Hybrid Digital/Analog Technique for Maxillofacial Prosthodontics
By Brandon Stapleton on January 24, 2018 | commentsI often feel as a prosthodontist that I’m constantly brainstorming new ways to make things that don’t work with traditional techniques possible with new or hybrid techniques.
That’s exactly what Bart Hyde, C.D.T., and I did with a recent provisional complete obturator prosthesis. Often times with these maxillofacial cases, we’re working in very difficult and restrictive spaces due to muscle contracture from radiation. This causes limited opening, microstomia and xerostomia along with other, often compounding, factors.
Let me introduce to you Debbie, a 52-year-old cancer survivor. In 2014, Debbie completed surgical and radiation therapy to treat primary adenoid cystic carcinoma, which resulted in a hemimaxillectomy of her right maxilla.
There were subsequent attempts to close and reconstruct the defect with grafts. After her last surgical revision in 2016, her remaining maxillary dentition was condemned and arch bars were used to stabilize the dentition until a plan could be made for transition.
It is clinically and radiographically very obvious that periodontal disease and caries have destroyed the supporting structures around the remaining maxillary teeth. Debbie has a history of periodontal disease in the mandible; however, that it is under control at the moment.

In terms of complications, Debbie presented with a unique scenario that took some creativity and molding of some old and new techniques/technologies to get us to a provisional complete obturator prosthesis.
First, while Debbie performed well with her presenting situation, she had zero desire to walk around without teeth for weeks or months following extractions. She had a severely restricted opening complicated by supraeruption of the maxillary and mandibular anterior teeth - yielding approximately 10 to 15mm of inter-arch space on her left side where she still had opposing teeth.
Also, the maxillary soft tissue flap that covered much of her defect actually complicated prosthesis fabrication (and function). Bart Hyde, C.D.T., and I came up with an interesting way to capture our data for the provisional complete obturator prosthesis utilizing some new technologies and mixing it with some fundamental (a.k.a “old school”) prosthodontic techniques.
Our treatment plan included extraction of the remaining maxillary teeth, grafting of extraction sites and a provisional complete obturator prosthesis. Debbie desires an implant rehabilitation; however, space and bone availability was too difficult to assess with the teeth still in place (not to mention her limited opening, which severely compromises our definitive prosthesis design). We elected to proceed with the staged approach and will return for Phase II planning after healing.
The proposed plan was accepted and Phase I was executed. The restorative sequence was as follows:
1. We attempted maxillary/mandibular alginate impressions (and failed due to difficulty opening and limited inter-arch space).
2. Intraoral scans of maxilla and mandible were taken. I was unable to capture everything required due to her limited opening; however, all of the hard tissue and enough soft tissue was obtained, allowing me to come back to capture the tissue in an altered cast impression technique.

3. Maxillary baseplate/custom tray were used to capture the lateral extent of the right maxilla and posterior defect utilizing border molding compound and VPS bite registration material.

4. Using the printed dental cast of maxillary teeth, the remainder of the palate was removed and grooves were added to allow conversion to an altered cast.


5. The impression and printed cast were joined and boxed to allow fabrication of a hybrid altered cast.




6. The new hybrid altered cast was articulated.

7. Esthetic changes made during a new setup following ESFB protocol and immediate maxillary complete obturator prosthesis was completed. The hybrid altered cast was duplicated by Bart to fabricate the provisional complete obturator prosthesis on.

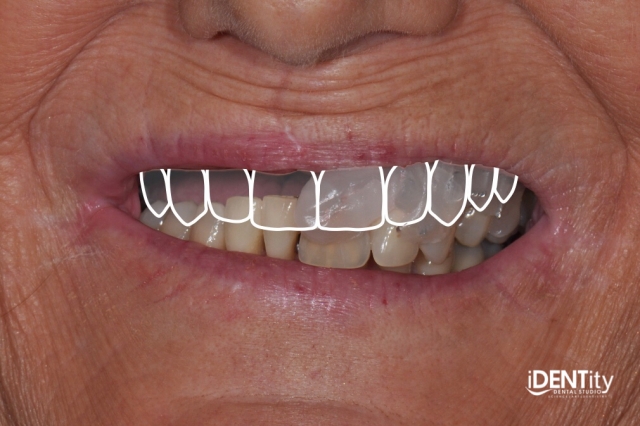


8. Maxillary teeth were removed and sites were grafted by oral surgeon Dr. Jason Ford, and the provisional maxillary complete obturator prosthesis was delivered.

We’re now approximately one month post-extraction and grafting. Once the graft and tissues have matured, we will proceed with a new CBCT scan, utilizing a double scan technique to integrate tooth position into the planning software.
Debbie has done remarkably well with the transition, although there were some initial adjustments required to retrofit the prosthesis around the defect and depressible tissues.
Maxillary provisional complete obturator prosthesis completed by Bart Hyde, C.D.T., Hyde Dental Prosthetics
Surgical procedures completed by Oral Surgeon, Jason Ford, D.M.D., M.D., The Kentucky Center for Oral and Maxillofacial Surgery
Brandon M. Stapleton, D.M.D., M.S.D.