Who Chooses the Implant Abutment: The Dentist or the Technician?
By Greggory Kinzer on April 25, 2016 | 1 comment
I discussed the treatment for this patient in an earlier post. The patient in Figure 1 didn’t like the metal showing on her implant crown and the dark color of the surrounding tissue.
(Click this link to read the article “Dark Tissue Around Implants?”)
The treatment plan was to re-do the implant restorations on #11 and #12. In addition to choosing a more esthetic custom abutment on #11, a facial connective tissue graft was planned to increase the thickness of the soft tissue. Knowing the patient’s chief concern upon initial presentation was the discoloration of the tissue, I wanted to make sure to choose something more esthetic than a metal abutment. When filling out the prescription, I decided to have the technician fabricate a custom zirconia abutment. However, was this the correct solution? Who should choose the implant abutment … the dentist or the technician?
(Click this link for articles on implant abutments.)
Typically, it is the dentist who chooses the implant abutment. The decision is obvious if the dentist is the technician or the dentist plans to make some sort of CAD/CAM hybrid abutment. However, even if the dentist is working with a technician, it’s generally the dentist who picks the abutment, as it is a box on the lab script that must be filled out when sending the case.
The difficulty of having the decision of abutment selection rest solely on the clinician is that quite often the clinician doesn’t know some of the decision parameters that must be considered. For instance: How does the angulation of the implant affect the potential thickness of the axial walls? How thick does the zirconia need to be to have adequate strength? Often, it is not until the technician has poured the model and either done a diagnostic wax-up or digitally designed the abutment/crown, that the proper implant abutment can be selected. (Figure 2)

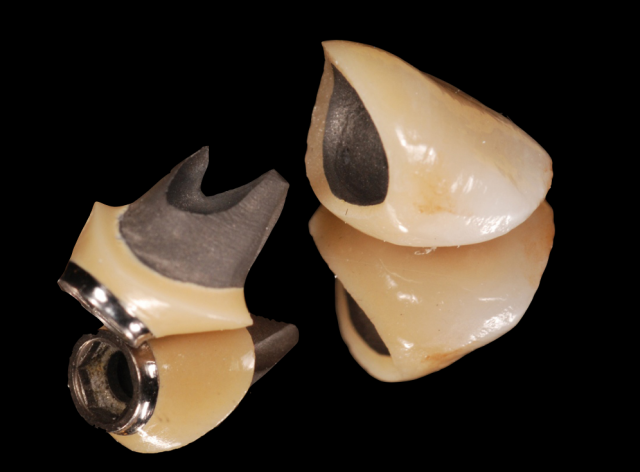
In this clinical example, I received a phone call from the technician telling me that if I truly wanted a custom zirconia abutment, structurally we may have some issues. The reason for this was that given the angulation of the implant, the axial walls on the distal and palatal of the abutment were going to end up extremely thin. (Figure 3)

Had the technician not passed along this crucial piece of information and instead just went ahead and followed the lab script, the patient would have ended up with a structurally weak abutment. In talking with the technician, we decided to use a custom metal abutment for strength but have ceramic baked on the sub-gingival cervical area so as not to negatively influence the esthetics of the tissue.
(Click this link for articles on dental esthetics.)
This abutment design is referred to as a Custom UCLA-metal ceramic abutment. (Figure 4 and 5) In my practice, this abutment design is one of the most common abutments that I use, as it can have the best of both worlds: strength and esthetics. Unfortunately, in this situation it meant the definitive restoration also had to be metal-ceramic (the restoration on #12 was designed as a screw-retained metal-ceramic crown). The final outcome is nearly indistinguishable from the natural teeth, resulting in a very happy patient. (Figure 6)


The take home message is that the decision on the definitive abutment should be a synergy between the dentist and technician. It is only through this “interdisciplinary” type of interaction that we can account for some of the nuances that arise in these types of situations. The responsibility of the dentist is to inform the technician of “what they need” and the technician can then propose “what options are available.”
(Click this link for more articles by Dr. Gregg Kinzer.)
Gregg Kinzer, D.D.S., M.S., Spear Faculty and Contributing Author
Comments
May 2nd, 2016