In a previous article I described how to efficiently modify a patient's existing “nightguard” into a useful diagnostic tool. In that case, the patient had an existing anterior bite plane, which he wasn’t wearing often and we both knew that he would need some significant restorative dentistry.
With the modifications to his appliance, I was able to learn a lot about the patient. Specifically, I was able to relatively quickly evaluate his muscles, joints and parafunctional movement patterns (Figs. 1 and 2).
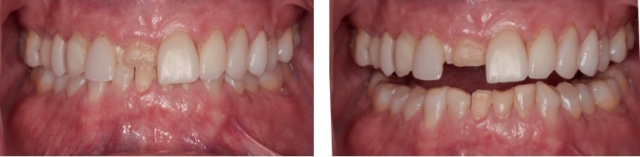
Muscles
Anterior bite planes are designed to eliminate any posterior tooth contact. By eliminating those contacts, anterior bite planes are generally very effective at reducing muscle activity – including the lateral pterygoid muscles.
In this case, the patient did not report any muscle tenderness even upon palpation during his examination. Despite his lack of muscle tenderness, the patient did report feeling less “tension” in his face (indicating the masseter and temporalis areas with his hands) after only one night of use.
Joints
By removing posterior tooth contacts, creating flat anterior tooth contacts with a smooth articulating surface, anterior bite planes can provide information about the joints. With the appliance inserted, the patient’s intercuspal position is temporarily eliminated. As the elevator muscles contract, the condyles attempt to reach their fully seated position within the glenoid fossae, uninhibited by posterior tooth contacts.
At this point any pain the patient may experience would likely originate from the lateral pterygoid muscle or from compressed, highly innervated retrodiscal tissue. Pain that decreases with time indicates muscle origin and pain that increases could implicate retrodiscal tissue and be an indication of intracapsular breakdown. In either case, determining whether or not the joint can be loaded is vital to comprehensive case planning.
Returning to the patient – both joints were comfortable with the loading situation created by his appliance and I was able to make repeatable bite records in this fully seated condylar position. Repeatable bite records would allow me to evaluate his articulated diagnostic casts and begin to develop the functional aspects of his comprehensive treatment plan.
Parafunctional analysis
As described in the previous article, the patient's existing appliance was adjusted for function (Fig. 3) then painted with a black permanent marker (Fig. 4).


In this case, the ink was used as a medium to characterize the mandibular movement during nocturnal parafunction. Ink is removed as the mandibular teeth glide over the painted surface. Areas of the appliance where the ink was rubbed off indicate the direction the mandible moves as well as providing information about how far the mandible travels during parafunction (Fig. 5).

This kind of technical information is valuable in beginning to understand a patient's movement pattern. In this case, the highly visual nature of the movement patterns developing on the appliance allowed the patient to discover for himself what he was doing with his teeth at night.
“I do grind my teeth!”
The visual information provided by the anterior bite plane and ink together with the patient’s awareness of decreased muscle tension allowed the patient to discover, for himself, how he was playing with his teeth. His observations were even more profound when he discovered that he was less comfortable in the mornings following a night where he failed to wear the appliance.
As a result, modifications to the patient's existing anterior bite plane allowed the patient to become a partner in developing his own treatment plan. By remaining curious and creating an “experiment” we both could learn from, I avoided a situation in which I had to convince the patient he was doing something he didn’t believe he was doing.
Now a partner in the process of treatment planning through treatment execution, the patient’s commitment level was high. He never missed an appointment, never questioned why a highly experienced lab technician was required and was able to accept responsibility for any future problems, especially those related to excessive force (Fig. 6).

I hope you found these articles helpful. If you have similar experiences to share we’d love to see them on Spear TALK.
(Click this link to read more dentistry articles by Dr. Darin Dichter.)
Darin Dichter, D.M.D., Spear Resident Faculty
References
Clark GT, Tsukiyama Y, Baba K, Watanabe T. Sixty-eight years of experimental occlusal interference studies: What have we learned? J Prosthet Dent. 1999 Dec;82(6):704-13.
Melkers MJ, McDonald JM. Diagnostics: Parafunctional Analysis in Diagnostics and Restorative Dentistry. Inside Dentistry 2007