The Challenge of Replacing Missing Central and Lateral Incisors
Replacing a single missing central or lateral incisor is quite predictable, especially if there is adequate bone and soft tissue to utilize a single tooth implant. Replacing adjacent missing central and lateral incisors is much more difficult, especially if an ideal esthetic result is desired.
Why is replacing the adjacent missing central and lateral more difficult? Gingival esthetics is a major factor. Achieving an excellent papilla between the adjacent missing teeth when using implants or a fixed partial denture (FPD) is not easy. In addition, achieving ideal gingival margin levels may be a problem as well, depending upon the amount of bone loss that occurred when the teeth were lost.
When teeth are present, we know the soft tissue behaves predictably in its relationship to the underlying bone – typically 3mm above the bone on the facial, and 4.5 to 5mm above bone on the interproximal. While variations from the above numbers exist, the majority of patients will have these normal relationships.
What establishes these average numbers is the biologic attachment of the gingiva to the tooth – the so-called biologic width. This is made up of the connective tissue and epithelial attachments, each averaging 1mm in height for a combined attachment height averaging 2mm. Coronal to this lives additional unattached soft tissue which creates the sulcus, averaging 1mm on the facial and 3mm on the interproximal. (1)
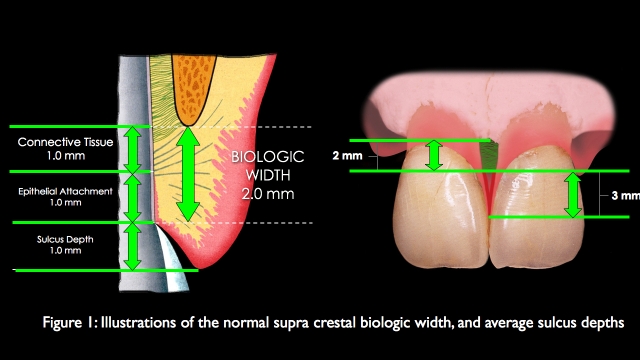
Biologic Width and Natural Teeth
The important point to remember about natural teeth is that the attachment is supra crestal; the biologic width starts at crestal bone and extends coronally, acting as a scaffold to support the overlying soft tissue. When adjacent teeth are lost, this supra crestal scaffold between the teeth is lost, resulting in a subsequent loss of papillary height. The supra crestal attachment is still present on the teeth adjacent to the teeth that were lost. This is what makes maintaining a papilla predictable when a single tooth is lost, the adjacent teeth still have a supra crestal attachment and will still produce a papilla height 4.5 to 5mm above the bone when a single tooth implant is placed next to the natural tooth. (2)
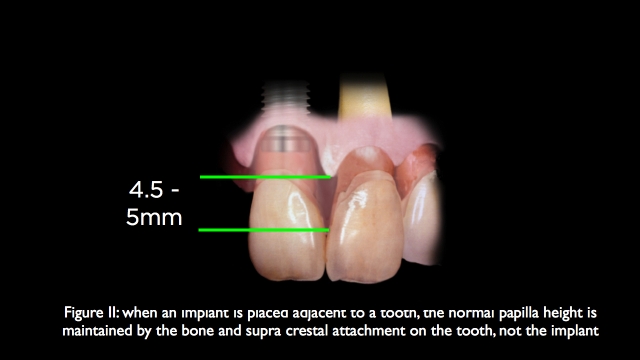
The behavior of the papilla next to the remaining teeth is not always predictable when we use pontics, even though the adjacent abutment teeth still have a supra crestal attachment, the papilla are not always maintained unless the embrasure form of the extracted tooth is maintained in the form of an ovate pontic the day of extraction. (3)
The biggest challenge when replacing an adjacent missing central and lateral is the loss of attachment height between adjacent implants, or adjacent pontics. This loss of attachment results in a papilla that is more apical in its relationship to the underlying bone. Research states that the typical papilla between adjacent implants will be 2 to 3.5mm above the underlying bone as compared to the 4.5 to 5mm it was between the natural teeth. (4)
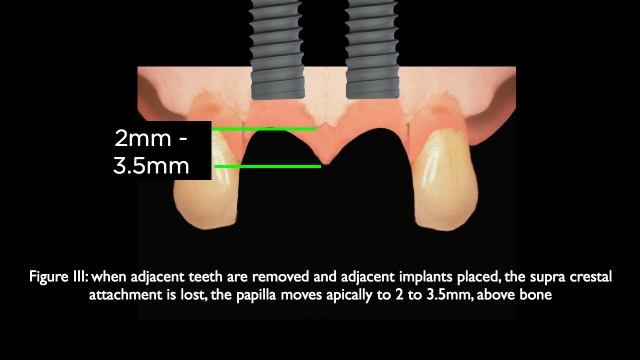
Even though the papilla between a pontic and abutment tooth aren’t always predictable, the papilla height between adjacent pontics can be excellent if the ridge is augmented with connective tissue, research showing the possibility of building the tissue 6 to 9mm above the underlying bone. (5) This allows ovate pontics to be created that can have an excellent interproximal papilla, but this is rarely the case unless the augmentation is done. And even the augmentation doesn’t guarantee an excellent papilla.
The one thing that is similar between single tooth replacement and the adjacent missing central and lateral is the concern over facial gingival margin levels. Anytime a tooth is lost there is always some loss of facial bone and this bone loss can result in recession. (6) This means that to get an acceptable gingival margin level it is common to perform augmentation for replacement of a missing single tooth, or adjacent teeth, this augmentation may be bone and/or soft tissue for implants or FPDs.
So where does the attachment go following tooth removal and implant placement?
Research has shown that the biologic width recreates itself on the implant, but on the majority of implants it is recreated by resorbing bone to expose the head of the implant, and a new connective tissue and epithelial attachment is formed, but it is now sub crestal, apical to the osseous crest.
This same bone die back occurs on the implant surface adjacent to the remaining natural tooth, and again a sub crestal attachment is created, but since the tooth still has a supra crestal attachment, the papilla height is maintained as long as the die back doesn’t affect the bone level on the tooth.
There are implant systems that attempt to minimize the die back of bone, most utilize some form of platform switching, where the abutment connection to the implant is smaller then the diameter of the implant. This exposes a portion of the head of the implant for the biologic width to attach to, minimizing the die back of bone.(7) Unfortunately this attachment is more lateral in direction rather then coronal, so the papilla height is not altered as significantly as it could be if there was a supra crestal attachment formed in a coronal direction.
Understanding biology becomes critical when considering placement of adjacent implants in the central and lateral site. We know that the papilla was 4.5 to 5mm coronal to the interproximal bone when the teeth were present, and that when adjacent implants are placed the papilla will be 2 to 3.5mm above the bone, meaning a loss of 1.5mm to 2.5mm of papilla height on average. But that is true only if the height of the interproximal bone is retained. If there is interproximal bone loss, the papilla level will move even more apically.
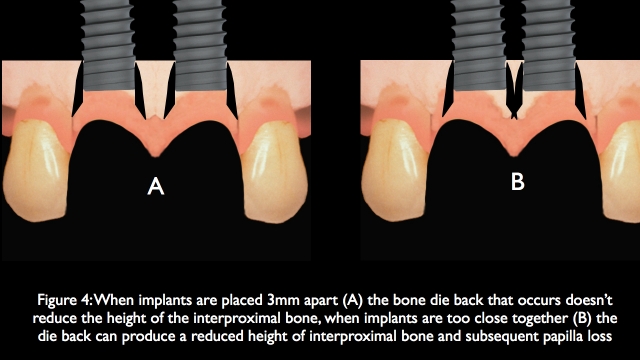
This is where the challenge of the adjacent missing central and lateral becomes an issue. Following anterior tooth loss, if adjacent implants are placed 3mm or more away from each other, the interproximal bone is typically retained. (8) Achieving the 3mm inter-implant distance is fairly easy when replacing adjacent central incisors due to the size of the teeth being lost, compared to the diameter of the implants. It is more difficult to achieve this distance when replacing an adjacent missing central and lateral.
This bone die back occurs when the implants are 3mm apart as well, but because of the inter-implant distance the funnel shaped bone loss doesn’t overlap between the implants, leaving the height of the interproximal bone unaffected. It is not uncommon when replacing an adjacent central and lateral, that the inter-implant distance may be as small as 1.5 to 2mm. Now when bone die back occurs, the funnels of resorption can overlap resulting in a loss of interproximal bone height. As the bone moves apically the soft tissue follows, and the papilla height becomes an esthetic compromise.
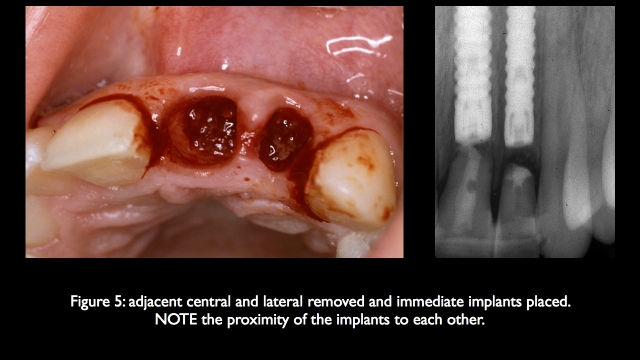
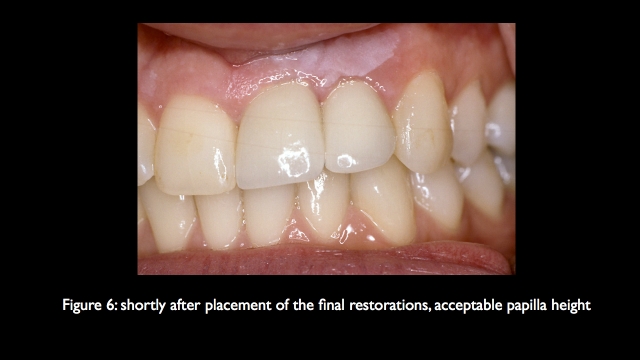

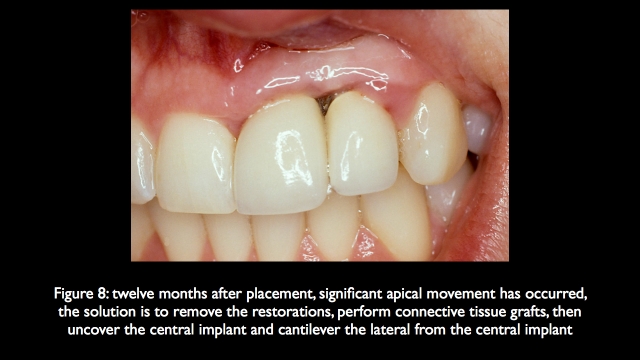
The use of platform switching can reduce this risk, allowing implants to be positioned closer together because of the decreased bone die back that occurs when the biologic width is formed. The ideal solution in the future would be implants and abutments that will promote an entirely supra crestal biologic width, if that was the case adjacent implant esthetics would be more predictable.
Avoiding Interproximal Bone Loss
The most common solution to avoiding the problem of interproximal bone loss and loss of papilla height when replacing an adjacent missing central and lateral, is to not place adjacent implants, instead utilize a central incisor implant and cantilever the lateral incisor pontic. This is also the solution when replacing an adjacent missing canine and lateral incisor, they have the same problems of reduced inter-implant distance as the missing central and lateral. I mention this because it is difficult to find any research on the long term success of a lateral incisor pontic cantilevered from a central incisor implant, but there is literature on single unit pontics cantilevered from both anterior and posterior implants, the research shows a high percentage of success. (9 & 10)
To achieve the best esthetic result in the case of the cantilevered lateral pontic, it is often necessary to perform a connective tissue graft in the lateral incisor position. This also holds true for achieving an ideal result on the appearance of the facial tissue on the implant, where a connective tissue graft can create a more ideal facial gingival thickness, color, and level.
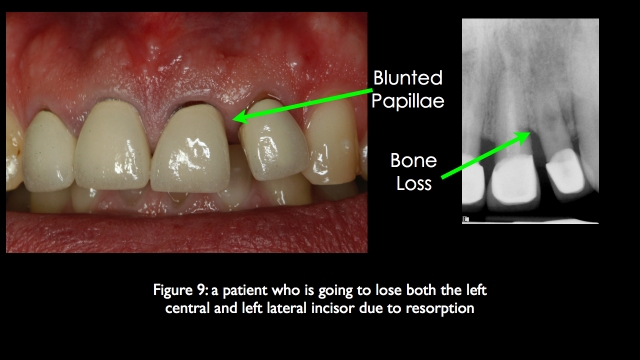
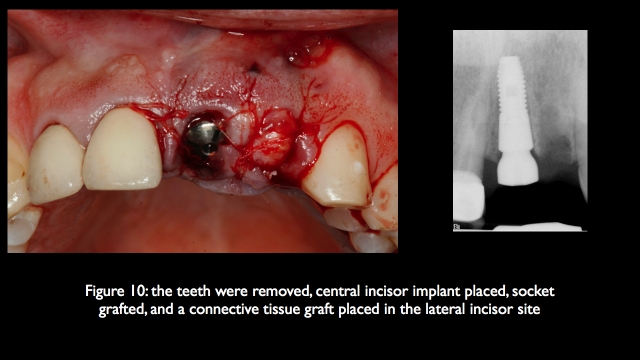
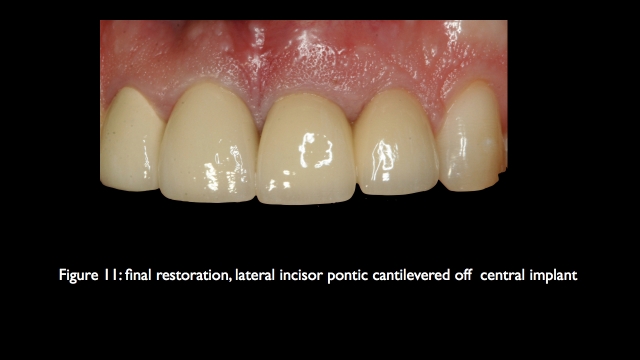
Another successful option for achieving an acceptable esthetic result when replacing an adjacent missing central and lateral is to choose a 4 unit FPD from the canine to the opposite central incisor. A connective tissue graft is almost always necessary in the pontic region if you desire a great esthetic outcome. It is important to remember that research shows an estimated 20-year survival rate of 77 percent on 4-unit FPDs with vital abutments, but if one of the abutments is non-vital, the success rate drops to 56 percent. If the non-vital abutment has minimal ferrule and a large post and core the success rate will be even worse. (11)
For these reasons, an FPD is typically not my first choice unless the canine and opposite central already have full coverage restorations on them and are vital—or the chance of achieving an acceptable result with implants is poor due to the condition of the bone, and the likelihood of augmenting the bone is unlikely to reach an acceptable result.
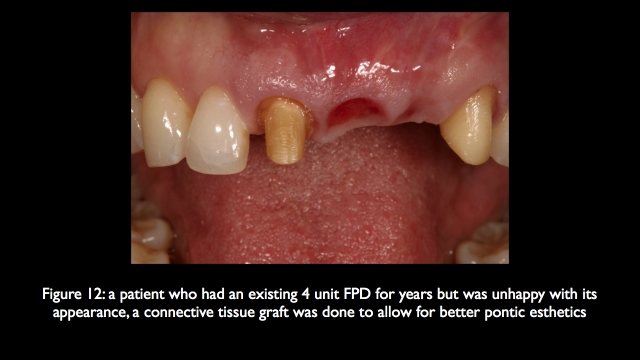
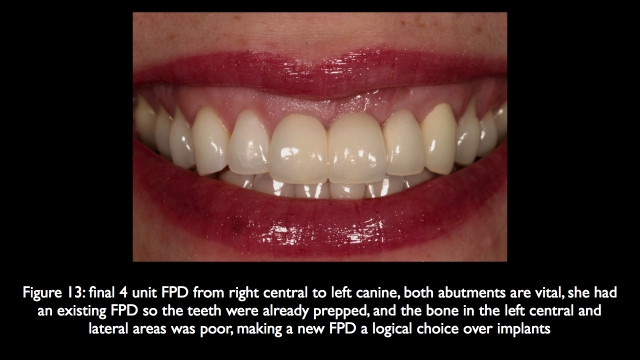
In fact in cases of significant bone loss in the central and lateral region, an FPD with pink ceramic replacing the soft tissue on the pontics is esthetically very predictable, and also easily maintained because it is possible to floss under the pontics. It is much more difficult to use pink ceramic over adjacent implants, have it look acceptable, and provide access for oral hygiene to the facial of the implants.
Another alternative in cases with significant bone loss, is to consider moving the canine into the lateral incisor position, this has the advantage of producing two single implant sites rather then two adjacent implants, or a single implant with a cantilevered pontic. In addition, as long as the canine has good bone on it, there will be excellent bone in the canine site following the mesial movement of the canine into the lateral position, and now you only have to deal with managing the central as a single tooth site.
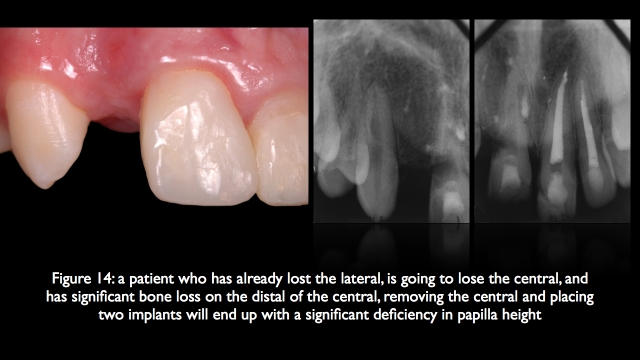
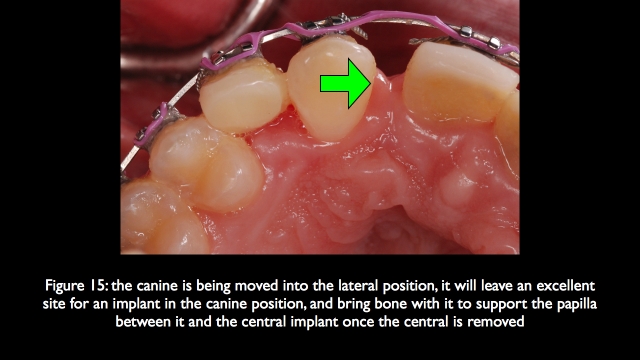

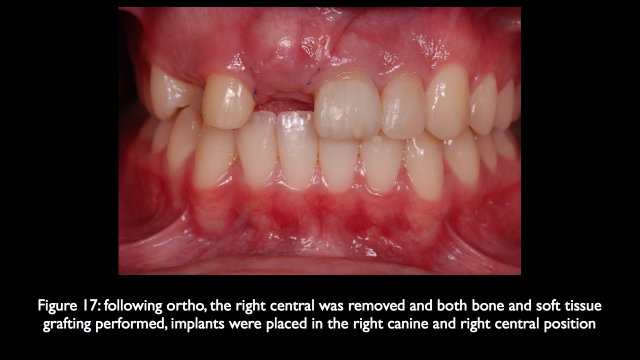
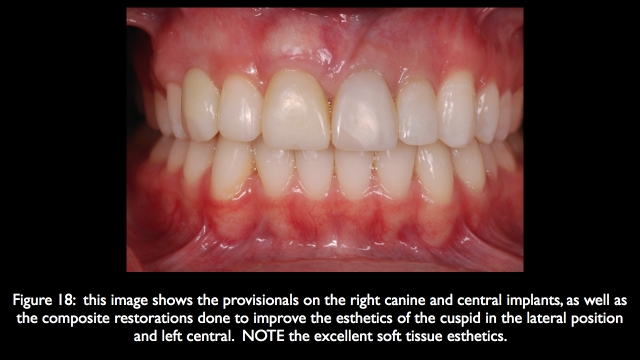
In addition as long as the remaining central has good mesial bone, there will be a good papilla between the central implant and natural central. And because the canine in the lateral position has good bone on it, there will be a good papilla between the central implant and the canine in the lateral position. This means the only challenge will be creating adequate height and thickness of bone in the central implant position to manage facial gingival levels.
Although this technique requires time to move the canine into the lateral position, it can often produce the best final result from a soft tissue esthetics perspective. And in fact concerning time, often multiple surgeries to try and augment an area with significant bone loss may require just as much time, and get an inferior result. One of the few obstacles to consider when moving the canine into the lateral position is the shape of the canine to be moved, if it is very large and bulbous, making it difficult to alter its shape to appear like a lateral incisor, the final result will be compromised. (12)
Avoid Removing Teeth if Possible
As a final recommendation, the simplest way to avoid the challenges of the missing lateral and central is to see if it is possible to avoid removing both teeth. In the 1980s, when implants first came to the US, we used them to replace teeth that were missing; we didn’t consider using implants as a way to avoid what was necessary to save a tooth.
Over the last three decades that thought process has changed for many clinicians, to the extent that some believe implants are better then teeth, so why save a compromised tooth. The answer is esthetics, as good as implants have gotten, they still don’t maintain bone and soft tissue levels like a natural tooth does, especially if the implants are placed adjacent to each other. For these reasons, I will try my best to avoid the loss of a lateral and central if possible. That means if I can manage to keep one of the teeth using whatever is necessary it leaves a single tooth site to manage that is much easier.
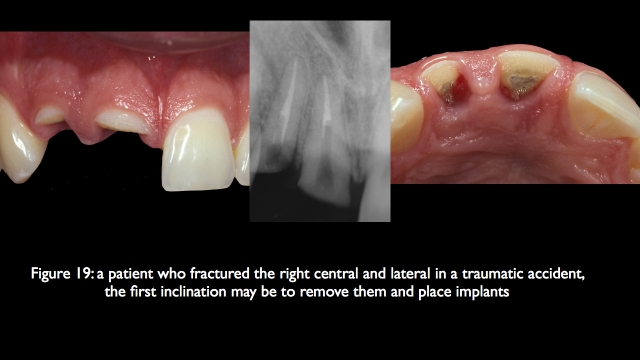
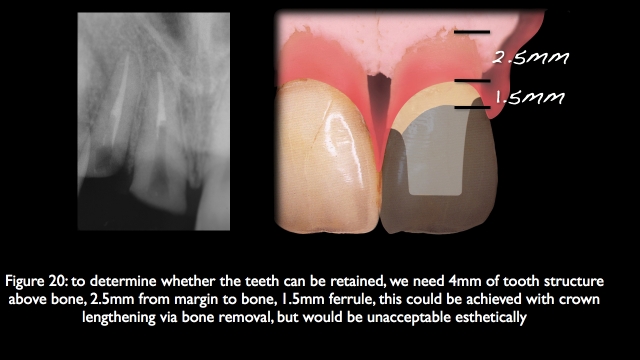
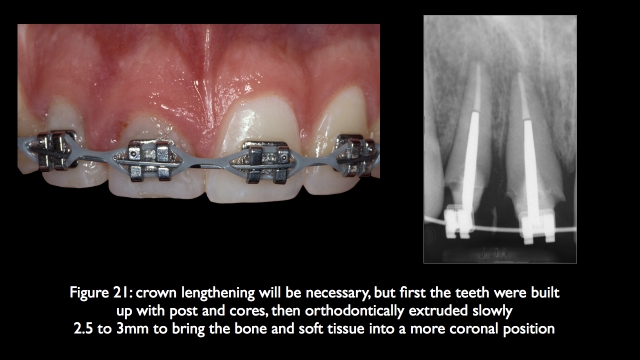
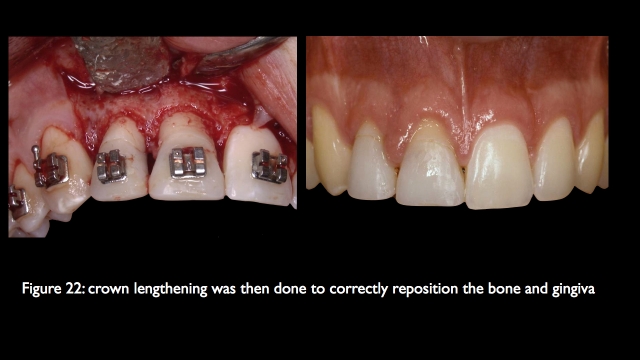
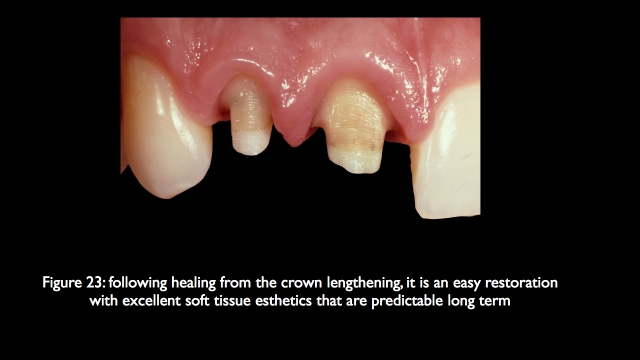
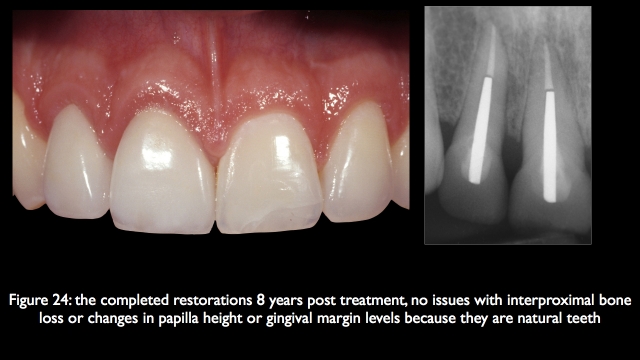
If it is possible to keep both teeth, often involving thing like forced eruption, crown lengthening, endo, post cores, and final restorations, it may be more involved then simply removing them and placing implants, but the esthetic result is much more predictable, it is certainly what I would choose for myself or my family as a first choice.
References
- Dimensions and relations of the dentogingival junction in humans. Gargiulo, Wentz & Orban Periodontal 32:261 1961.
- Clinical and radiographic evaluation of the papilla level adjacent to single tooth dental implants. A retrospective study in the maxillary anterior region. Choquet V1, Hermans M, Adriaenssens P, Daelemans P, Tarnow DP, Malevez C. J Periodontol. 2001 Oct;72(10):1364-71.
- Maintenance of the interdental papilla following anterior tooth removal. Spear FM. Pract Periodontics Aesthet Dent. 1999 Jan-Feb;11(1):21-8; quiz 30.
- Vertical distance from the crest of bone to the height of the interproximal papilla between adjacent implants. Tarnow D1, Elian N, Fletcher P, Froum S, Magner A, Cho SC, Salama M, Salama H, Garber DA. J Periodontol. 2003 Dec;74(12):1785-8.
- The inter-proximal height of bone, a guidepost to predictable aesthetic strategies and soft tissue contours in anterior tooth replacement. Salama H, Salama M, Garber D, Adar P. Pract Periodontics Aesth Dent 1998;10:1131-1141.
- Single-tooth replacement in the anterior maxilla by means of immediate implantation and provisionalization:a review. De Ruck T, COllys K, Cosyn J. Int J Oral Maxillofac Implants. Sep-Oct;23 (5): 897-904.
- Platform switching for marginal bone preservation around dental implants: a systematic review and meta-analysis. Atieh MA1, Ibrahim HM, Atieh AH. J Periodontol. 2010 Oct;81(10):1350-66. doi: 10.1902/jop.2010.100232.
- The effect of interimplant distance on the height of the interimplant bone. Rodríguez-Ciurana X1, Vela-Nebot X, Segalà-Torres M, Calvo-Guirado JL, Cambra J, Méndez-Blanco V, Tarnow DP. Int J Periodontics Restorative Dent. 2009 Apr;29(2):141-51.
- Cantilever fixed prostheses utilizing dental implants: a 10-year retrospective analysis. Becker CM. Quintessence Int. 2004 Jun;35(6):437-41.
- Survival rates of short-span implant-supported cantilever fixed dental prostheses. Stafford GL. Evid Based Dent. 2010;11(2):50-1. doi: 10.1038/sj.ebd.6400722.
- Long-term survival of complete crowns, fixed dental prostheses, and cantilever fixed dental prostheses with posts and cores on root canal treated teeth. De Backer H, Van Maele G, Decock V, Van den Berghe L. Centre for Special Care, PaeCaMed Research, Unit of Gnathology and Temporomandibular Disorders, Dental School, Faculty of Medicine and Health Sciences, Ghent University, Belgium. Int J Prosthodont. 2007 May-Jun;20(3):229-34.
- Managing congenitally missing lateral incisors. Part I: Canine substitution. Kokich VO Jr1, Kinzer GA. J Esthet Restor Dent. 2005;17(1):5-10.
SPEAR campus
Hands-On Learning in Spear Workshops
With enhanced safety and sterilization measures in place, the Spear Campus is now reopened for hands-on clinical CE workshops. As you consider a trip to Scottsdale, please visit our campus page for more details, including information on instructors, CE curricula and dates that will work for your schedule.

By: Frank Spear
Date: June 25, 2015
Featured Digest articles
Insights and advice from Spear Faculty and industry experts