Definitive Guide to Diagnosing Periodontitis Today
What is diagnosing periodontitis using the 2018 classification?
Diagnosing periodontitis with the 2018 classification means identifying the presence of disease and then assigning a stage and grade based on severity, complexity, and risk. This system shifts diagnosis from simple labels to a structured clinical framework that supports long-term treatment planning and risk assessment.
Why did diagnosing periodontitis change in 2018?
The 2018 classification emerged from the 2017 World Workshop to address a long-standing issue: clinicians struggled to consistently diagnose periodontitis.
Earlier systems relied heavily on age-based categories and complex attachment loss calculations. The updated framework focuses on:
- Clear case definitions
- Disease staging based on severity
- Risk-based grading
- Lifelong disease identification
Clinically, this matters because periodontitis is no longer viewed as episodic. Once diagnosed, the patient remains a periodontitis patient for life, even when stable.
What are the key concepts behind diagnosing periodontitis?
The 2018 classification introduced several foundational ideas that directly impact diagnosis:
Periodontal health is now clearly defined
For the first time, clinicians have a formal definition of periodontal health on both intact and reduced periodontium.
Periodontitis is a lifelong condition
Attachment loss is irreversible. Even when inflammation is controlled, the patient remains at risk.
Risk is built into diagnosis
Diagnosis now reflects not just what has happened, but how likely the disease is to progress.
Extent matters
A 30% threshold distinguishes localized from generalized disease, improving diagnostic clarity.
How is periodontitis classified today
The 2018 system identifies three primary forms:
- Periodontitis (most common inflammatory form)
- Necrotizing periodontitis (associated with tissue necrosis)
- Periodontitis as a manifestation of systemic disease
For most general practices, the focus remains on diagnosing and managing standard inflammatory periodontitis.
How does staging help in diagnosing periodontitis?
Staging defines how severe the disease is and how complex treatment will be.
Stage I–II
- Mild to moderate attachment loss
- Mostly horizontal bone loss
- Lower complexity
Stage III–IV
- Severe attachment loss
- Deep probing depths
- Vertical bone loss or furcation involvement
- Potential need for complex rehabilitation
Clinically, staging answers this question: How difficult will this case be to treat and maintain?
How does grading influence diagnosis?
Grading determines how fast the disease is progressing and the patient’s risk profile.
Grade A
- Slow progression
- Minimal destruction relative to biofilm
Grade B
- Moderate progression (default assumption)
Grade C
- Rapid progression
- Destruction exceeds expectations
Modifiers include smoking status and diabetes control.
This is a major shift. Diagnosis now incorporates systemic and behavioral risk, not just clinical findings.
Why is diagnosing periodontitis still challenging?
Despite improvements, many clinicians still struggle to apply the system chairside. Common challenges include:
- Interpreting staging vs. grading differences
- Navigating multiple decision pathways
- Reconciling conflicting clinical indicators
- Applying tables efficiently during exams
Even experienced clinicians may find the process time-consuming without a structured workflow.
How can clinicians apply the 2018 classification in practice?

To simplify diagnosing periodontitis in daily practice:
Step 1: Confirm disease presence
- Clinical attachment loss
- Radiographic bone loss
Step 2: Assign a stage
- Based on severity and complexity
Step 3: Assign a grade
- Based on progression and risk factors
Step 4: Define extent
- Localized vs. generalized
Step 5: Evaluate stability
- Stable vs. unstable (formerly “active”)
This structured approach turns a complex system into a repeatable clinical process.
Why diagnosing periodontitis matters for treatment planning
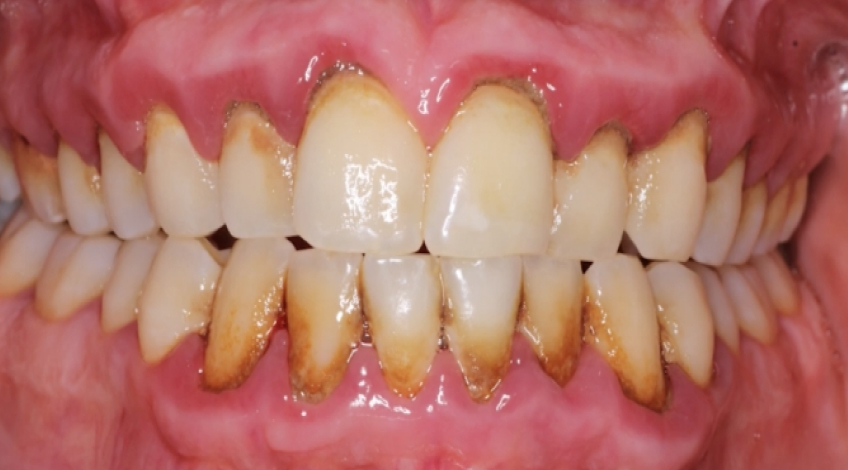
Accurate diagnosis is not just academic; it directly impacts outcomes.
When diagnosing periodontitis correctly, clinicians can:
- Match treatment to disease severity
- Identify high-risk patients early
- Improve long-term stability
- Reduce restorative failure
This is where diagnosis connects directly to advanced dental treatment planning, ensuring decisions are biologically and functionally sound.
When should a dentist intervene?
Intervention is necessary when:
- Probing depths exceed 4 mm with bleeding
- Progressive attachment loss is evident
- Risk factors (smoking, diabetes) are present
- Stability cannot be maintained with hygiene alone
Early intervention improves prognosis and reduces complexity over time.
Key takeaway
Diagnosing periodontitis using the 2018 classification provides a more complete picture of disease by integrating severity, risk, and long-term prognosis. While the system is more complex, it allows clinicians to move beyond labels and toward structured, predictable care, an approach central to comprehensive dentistry.
Frequently Asked Questions
References
- Wen, P. Y. F., Chen, M. X., Zhong, Y. J., Dong, Q. Q., & Wong, H. M. (2022). Global Burden and Inequality of Dental Caries, 1990 to 2019. Journal of Dental Research, 101 (4), 392-9.
- Zhang, X., Wang, X., Wu, J., Wang, M., Hu, B., Qu, H., et al. (2022). The global burden of periodontal diseases in 204 countries and territories from 1990 to 2019. Oral Diseases.
- American Academy of Periodontology. (2015). Task Force Report on the Update to the 1999 Classification of Periodontal Diseases and Conditions. Journal of Periodontology, 86 (7), 835-8.
- Chapple, I. L. C., Mealey, B. L., Van Dyke, T. E., Bartold, P. M., Dommisch, H., Eickholz, P., et al. (2018). Periodontal health and gingival diseases and conditions on an intact and a reduced periodontium: Consensus report of workgroup one of the 2017 World Workshop on the Classification of Periodontal and Peri-Implant Diseases and Conditions. Journal of Periodontology, 89 (Suppl 1), S74-s84.
- The American Academy of Periodontology. Proceedings of the World Workshop in Clinical Periodontics. Chicago: The American Academy of Periodontology; 1989: I/23-I/24.
- Armitage, G. C. (1999). Development of a classification system for periodontal diseases and conditions. Annals of Periodontology, 4 (1), 1-6.
- van der Velden, U. (2005). Purpose and problems of periodontal disease classification. Periodontology 2000, 39, 13-21.
- Caton, J. G., Armitage, G., Berglundh, T., Chapple, I. L. C., Jepsen, S., Kornman, K. S., et al. (2018). A new classification scheme for periodontal and peri-implant diseases and conditions – Introduction and key changes from the 1999 classification. Journal of Clinical Periodontology, 45 Suppl 20, S1-s8.
- Tonetti, M. S., Greenwell, H., & Kornman, K. S. (2018). Staging and grading of periodontitis: Framework and proposal of a new classification and case definition. Journal of Periodontology, 89 Suppl 1, S159-s172.
- El-Naggar, A. K., Chan, J. K. C., Rubin Grandis, J., Takata, T., Slootweg, P. J., International Agency for Research on C. (2017). WHO classification of head and neck tumors. Lyon, France: International Agency for Research on Cancer (IARC) Lyon, France.

By: Jonathan Du Toit
Date: February 26, 2024
Featured Digest articles
Insights and advice from Spear Faculty and industry experts


