Creating a Radiographic Template for Implant Planning Step-by-Step
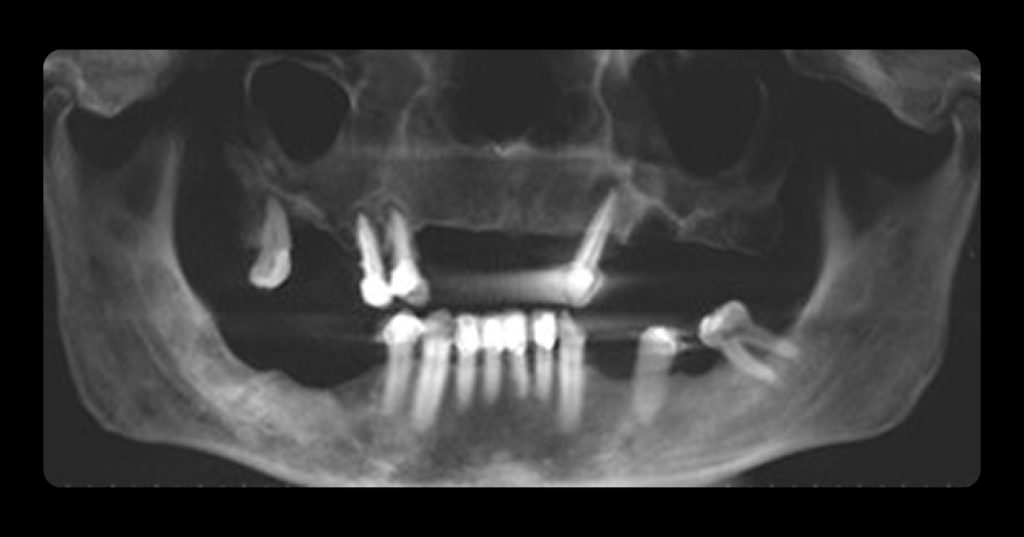
Implant planning has become more sophisticated in recent years, and the easy availability for most dentists to utilize CBCT makes the process easier.
As a restorative dentist, my job is to determine where the tops of the teeth should be positioned to create the most esthetic and functional outcome for the patient. Then I need to figure out how to support that tooth position.
If the support comes in the form of an implant, the next job is to help my surgeon understand the optimal implant position in order to create the best restorative outcome. The surgeon’s job is to tell me if that is possible and what needs to be done to get there.
The best information for both the restorative doctor and the surgeon comes from a radiographic template that transfers the desired tooth position to the mouth in a form that can be included in a CBCT. There are many ways to create a radiographic template and, regardless of which you choose, it should satisfy these basic requirements:
- It should accurately replicate the desired final tooth position.
- The template should be radiolucent except for the teeth that will be restored with implant restorations.
- It must be stable and immoveable during the process of exposing the CBCT.
- It should have a channel through the radiopaque teeth that represents where the restorative dentist would like to have the screw head of the abutment exit the occlusal or incisal of the implant.
Radiographic templates are not surgical guides, they are a means to determine if the desired implant position is possible in a given situation and, if not, can help the surgeon make decisions on how to augment a surgical site. However, sometimes a radiographic template can be converted to a surgical guide if the desired implant position that is represented by the guide does not change after seeing the scan.
These templates can be easily and inexpensively fabricated in your office if you have a vacuform machine or a mini-star.
Steps in Creating a Radiographic Template
1. Start with a set of articulated diagnostic casts to determine if there is adequate restorative space.
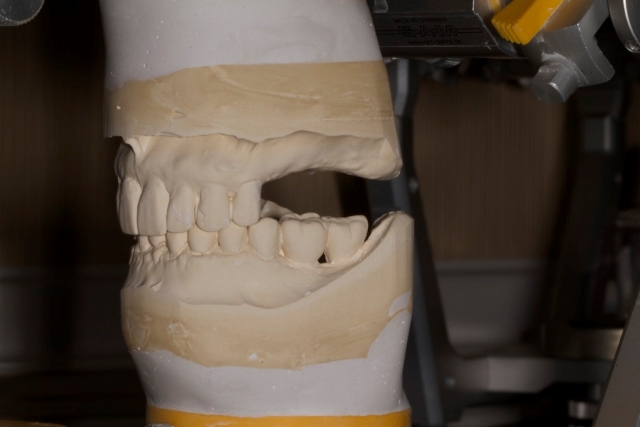
2. Complete a diagnostic wax-up or place denture teeth of an appropriate size in the restorative space. Use weather-stripping compound or autopolymerizing epoxy to hold the denture teeth in place or make a model of the wax mock up.
(Click here for more information on creating diagnostic wax-ups.)
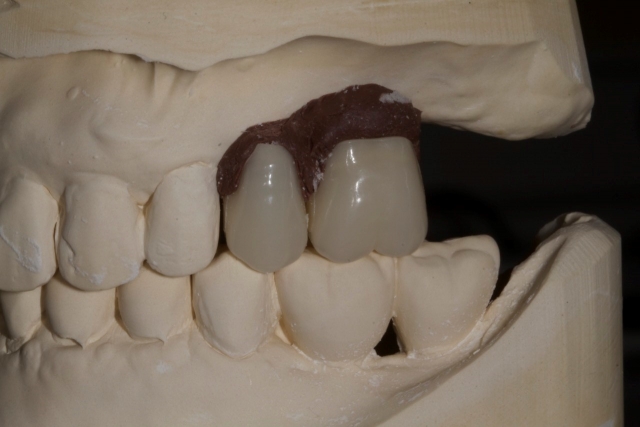
3. Using 1.5 mm clear splint material, do a vacuform over the denture teeth or model of the wax-up.
4. The appliance should then be trimmed so that the desired gingival levels of the final restorations are intact. The remaining teeth should be trimmed back so that 1-2 mm of overlapping acrylic remains to stabilize the template. This is an important landmark for the surgeon.
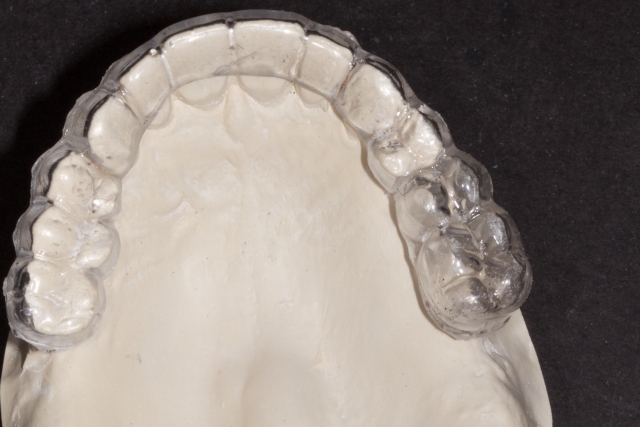
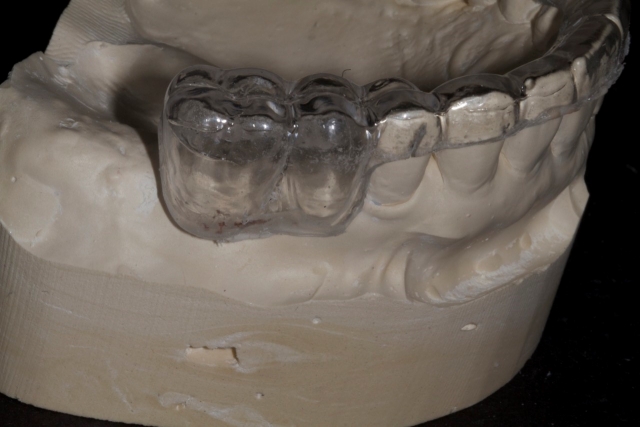
5. Using a radiopaque self-curing methylmethacrylate mixed to a putty consistency, fill the space left by the denture teeth or wax-up.
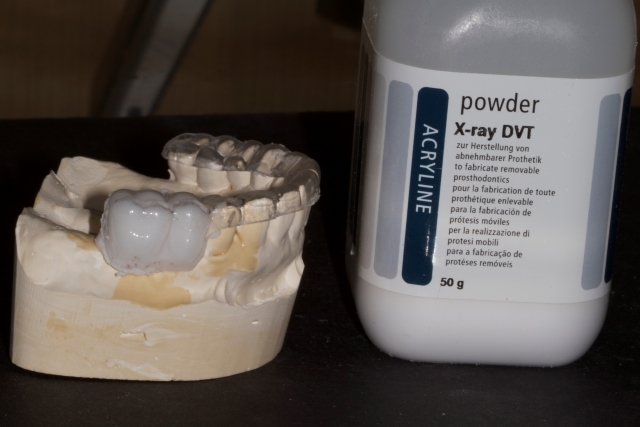
6. Trim the excess acylic back to the gingival margins.
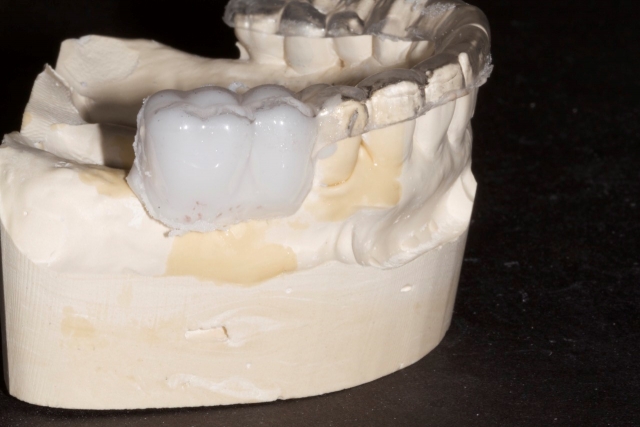
7. Spot the desired exit point of the implant platform on occlusal surface of the teeth.
8. Using a 2 mm twist drill or disposable implant drill cut a hole through the acrylic until the drill touches the stone model.
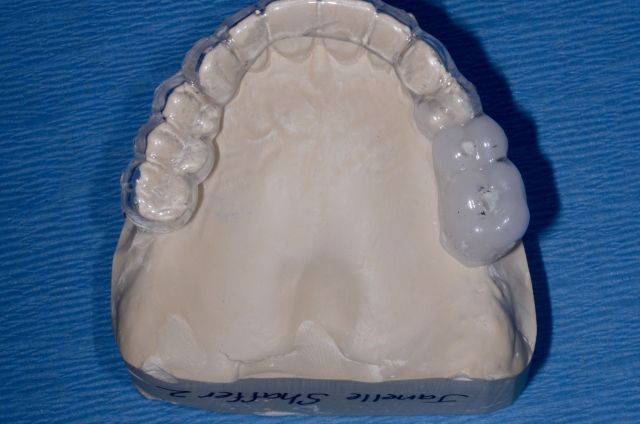
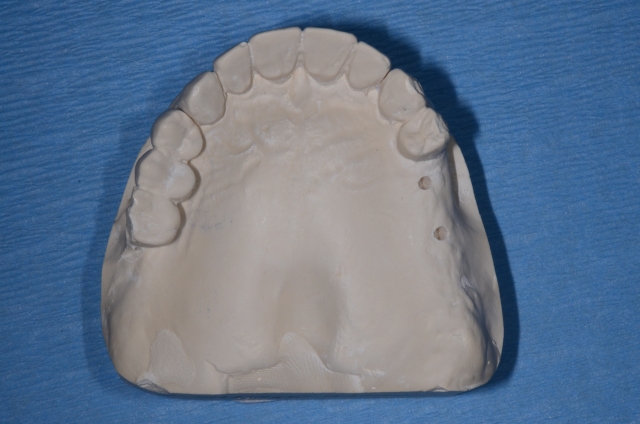
9. Clean up the edges using an acrylic finishing bur.
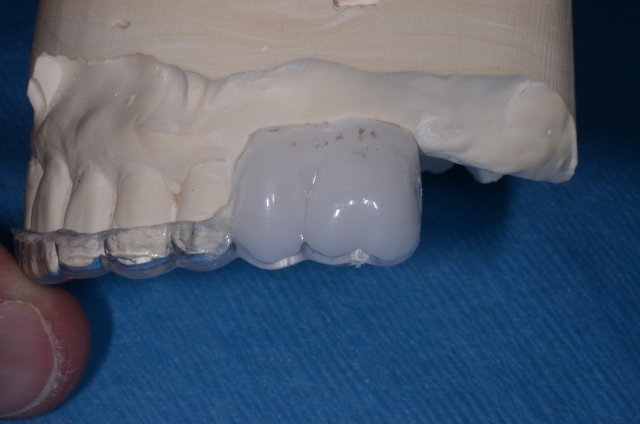
10. When tried in, the template should be solid and stable and have a “snap-fit.”
The patient can be instructed in how to insert the appliance and can take it with them if they are having the CBCT done outside of your office. The end result will give you and the surgeon a more clear understanding of potential implant positions. The hole that is drilled through the teeth will be radiolucent on the CBCT and serve as an indicator of possible implant angulation that can be corrected by the surgeon as the case is planned.
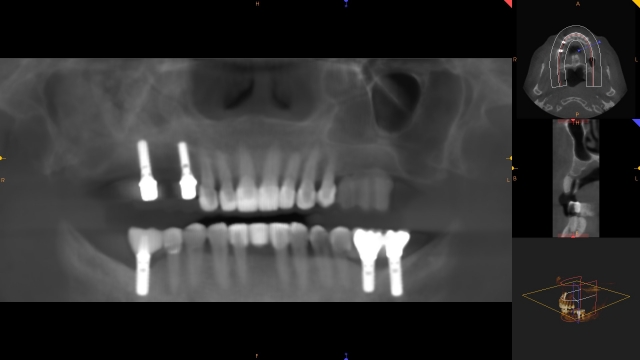
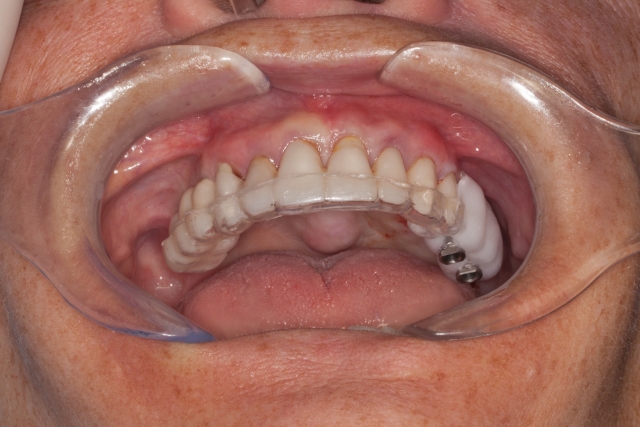
If the CBCT exam shows that the proposed position is acceptable and that no grafting is needed, this radiographic guide can be converted to a surgical guide by simply inserting metal sleeves that are the appropriate diameter to the drills the surgeon prefers.
VIRTUAL SEMINARS
Stay Sharp. Stay Current. Stay Ahead.
Join live, focused training designed to help you implement immediately and strengthen your expertise.

By: Steve Ratcliff
Date: January 25, 2016
Featured Digest articles
Insights and advice from Spear Faculty and industry experts