These 4 Questions Can Save Your Patient’s Life
One of the single best classes I have taken at Spear Education is a dental sleep medicine course. I learned a great deal about obstructive sleep apnea and its serious health consequences. It wasn’t just about the snoring but also included airway and tooth-wear issues and, most importantly, it gave me the tools to evaluate sleep apnea in my existing practice. Once I knew what to look for, I could have the appropriate conversations, and many of my patients have since been diagnosed with OSA. (I think we’re at 11.)
What alarms me is that if I hadn’t known this, many of these patients — who have been in the practice for years — would never have been diagnosed or diagnosed after having developed other medical issues.

One of the tools I use is the STOP-Bang Sleep Apnea Questionnaire, originally developed by a group of anesthesiologists and published in 2008 as a screening guide for surgical patients. The STOP-Bang questionnaire was developed to be concise and easy to use, and their research using this showed it was an excellent screening tool with a high degree of sensitivity.1
I like that it consists of eight simple questions, only four of which the patient has to directly answer. It can be printed out and given to a patient at the time they update their medical history form or be part of the questions I ask during the periodic exam. My hygienist is now trained to ask these questions when conducting her medical update. It shows a patient yet another level of thoroughness in evaluating their health.
I want to emphasize that this information should become part of your patient record, every bit as important as their medical and dental history.
If a patient answers “yes” to all of the STOP portion of the questionnaire and is obviously overweight, I may not actually figure out the BMI. However, measuring the BMI is easy to do. To calculate the BMI, divide the patient’s weight in kilograms by his height in meters, then divide that answer by his height again.
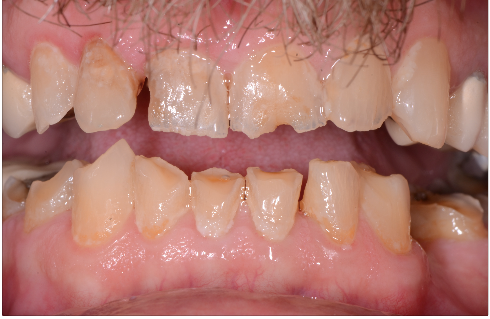
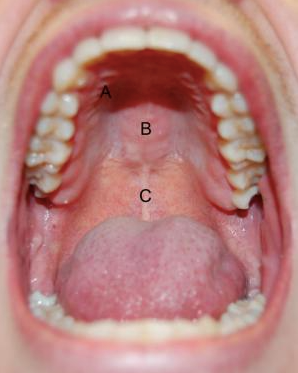
When I examine their dentition and observe anterior tooth wear, or a large tongue with scalloped border or a long drape of the pharynx, it sends up red flags that this patient may have a problem. The conversation shifts from teeth, which is what they’re concerned about, to the STOP-Bang score and all the other concomitant oral findings.
I clearly tell the patient that I can’t make the diagnosis but I recommend she contact her MD and set up a home sleep study as soon as possible. I suggest she specifically tell her MD that she wakes up tired and her sleep partner tells her that there is a cessation in breathing. My thought is that saying those two things should impress the physician to further investigate. Although I recognize there are many physicians who will not consider the relevance and importance of my dental/oral findings and recommendations, I have not encountered any resistance thus far, thankfully.
I believe my patients are most comfortable starting what can be the frightening process of the diagnosis with their own physician. There are sleep disorder centers with physicians who solely treat this, but I prefer to have my patients’ personal physicians make the referral. There isn’t a standard of care for this, but many dentists who evaluate sleep disorders recommend referring the patient directly to a sleep physician and bypass the primary care MD. Alternatively, if you know a sleep medicine physician in your community, establish a relationship with them so you’ll be comfortable referring your patient directly to the expert.
It can be difficult for patients to access the best level of care, but it’s extremely important to discuss the advantages of doing so. Most physicians will default to the CPAP machine for treatment because it’s considered the gold standard; however, this is what frightens patients most. If they have mild or moderate OSA, I let them know there are alternatives that involve a dental sleep appliance.
The STOP-Bang questionnaire provides a template for screening and a foundation to having a conversation. It is now part of the protocol for all of my new and existing patients. And I know it has saved some lives.
Reference
- Chung F, Yegneswaran B, Liao P, et al. STOP Questionnaire. Anesthesiology. 2008;1 08(5):812–821.
SPEAR ONLINE
Team Training to Empower Every Role
Spear Online encourages team alignment with role-specific CE video lessons and other resources that enable office managers, assistants and everyone in your practice to understand how they contribute to better patient care.

By: Mary Anne Salcetti
Date: February 17, 2016
Featured Digest articles
Insights and advice from Spear Faculty and industry experts


