Pontic Design Considerations: A Comprehensive Review
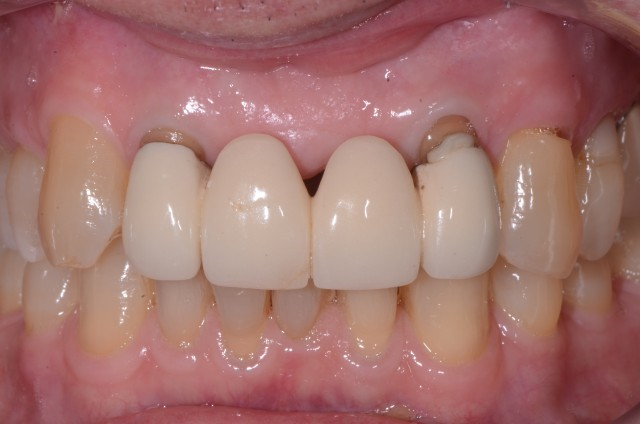
I recently had a 70-year-old patient present for the replacement of his bridge. He had it for 50 years. It was placed after an automobile accident when he was in college, and I was impressed how well it had serviced him.
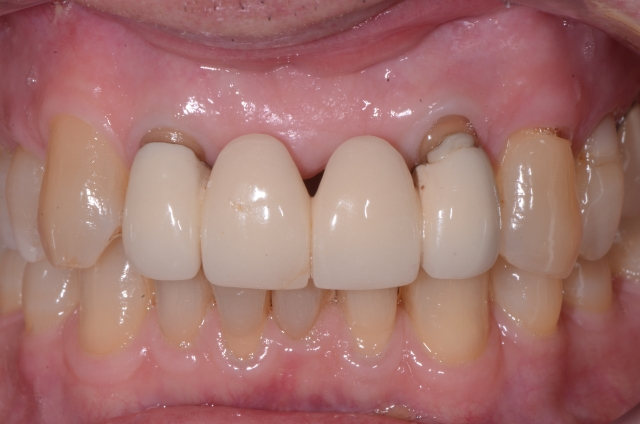
I knew that the remaining edentulous ridge might be a challenge, so I began my conversation with the difficulties involved in trying to make the artificial teeth look individual and natural. In the end, he was not interested in developing the ridge. He doesn’t have a high smile line, and he wanted the treatment completed in a more timely way.
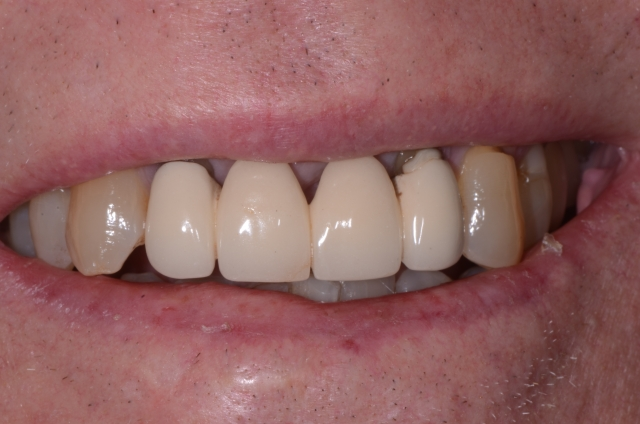
It did bring up lengthy conversations with the lab technician about how they design pontics based on the cases they receive. (And it’s usually the lab technicians who are designing the pontics.)
These discussions occur routinely in the lab: It’s a daily little topic of discussion but a big subject. The lab receives the model work and then the technician wonders exactly what type of pontic they’re supposed to design. It’s a fairly common occurrence that the design is not chosen on the prescription form despite a check box for it. If one is checked, how often do you give additional information?
Pontic shapes
Most laboratory prescription forms will give you the option to select one of four types of pontic shapes. A quick summary describes the types this way:
- Hygienic: Readily cleanable and great for the health of the tissue, but not at all esthetic.
- Ridge lap. Laps over both sides of the ridge like a saddle thrown over the back of a horse. It’s fairly esthetic but not cleanable, and can result in chronic tissue irritation.
- Modified ridge lap. Designed so the saddle laps over the buccal side only. The shape and size of the ridge and restoration dictate the lingual design. It curves in and leaves the lingual ridge exposed. It is fairly esthetic and more cleanable than the full ridge lap.
- Ovate. Designed to look like an egg or bullet. It is ideal for anterior teeth; however, it’s not limited for posteriors, because it is highly esthetic and cleanable. It is developed by a depression created in the residual tissue ridge that mimics the shape of the natural root and crown. The tooth looks as if it is growing out of the gum tissue and not just resting on top of it. If you demand the best esthetics available, and the least maintenance, the ovate pontic is the best choice.
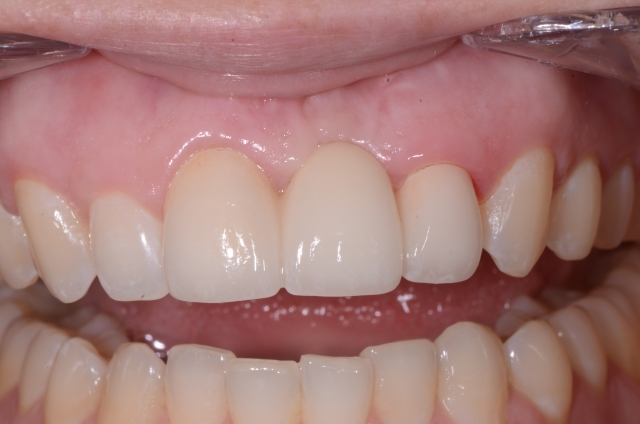
Ideally, making an ovate pontic shape would give the best result, but it takes another level of knowledge and skill by the clinician to develop this. It also takes patience and time, and is ideally accomplished immediately after the tooth is extracted.
Questions lab techs have
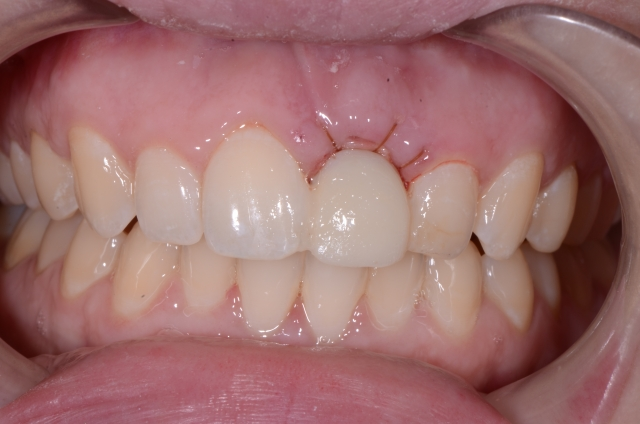
When the lab is faced with a pontic space, they have to consider what type of pontic is best for the existing ridge. They spend much time discussing how to design what might look best on the ridge. Sometimes the tissue is so irregular that a technician will have no idea how to design around it. Yet are we doing them and our patients the best service by not specifically addressing it with the tech?
Here are some of the questions that lab technicians have to guess answers for every day:
- Should they grind out a model or design around it?
- If it’s a modified ridge lap, where exactly and how much should they adjust the lingual?
- If it’s an ovate pontic, how many millimeters into the cast should they grind it?
- If the bridge goes to completion with an ovate pontic shape and you haven’t previously shaped the tissue, how will you get the bridge to seat?
- Are you prepared to modify the tissue accordingly?
Did you know that ovate pontics in the posterior site come in different shapes — bullet and square? It’s difficult for the tech to get the shape and size correct on these posterior sites.
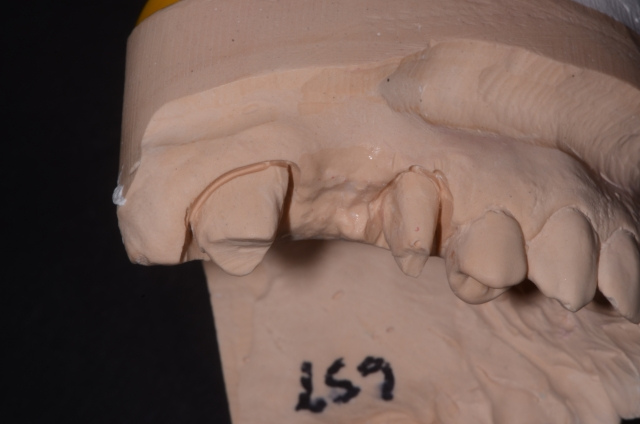
Some technicians think that “modified ridge lap” means modify the cast, not the overall shape of the actual design.
Technicians tell me that the edentulous areas where a fixed partial denture is to be provided may be overlooked during the treatment-planning phase. Conversely, some deficiencies may arise during the fabrication of a bridge pontic if adequate healing time after extraction is not appreciated. These issues are identified only after the teeth have been prepared or the existing bridge removed, or even when the definitive cast is at the lab.
Pontic design principles
The residual ridge needs to be carefully analyzed for mesiodistal width, buccolingual dimension and occlusocervical distance. An ideally shaped ridge has a smooth and regular surface of attached gingiva. It should have adequate facial height to sustain the appearance of a papilla. The problems of an insufficient residual ridge can include black triangles, unnatural esthetics, food impactions, and saliva percolation during speech. We often will have to manage these issues with our pontic design.
To design a pontic that meets hygienic requirements and prevents irritation of the tissue, one has to be attentive to the form and shape. The form and shape must incorporate mechanical principles for strength and longevity.
- Biologic principles. These include cleanable tissue surface, access to abutment teeth, and no pressure on the ridge.
- Mechanical principles. These include strong connectors to prevent fracture, rigidity to resist deformation, and material choice to resist porcelain fracture.
- Esthetic principles. These have to include looking like the tooth it’s replacing, appearing to “grow” out of the ridge, and having space for porcelain design.
The pontic assumes a dynamic role as a component of the prosthesis and cannot be viewed as an “insert” of material.
When considering pontic design in the posterior region, the contours can be modified in the interest of oral hygiene, but these can be difficult to design. Very few clinicians will spend the time creating an ovate shape, and it’s less predictable than developing an anterior bullet-shaped tissue profile. The resultant pontic shape will be more square or triangular. Often the ridge is too thin for this, which is why the modified ridge lap is the most-utilized design in the posterior.
Postlaboratory modifications
There is no lab standardization in designing pontics: If a cast has to be modified, there’s a good chance that each technician in the same laboratory will do it differently. This is why it’s important to describe exactly how much you want the tissue on the cast modified. Photographs and drawings are always helpful to the tech when getting started.
If the lab tech modifies your cast 1 mm, you can probably get the fabricated bridge to seat. But if it’s supposed to duplicate an emergence profile of an adjacent tooth, the cast has to be carved more aggressively. The dentist needs to know that this will be completed; it provides a heads-up to be prepared to adjust tissue on the insert appointment.
Many dentists are not comfortable adjusting in the mouth what is necessary. If they don’t adjust the tissue the same way the cast was adjusted, the bridge won’t seat. The clinician will then have to adjust the pontic, which the technician spent so much lab time developing. The unfortunate result is that it often won’t look esthetic at all, because both sides are guessing.
Additionally, the labs will often get a request to add more material to the pontic site. The question, though, is will the material choice accommodate this?
Full contour and full metal cannot be modified except for reduction and, even then, there is always the risk of microfractures. If you request additional material, the lab will usually incur the cost of that additional procedure. Therefore, pontic design, especially when replacing an existing bridge, needs to specifically be addressed just as you would the length and shape of the abutment teeth.
I will readily admit that for many years of practice, I never gave instructions. My expectation was that the bridge would be returned with a pontic shape that looked appropriate and was cleanable. I didn’t have any sense of how difficult that could be for the technician to design. There were times when an ovate pontic shape was made because the technician knew that would “look best,” but I was not comfortable modifying the tissue intraorally or telling a patient to see the surgeon to have this done.
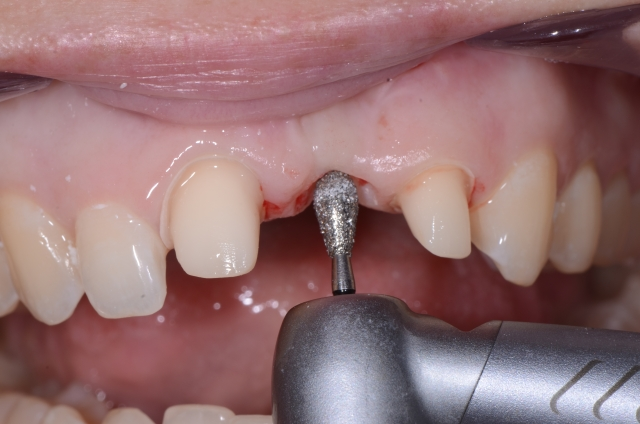
The laboratory technicians understand that when designing pontic shapes around implants, the challenges can increase dramatically. This requires, at the very least, a verbal conversation with the restorative dentist, but if tissue hasn’t been clinically managed, then a design choice by the dentist — not the tech — must be accomplished.
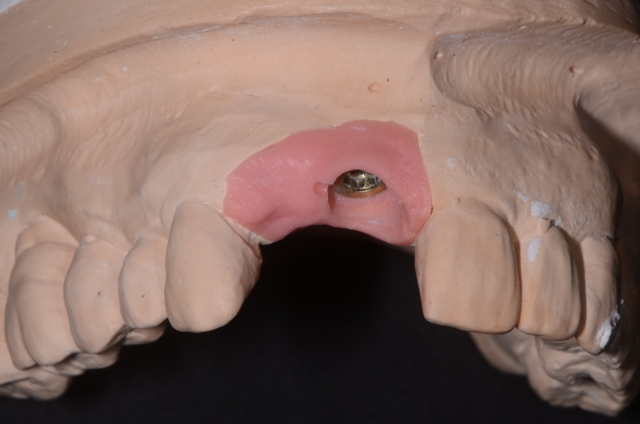
As clinicians who aspire to excellence when creating restorations, we need to evaluate our pontic design just like we do our abutment tooth preparation design. It will ensure the best long-term result in appearance, strength, and health.
SPEAR Membership
Learn Faster. Treat Better.
Whether you have 10 minutes or time to dive deeper, Spear Membership gives you the learning, tools, and support to keep improving.
Choose the level of support and structure that fits your goals.

By: Mary Anne Salcetti
Date: August 29, 2016
Featured Digest articles
Insights and advice from Spear Faculty and industry experts