Using a Leaf Gauge With Intention: Part II

In a previous article, I discussed the common dilemma of using one tool, the leaf gauge, for four different objectives. I also went over the confusion that can seem somewhat overwhelming if we don’t separate the information for which we are looking and recognize a different flow for each.
The four common uses for the leaf gauge are:
- Loading the TMJ
- Deprogramming the lateral pterygoid
- Identifying first point of contact in centric relation
- Obtaining centric relation bite records
In the first article, I suggested that the leaf gauge not be seen as one tool with many uses, but to actually be viewed as two different tools:
- The joint loader tool
- The muscle releasing tool
This article will review the last two objectives and the “tools” to be used to complete those objectives.
Identification of first point of contact
Using the leaf gauge (aka the Tooth I.D. Tool)
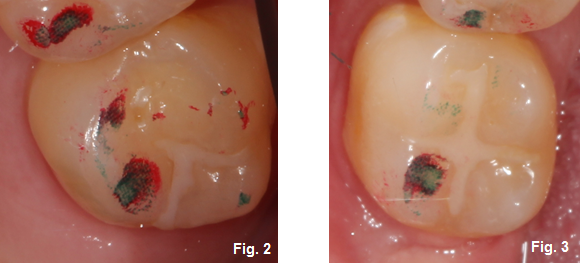
The Tooth I.D. Tool is used to predictably identify which tooth/teeth touch in centric relation or, minimally, the tooth or teeth that touch when the lateral pterygoid is fully released based on the condition of the TMJ that day. The CR bite du jour, if you will. (Figures 2 and 3)
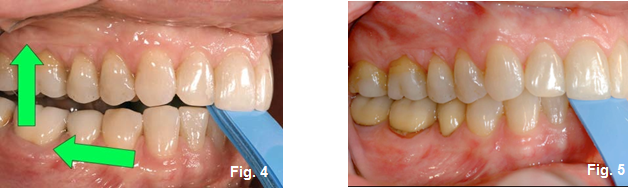
Regardless of any other signs and symptoms, the Tooth I.D. Tool will allow the practitioner to initially keep all teeth from touching, while methodically removing leafs until the patient feels the first point of contact. (Figures 4 and 5)
By asking the patient to move “forward, back, and squeeze lightly like you are trying to bite on your back teeth,” the tool will always guide both practitioner and patient to identifying the first point of contact. This is often referred to as leafing the patient down.
- How many leafs are needed to start?
- Enough to initially keep the back teeth apart, while teaching and reviewing the process with the patient. The process can be simplified by using verbiage similar to the following:“Right now as you slide forward, backwards, and squeeze like you are trying to bite on your back teeth, I assume you are only feeling plastic touch on your front teeth. I am going to remove a few of these leaves at a time and ask you if you feel anything else touching. We’ll do this several times until eventually you feel one or two teeth touch when you squeeze. Can you pay attention for me each time and let me know when you feel something besides the plastic on your front teeth touch?”
- What signs and symptoms are being evaluated?
- The only thing being evaluated is when the first tooth contacts. You and the patient may notice other signs and symptoms, but the only thing being evaluated is what tooth touches first.
- What is the intended goal or outcome?
- The intended goal is to release the lateral pterygoid, while using the muscles of mastication to seat the condyle. The intended outcome, however, is to identify the first point of contact for that point in time.
In Part III of this series, I will review the accuracy of the first point of contact based on the results of the other tools (Joint Loading Tool and Muscle Releasing Tool, that just happen to look eerily similar to this one); however, the use of the Tooth I.D. Tool is very specific and is the only tool in which the leafs are removed and teeth allowed to touch.
Obtaining centric relation bite records
Using the leaf gauge (aka the Bite Holder)
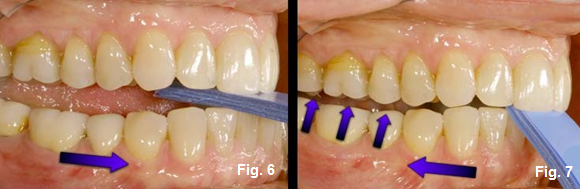
The Bite Holder not only helps the patient predictably and repeatedly slide into the desired bite position, but it also provides a very solid holding area while the bite registration sets up. (Figures 6 and 7) The best part about the bite holder is that it is adjustable, allowing for just the right space for the desired amount of material.
I would suggest practicing with the patient several times while refining the space to the desired thickness.
What is that thickness?
Great question! Thank you for asking …
That depends on what you are using it for. Similar to the joint loading tool in Part I of this series, it makes sense that the bite be recorded within the arc of closure – rotation, not translation. So, for the sake of this article, let’s assume the record will be used for diagnostic casts. For most of us, the records will be used to mount models on a semi-adjustable articulator. The closer the record is to the axis of rotation, the more likely we will be within the parameters of the arbitrary facebow.
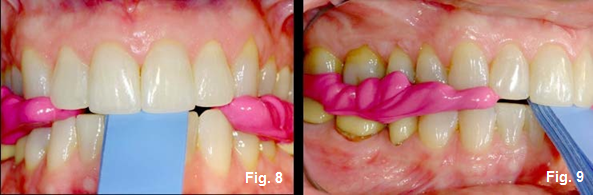
With that in mind, it makes sense for the record to be as close to the first point of contact as possible without actually touching. But remember, it is equally, if not more, important to make sure that you have enough thickness to properly trim the record to the cusp tips without sacrificing the integrity of the record. (Figures 8 and 9) Examples of this are creating a flimsy record that is hard to trim or one that falls into pieces and cannot be used at all.
- How many leafs are needed to start and why?
- Take a quick look at the overbite and overjet. How much space do you need to initially clear the back teeth? Is there excessive overjet? More leafs are needed to separate the back teeth. A deep overbite? It’s not going to take many leafs to get the back teeth apart.
- What signs and symptoms are being evaluated?
- The name is a Bite Holder, remember? In Part III of this series, I will review the variables that correlate to what we see clinically, but the Bite Holder has only one job. The signs and symptoms were evaluated using other tools.
- What is the intended goal or outcome?
- The goal is to use the tool to create adequate space for the bite registration material and hold it in the best possible place on that day (as close to a fully-seated condyle as possible with the lateral pterygoid as released as possible) while the material sets up. For most silicone bite registration material, 1.5mm to 2mm at the closest point of contact seems to be as close to the first point of contact as possible, while still allowing for ease of trimming to the cusp tips.
The Bite Holder is a wonderful tool that is easy to use, very predictable and allows the practitioner to take a high-quality centric record.
Too often, the practitioner will have some confusion regarding the intentional use of the leaf gauge at different points of the exam. Part I and Part II of this series reviewed the four common uses for the leaf gauge, separating the intent and use for each. In Part III, I will review the overlap and hopefully help the practitioner embrace the versatility of all four tools.
SPEAR campus
Hands-On Learning in Spear Workshops
With enhanced safety and sterilization measures in place, the Spear Campus is now reopened for hands-on clinical CE workshops. As you consider a trip to Scottsdale, please visit our campus page for more details, including information on instructors, CE curricula and dates that will work for your schedule.

By: Kevin Kwiecien
Date: March 5, 2015
Featured Digest articles
Insights and advice from Spear Faculty and industry experts