Invasive Cervical Root Resorption: The New Dental Epidemic?
If you have been in clinical practice for more than five years, you have probably thought you are now seeing many more cases of root resorption than you ever did before. If you have been in clinical practice for more than 20 years, you probably think there is a new epidemic of root resorption.
I’m not referring to replacement resorption, or ankylosis, which is typically seen after an avulsed tooth is replanted, nor the classic internal root resorption, but rather, “invasive cervical root resorption,” which is also known as “extra-canal invasive root resorption.” This type of root resorption starts on an external root surface, usually around the cervical level, progressively invading the root, going in a coronal and apical direction (Fig. 1).
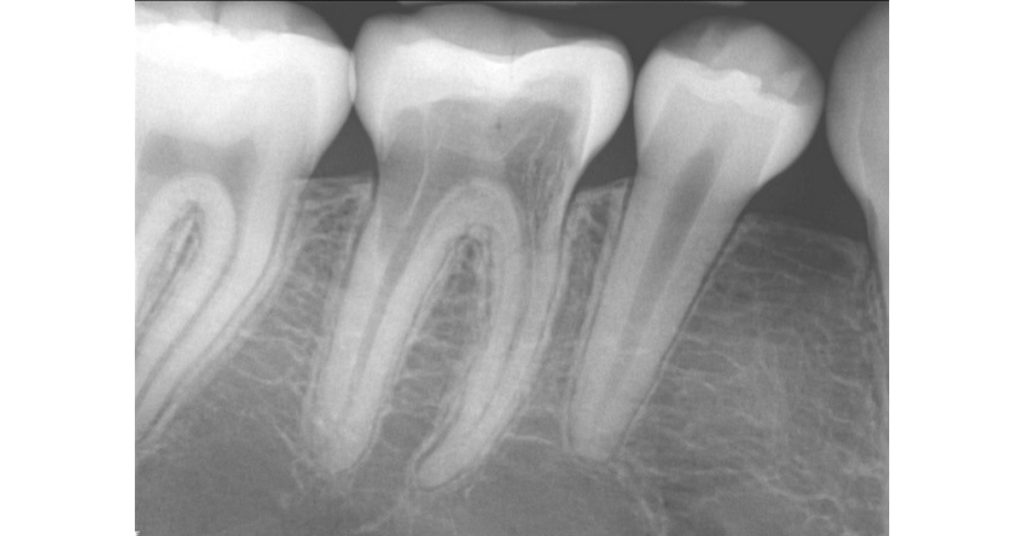
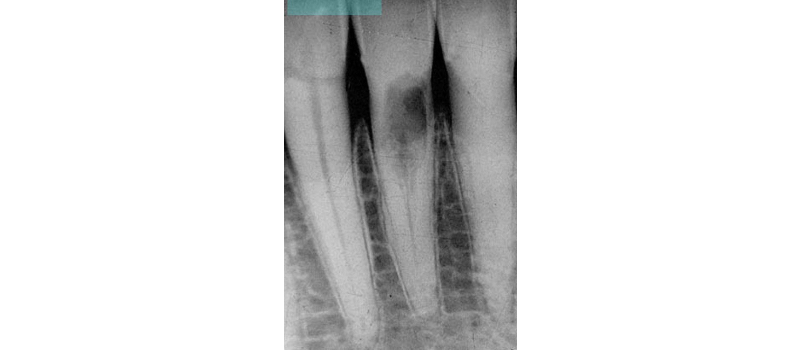
What’s unique about this type of root resorption is that it does not invade the pulp. In fact, the pulp in these teeth remains vital, and the resorption tends to navigate around the pulp canal (hence the alternate designation of extra-canal invasive root resorption). Radiographically, even with extensive cases of invasive cervical root resorption, you can still visualize an intact canal space (Fig. 2).
In years past, the treatment management was to initiate endodontic treatment, place calcium hydroxide, and continue changing the calcium hydroxide every few months with the hope of slowing down or stopping the resorption process. This was not met with great success, but with no surprise, since the pulp in these teeth is normal unless there was an underlying pre-condition (noting that this resorption often occurs on virgin teeth).
Recognition and location of these resorption defects can be a challenge. Multiple radiographic angles can be helpful, but CBCT has been a great asset for determining the location and extent of the resorption. The extent of the lesions has been classified, with a Heithersay 1 defect indicating the least amount of resorption and a Heithersay 4 defect indicating the most resorption.
There is no great answer to why these defects occur, or even why we seem to think that they are occurring more now than before. Orthodontic treatment seems to be correlated with invasive cervical root resorption, and in a small study, a particular feline herpetic virus has been associated with it (yes, a cat virus, noting that about 50% of cat teeth have this type of defect).
In the most general terms, this type of root resorption will continue to progress unless the defect is wholly removed. This is done by a surgical approach, reflecting a full-thickness gingival flap from the sulcus, debriding the entire defect with burs, curettes, and/or various acidic compounds (such as trichloro-acetic acid), and then filling the defect with a restoration.
Typically, Geristore® is the restoration of choice because it helps to promote a connective tissue attachment to the tooth. So, the big question is: if you reflect a full-thickness gingival flap from the sulcus, remove the resorption defect, place a restoration in the defect, and suture the flap back in place, will the gingival healing result in a gingival and bony dehiscence over the root surface? Will the treatment be worse, “just leaving it alone?”
When considering whether to treat these types of defects, two main considerations are the speed of the defect’s progression and how much resorption has taken place, both of which are difficult to assess.
Historic radiographs can be very helpful in determining how fast the resorption is progressing. If the resorption has not changed over many years, you may consider no treatment at all. If the resorption has taken away so much root structure that removing it and restoring it may either compromise the integrity of the root or have a great chance of creating a gingival or bony dehiscence, then you may want to think twice about considering treatment.
Another factor that is not discussed much is the age of the patient. For example, if the patient is asymptomatic (and usually are with these types of defects), you may consider managing a 25-year-old differently than a 90-year-old. Hypothetically, if no treatment is a consideration, and if your best guess is that you will get at least 10 years with no treatment, then you may be safe with no treatment for the 90-year-old.
The proper management of invasive cervical root resorption depends on a proper diagnosis (where is the defect, is it accessible for surgical removal, and how extensive is it?) and the prognosis in the event of treatment or no treatment. Unfortunately, these considerations are not so black and white. With no treatment, you run the risk of providing “supervised neglect” and allowing the defect to get worse over time. In contrast, with treatment, you run the risk of creating a gingival and bony dehiscence and subsequently compromising the socket for an implant.
Many variables must be considered when managing invasive cervical root resorption. The Endodontic Diagnosis and Dental Traumatology Spear Online courses offer more detailed endodontics training.
SPEAR ONLINE
Follow a Clear Path to Clinical and Practice Confidence
Next-level confidence isn’t random. It’s structured. Follow a clear pathway that will accelerate your clinical and practice progression.

By: Lou Berman
Date: September 4, 2019
Featured Digest articles
Insights and advice from Spear Faculty and industry experts