
You would think after 36 years in dentistry that I would know better. The patient seems great, the story sounds plausible, the exam is promising and the case looks like it would be fun. Yeah, the patient seems a little quirky, but I can manage that right?
I have finally come to understand that my ability to see potential trouble with a patient is almost always overshadowed by my lust to do the challenging case. In my earlier career it was more about wanting the big production so I could pay my bills. As I became more financially secure, it was more about excess testosterone and wanting to prove I could do the big cases. Today, it is about trying to do cases I’ve never done before or cases that seem really hard to figure out—just to see if I can do it.
Every time I get in trouble with a patient it is because I let some “need” of mine get in the way of what I could see if I just listened. This is a case I completed about 10 years ago. Implants are in the 20, 21, 22, 27, 28, 29 positions and there is a bridge from 21-28.
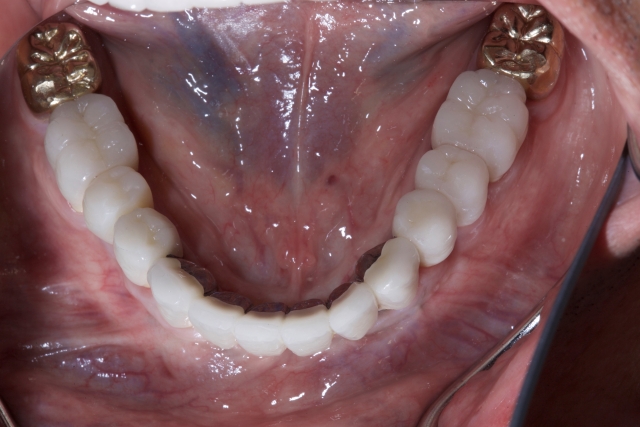
Figure 2 shows a porcelain fracture that occurred about six weeks after delivery. It was the first of 14 porcelain fractures that would occur over the next two years.
This was the single largest case I had done to that point. All those implants and a complicated occlusion and I was pumped up to move forward. I am pretty good with occlusion, as I’ve studied it for years and I know how to make teeth work together. So, what did I miss?

I knew this patient was brachycephalic and could really benefit from orthodontics and orthognathic surgery. I knew that the patient seemed intense and that I observed him clenching and squeezing his teeth together at every appointment. And finally, I knew that it took me a year to get his bite comfortable on his bite splint. I also knew that he complained of poor sleep patterns and took Ativan every night to sleep.
The patient’s class II occlusion made creating a well-tuned anterior guidance challenging, even with planning for group function. Opening the bite to create more restorative room made cusp placement more difficult.
I hope you are seeing red flags all over the place. At some level I did, but I chose to ignore them. The driver for me was a desire to do the case so I could use it for teaching. Now, I do use it for teaching, but mostly about what can go wrong.

What I didn’t know 10 years ago when I did this case was the relationship between sleep disordered breathing, bruxing and Class II occlusions. That information was just surfacing at the time I started. However, I did understand that correcting the jaw relationship would make it much easier to create a better occlusal relationship. The patient refused to see the orthodontist and absolutely refused to even consider a surgical solution.
I did the case anyway.
Then over the next two years I managed broken porcelain, all at my expense. managed an upset patient, felt bad about myself, damaged my relationship with my surgeon and lost sleep many nights. But I got my pictures so I could teach.
I don’t know how to help others avoid this dilemma. I think most of us have to go through it at least once to understand that sometimes we have to give up a case to do the right thing for the patient.
Today, I would send him for a sleep study, insist that he get off of the Ativan (it stimulates bruxing in some individuals), and decline to do the case unless he did the orthognathics surgery. The orthognathics would likely correct the sleep issue as well as allow for a much better occlusal scheme. Even then, there is no way to know if he would stop the daytime bruxing. We know that 20 percent of bruxers have a daytime habit and it is very hard to stop.
Although he refused the ortho and surgery, I believe that had I approached it differently, it is entirely likely that he would have gone forward with it if he understood what the consequences could be otherwise.
This is a very high-risk case and I failed to help my patient fully understand the implications of moving forward. No teacher is as good as experience and I hope the next time I am faced with this kind of challenging case, I’ll remember the price of ego.
Steve Ratcliff, D.D.S., M.S., Spear Faculty and Contributing Author

Comments
June 22nd, 2015
June 25th, 2015