The Hidden Roles of the TMJ Disc and Craniofacial Growth
The temporomandibular joint (TMJ) disc and craniofacial growth are more connected than many clinicians realize, particularly in developing patients.
Disc position is not just about joint mechanics. It plays a direct role in protecting the mandibular condylar cartilage, the primary growth center of the facial skeleton. When that protective relationship is compromised, skeletal development can shift in ways that extend far beyond clicking or intermittent discomfort.
Most dentists are trained to associate TMJ issues with clicking, popping, or intermittent discomfort. But in growing patients, the more important question isn’t whether the joint makes noise; it’s whether disc position is influencing facial development.
Understanding how TMJ disc and craniofacial growth shape our diagnostic focus from symptom management to developmental risk evaluation. And that shift can change the timing, direction, and long-term stability of treatment.
Why does TMJ disc and craniofacial growth matter during development?
TMJ disc position matters during development because the disc protects the mandibular condylar cartilage, the primary growth center of the facial skeleton. When the disc properly covers the condyle, it supports normal cartilage maturation and bone formation.
When the disc is displaced, that protective relationship is compromised. The result may be altered condylar growth, reduced mandibular height, asymmetry, or compensatory maxillary changes. In growing patients, even subtle disruption of the condyle-disc interface can influence long-term skeletal development.
Most dentists learn to associate TMJ displacement with familiar symptoms, including clicking, popping, or patient discomfort that comes and goes. But what if the more important story isn’t the noise in the joint, but what’s happening to facial growth beneath the surface?
Understanding the connection between TMJ disc and craniofacial growth shifts clinical focus from joint sounds to growth patterns. Diagnosis becomes less about managing symptoms and more about identifying developmental risk early when intervention can still influence skeletal outcomes.
Let’s examine the science behind the TMJ disc and its critical role in craniofacial growth, with important implications for everyday clinical decision-making.
How does the TMJ disc protect condylar growth and craniofacial development?
The TMJ disc serves several vital functions within the TMJ. The most commonly discussed include load dissipation, lubrication, and nutrition to the condyle and joint socket.
Perhaps the most crucial role of the disc, however, is its protection of the mandibular condylar cartilage in both the growing and adult patient. This protective role is crucial in understanding the connection between the TMJ disc and craniofacial growth, particularly in developing patients.
“In growing patients, timing is not a detail. It’s the treatment.”
The mandibular condylar cartilage functions as the primary center of growth in the craniofacial complex. It’s closely associated with temporomandibular joint function and with morphogenesis of the craniofacial skeleton.1
Appreciating the connection between TMJ disc and craniofacial growth allows clinicians to anticipate skeletal changes earlier in developing patients.
What is the role of the mandibular condylar cartilage in growth?
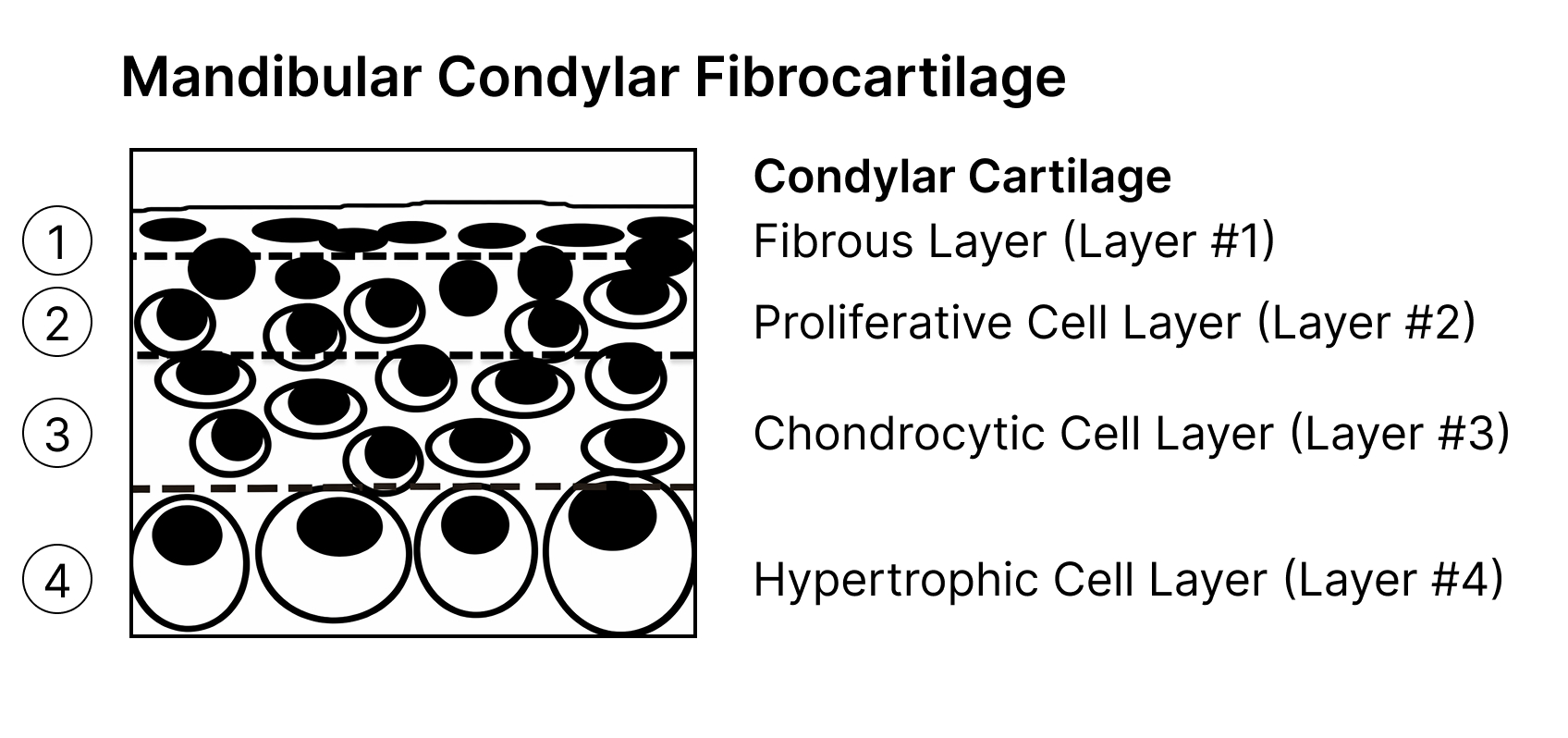
The mandibular condylar cartilage consists of four distinct cellular layers.
- Layer 1: This is the most superficial and fibrous layer. This dense fibrous connective tissue serves as a protective covering for the underlying cartilaginous tissue.
- Layer 2: Beneath Layer 1 lies the proliferative layer. Cells in this layer have the capacity to differentiate into either osteoblasts or chondrocytes.
- Layer 3: The third layer is the chondrocytic cell layer, which contains chondrocytes at various stages of maturation.
- Layer 4: The final layer is the hypertrophic layer. In this layer, cartilaginous tissue degrades and is replaced by new bone tissue.2
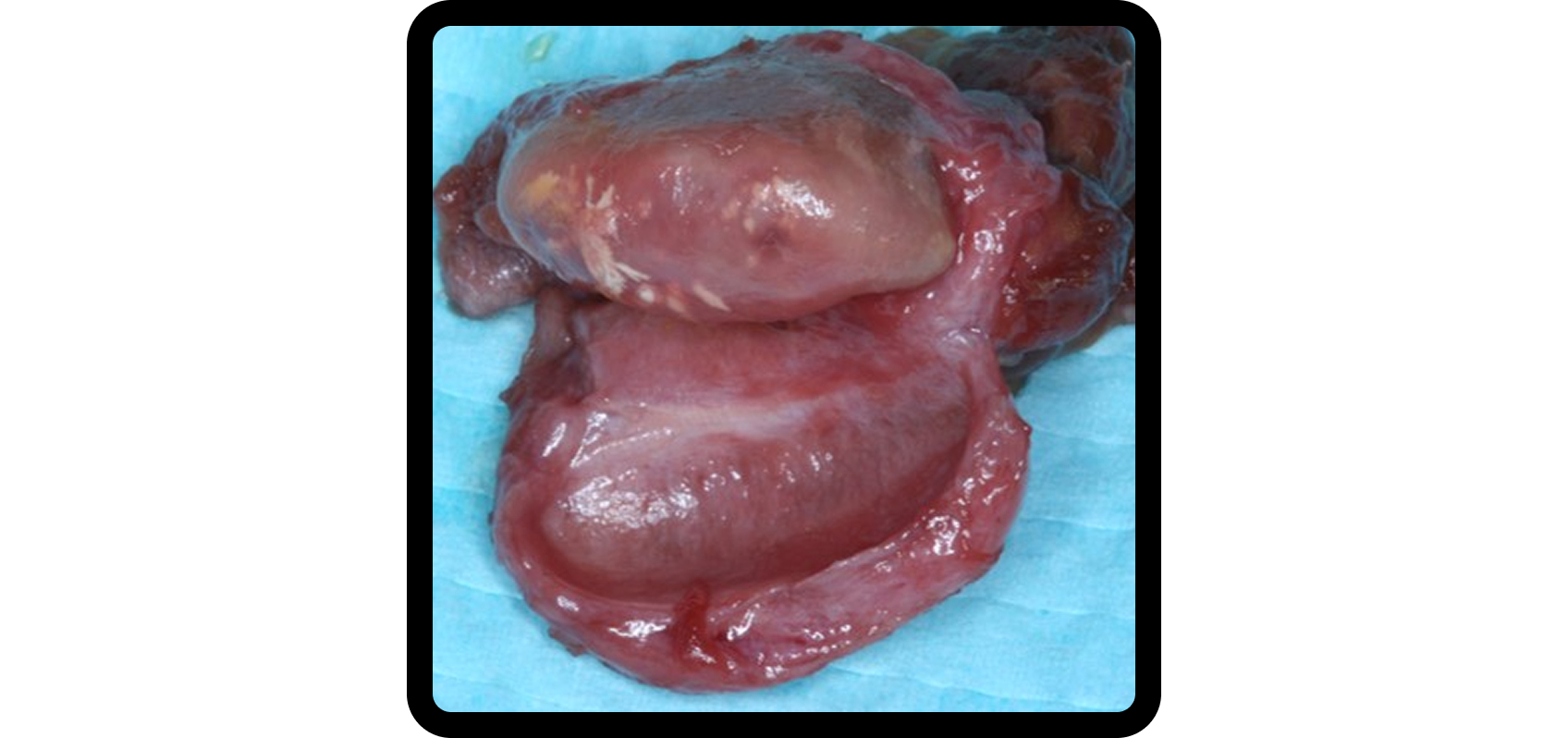
How does TMJ disc displacement disrupt craniofacial growth?
For this complex growth process to occur normally, the disc must adequately cover the mandibular condylar cartilage. When the disc is displaced, often due to ligament injury, the relationship between the TMJ disc and craniofacial growth is disrupted, with potential consequences for both mandibular and maxillary development.
This disruption may result in a measurable condylar growth disturbance, particularly in patients who have not yet completed skeletal maturation.
In a landmark paper, Schellhas demonstrated, using MRI, a causal relationship between TMJ derangement, joint degeneration, and secondary remodeling or disturbed growth of the facial skeleton.3 These findings helped establish the role of pediatric TMJ internal derangement in altered facial development.
Defabianis suggested that TMJ derangement in children may significantly impact facial growth and contribute to the development of retrognathia, with or without asymmetry. I contend that jaw injuries sustained during impact trauma to the face or mandible are the single most important cause of subsequent TMJ internal derangement.4
Does disc position affect both mandibular and maxillary development?
The traditional perspective has been that disc displacement primarily affects mandibular growth. Current evidence suggests that disc displacement can influence both mandibular and maxillary growth.
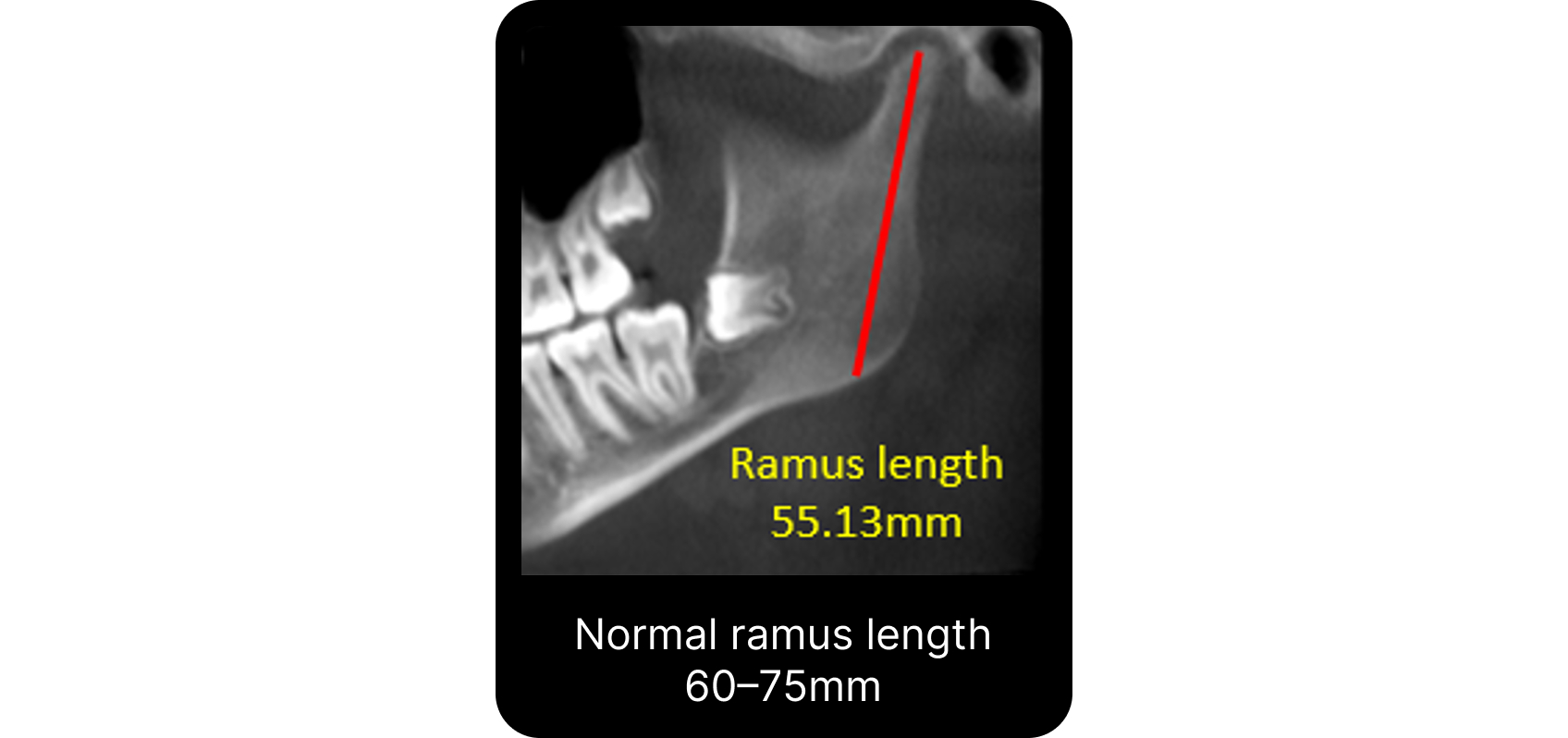
Nebbe reported that internal derangement may be associated with altered craniofacial morphology in adolescents. Findings included reduced total posterior facial height and ramus height, along with compensatory adaptation in the maxillary dentoalveolar region. This adaptation was characterized by reduced vertical development of the maxillary first molar region.5
These relationships between occlusion, joint health, and facial growth are explored in greater depth in Spear’s Occlusion in Everyday Practice seminar and the Advanced Occlusion workshop.
Common clinical signs of disc-related growth disturbance
These structural changes are not limited to imaging findings. In growing patients, altered disc position often presents with recognizable clinical patterns that evolve.
- Progressive mandibular retrognathia
- Progressive facial or mandibular asymmetry
- Reduced posterior facial height
- Early joint degeneration visible on imaging
Recognizing these patterns early allows clinicians to investigate joint health more intentionally and consider whether disc displacement may be contributing to altered craniofacial development.
Understanding how TMJ disc position influences craniofacial growth is only one piece of a larger diagnostic puzzle. To consistently evaluate risk, sequence findings, and make confident clinical decisions, clinicians benefit from a structured approach to advanced dental treatment planning that integrates airway, esthetics, function, structure, biology (AEFSB) into a single framework.
What does experimental research show about TMJ disc and craniofacial growth?
Legrell evaluated the effects of experimentally induced TMJ disc displacement in an animal model. The study concluded that disc displacement in a growing individual can reduce mandibular height and length before visible osteoarthritic changes occur. This suggests a primary adverse effect on condylar growth.6
Qadan studied mandibular and cranial base asymmetries using an animal model with surgically induced unilateral disc displacement. At 22 weeks, the glenoid fossa on the experimental side was positioned more anteriorly, while the root of the zygomatic arch was more inferior. The anterior aspect of the fossa was also more inferior on frontal radiographs. These findings indicate that disc displacement can produce asymmetry in both the developing mandible and the cranial base.7
When should clinicians attempt to re-establish the condyle-disc relationship?
Because the TMJ disc and craniofacial growth play critical roles, and because disc displacement often occurs early in life, a logical treatment goal is to re-establish the condyle-disc interface to support normal growth.
Supporting normal TMJ disc and craniofacial growth should remain the priority during active growth phases. This may be achieved indirectly through functional appliances designed to re-establish the condyle-disc assembly, or surgically through disc repositioning.
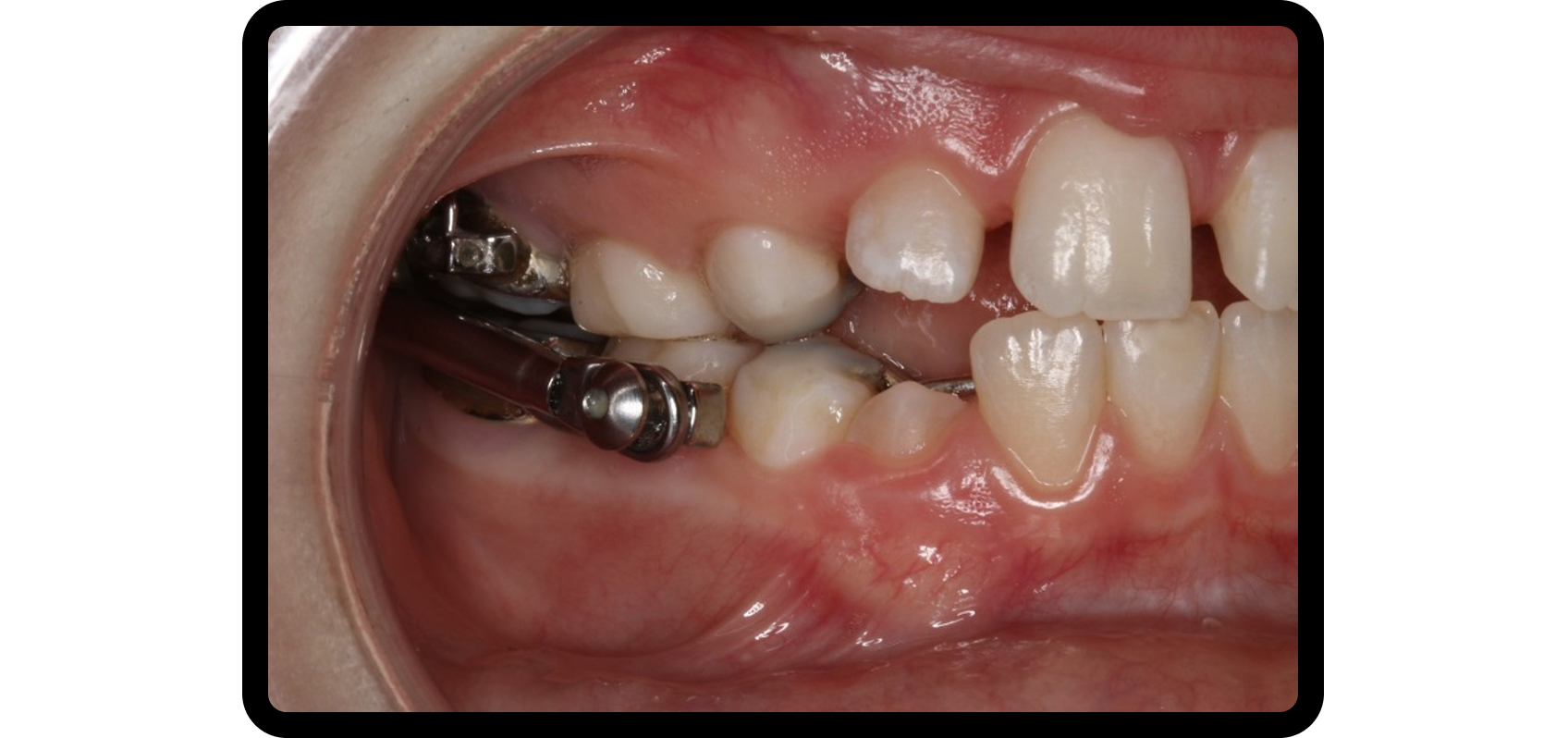
Lei evaluated the role of TMJ disc position in functional appliance therapy. Eight patients had anterior disc displacement with reduction (ADDWR) on one side and anterior disc displacement without reduction (ADDWoR) on the other, as confirmed by MRI.
New bone formation occurred in seven ADDWR joints and only one ADDWoR joint. Condylar height increased by 1.4 mm in the ADDWR group and decreased by 0.1 mm in the ADDWoR group.
These findings suggest that functional appliances are ineffective for Class II adolescents with ADDWoR, and that only a normal disc-condyle relationship supports condylar growth. The study emphasized the importance of early disc repositioning.8
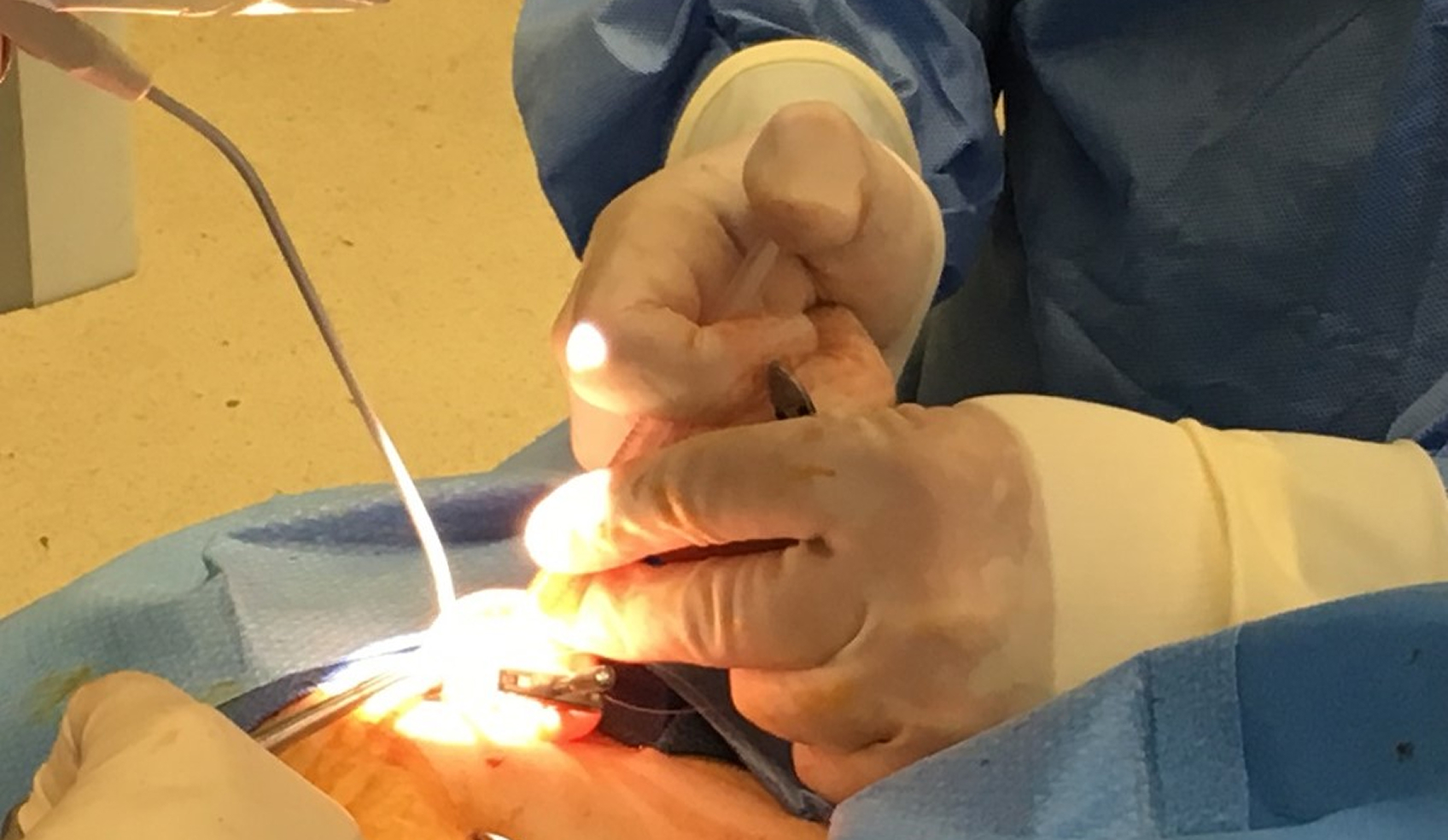
Liu examined the effects of disc repositioning surgery on condylar development and mandibular asymmetry in juvenile patients with unilateral anterior disc displacement. The study concluded that surgical repositioning significantly improved condylar height. Early treatment was recommended to support condylar development and reduce the risk of jaw deformities.9
Why does TMJ disc and craniofacial growth position matter in everyday clinical decisions?
While disc displacement is often discussed in terms of joint clicking or popping, the more significant concern may be its impact on mandibular and maxillary growth. Recognizing the interconnection between the TMJ disc and craniofacial growth enables clinicians to anticipate developmental changes and plan treatment more effectively.
A strong understanding of disc function in the growing patient allows clinicians to communicate more effectively with patients and parents, explain treatment options with greater confidence, and make more informed clinical decisions.
For clinicians seeking deeper clinical application, Spear Online offers a range of occlusion-focused video courses that explore TMJ health and its relationship to comprehensive care.
Why early diagnosis and collaboration matter the TMJ disc and craniofacial growth
TMJ disc and craniofacial growth are inseparable in the developing patient. When disc position is compromised, condylar growth, facial symmetry, and occlusal development may all be affected. Early diagnosis allows clinicians to identify risk factors for condylar growth disturbance and mandibular asymmetry before irreversible skeletal changes occur.
Spear’s philosophy emphasizes growth-sensitive treatment planning, interdisciplinary communication, and proactive intervention. By collaborating across orthodontic, restorative, and TMD disciplines, clinicians can protect condylar development, guide facial growth more predictably, and deliver long-term stability rather than reactive correction later in life.
In growing patients, timing is not a detail when it comes to TMJ disc and craniofacial growth. It’s the treatment.
References
- Mizoguchi, I., Toriya, N., & Nakao, Y. (2013). Growth of the mandible and biological characteristics of the mandibular condylar cartilage. Japanese Dental Science Review, 49(4), 139-150.
- Robinson, J., O’Brien, A., Chen, J., & Wadhwa, S. (2015). Progenitor cells of the mandibular condylar cartilage. Current Molecular Biology Reports, 1(3), 110-114.
- Schellhas, K. P., Pollei, S. R., & Wilkes, C. H. (1993). Pediatric internal derangements of the temporomandibular joint: effect on facial development. American Journal of Orthodontics and Dentofacial Orthopedics, 104(1), 51-59.
- Defabianis, P. (2003). Post-traumatic TMJ internal derangement: impact on facial growth (findings in a pediatric age group). Journal of Clinical Pediatric Dentistry, 27(4), 297-303.
- Nebbe, B., Major, P. W., Prasad, N. G., Grace, M., & Kamelchuk, L. S. (1997). TMJ internal derangement and adolescent craniofacial morphology: a pilot study. The Angle Orthodontist, 67(6), 407-414.
- Legrell, P. E., Reibel, J., Nylander, K., Hörstedt, P., & Isberg, A. (1999). Temporomandibular joint condyle changes after surgically induced non-reducing disc displacement in rabbits: a macroscopic and microscopic study. Acta Odontologica Scandinavica, 57(5), 290-300.
- Qadan, S., Macher, D. J., Tallents, R. H., Kyrkanides, S., & Moss, M. E. (1999). The effect of surgically induced anterior disc displacement of the temporomandibular joint on the midface and cranial base. Clinical Orthodontics and Research, 2(3), 124-132.
- Lei, J., Yap, A. U. J., Liu, M. Q., & Fu, K. Y. (2019). Condylar repair and regeneration in adolescents/young adults with early‐stage degenerative temporomandibular joint disease: A randomised controlled study. Journal of Oral Rehabilitation, 46(8), 704-714.
- Liu, Z., Xie, Q., Yang, C., Chen, M., Bai, G., & Abdelrehem, A. (2020). The effect of arthroscopic disk repositioning on facial growth in juvenile patients with unilateral anterior disc displacement. Journal of Cranio-Maxillofacial Surgery, 48(8), 765-771.
Frequently Asked Questions
SPEAR campus Workshops
Step Into a Place Built for Mastery
Step away from the noise of practice and into focused, immersive training that changes how you think, diagnose, and lead.

By: Jim McKee
Date: April 21, 2026
Featured Digest articles
Insights and advice from Spear Faculty and industry experts