Implant-Supported Restoration for a Lower Second Molar
Sharing the news with our patient that a tooth can no longer be restored can elicit a variety of reactions, ranging from apathy to an emotional sense of urgency regarding what can be done to replace this tooth. I’m curious how you handle the discussion related to a lower second molar.
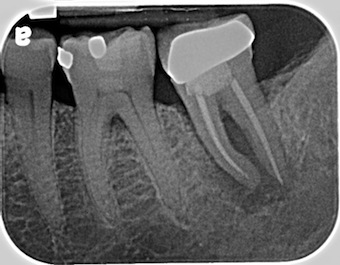
How much treatment is required to prepare this site for a dental implant-supported restoration? Dental implants have improved the options available to our patients for solutions related to missing teeth. There are many advantages to preserving adjacent teeth and maintaining alveolar bone, and it can become automatic to recommend a dental implant-supported restoration for our patients, making a decision on how to proceed. Super eruption of the opposing tooth (maxillary second molar) is a possibility; however, according to Shugars, bound edentulous spaces over a median follow-up period of 6.9 years did not, as a general rule, demonstrate adverse consequences when deciding against the replacement of the missing tooth.
It would be unlikely that a super eruption of the maxillary second molar into the space of a missing mandibular second molar could interfere with protrusive movements. Anatomically, in terms of supporting bone, concerns arise as to the natural undercut of the mandible at the beginning of the retromylohyoid fossa, as well as the relatively superior position of the inferior alveolar nerve.
A recent study by Ham set out to gain insight into the justification of a second molar implant-supported restoration. They found both a measurable increase in masticatory efficiency as well as a subjective increase in patient satisfaction following insertion of the definitive restoration.
For a patient who had premolars removed to facilitate orthodontic tooth movement, maintaining the chewing surface of a mandibular second molar can intuitively provide a functional benefit. The discussion can be more interesting when the patient has maintained all their teeth (premolars), providing functional contact for first molar occlusion.
At the least, it is an opportunity to discuss treatment with our patient while increasing their awareness of the importance of maintaining their dentition.
References
- Shugars, D. A., BADER, J. D., PHILLIPS JR, S. W., WHITE, B. A., & BRANTLEY, C. F. (2000). The consequences of not replacing a missing posterior tooth. The Journal of the American Dental Association, 131(9), 1317-1323.
- Nam, D. H., Lee, D. W., Chung, C. J., Kim, K. H., Park, K. H., & Moon, I. S. (2014). Change in masticatory ability with the implant restoration of second molars. The Journal of Prosthetic Dentistry, 111(4), 286-292.
SPEAR All access
An Integrated System for Practice Growth
Spear All Access is an integrated growth system for dentists who want to build a high-performing practice. Attend any Spear or CDOCS workshop, access all our online courses and chairside tools, and work with a Practice Growth Partner to implement the system.

By: Doug Benting
Date: March 26, 2018
Featured Digest articles
Insights and advice from Spear Faculty and industry experts


