Success in Space With a Fixed Hybrid Prosthesis
(Dr. William Runyon co-authored this article.)
The fixed hybrid has become an efficient and reasonable opportunity for patients to achieve a fresh new start with their dentition. But for the dental provider, it can also be considered as the final frontier, the last definitive opportunity for patients with terminal dentition. Success or failure is in our hands.
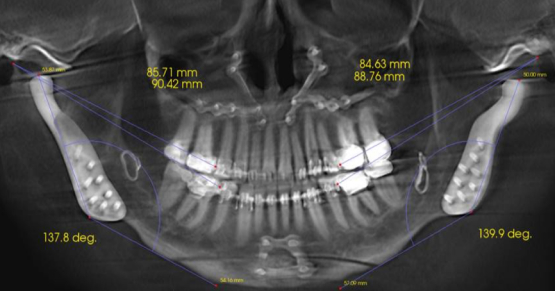
It is incredibly important for us to properly treatment plan these cases to mitigate potential risk and complications. Certainly the greatest risk is not providing enough prosthetic space. It is paramount the surgical team create enough vertical height from the implant level to the incisal edge of the prosthesis.
There has to be enough vertical height to stack components: abutments, Ti bar, the acrylic wrap and denture teeth. It is commonly reported in the literature that a minimum vertical height requirement is 15 to 16 mm from the fixture to the incisal edge.
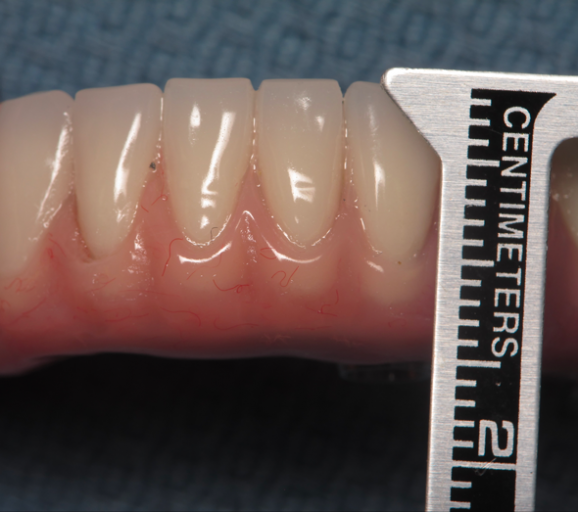
It is possible to restore a case with only 13 mm, but careful coordination is required with the lab, and certain patient anatomic and occlusal relationships are required.
If there is insufficient space, the patient will suffer from a failure of the prosthesis (displaced teeth, fractured provisional, or – rarely – a fractured bar or abutments) or potentially an un-esthetic outcome with the plane of occlusion in the wrong position in the vertical dimension of the face.
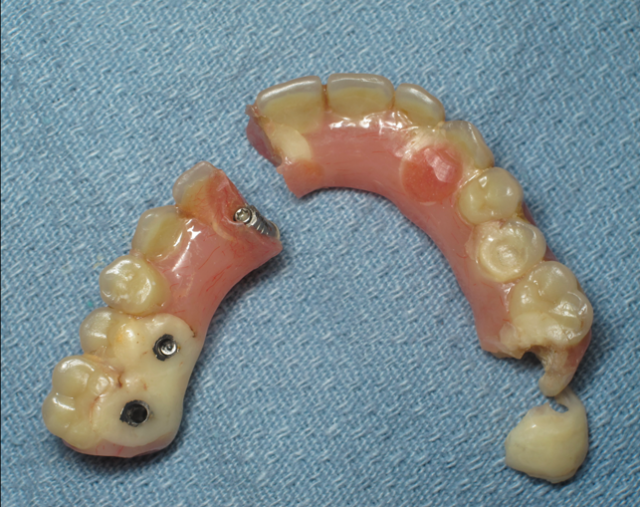
I have a dogma: A prosthetic failure of a fixed hybrid is a surgical complication, until proven otherwise. It’s important for the surgical team to accept this responsibility of creating enough space.
So where do we find success in space? Here are eight opportunities that our team considers:
1. The majority of our space is achieved through an aggressive alveolar reduction. Prior to extracting teeth but after the muco-periosteal reflection is completed, I will anatomically indicate the vertical reduction on the alveolus.
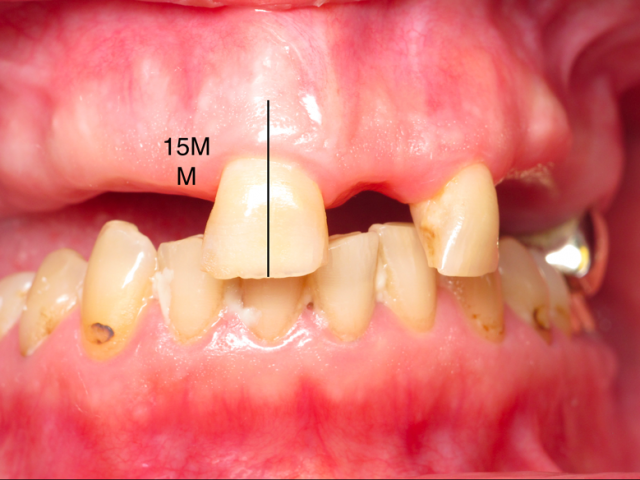
Using calipers set at 15 mm, I will measure from the incisal edge or buccal cusp tips and mark the alveolus. After the teeth are removed, then the bone reduction is completed down to the indicated marks, and I then have created the required space.
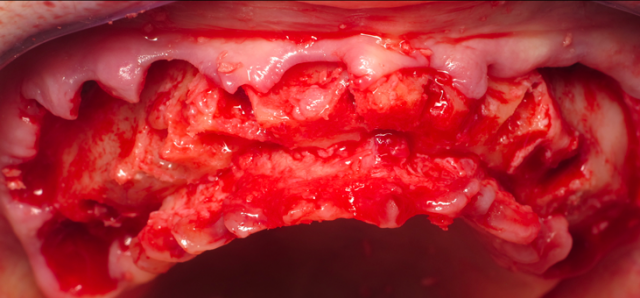
If the existing teeth are in the wrong position in the face, this needs to be taken into account for the calculation. I address these cases in an aggressive nature and will consider bone “as the enemy.” It’s an unnatural way for us in implant dentistry to “feel” about bone. But the consequences of leaving too much bone height is devastating to the patient’s final outcome with a fixed hybrid prosthesis.
2. If a patient has lost vertical and the anterior tooth show is insufficient, then we get “free space.” If a patient has minus 1 mm show in repose and the goal is 2 mm show in repose, then we get to subtract 3 mm from our 15 mm bone reduction.
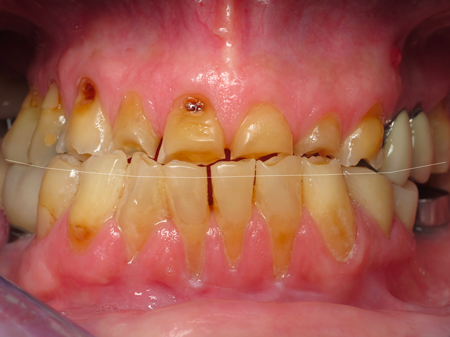
3. In a single arch case, reducing the opposing dentition is a quick way to gain a millimeter or two. We usually see this with super-erupted lower anterior teeth, especially if there is crowding. Performing an enamelplasty to equilibrate the opposing arch is a quick and easy opportunity to gain space.
4. Another opportunity in a single arch case – and when treatment time is on your side – is to consider orthodontic intrusion of the opposition dentition. We recently completed a maxillary arch, and the patient was extremely happy with the results. The lower dentitions were in great shape despite being crowded anteriorly with an uneven plane from canine to canine. She was excited to initiate orthodontics as an option to level and align her mandibular arch, and we were able to intrude the incisors 1.5 mm. This can be accomplished during the healing period when in the provisional.
5. When the anatomy allows, plan the case for straight abutments, which will save you a minimum of 2.5 mm with any implant system on the market. It’s not always possible, but when I can, I routinely use straight abutments, especially in the anterior.

6. Use a soft-tissue implant in the posterior and eliminate the use of an abutment. Take the final bar straight to the implant. I frequently use this option when there is enough bone after the reduction and the anatomy allows the use of a vertically placed implant. I like using a wide-neck, wide-body implant in the first molar sites; the final bar will go straight to the implant connection. Additionally, the screws are big and beefy and are torqued to 35N/Cm. The A-P spread is very favorable, there is a huge surface area with these implants with higher bone-implant contact, and second molar occlusion is achievable. Posterior space is always at a premium with the arc of closure, and eliminating a posterior abutment will save at least 3.5 mm of space over an angled abutment.
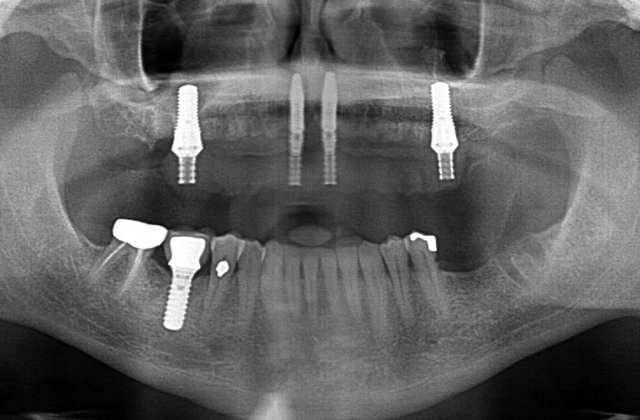
7. A metal intaglio surface instead of acrylic could save some height. Dr. Steve Parel has described this variant as the Dallas Bar, where the posterior portion of the bar is metal at the intaglio surface. We recently took this a step further in a medical compromised case with a severely autistic adult who had limited space with a very small maxillomandibular complex. She was extremely hard on her prosthesis and it kept breaking. Space requirements were not available despite our best efforts. Eventually, the prosthesis was remade where the posterior was all metal chrome, cobalt and titanium alloy, and the anterior was veneered with porcelain.
8. The last opportunity is not a significant option in most cases, but in some cases with thick fibrous tissue, we can thin the tissue and manipulate it with pressure from the prosthesis.
William Ralstin, D.D.S., Spear Contributing Author
William Runyon, D.D.S., Spear Contributing Author
SPEAR campus
Hands-On Learning in Spear Workshops
With enhanced safety and sterilization measures in place, the Spear Campus is now reopened for hands-on clinical CE workshops. As you consider a trip to Scottsdale, please visit our campus page for more details, including information on instructors, CE curricula and dates that will work for your schedule.

By: William Ralstin
Date: November 23, 2016
Featured Digest articles
Insights and advice from Spear Faculty and industry experts