Maxilla Is Key in Comprehensive Treatment Planning
Overjet makes rehabilitation dentistry technically difficult. Too much overjet can be problematic, but the solution is almost universally a surgical correction. Too little overjet (end-to-end) is much more difficult.
Posteriorly, we can accept cross-bites or camouflage them by altering the crown form. Anteriorly, there are few restorative options to correct or camouflage. Unworn posterior teeth typically take away the option of altering vertical dimension, given the amount of dentistry required on virgin teeth. Prerestorative orthodontics can improve the spacial relationship of the teeth. Orthodontic intrusion can align gingival margins and correct interarch discrepancy and allow the teeth to be restored.
The limitation is that we’re still working within the confines of the existing skeletal relationship. If the problem is greater than dentoocclusal and is skeletal, the damage to the patient may be significantly more impactful than poor dentofacial esthetics and altered function — it may be life-threatening. More importantly, it may be improved or cured by idealizing the skeleton.
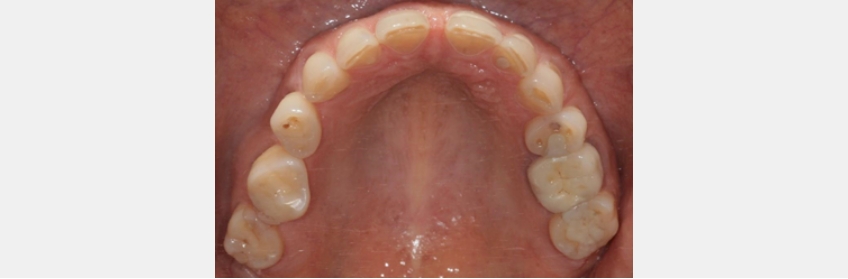
Airway before tooth position
Facially Generated Treatment Planning (FGTP) has its foundation in EFSB (Esthetics, Function, Structure, Biology). Esthetics leads the planning of comprehensive care by determining the incisal edge position of the central incisor. Once that position is properly established, we then determine how the lower arch will function against it. Finally, structural and biologic issues are addressed.
In 2016, Spear Education evolved the FGTP concept by declaring that the airway should be examined before tooth positioning is initiated. In many cases, the esthetic and functional positioning of teeth can be carried out in several ways. Some of those plans are more positive for the airway and others more negative.
For example, for a patient with a hypoplastic maxilla and end-to-end tooth wear, expanding the maxilla surgically would routinely be more positive for the airway than extracting lower teeth and retracting the lower arch. The esthetics of the smile and bite may appear the same, but technically the extraction and retraction idea may create or worsen an already compromised airway.
Focusing on the maxilla is not new
The idea of focusing on the maxilla as we begin treatment planning is not new to Spear Education. FGTP uses a 2D template to position incisal edges and free gingival margins in the smiling face. The addition of airway makes the templates 3D, adding the sagittal and transverse.
The best example of this returns to the original principles taught by Dr. Frank Spear. He would say all complex rehabilitations begin by figuring out the incisal edge position of the maxillary central incisors, just like setting a denture. The simplicity of the technique allowed us to become comfortable with comprehensive case planning.
There was, however, a flaw in what Dr. Spear taught: Dentists never begin by putting the wax rim in the mouth, marking the midline, and setting the centrals. Instead, every dentist places the maxillary wax rim in the mouth and adjusts the vertical, anteroposterior, and transverse position of the wax before considering setting teeth.
A dentist would never consider leaving the wax deficient and simply adjust the number, size, or inclination of the teeth to fit within the confines of the wax. All practitioners would simply add wax or move the rims to idealize the position.
In analyzing the wax rim, the A/P and transverse dimensions represent the airway. People with narrow or deficient wax rims aren’t as healthy as those with ideal wax rims. Therefore, the evolution in FGTP is to always consider making the skeletal base or alveolar housing normal before considering “setting teeth.”
Maxillary growth and development are intramembranous. The mandible’s growth is endochondral. It has a preestablished pattern (e.g., Meckel’s cartilage in the mandible), whereas the maxilla is more like a papier-mache balloon. The skeleton is laid down around the form that you grow.
The elements that help the maxilla grow are force and pressure. Pressure is from nasal breathing. Force is from the tongue in the roof of the mouth during breathing, proper tongue function in swallowing, and utilization of the face muscles in eating, gnashing, and grinding.
Dysfunction of any or all these elements will alter craniofacial development. Common dysfunctions include large tonsils and adenoids limiting nasal breathing and a tongue tie preventing proper positioning and function.
While function can alter the form of the developing maxilla, a poorly developed adult arch form can also alter function. A hypoplastic maxilla can alter how a person breathes and affect their health. If the maxilla is normalized, their health may improve. Said another way, improving the esthetics and function of the maxilla may improve our patients’ overall health. This concept is used in case presentations to provide a desire for patients to seek comprehensive care.
Here’s the proof
Recent studies in the otolaryngology literature are providing dentists with support for a new paradigm. The newest research shows that a narrow, highly vaulted maxilla in the premolar region increases the risk of having obstructive apnea.
In a separate study, it was determined that a narrow maxilla creates palatal or base tongue collapse. Further, the location of the narrowing is linked to different types of blockages: Molar narrowing creates different obstructive points than premolar narrowing. Lastly, if the maxilla is expanded, the airway collapse is reduced significantly.
In conclusion, given that the maxilla forms the support for the nose and nasal function, idealizing its dimensions by placing the teeth and bone in the ideal esthetic and functional position can reduce nasal resistance and nasal valve collapse. Additionally, maxillary expansion in adults can improve oral volume for the tongue function and clearance from the airway and increase tension and tone the muscles and soft tissues of the velopharynx, thus reducing collapse.
References
- Vinha PP, Thuler ER, de Mello-Filho FV. (2020). Effects of surgically assisted rapid maxillary expansion on the modification of the pharynx and hard palate and on obstructive sleep apnea, and their correlations. Journal of Cranio-Maxillofacial Surgery, 48(4), 339-348.
- Thuler E, Rabelo FA, Yui M, Tominaga Q, dos Santos V Jr., Arap SS. (2021). Correlation between the transverse dimension of the maxilla, upper airway obstructive site, and OSA severity. Journal of Clinical Sleep Medicine, 17(7), 1465-1473.
SPEAR campus Workshops
Step Into a Place Built for Mastery
Step away from the noise of practice and into focused, immersive training that changes how you think, diagnose, and lead.

By: Jeffrey Rouse
Date: March 28, 2022
Featured Digest articles
Insights and advice from Spear Faculty and industry experts


