Clinical and Practice Confidence
Next-level confidence isn’t random. It’s structured. Follow a clear pathway that will accelerate your clinical and practice progression.

By: Abigail Pfeiffer
Date: January 17, 2022
Featured Digest articles
Insights and advice from Spear Faculty and industry experts


