Implant Crowns: Cement, Screw or Both?
A considerable debate in implant dentistry is whether to use a screw-retained or cement-retained restoration. Knowing the early history of dental implant restorations helps us understand the options available in modern implant dentistry.
When implants were first introduced, many of today’s common features, such as internal connections and anti-rotational designs, were absent. Since implant systems lacked anti-rotational features, splinting an implant restoration to a natural tooth was necessary. As implant technology advanced, anti-rotational designs were introduced to help fabricate free-standing implant crowns1.
In the late 1980s, screw-retained implant restorations were developed to address concerns about retrieving implant crowns and whether they needed to be repaired or replaced. With advancements in implant restoration techniques, such as custom abutments, cement-retained implants became more popular2. By the early 2000s, most implant restorations were cement-retained.
Cement-Retained Implant Restorations
Cement-retained implant restorations consist of an abutment upon which the implant crown is cemented. Abutments can be prefabricated “stock” or custom.
One advantage of a custom abutment is that the margins can be modified to create a supragingival interface between the implant crown and the abutment. This helps make it easier to remove excess cement. Cement-retained implant crowns are often considered more esthetic than screw-retained implant crowns since the cement-retained implant crown does not have an access hole.
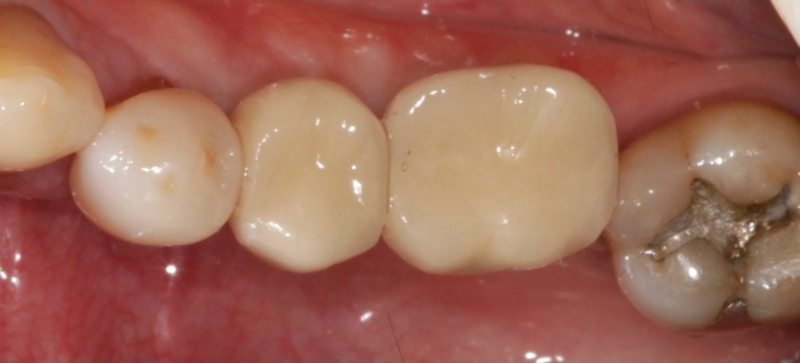
However, cement-retained implant crowns can present challenges if cement is not effectively removed. This is especially true for prefabricated abutments, where the margins can be millimeters subgingival. Multiple studies have demonstrated that patients with cement-retained implant crowns with excess cement are at a higher risk of developing peri-implantitis.
Dr. Chandur Wadhwani, a Seattle-area prosthodontist, demonstrated how excess implant cement can lead to inflammation around implants, contributing to bone loss and peri-implantitis3. As a result, it is advised to design implant crown margins to remove excess cement and take a post-cementation radiograph to determine if excess cement remains after delivering a cement-retained implant crown.
Dr. Georgios Kotsakis, a University of Texas Health Science Center School of Dentistry faculty member, suggests designing implant crown margins that do not extend more than 1.0 mm subgingivally and considering using zinc oxide eugenol or zinc phosphate cement rather than a resin-based cement. Resin-based cements may experience greater biofilm accumulation than zinc oxide eugenol or zinc phosphate cements, leading to a significant risk of inflammation around the implant restoration2.
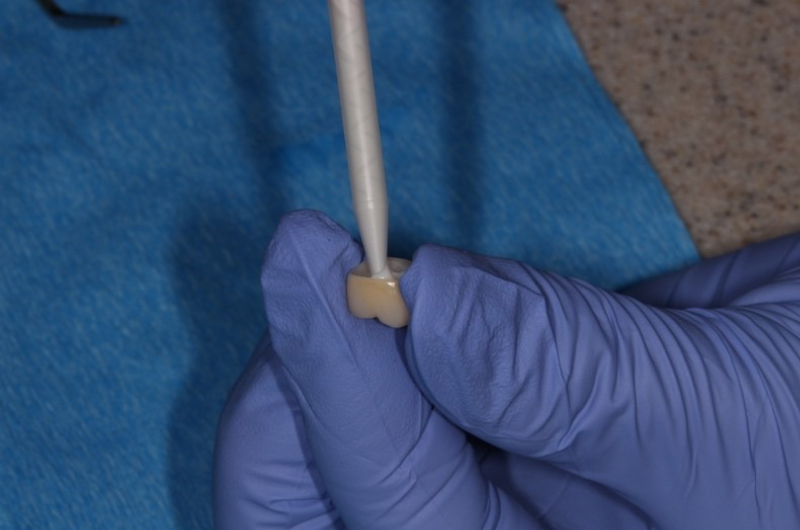
In addition, an impression of the intaglio surface of the crown can be used to minimize the amount of excess cement in an implant crown. Before cementing the restoration, the intaglio surface of the implant crown is lined with Teflon tape. Putty, impression, or bite registration material is injected into the intaglio surface and allowed to set. This creates a die of the implant crown. When it is time to cement the restoration, the Teflon tape is removed, a thin layer of cement is placed in the intaglio surface of the crown, and the crown is seated back on the die. Excess cement will be extruded extraorally, minimizing the chance of leaving excess cement around the implant restoration4.
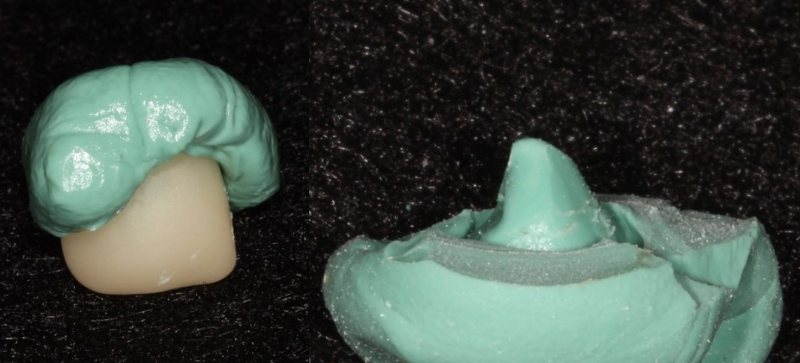
Figure 2B: Custom die created to express excess cement extraorally prior to cementation.
Screw-Retained Implant Restorations
A screw-retained implant restoration can be fabricated instead of a cement-retained implant restoration. Screw-retained implant restorations comprise a one-piece structure with the implant connection and restoration as a single unit.
Current research demonstrates the risks of peri-implantitis associated with cement-retained implant restorations, so many dentists are utilizing screw-retained implant crowns for single-unit implant restorations.
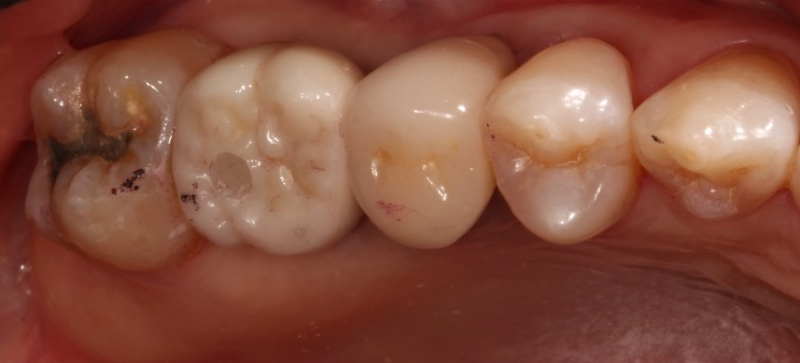
Two main advantages of screw-retained implant crowns are that they minimize the risk of peri-implantitis compared to cement-retained implant crowns and are also easier to retrieve. The ability to retrieve the restoration is helpful if the implant crown needs to be repaired or replaced due to fractured porcelain or an open contact between the implant crown and the natural tooth5.
However, drawbacks of a screw-retained design are that these restorations can be challenging to seat on the implant platform, and the presence of a screw access hole can lead to an unesthetic result if not appropriately managed.
The ‘Screwmentable’ Implant Crown
The “screwmentable” implant crown is another possible treatment option that combines the advantages of cement-retained and screw-retained implant restorations. In this crown, the abutment and implant crown are cemented extraorally. This can be done by the lab before the appointment or chairside.
In the chairside procedure, the abutment is placed on the implant, and the implant crown is adjusted as if it were a cement-retained restoration. After the contacts and occlusion are adjusted, the abutment is removed, the implant crown is cemented to the abutment extraorally, and excess cement is removed.

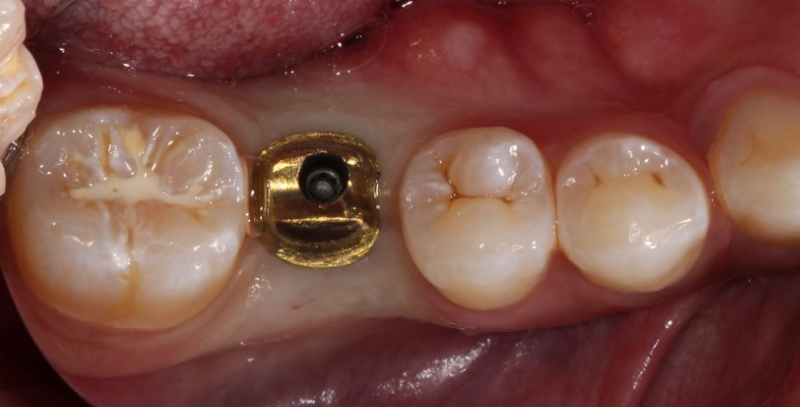

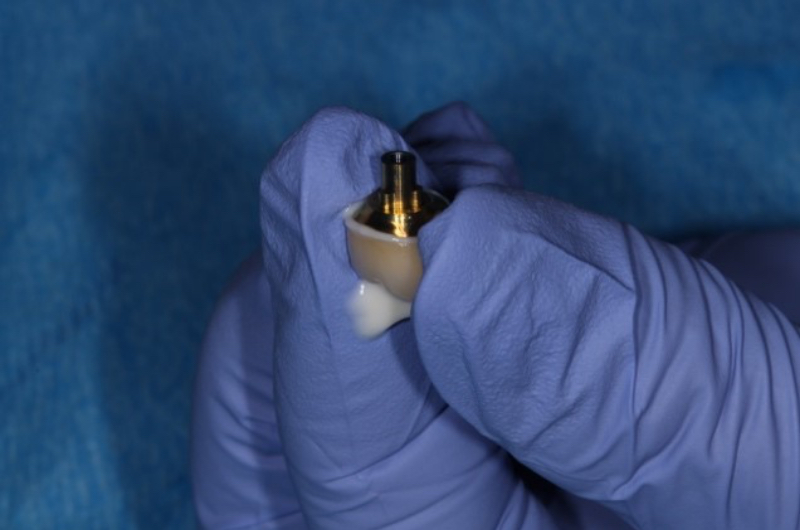
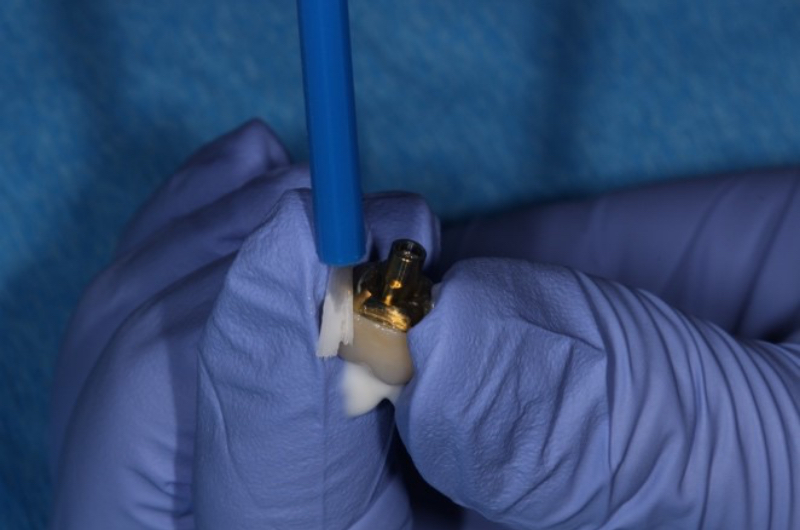
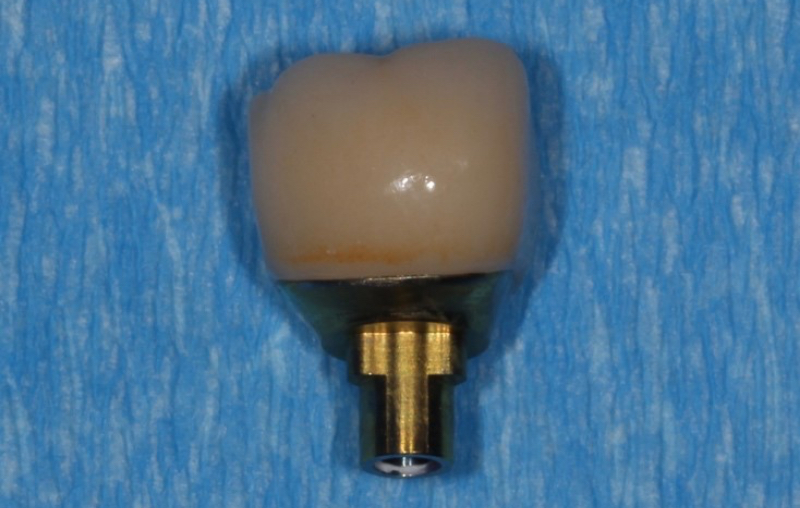
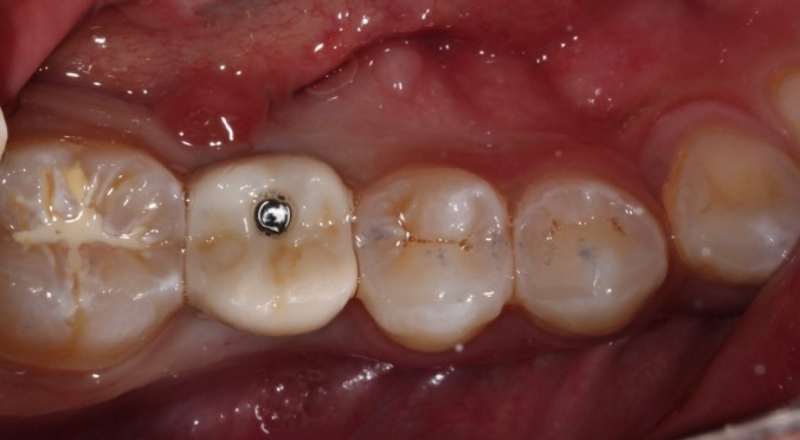
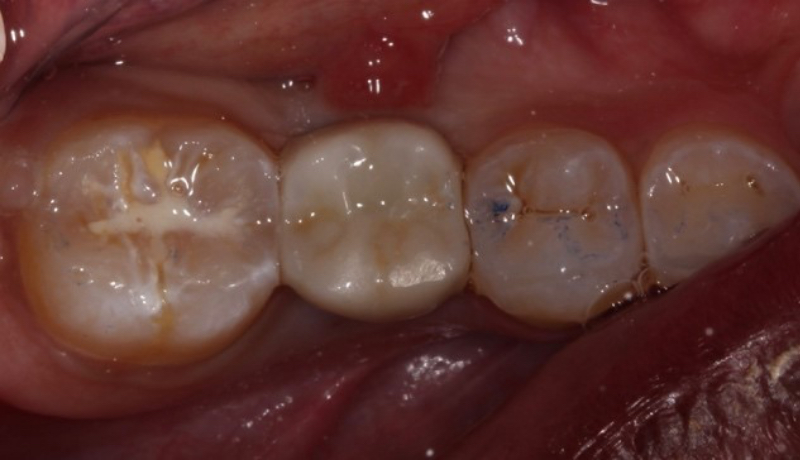
The abutment-crown complex now acts like a screw-retained restoration ready to be delivered.
In conclusion, there are various ways to restore single-unit implants. Depending on the clinical situation, screw-retained, cement-retained, or screwmentable options can be predictably utilized to restore implants with restorations that have ideal form and function.
References
- Spear, F. (2009). Connecting teeth to implants: The truth about a debated technique. The Journal of the American Dental Association, 140(5), 587-593.
- Kotsakis, G. A., Zhang, L., Gaillard, P., Raedel, M., Walter, M. H., & Konstantinidis, I. K. (2016). Investigation of the association between cement retention and prevalent peri‐implant diseases: a cross‐sectional study. Journal of Periodontology, 87(3), 212-220.
- Wadhwani, C., Rapoport, D., La Rosa, S., Hess, T., & Kretschmar, S. (2012). Radiographic detection and characteristic patterns of residual excess cement associated with cement-retained implant restorations: a clinical report. The Journal of Prosthetic Dentistry, 107(3), 151-157.
- Wadhwani, C., & Piñeyro, A. (2009). Technique for controlling the cement for an implant crown. Journal of Prosthetic Dentistry, 102(1), 57-58.
- Greenstein, G., Carpentieri, J., & Cavallaro, J. (2016). Open contacts adjacent to dental implant restorations: etiology, incidence, consequences, and correction. The Journal of the American Dental Association, 147(1), 28-34.
SPEAR campus Workshops
Step Into a Place Built for Mastery
Step away from the noise of practice and into focused, immersive training that changes how you think, diagnose, and lead.

By: Andy Janiga
Date: January 22, 2020
Featured Digest articles
Insights and advice from Spear Faculty and industry experts


