Have you heard this question from a patient? “Do I really need a dental implant? Are implants really necessary?”
The first patient of the day prefers to proceed with a three-unit fixed bridge to replace a missing tooth because it was a shorter treatment process that did not require surgery and it appeared to be partially covered by insurance.
The patient right before lunch comes in for a second opinion. (Click this link to learn more about working with second-opinion patients.) She is upset because she wasn’t given an option for a dental implant supported restoration – only learning about the possibility after the teeth adjacent to the space were prepared and covered with a three-unit fixed bridge. This patient is even willing to proceed with orthodontic treatment prior to having the dental implant placed with the understanding that it will all require a period of time for moving the teeth as well as for a healing period following the placement of a dental implant before the definitive restoration can be made and inserted. This patient has the idea that she would like to floss between the lower back teeth and that keeping individual teeth/restorations could limit the need for more extensive treatment in the future in the event that one tooth fractures or breaks down in some fashion.
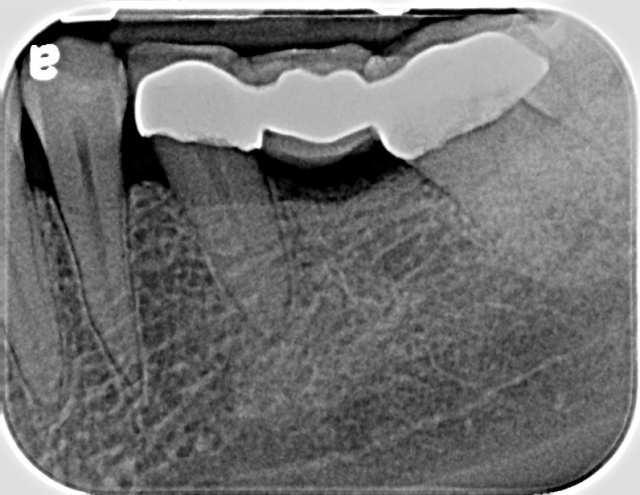

Wow! Definitely not an every day occurrence in my practice. As I write this article, this patient has already been evaluated by the orthodontist and the periodontist of our “team” in an effort to achieve the end-result she’s looking for. How many dentists with the knowledge and understanding would consider or even move forward on a path similar to what this patient is taking on – for #19, no less?
What about the discussion that takes place related to a structurally compromised tooth? The full coverage restoration was placed on an endodontically treated tooth and has been loose for several months. There is a significant amount of bone immediately surrounding the remaining tooth root. The remaining tooth structure is compromised as a result of dental decay. The free gingival margin is much more apical adjacent to this tooth than what is found with the other anterior teeth. The gingival tissues are visible during a spontaneous smile. The patient’s husband asks, “What would you do if you were attempting to get the perfect result?”



The rapid development of new techniques related to the placement and restoration of dental implants have provided options for our patients with one or more missing teeth. The advanced surface treatments applied to the dental implants and the restorative abutment along with the plethora of information and education opportunities available contribute to a general feeling that it may not be worth the effort involved in restoring a natural tooth.
Dental treatment involving dental implants is currently met with a wide variety of expectations from the restorative dentist. Systematic reviews (Lang & Muller 2007 and Tomasi, et. al. 2008) have concluded that natural teeth have a higher survival rate than dental implant-supported restorations. The relative favorability of natural teeth proved to be true even with structurally compromised teeth that were treated and maintained.
What are the guidelines, however, as to where treatment can be designed and planned for future tooth loss on one extreme? Or is it preferred to remove the remaining teeth and begin with an edentulous arch as an option on the other extreme?
It appears to make rational sense … in a situation where there is a missing tooth, a dental implant-supported restoration should at least be one of the options.
Dental implants were initially developed for “mal-adaptive” denture patients – the picture comes to mind of a patient with a flat lower residual ridge that is equal to or below the level of the floor of the mouth. Dhima, et. al. (2014), evaluated 190 patients with edentulous arches restored with dental implant supported prostheses placed between 1983 & 1991. They concluded that restorative treatment in areas of missing teeth should be planned and cared for as a “chronic condition” with the goal of providing “realistic care expectations” to our patients that may be working with dental implant-related restorations for many years to come.
Realistic care expectations means that the patient is willing to participate in and can afford the maintenance involved with an implant related restoration – certainly more important for an edentulous patient with a more extensive restoration.
The obstacles to treatment are not limited to economic means. A study by Walton, et. al., demonstrated that 36 percent of the patients interviewed for their study declined “free” dental implants for participating in their research. While there are people that simply do not wish to go through what might be considered an elective surgery, some of the people that declined the “free” dental implants explained that they were doing just fine with their complete dentures. Really?!
What are some of the factors you consider in your decision to either maintain or remove a tooth or even several teeth in favor of a dental implant related restoration? Share your thoughts in the Comments below or, if you’re a Spear member, start a conversation on Spear TALK.
(Click this link for more articles by Dr. Doug Benting.)
Douglas G. Benting, DDS, MS, FACP, Spear Visiting Faculty and Contributing Author - www.drbenting.com
References
Lang, NP, Muller, F. Epidemiology and oral function associated with tooth loss and prosthetic dental restorations. Consensus report of Working Group 1. Clinical Oral Implants Research. 2007;18:46–49.
Tomasi, C, Wennstrom, JL, Berglundh, T. Longevity of teeth and implants – a systematic review. J Oral Rehabil Journal of Oral Rehabilitation. 2008;35(s1):23–32.
Dhima, M, Paulusova, V, Lohse, C, Salinas, TJ, Carr, AB. Practice-Based Evidence from 29-Year Outcome Analysis of Management of the Edentulous Jaw Using Osseointegrated Dental Implants. Journal of Prosthodontics on Dental Implants. 2015:121–130.
Walton, J, Macentee, M. Choosing or refusing oral implants: A prospective study of edentulous volunteers for a clinical trial. The Journal of Prosthetic Dentistry. 2006;96(5):353.