To Floss or Not To Floss: Why Is That a Question?
In more than 40 years of treating patients experiencing periodontitis, I’ve often been asked why effective flossing two to three times a day is a core principle in my strategy for their success.
Well-intentioned dental professionals and patients alike ask if another, more “patient-friendly” approach would be as or more effective at removing biofilm from proximal surfaces of teeth. Various products that hold a span of floss on some sort of handle, various designs of interproximal brushes, and the “safe” use of toothpick-like devices are often suggested as preferred alternatives to manually using dental floss. My preference for unwaxed floss — ideally very thin and not braided — seems to some to be ridiculously difficult and frustrating to use while being an unreasonable chore to ask patients to perform.
In this article, I will offer the reasons I believe my patients have been remarkably successful in accomplishing a therapeutic level of home care, substantially moderating the need for periodontal surgery and sustaining periodontal stability after effective nonsurgical and surgical interventions provided by me and my team. I’m fully aware of dental literature that suggests flossing is not as effective as interproximal brushing, I am keenly aware of proximal surfaces of teeth and roots exposed by bone loss presenting varying degrees of concavity, and I do not believe patients are unwilling or unable to master difficult skills when they expect and experience improved oral health.
A meta-analysis of flossing versus interproximal brushing began with the stated condition there had to be “room” for the proximal brush. Many patients have asked me why their gingival papilla no longer fill the interproximal gingival embrasure, because they’re frustrated with the appearance and frequent food collection. When those individuals present with only minimal to moderate periodontitis, I ask what they use to clean between their teeth. Almost invariably, they use an interproximal brush or something resembling a toothpick. Compression of the gingival papilla appears to be necessary and can be carried to the extreme by patients attempting to be conscientious.
As the incidence of food collection occurs more often, patients seem to use those instruments more frequently and more vigorously, often compounding the issues that concern them. If they have some degree of periodontitis, the level of inflammation and disease activity usually is relatively unchecked on the lingual surface of their teeth, because most believe approaching their teeth from the facial is fully adequate.
Unless forcibly jammed subgingivally, none of the interproximal aids reach more than approximately 1 mm of the subgingival surface of the proximal surface of the tooth. Proximal sulcus depths are typically 2–3 mm deep in health and at least somewhat deeper in many sites of periodontitis, so how can these instruments disrupt and remove adherent biofilm from the remainder of the intrasulcular proximal surface of a tooth beyond 1 mm? How effective can they really be?
I am also quizzed about why waxed or Teflon-like floss is not equivalent to unwaxed. I offer the example of spilled cooking oil on a kitchen countertop: Would one reach for waxed paper or a paper towel to clean it up? Bacterial biofilms are much like cooking oil in consistency and their ability to adhere to a surface of a tooth. Why would I give my patients something to do that can be partially efficient at best?
Skillful, careful flossing while wrapping the floss around to the lingual and facial of the tooth, forming a deep C or U shape when viewed from the occlusal, is both safe and the most effective means of removing biofilm. The floss can reach 2–4 mm subgingivally because the wrapping allows it to miss the gingival papilla entirely and barely touch the gingival margins on the facial and lingual aspects of teeth. Close proximity of the fingers directing the floss vertically scrubs apicocoronally, avoiding the papilla and possible cutting of marginal gingiva. Moving along a long piece of floss so as to never reuse a segment again minimizes fraying and frustration while increasing effectiveness and addressing any concern about moving pathogens from one tooth to the next. This is a difficult skill to master and there don’t seem to be many “naturals” out there, so coaching with patience and encouragement is a requirement for the patient’s success.
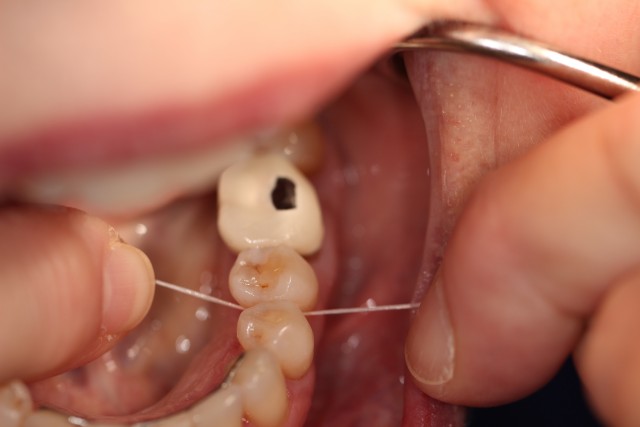
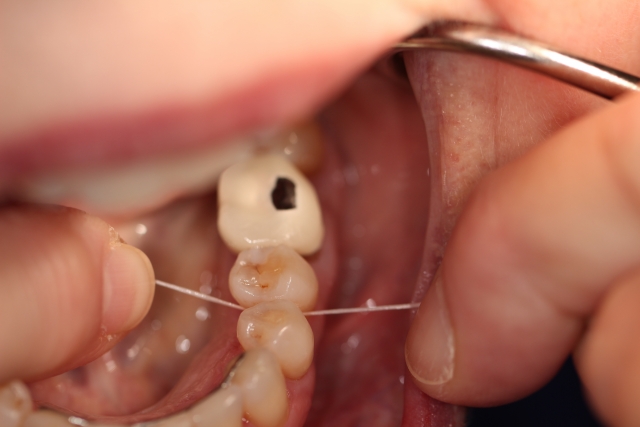
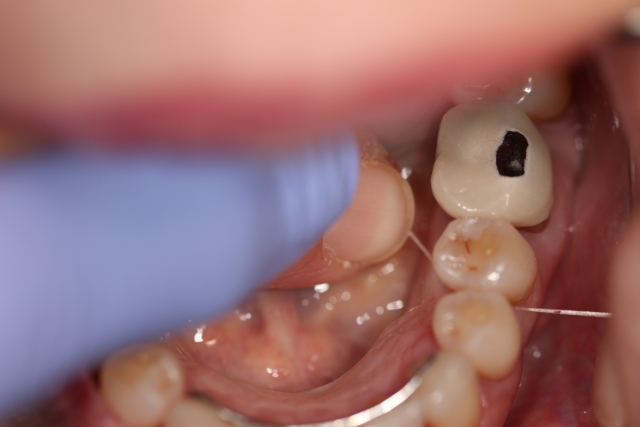
Figs. 1–3 depict the essential elements of our patient’s success. Fig. 1 is what we often observe when we ask patients to show us how they have flossed that day. Thoughtfully and carefully developed language that prefaces this requested demonstration avoids a critical or judgmental assessment. Fig. 2 shows my dental assistant’s gentle guidance of the patient’s fingers so they learn that wrapping the floss effectively removes the biofilm (the tooth becomes squeaky clean) while avoiding any trauma to the gingiva. Fig. 3 illustrates that the patient has learned this skill through coaching in an atmosphere of encouragement.
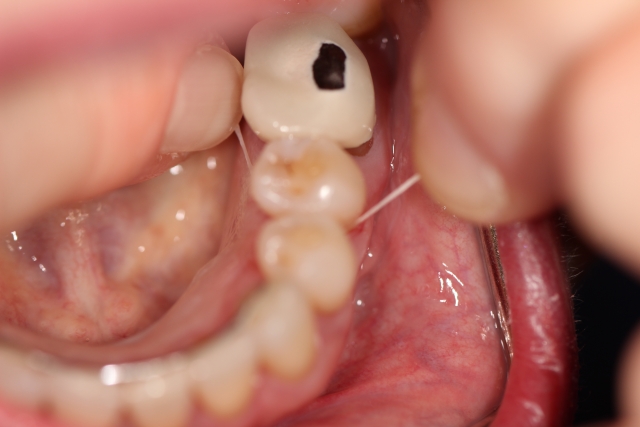
Of course, for patients who are physically unable to do this, substitute strategies are needed and used. Proximal brushing in open gingival embrasures is frequently helpful for patients with a history of proximal bone loss, but they complement that technique with the more therapeutic effect of flossing.
I hope you will give my findings a fair and open consideration in spite of the prevailing trend to discount flossing as a viable therapy that our patients really can and really will accomplish with nearly predictable success. If you do, expect to celebrate their success with them.
FOUNDATIONS MEMBERSHIP
New Dentist?
This Program Is Just for You!
Spear’s Foundations membership is specifically for dentists in their first 0–5 years of practice. For less than you charge for one crown, get a full year of training that applies to your daily work, including guidance from trusted faculty and support from a community of peers — all for only $599 a year.

By: Michael McDevitt
Date: June 12, 2015
Featured Digest articles
Insights and advice from Spear Faculty and industry experts