The Infamous Mandibular Block
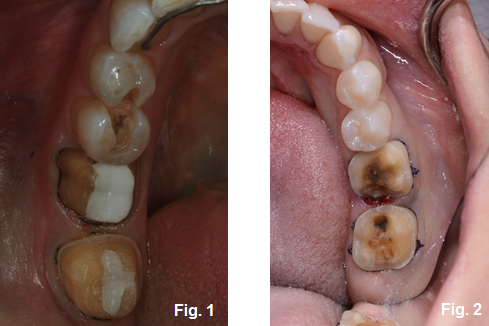
At a recent Facially Generated Treatment Planning workshop, I was having lunch with a group of dentists with a wide range of experience and age–from one year out of school to 20 years of practice. Frustration with the lack of predictable mandibular blocks stimulated a great conversation with a lot of energy. We have all experienced the complication and embarrassment of attempting to finish a crown preparation (Fig. 1), remove deep decay (Fig. 2), or access a pulp chamber with less than profound anesthesia on a lower molar due to a mandibular block.
The participants (and I) were wondering if they were missing something – besides the nerve that they assumed they were missing – that could help them. Was there something that could prevent a mandibular block? Are there supplemental injections besides the long buccal, mylohyoid, intraosseous, PDL, etc.?
The Infamous Mandibular Block… You Are Not Alone
Having recently transitioned from private practice with similar experiences and subsequently seeing the frustrations of dental students and faculty almost every day, while working with brilliant people who teach anatomy and injection techniques, I thought it might be a good idea to take a fresh look at the current literature regarding the infamous mandibular block. The review sadly revealed that even in 2014, they are not alone with this dilemma that has hindered our profession for so long, and neither are you.
Misery loves company, right?
We talked about so many reasons that could lead to the variability of results, including the use of Articaine. There is still some hesitation to use Articaine due to years of reports of increased parasthesia with mandibular blocks. Even though it has been shown that the efficacy is statistically better than Lidocaine in several studies, we avoid using it knowing it could predictably help one of our biggest stressors of mandibular dental work.
More and more, however, we start to see that our fears are unwarranted. One fairly recent article documented a well-done meta-analysis demonstrating that, “Articaine is more likely than Lidocaine to achieve an anesthetic success in the posterior first molar area…” and that there is, “no difference in post-injection adverse events or post-injection pain.” 1
In no way do I think that any one article should shape our decision to use Articaine or any other local anesthetic or offer great hope for predictable outcomes for mandibular blocks. However, after a fairly extensive review, I do think that there is sufficient evidence, understanding and there are certain techniques to present to each patient with a variety of options or tools in our tool-belt to dramatically increase our odds, decrease stress and know that we are doing the best we can. It also helps to know that we are not alone or missing something.
I will be sharing those articles and findings with you in a subsequent Spear Monthly Digest article. For now, you might just try trusting the research and a new carpule in your syringe before your next mandibular molar procedure.
References
J Dent. 2010 Apr;38(4):307-17. doi: 10.1016/j.jdent.2009.12.003. Epub 2009 Dec 16.The efficacy and safety of articaine versus lignocaine in dental treatments: a meta-analysis. Katyal V.
SPEAR campus
Hands-On Learning in Spear Workshops
With enhanced safety and sterilization measures in place, the Spear Campus is now reopened for hands-on clinical CE workshops. As you consider a trip to Scottsdale, please visit our campus page for more details, including information on instructors, CE curricula and dates that will work for your schedule.

By: Kevin Kwiecien
Date: October 22, 2014
Featured Digest articles
Insights and advice from Spear Faculty and industry experts


