Records Necessary for Delivery of an Immediate Fixed Hybrid Case
The immediate fixed hybrid treatment plan was accepted. Now what?
Once the patient has accepted the treatment plan of an immediate fixed hybrid, the next question is almost always, “What do we do next?” As the restorative doctor on the case, the answer to that question is to begin taking records. These pre-operative records are the actual building blocks for the immediate fixed hybrid case. The appointment allows you to collect data that will help determine the vertical dimension of occlusion (VDO) and the overall bone reduction requirements needed to deliver a beautiful prosthesis. This data will be necessary for your laboratory partner and the surgeon as well.
The steps to preparation and data collection are not difficult. While the components of pre-op records are familiar, you just may not collect them on a daily basis. The three primary components are:
- 35 mm photos,
- Facebow-assisted, mounted diagnostic casts
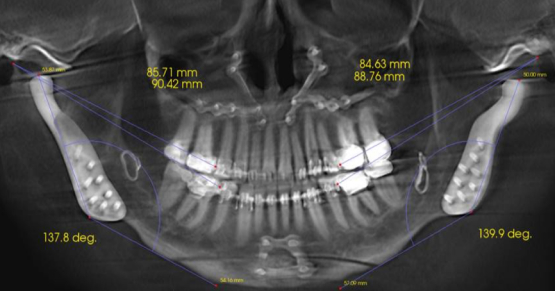
- Panograph/cone beam commuted tomography (CBCT)
Taking Photos for Fixed Hybrid Treatment Planning
If you routinely take 35 mm photos of new patients, they are likely the reason you are moving forward with this treatment plan for your patient. In my experience, nothing has been more effective in promoting treatment plan acceptance than 35 mm photos. The six photos we take are the following:
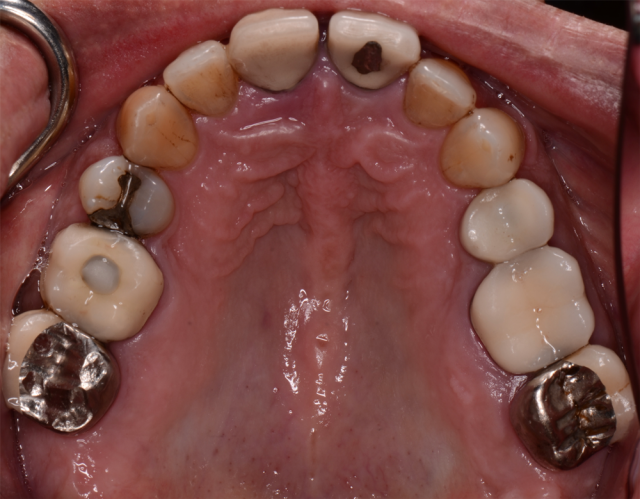
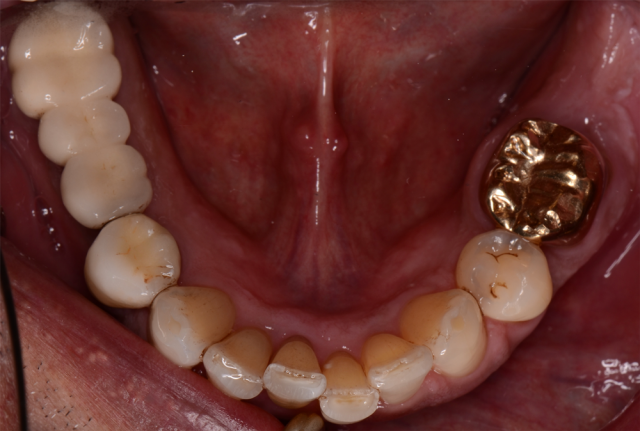
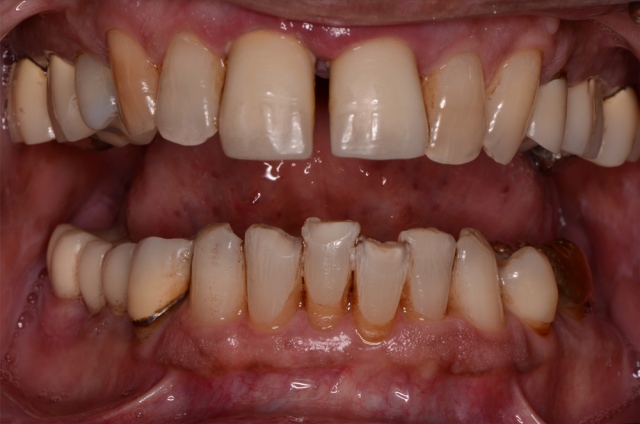
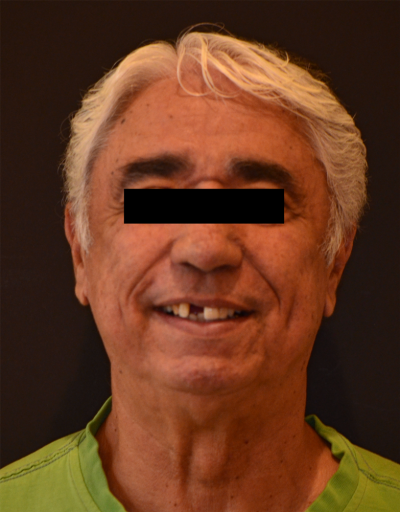
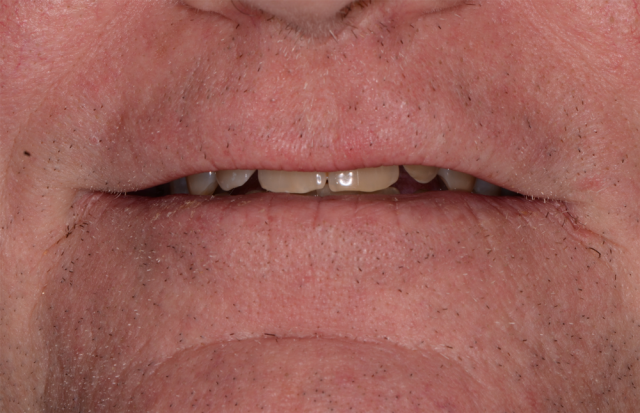
The last two photos are the ones we will discuss first. The close-up “lips-at-rest” and the close-up “smile” are specifically used for planning the overall esthetics and functional aspects for the immediate fixed hybrid build. The foundation of design is the same concept taught at Spear Education’s “Facially Generated Treatment Planning” workshop.
Evaluating Position
First evaluate the position of the maxillary central incisors. This is of vital importance not only for the esthetic design of this restoration, but the functional and structural requirements of components in the immediate fixed hybrid prosthesis as well. The structural requirement to which I am referring is the minimum inter-arch space required to build and maintain the prosthesis. The calculation and design of this aspect of the fixed hybrid is done with specific intent.
The space required for an acrylic-based restoration is different than the space required for a zirconia fixed hybrid restoration. For the sake of discussion in this article, an acrylic denture material wrapped around a milled bar will be the final restoration. The thickness of the final prosthesis is not determined by accident.
We do take into consideration the size and functional history of the patient. For example, a small female patient that exhibits little wear on her natural dentition will be fine with a 13 mm prosthesis, while a large male patient with well defined masseters and a badly worn dentition would require we build 15 or 16 mm inter-arch space into his fixed hybrid. So if we are planning an upper and lower case on small male or female with no history of bruxism, the overall inter-arch space required will be 26 mm total: 13 mm maxillary and 13 mm mandibular. That is a minimum space requirement.
Using Diagnostic Models in Fixed Hybrid Treatment Planning
So, how do we insure this measurement is incorporated into the design? The 35 mm photos and diagnostic models are ultimately what will insure that both the esthetic design and structural requirements are met.
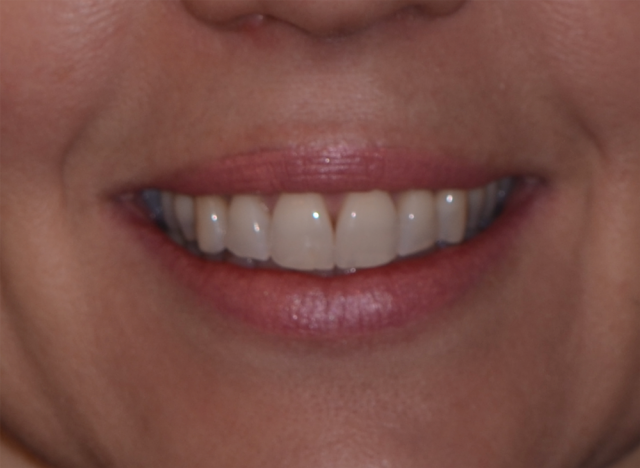
Let’s look at two possible scenarios. The first will involve a patient that is set up nicely with teeth 8 and 9 in the correct and desired position. When the maxillary centrals are in the right place, they look good in the “full smile” close-up (Figure 6) and in the “lips at rest” photos (Figure 5). We use the incisal edge position as a landmark for determining the incisal component of the 13 mm space requirement. We would now go to our diagnostic casts and measure apically from the incisal edge up 13 mm and mark this point on the maxillary cast. This is the minimum amount of space required for the prosthesis. Both the laboratory technician and the surgeon will rely on this measurement for specific aspects of their work in delivering the immediate fixed hybrid. Specifically, a reduction guide will be made using this physical landmark as a point of reference.
The second scenario occurs when the central incisors are not in the proper position esthetically. If, for example, there has been a great deal of attrition/abrasion of the tooth structure, or the teeth have possibly super-erupted, it will be important to determine the proper location prior to case planning/laboratory work. In these instances, you must determine the proper position and indicate that position for your lab technician and surgeon. This may involve waxing missing tooth structure back to the existing edge position on the cast and/or reducing the cast to compensate for teeth in the improper position. The photos and diagnostic casts you have acquired are both used in this planning process.
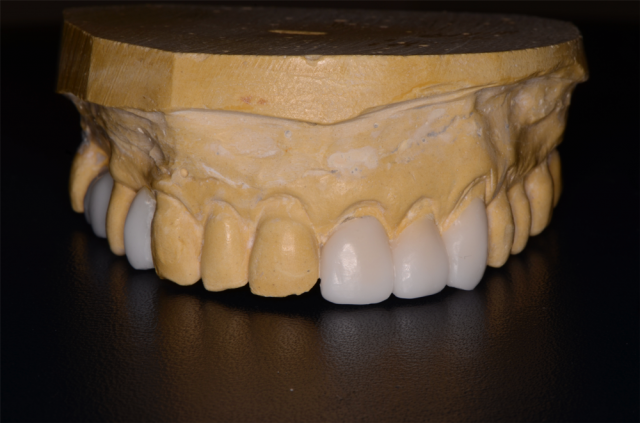
Additionally, the diagnostic casts are used for the actual manufacture of the full denture that will be fabricated prior to surgery. It is extremely important that these casts are of high quality and complete in the peripheral broader anatomy.
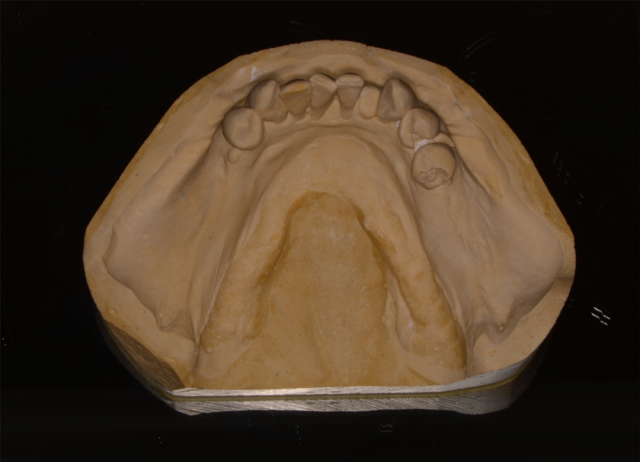
Careful attention to leaving peripheral anatomy intact will prove instrumental in a functional denture fabrication. We must mention here, it is never by design that a patient wears a full denture home after extractions and implant placement. It is, however, a condition for which we need to be ready if the implants do not have primary stability at the time of placement. This primary stability aspect will be further discussed in other articles but is crucial to immediate placement of the provisional prosthesis. Primary stability is a torque value observed and determined by your surgeon when he places each implant.
The diagnostic cast will be important in later steps of fabrication. A facebow mounting is important for initiating and designing the occlusion of your case. The mounted models will be used again at the wax try-in and fabrication of the final prosthesis.
CBCT Scans in Fixed Hybrid Treatment Planning
The final piece of pre-surgical data we want to collect is a CBCT scan. This technology is becoming the standard of care for diagnostic planning in implant surgery. My surgeon has a CBCT and acquires an image during the consultation phase. It is a diagnostic piece we use together when planning our cases.
Like any procedure, the collection of appropriate clinical data is necessary to deliver the immediate fixed hybrid. The critical data described will insure success. Thoughtful attention to restorative principles like proper vertical dimension of occlusion and adequate bone reduction will be required for this successful outcome. The data we collect for the fixed hybrid restoration is really very much like the data required for a full denture. The restoration differs for many of us in that it requires a team approach: surgeons, laboratories and restorative dentists all pooling their unique talents and skill sets to deliver a full-mouth rehabilitation. As the restorative doctor on the case, it is my responsibility to build the data for the team.
Good 35 mm photography, mounted diagnostic casts and the proper radiographic evidence will allow your team to successfully deliver this prosthetic full-mouth rehabilitation.
SPEAR campus
Hands-On Learning in Spear Workshops
With enhanced safety and sterilization measures in place, the Spear Campus is now reopened for hands-on clinical CE workshops. As you consider a trip to Scottsdale, please visit our campus page for more details, including information on instructors, CE curricula and dates that will work for your schedule.

By: William Ralstin
Date: December 30, 2016
Featured Digest articles
Insights and advice from Spear Faculty and industry experts