Restoration of the Peg Lateral: The Direct Resin Approach
The peg lateral is a form of microdontia, a condition of having one or more disproportionately small teeth. Other teeth commonly involved are the third molar and premolar teeth. Microdontia may be classified as:
- True Generalized: This is where all the teeth are well-formed and of normal anatomy. However, the teeth are smaller than the normal range. It is a rare condition and usually affects patients with syndromes such as Down syndrome or pituitary dwarfism. It isn’t commonly seen outside specialist pedodontic practice.
- Relative Generalized: In this condition, the teeth are within the normal range of size and anatomy; however, dento-alveolar disproportion gives the impression of microdontia.
The condition tends to be inherited and is more common in some racial groups, especially those from West Africa and the Gulf Arab states. In my opinion, it’s a normal variant. However, if the patient requests treatment, it is often better approached via a combination of orthodontics, so the tooth substrate is within the restorative envelope, in addition to a final restoration with indirect ceramic veneers.
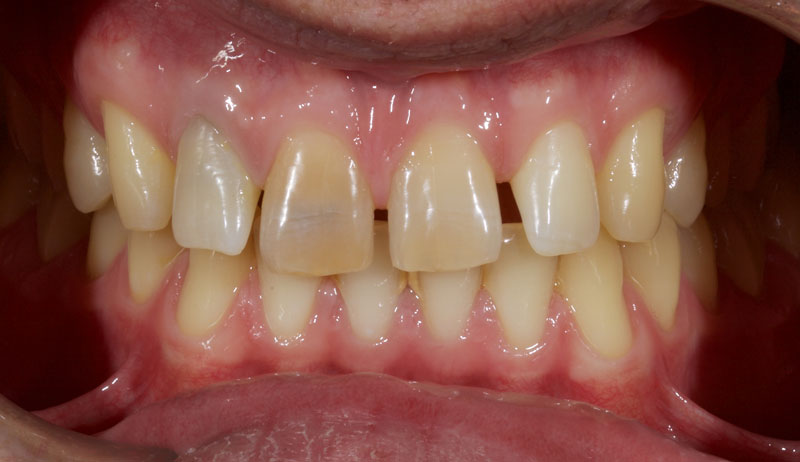
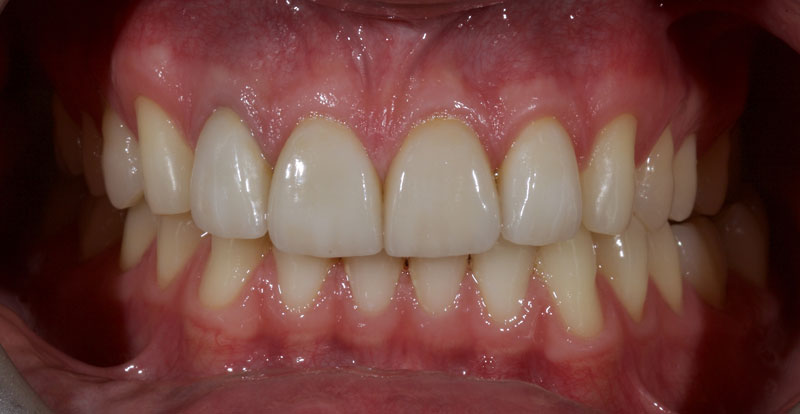
Treatment with direct resin is challenging due to the multiple diastemata and the potential risks of overhangs, defective contact points, and canted midlines. See Fig. 1 (before treatment) and Fig. 2 (after treatment).
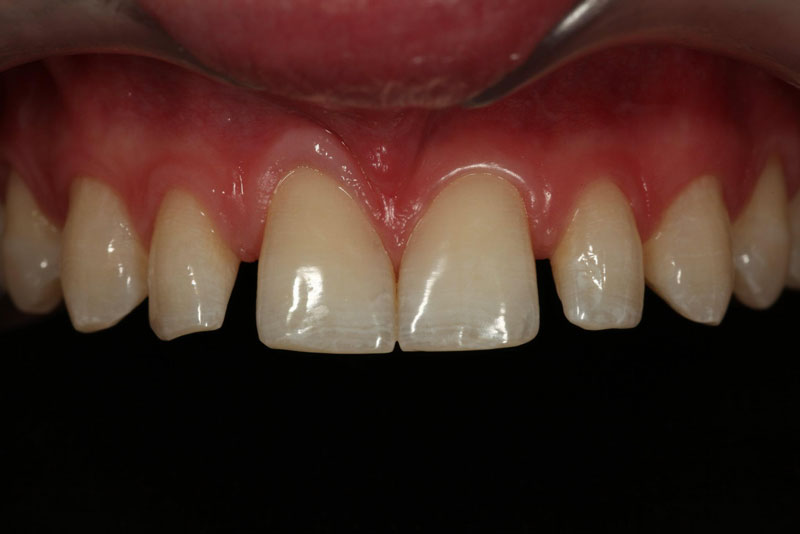
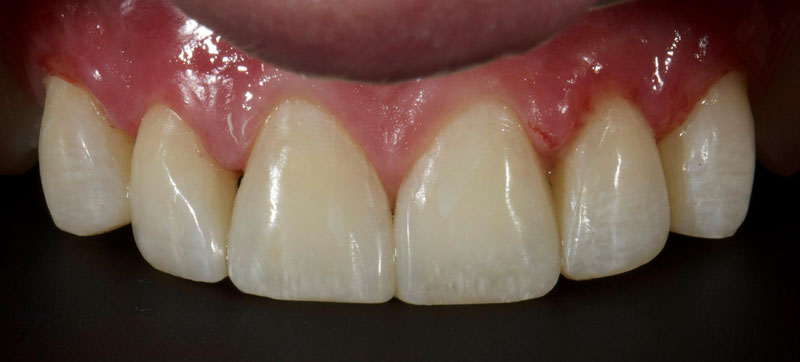
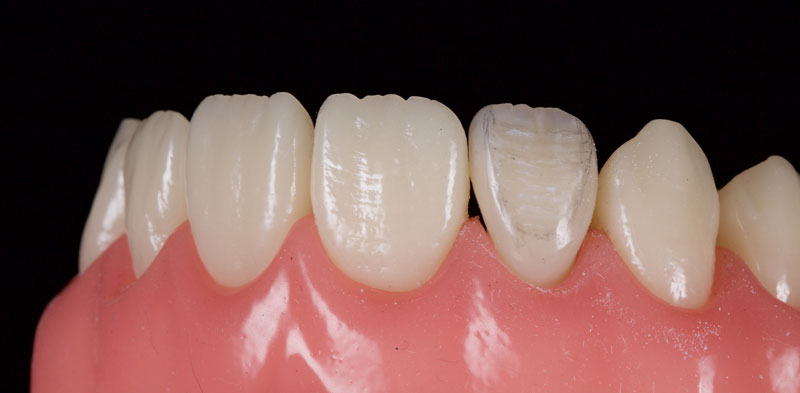
- Single Tooth: This is a microdontia localized to one tooth. Most peg laterals seen in a general dental practice setting will be of this type. See Fig. 3 (pre-op) and Fig. 4 (immediate post-op treated with direct resin).
How common is the single tooth localized peg lateral in clinical practice? The answer really depends on your patient base and location. According to 1986 research, results showed a very low incidence of 0.3% in a northern European population, whereas in 1996, research demonstrated a much higher incidence of 8.4% within a Japanese cohort.
The incidence appears to be much higher within patients seeking orthodontic therapy for obvious reasons, as an additional researcher cited 9.9% in 1998.
This highlights the need for a team, multi-specialty approach to orthodontics. It may allow an interested generalist to create a micro-specialty of composite resin-ortho interface within their practice.
I’ve found this to be well-received by both orthodontists, patients, and referring dentists. It’s also professionally and financially rewarding.
- Treatment planning: The assessment can be done simply via clinical examination, though study casts/scans may be employed if they are available. The peg lateral should be observed from the occlusal aspect (Fig. 5).
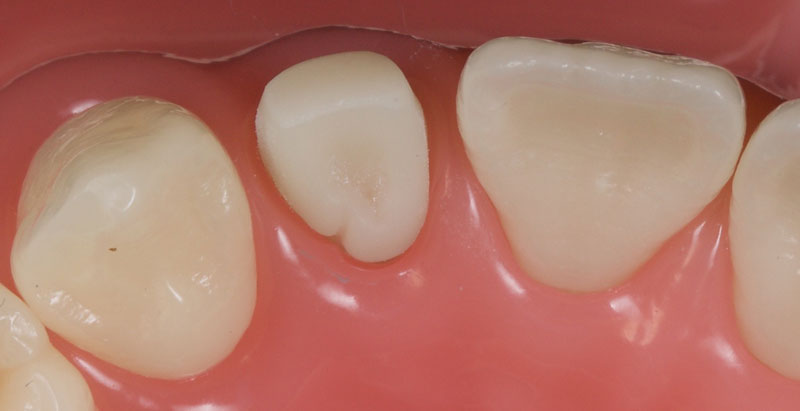
Ideally, the tooth should be in the center of the space mesio-distally, so the mesial and distal gingival emergence profiles are optimized. Furthermore, the incisal-facial portion of the tooth must be around 1 mm palatal to the adjacent canine and central incisor — that is, the peg lateral needs to be slightly palatally placed.
In my experience, the most common reason for the peg lateral restoration’s restorative failure is inadequate restorative space, which results in a bulky buccally placed veneer.
A diagnostic mock-up is critical to control the palatal aspect of the restorative envelope, and then, by default, the layering thicknesses of the resin. This is achieved by either:
- Analog: An alginate impression is taken, and stone models are cast. The proposed final restoration anatomy is then waxed onto the cast.
- Digital: A scan is taken, and the restoration is digitally waxed. The model is then 3-D printed. I prefer this approach since it offers more control and allows a digital preview. Models can also be stored as files.
Either way, a palatal putty matrix is fabricated on the model.
If there is inadequate space to restore the tooth or it is incorrectly positioned, consideration should be given to:
- Orthodontic therapy: This is usually the best course of action; although is sometimes declined (particularly in older patients) due to costs or timeframes.
- Minimal tooth preparation/reduction (Fig. 6): This is employed when orthodontics is declined or if the patient already has a Class I incisal relationship with an acceptable overjet and overbite.
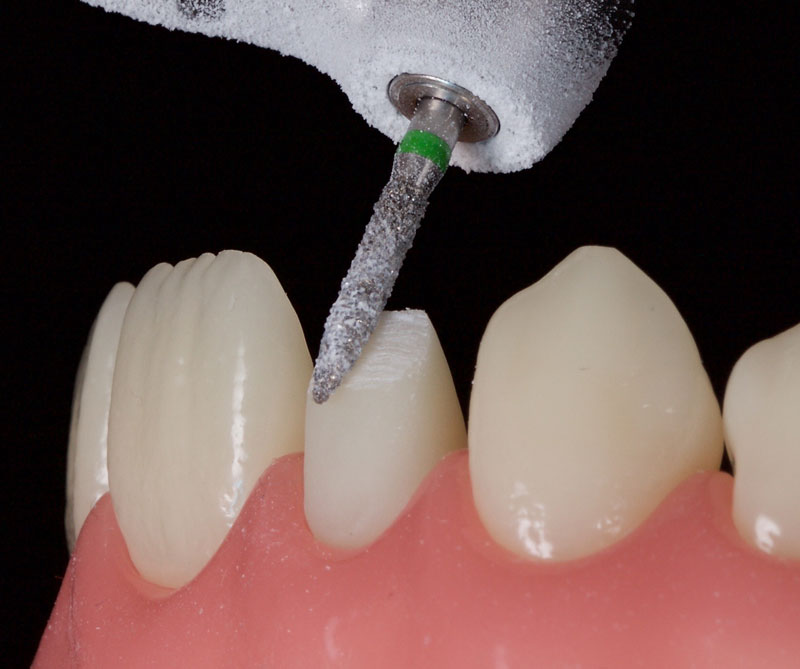
This is best achieved by cutting uniform 1.0 mm-deep cuts (dimples or grooves). The tooth is then reduced with a coarse crown diamond, followed by polishing with fine diamonds/discs to smooth the enamel and reduce the risks of white lines due to “enamel peel” (cohesive enamel failure). Typically, only the incisal-facial half must be reduced, leaving the gingiva untouched.
Clinical Pathway
The tooth is isolated for restorative convenience ideally with “split” rubber dam. Conventional rubber dam placement is not encouraged since gaining access to the gingival sulcus to obtain the correct emergence profile is challenging.
The tissues are retracted with a simple retraction cord to optimize access and reduce contamination via crevicular fluid. Preoperatively, the tissues should be in optimal health, and the cord should be soaked only in water (hemostatic agents tend to discolor the resin margins).
Particle abrasion (sandblasting) is carried out with 27-micron alumina at a pressure of around 2-3 bar. The aim is to remove aprismatic enamel and optimize bond strengths. Particular attention should be paid to the cingulum pit, which is often very deep, teardrop-shaped, and debris-filled. Care should be taken to avoid the tissues, which may cause bleeding.
The tooth is then etched, primed, and bonded with a dentin-bonding agent. I prefer a 4th-generation dentin bonding agent since it has the best data and highest bond strengths (Fig. 7).
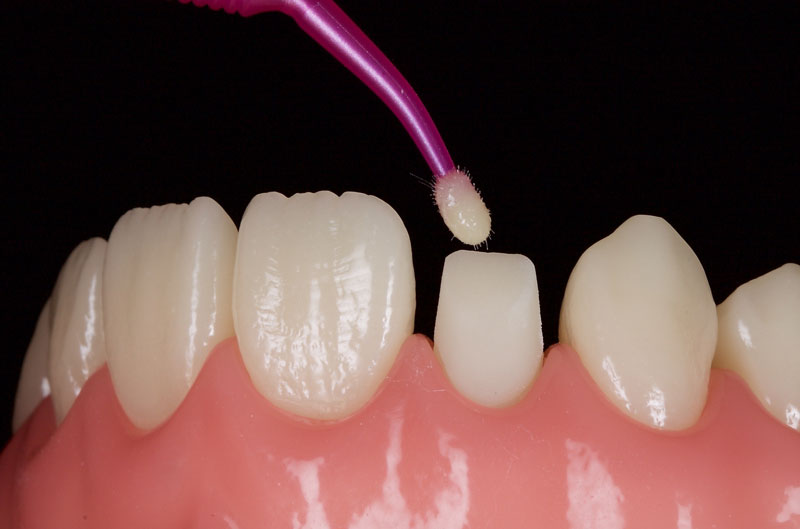
It’s often prudent at this stage to fissure seal the palatal cingulum with a high viscosity flowable composite.
An achromatic enamel shade of low opacity (e.g., GC G-aenial Junior Enamel) is placed on the putty matrix and thinned to a section of 0.1–0.3 mm with an artist’s brush and a modeling resin (e.g., Brush and Sculpt, Cosmedent). This is then adapted to the tooth to form a palatal shell (Fig. 8).
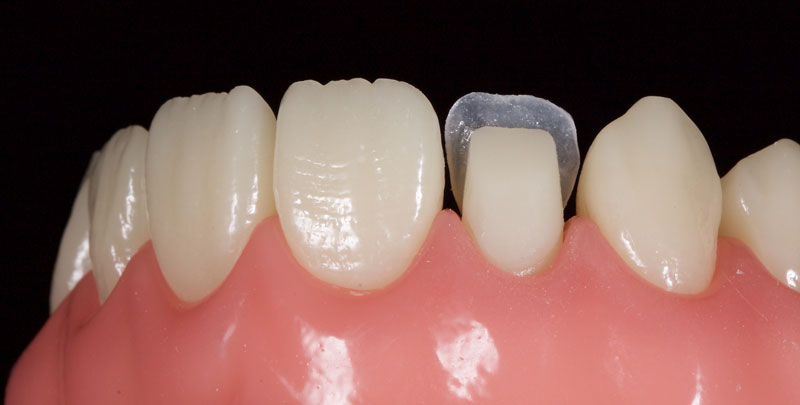
Matrices are then placed to aid the creation of contacts and an ideal emergence profile. My preference is either Mylar strips or posterior matrix bands (e.g., Paladent or Garrison) placed on end (Fig. 9).
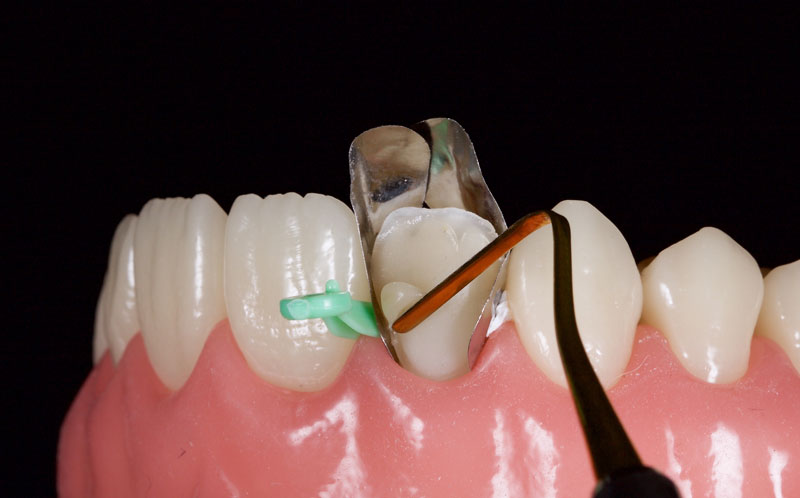
These can be anchored with Teflon tape or conventional plastic wedges. A dentin (medium opacity) resin is placed to block out light transmission and maintain the restoration’s value in comparison to the surrounding tooth structure. This should be under contoured facially.
Chromatic composite of the correct VITA shade is then placed to full contour in the gingival and mid thirds (Fig. 10). The incisal third is under contoured and dentin mamelons are modeled.
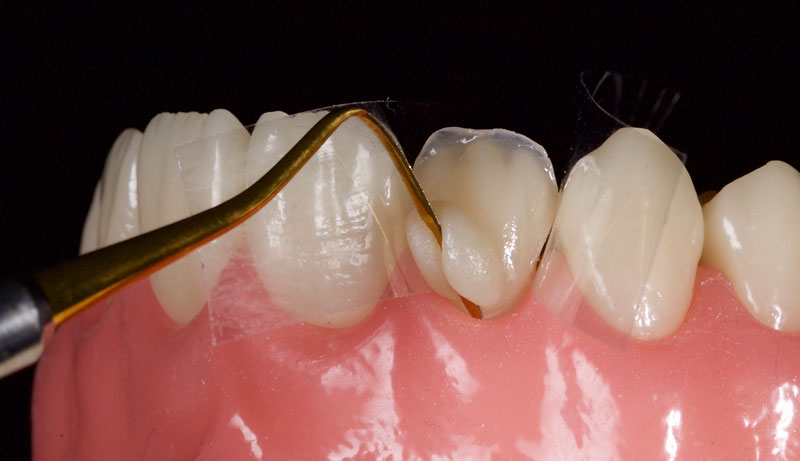
White, amber, and other characterizations can be added to the incisal edge as desired (Figs. 11 and 12).
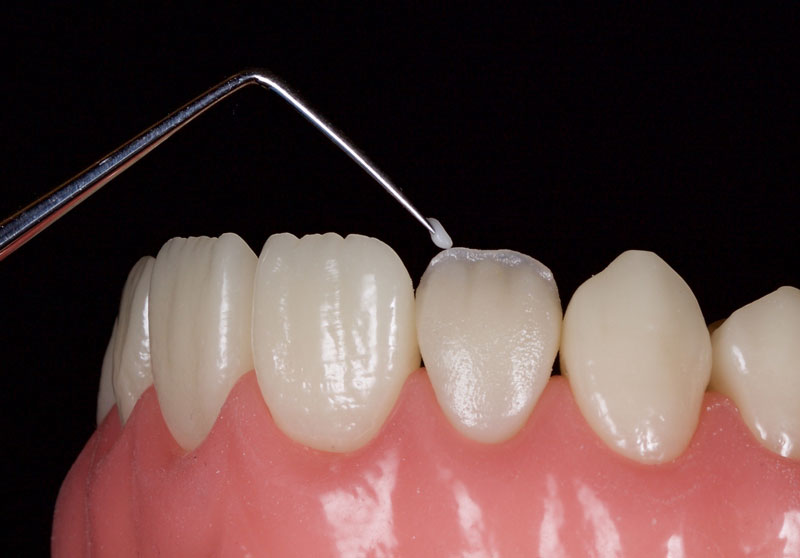
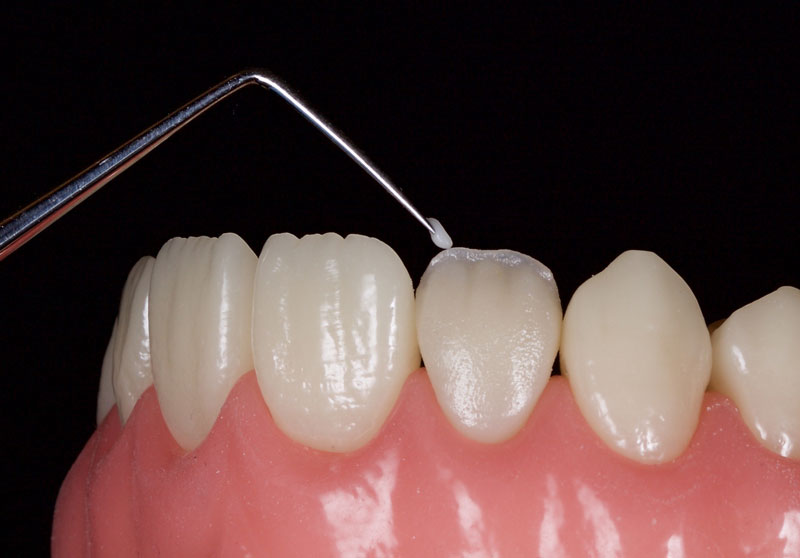
If appropriate, a highly translucent opalescent enamel mass can be modeled sparingly at the incisal edge, for example OBN, Micerium (Fig. 13).
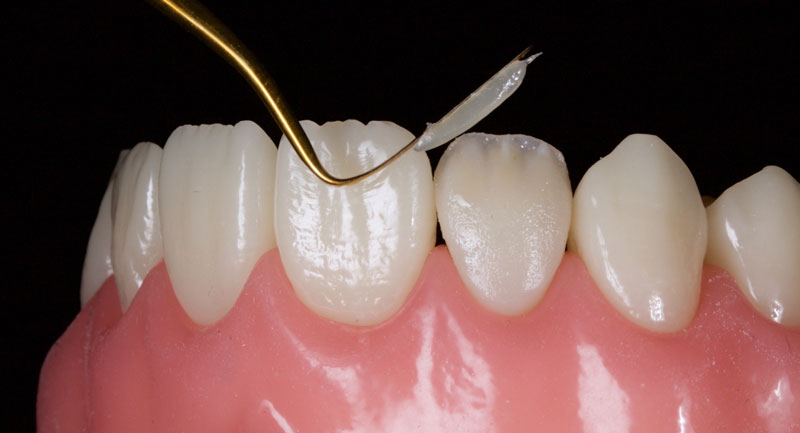
Finally, the incisal third is overlaid facially with a highly translucent enamel shade, e.g., WE Tokuyama (Fig. 14). This is smoothed and adapted with a No. 3 artist’s brush and a wetting resin.
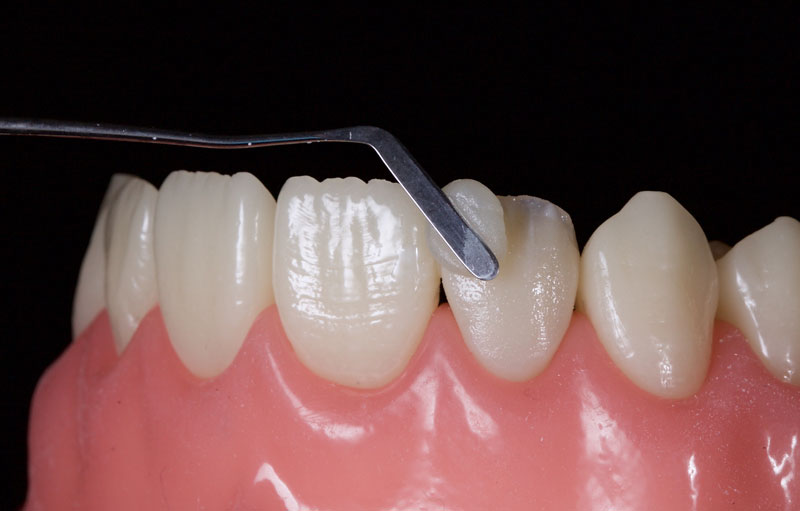
The entire restoration is then covered with glycerin and polymerized with a curing light for 40s per surface to remove the oxygen-inhibited layer.
The restoration is then finished with a combination of discs (e.g., 3M Soflex or Cosmedent Flexidisc) to create the height of contour and line angles. Rubber points of varying grades (e.g., Astropol, Ivoclar) are then used to create mamelon grooves and lobes (Fig. 15).
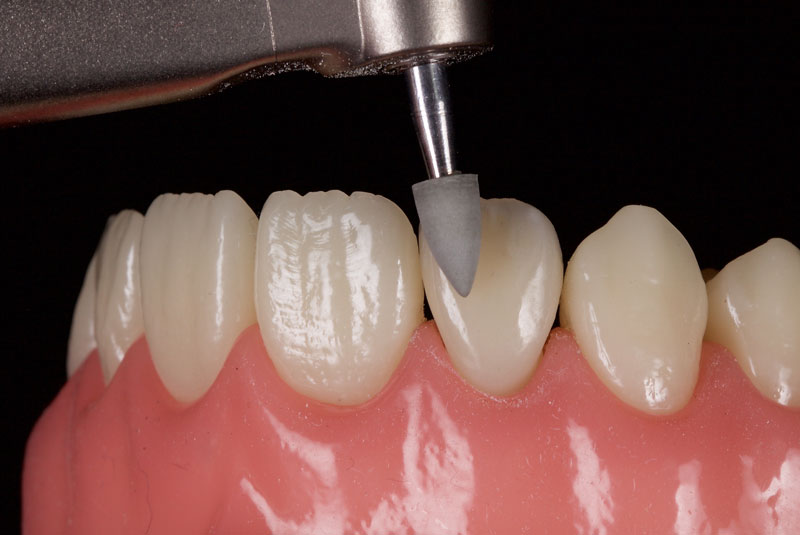
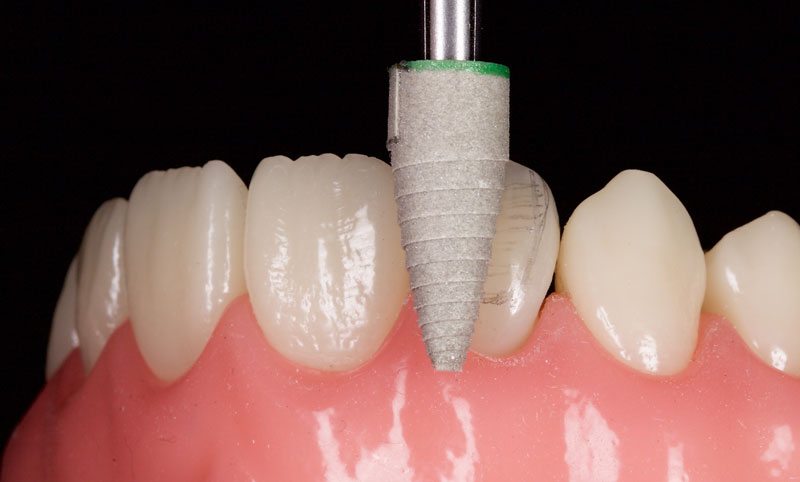
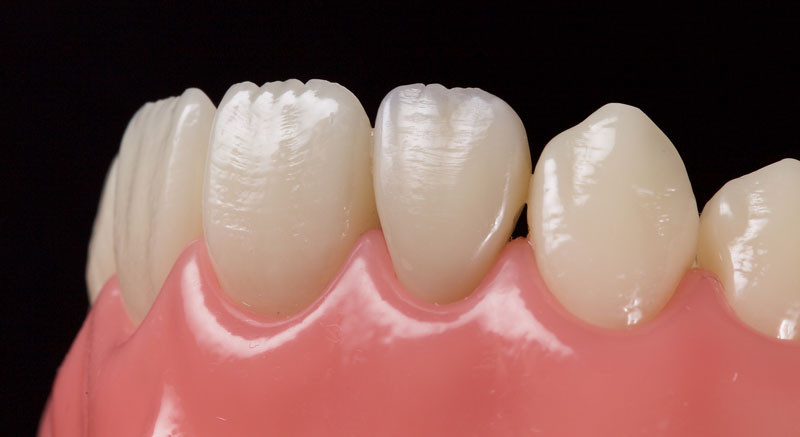
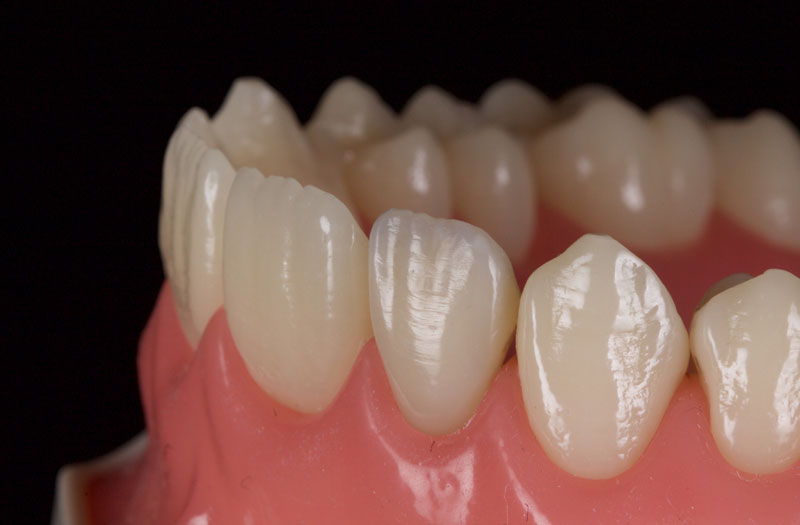
After a final polish with a felt wheel and aluminum oxide polish (Flexibuff and Enamelise, Cosmedent) at decreasing pressure and increasing speed, the restoration is complete (Figs. 18 and 19.)
References
- Brin, I., Becker, A., & Shalhav, M. (1986). Position of the maxillary permanent canine in relation to anomalous or missing lateral incisors: a population study. The European Journal of Orthodontics, 8(1), 12-16.
- Ooshima, T., ISHIDA, R., MISHIMA, K., & SOBUE, S. (1996). The prevalence of developmental anomalies of teeth and their association with tooth size in the primary and permanent dentitions of 1650 Japanese children. International Journal of Paediatric Dentistry, 6(2), 87-94.
- Thongudomporn, U., & Freer, T. J. (1998). Prevalence of dental anomalies in orthodontic patients. Australian Dental Journal, 43(6), 395-398.
VIRTUAL SEMINARS
Stay Sharp. Stay Current. Stay Ahead.
Join live, focused training designed to help you implement immediately and strengthen your expertise.

By: Jason Smithson
Date: October 5, 2020
Featured Digest articles
Insights and advice from Spear Faculty and industry experts


