How to Plan Phased Restorative Dentistry for Complex Wear
Managing VDO changes and complex wear with a structured, predictable approach
Phased restorative dentistry gives you control in complex wear cases. Especially when vertical dimension, occlusion, or multiple disciplines are in play.
The strategy is simple in principle. Do not rush to definitive treatment. Instead, sequence the case. Use provisional restorations to test changes. Validate the diagnosis. Allow the patient to adapt before you commit.
Each phase builds on the last. Provisionalization confirms function. Diagnostics reduce uncertainty. Biologic response guides the next step.
The goal is not just to complete the case. It is to complete it with confidence. Phased restorative dentistry reduces risk, improves predictability, and supports long-term functional outcomes.
What causes VDO loss and occlusal collapse?
Loss of vertical dimension of occlusion (VDO) typically results from progressive posterior wear, missing teeth, or long-standing bruxism and often requires full arch and full-mouth restorative treatment to achieve a stable, functional occlusion.
When posterior support collapses, patients often present with:
- Reduced lower facial height
- Uneven occlusal wear
- Super-eruption of anterior teeth
- Compromised esthetics
- Muscle discomfort or fatigue
Successful rehabilitation requires understanding occlusion, joint health, and restorative sequencing.
According to Spear’s occlusion curriculum, predictable outcomes depend on reestablishing harmony among teeth, temporomandibular joints, and masticatory muscles before definitive restorations are placed.
Why does phased restorative dentistry matter in complex cases?
Ideally, clinicians complete full-mouth rehabilitation in one coordinated sequence. In reality, financial constraints, insurance limitations, and patient scheduling often make that impractical.
Phased restorative dentistry allows clinicians to:
- Test changes in vertical dimension
- Evaluate patient adaptation
- Maintain biologic stability
- Control occlusion throughout treatment
- Spread financial impact over time
Spear emphasizes diagnostic clarity and provisionalization as tools to preserve predictability when treatment must occur in stages.
These cases require meticulous planning, thoughtful case selection, and precise execution guided by advanced dental treatment planning principles that ensure occlusal changes are both biologically and mechanically sound.
While inherently complex, these rehabilitations are often among the most rewarding procedures for both clinician and patient, restoring function, esthetics, and long-term stability.
Case #1: How can phased restorative dentistry rebuild a collapsed maxilla?
This case demonstrates how phased restorative dentistry enables the reliable attainment of functional and esthetic goals while giving the patient time to adapt and manage treatment costs.
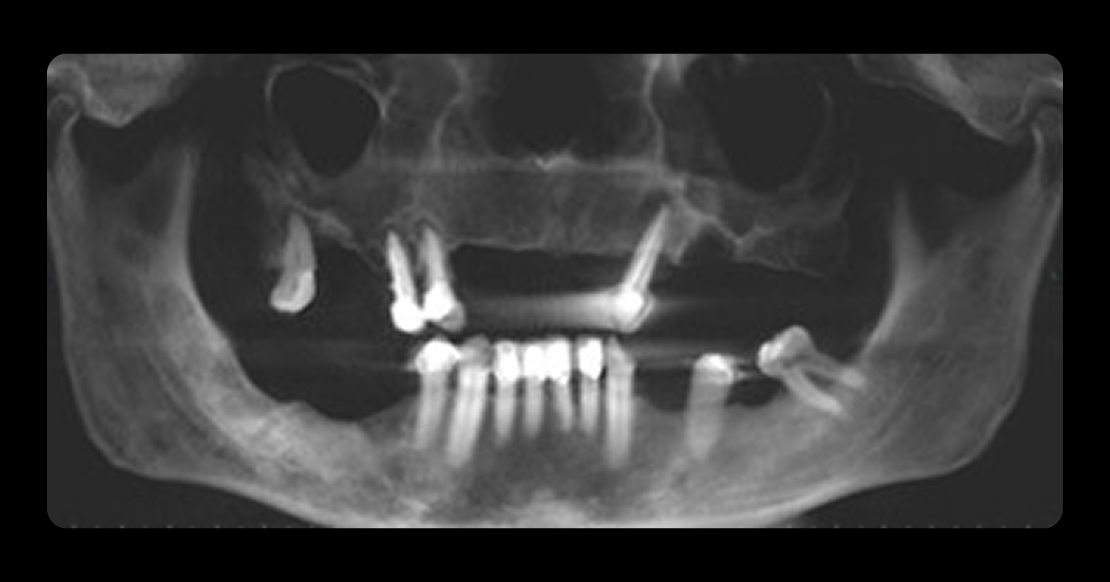
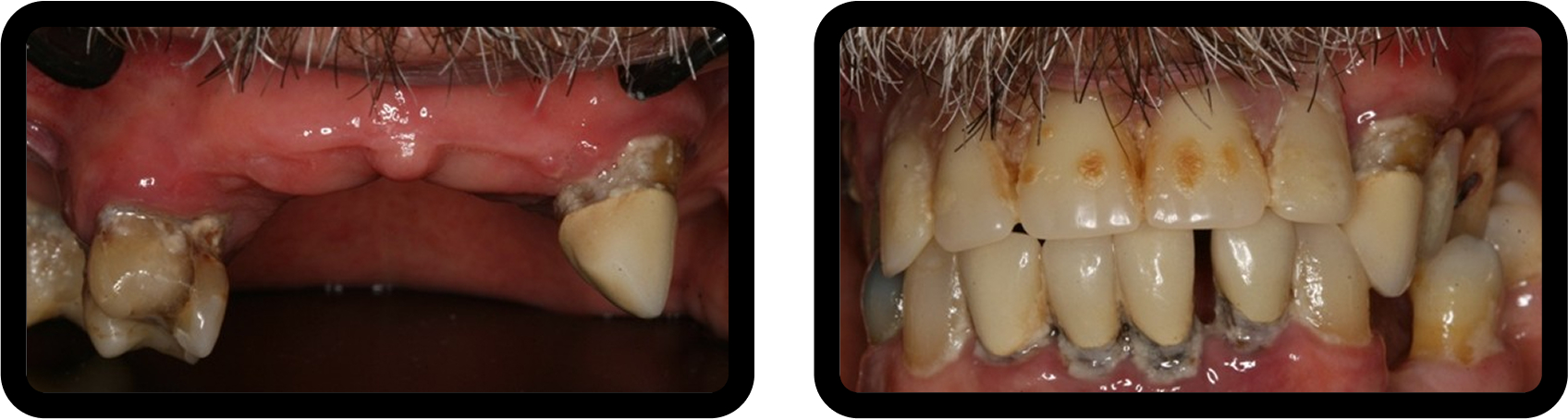
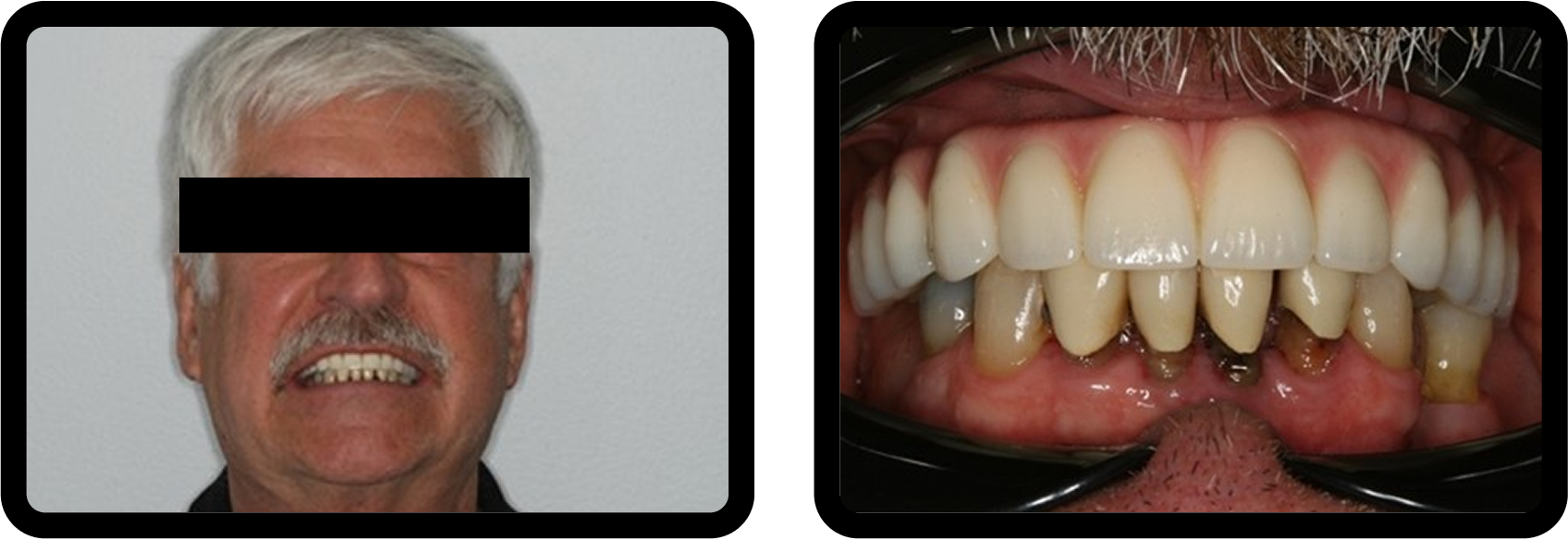
After radiographic analysis, periodontal assessment, and occlusal examination, Jerry presented with failing maxillary dentition supported by a removable partial denture, significant occlusal collapse, and esthetic dissatisfaction, all of which negatively affected his confidence at work (Fig. 1).

His occlusal collapse included uneven wear and super-eruption of the left maxillary cuspid, contributing to his functional and esthetic concerns (Fig. 2).
What were the treatment objectives?
- Restore function and comfort
- Re-establish stable VDO
- Improve esthetics
- Reinforce oral hygiene
Phase 1: Periodontal stabilization and interim prosthesis
Hopeless teeth were extracted, oral hygiene was addressed, and VDO was adjusted. An interim maxillary complete denture preserved esthetics and function during healing (Fig. 3).
The remaining maxillary teeth were extracted, along with tooth #18, which interfered with both interim and definitive restorative plans. Orthodontic uprighting was considered, but the patient elected to have extractions.
Phase 2: Surgical preparation
An interim maxillary complete denture was fabricated and delivered immediately to preserve esthetics, function, and vertical dimension during healing.
This phase allowed soft tissue and ridge healing and patient adaptation before definitive care.
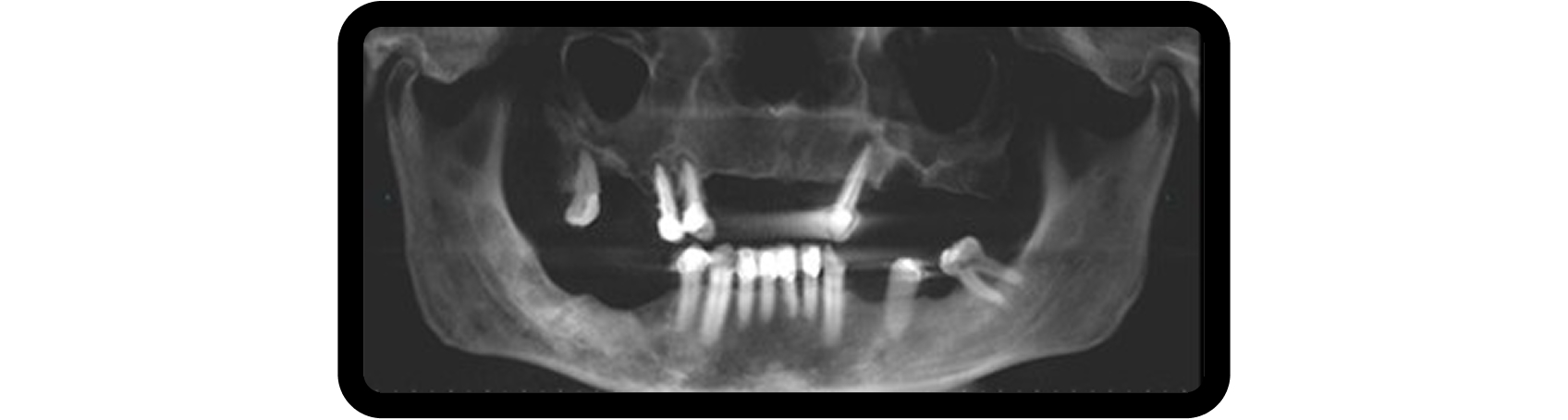
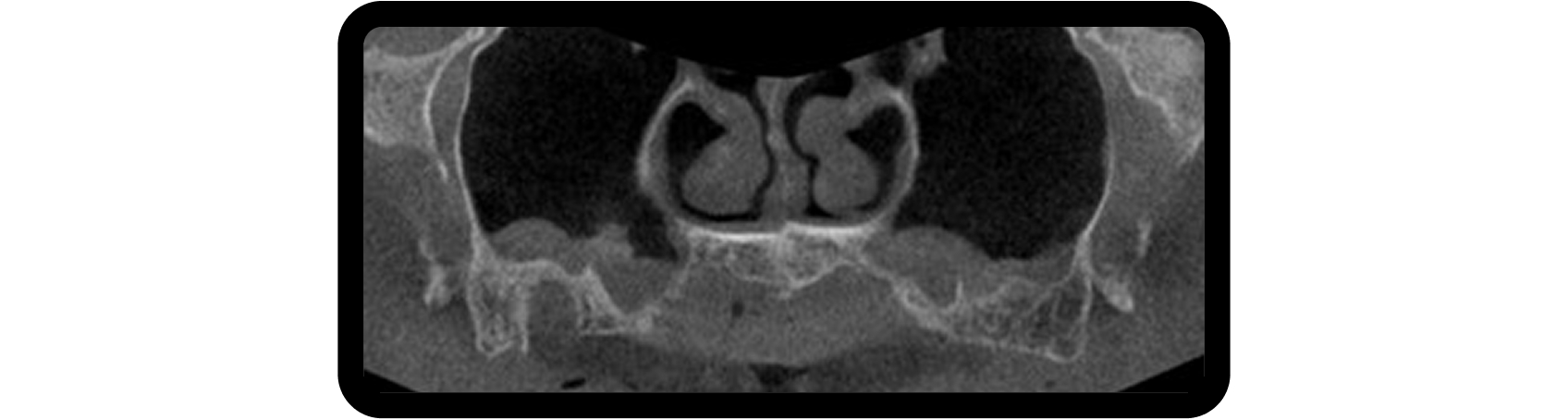
Bilateral sinus augmentation was required to support a six-implant, screw-retained zirconia restoration. A CBCT scan revealed radiolucencies in both maxillary sinuses, prompting referral to an ENT specialist before proceeding (Fig. 4).
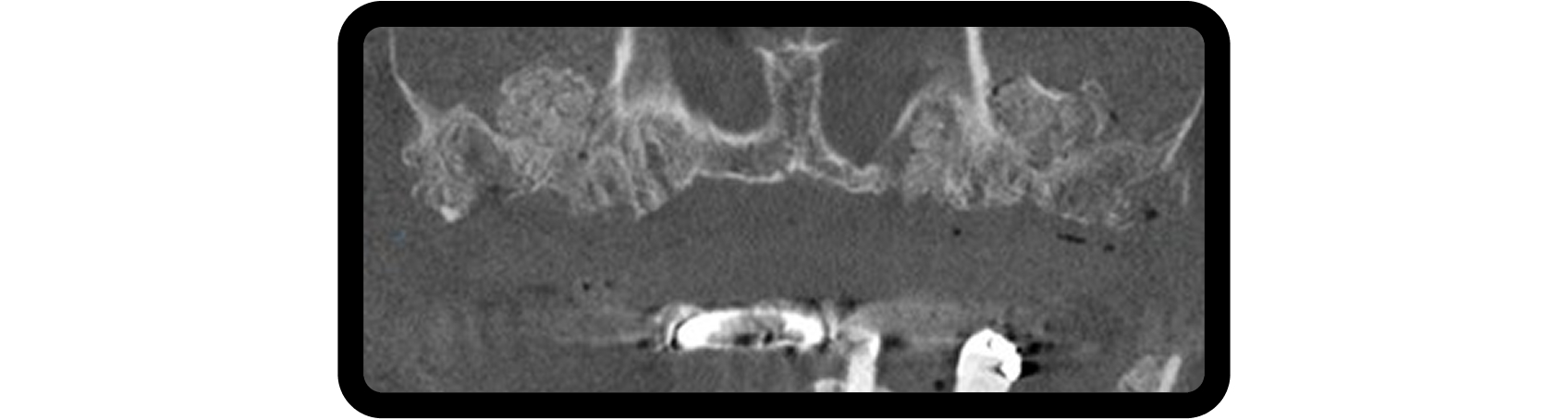
Following ENT clearance, lateral window sinus augmentation was performed, with additional grafting in areas affected by periodontal disease (Fig. 5). After six months of healing, six implants were placed to support the planned restoration.
Phase 3: Definitive rehabilitation
The maxillary arch was restored first, followed by mandibular rehabilitation (Fig. 6) and provisionalization at the new VDO to allow patient adaptation and functional evaluation (Fig. 7).
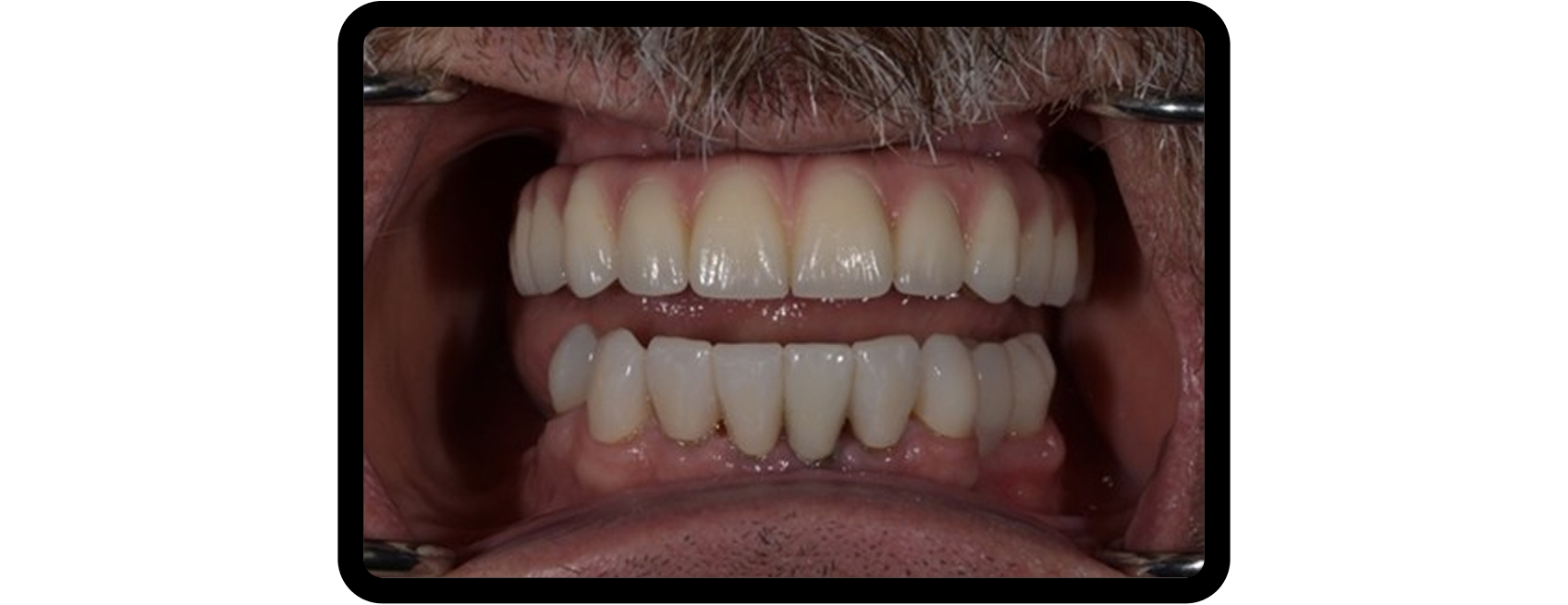
This sequence allowed controlled occlusal management and long-term stability — a hallmark of phased restorative dentistry.
Case #2: Can phased restorative dentistry work for younger patients with wear?
This case illustrates the importance of phased restorative dentistry and presents feasible, diagnosis-driven alternatives.
Robert, age 34, presented with severe wear, GERD, and mild obstructive sleep apnea (Fig. 8). Two practices recommended full-mouth reconstruction, but financial barriers prevented treatment.
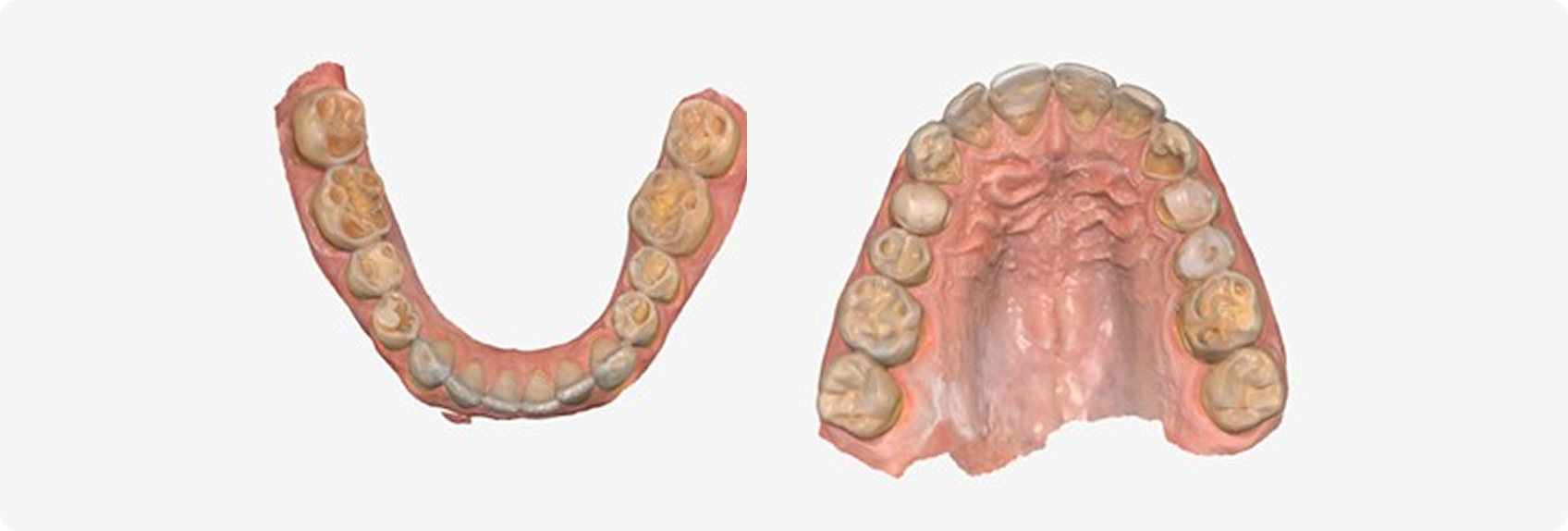
Why was medical management critical?
Clinical and radiographic evaluation revealed multifactorial wear, including erosive and attritional components. Medical history was significant for gastroesophageal reflux disease (GERD) and obstructive sleep apnea (OSA), with an apnea-hypopnea index of 7.5.
GERD and OSA contribute to erosive and attritional wear. Before restorative intervention:
- GERD was controlled with medication
- VDO was tested using an oral appliance
- AHI was reduced to below 5
Spear’s interdisciplinary philosophy emphasizes stabilizing systemic contributors before definitive care.
Robert’s GERD was managed with a proton pump inhibitor, while sleep apnea interventions included mouth taping and incremental increases in VDO using an oral appliance. Effectiveness was confirmed using the Seattle Protocol developed by Spear Faculty Drs. Rouse and Kinzer. Robert’s AHI decreased to below 5 before restorative care began.
How was treatment phased?
- Posterior bonded resin onlays were placed without preparation
- Anterior composite restorations restored lingual contours
- Occlusion was equilibrated at the increased VDO
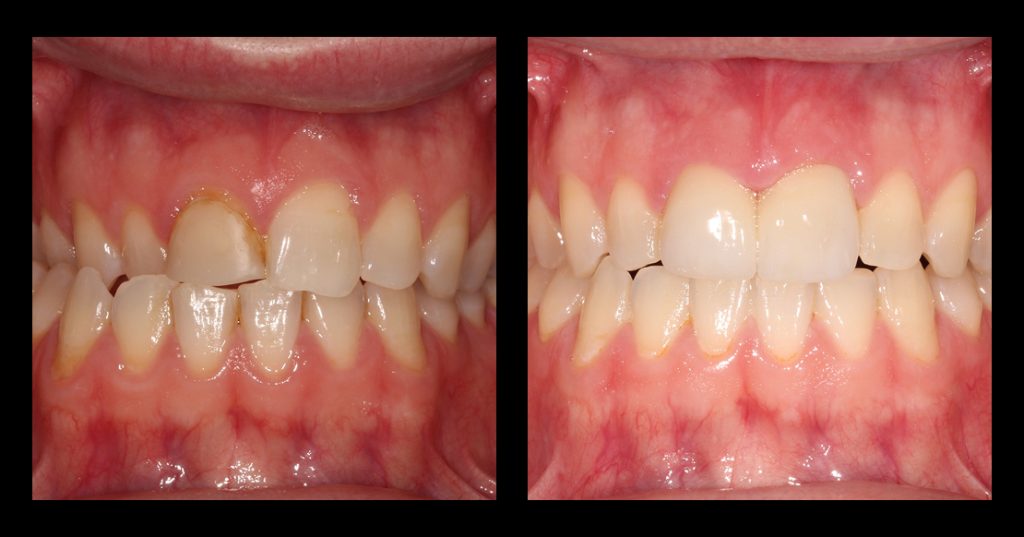
Digital scans were used to create a diagnostic wax-up and design posterior resin onlays (Fig. 9). Teeth were air-abraded to enhance adhesion, and onlays were bonded without tooth preparation.
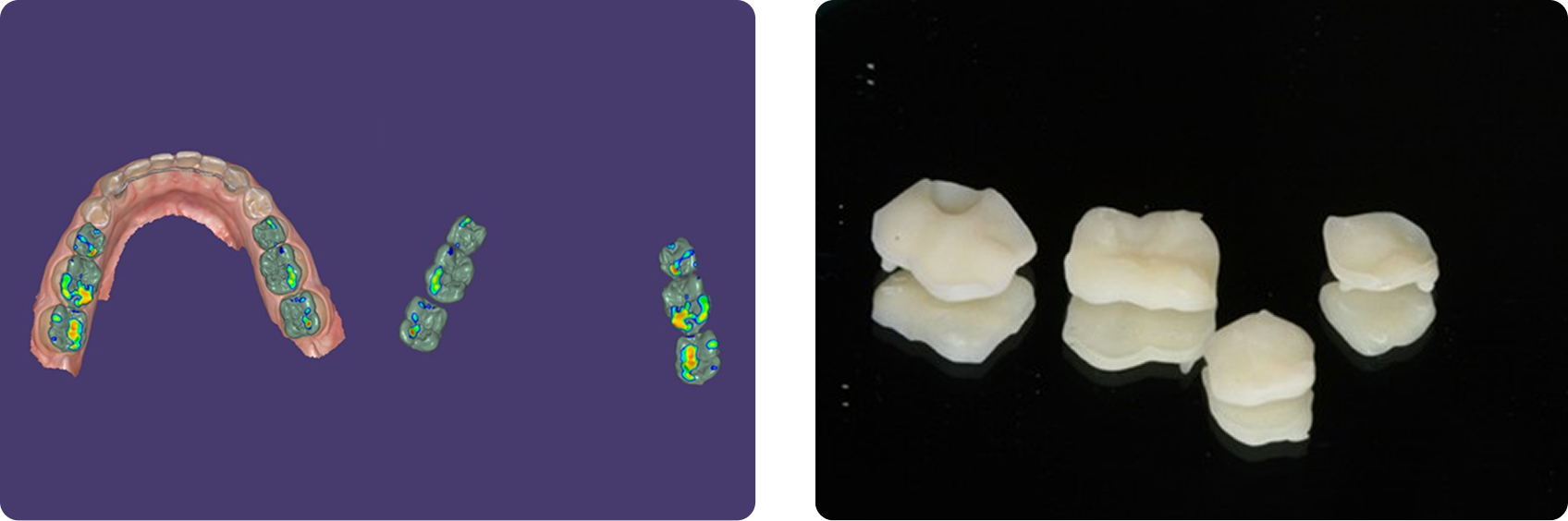
Occlusion was equilibrated, followed by direct composite restoration of the anterior teeth, with emphasis on lingual contours to support the increased VDO (Fig. 10).
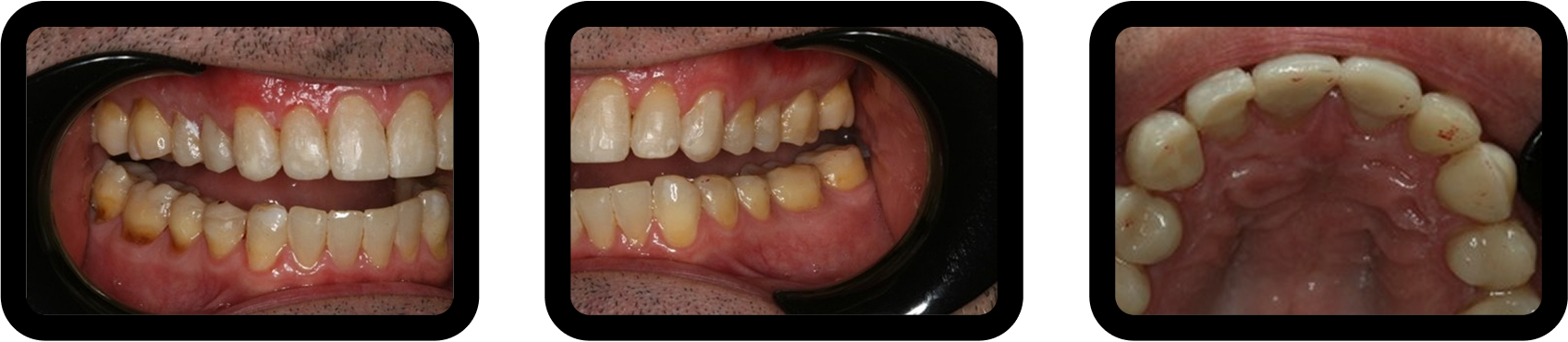
This conservative, staged approach protected dentition while preserving financial feasibility.
Phased restorative dentistry provided functional stabilization without immediate full-mouth reconstruction.
Phased restorative dentistry vs full-mouth reconstruction
Both approaches aim to restore function, esthetics, and long-term stability. The difference lies in sequencing, adaptability, and financial structure. Phased restorative dentistry spreads treatment over time, while full-mouth reconstruction completes care in one coordinated sequence.
While both approaches can produce excellent outcomes, the decision often hinges on adaptability, financial logistics, and diagnostic certainty.
| Phased Restorative Dentistry | Full-Mouth Reconstruction | |
| Treatment sequencing | Completed in structured stages with interim evaluation | Completed in one comprehensive treatment sequence |
| Vertical dimension management | VDO is tested and adjusted before definitive restorations | VDO changes are finalized during definitive reconstruction |
| Patient adaptation | Allows functional and muscular adaptation between phases | Requires immediate adaptation to full occlusal changes |
| Financial structure | Costs distributed over time | Larger financial commitment upfront |
| Clinical flexibility | Adjustments can be made between phases based on response | Limited opportunity for modification once definitive restorations are placed |
Phased restorative dentistry is not a compromise in quality. It is a strategic approach that prioritizes diagnostic confirmation, patient adaptation, and controlled occlusal management before finalizing definitive care.
When should clinicians consider phased restorative dentistry?
Consider a phased approach when:
- VDO changes are required
- Patients have medical comorbidities (GERD, OSA)
- Financial constraints limit comprehensive care
- Diagnostic uncertainty exists
- Provisional testing is needed before finalization
Phasing is not a compromise. It is controlled sequencing.
Why phased restorative dentistry improves long-term outcomes
When treatment occurs in stages:
- Occlusion can be tested before definitive materials
- Muscles adapt gradually
- Patients experience fewer surprises
- Financial stress decreases
- Maintenance planning improves
Spear’s philosophy reinforces that predictability comes from diagnosis and sequencing, not speed.
Phased restorative dentistry provides a practical, predictable pathway for managing VDO changes and complex wear cases. By sequencing treatment, testing occlusal changes, and respecting biologic adaptation, clinicians can restore function, esthetics, and long-term stability without compromising outcomes.
For dentists managing complex rehabilitations, phased restorative dentistry transforms overwhelming cases into structured, achievable treatment plans.
Building clinical confidence through structured education
Clinicians seeking structured frameworks for managing VDO changes can pursue advanced continuing education, especially within the Spear philosophy of interdisciplinary treatment planning for phased restorative dentistry. This approach provides clinicians with the diagnostic framework, communication strategies, and clinical techniques needed to handle these cases predictably.
Programs such as Spear’s Occlusion in Clinical Practice workshop and the virtual seminar Occlusal Confidence in the Age of Digital Dentistry emphasize the principles discussed in this article, with additional on-demand occlusion content available through Spear Online.
Frequently Asked Questions
SPEAR campus Workshops
Step Into a Place Built for Mastery
Step away from the noise of practice and into focused, immersive training that changes how you think, diagnose, and lead.

By: Curt Ringhofer
Date: April 7, 2026
Featured Digest articles
Insights and advice from Spear Faculty and industry experts